Abstract
Background and Aims
The role of lymph node dissection (LND) in patients with small intrahepatic cholangiocarcinoma (ICC) is still under debate.
The aims of this study were to compare the lymph node (LN) status and its correlation with survival among patients with ICC stratified by tumor size.
Methods
A retrospective analysis of a multi-institutional series of 259 patients undergoing curative-intent surgery was carried out. Patients were stratified into Small-ICC (≤ 3 cm) and Large-ICC (> 3 cm) based on tumor size.
Results
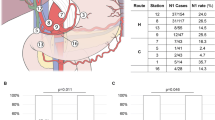
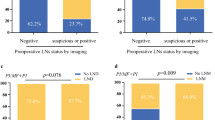
There were 53 and 206 patients in Small-ICC and Large-ICC groups, respectively. The incidence of LND was 62% among Small-ICC patients and 78% among Large-ICC patients (p = 0.016). LN metastases were identified in 30.3% and 38.5% of Small-ICC and Large-ICC patients, respectively (p = 0.37). No differences in terms of number of harvested LN and LN metastases were identified comparing Small- and Large-ICC patients. The 5-year overall survival (OS) was 52.6% for Small-ICC and 36.2% for Large-ICC (p = 0.024). The 5-year OS according to the LN status (N0 vs N+) was 84.8% and 36.0% (p = 0.032) in Small-ICC, and 45.7% and 12.1% in Large-ICC (p < 0.001), respectively.
Conclusion
While Small-ICC patients with no LN metastasis had a good long-term survival, the LN resulted in an important variable associated with survival also for patients in this group. Moreover, the incidence of LN metastasis did not differ when comparing Small-ICC and Large-ICC patients, suggesting that LND is mandatory in the surgical treatment of ICC regardless of tumor size.


Similar content being viewed by others
References
Gupta A, Dixon E. Epidemiology and risk factors: intrahepatic cholangiocarcinoma. Hepatobiliary Surg Nutr 2017;6(2):101–104.
Shaib YH, Davila JA, McGlynn K, El-Serag HB. Rising incidence of intrahepatic cholangiocarcinoma in the United States: A true increase? J Hepatol 2004;40(3):472–477.
William C. Palmer, MD and Tushar Patel. Are common factors involved in the pathogenesis of primary liver cancers? A meta-analysis of risk factors for intrahepatic cholangiocarcinoma. J Hepatol 2012;57(1):69–76.
Ruzzenente A, Conci S, Valdegamberi A, Pedrazzani C, Guglielmi A. Role of surgery in the treatment of intrahepatic cholangiocarcinoma. Eur Rev Med Pharmacol Sci 2015;19(15):2892–900.
de Jong M.C., Nathan H., Sotiropoulos G.C., Paul A., Alexandrescu S., Marques H. et al. Intrahepatic cholangiocarcinoma: an international multi-institutional analysis of prognostic factors and lymph node assessment. J Clin Oncol 2011;29:3140–3145.
Bagante F., Spolverato G.; Weiss M., Alexandrescu s., Marques H., Aldrighetti L. et al. Defining Long-Term Survivors Following Resection of Intrahepatic Cholangiocarcinoma. J Gastrointest Surg 2017; 21:1888–1897.
Spolverato G, Kim Y, Ejaz A, Alexandrescu S, Marques H, Aldrighetti L, et al. Conditional probability of long-term survival after liver resection for intrahepatic cholangiocarcinoma: a multiinstitutional analysis of 535 patients. JAMA Surg 2015;150:538–545.
Ribero D, Pinna AD, Guglielmi A, Ponti A, Nuzzo G, et al. Surgical Approach for Long-term Survival of Patients With Intrahepatic Cholangiocarcinoma: A Multi-institutional Analysis of 434 Patients. Arch Surg 2012;147(12):1107–13.
Mavros MN, Economopoulos KP, Alexiou VG, Pawlik TM. Treatment and prognosis for patients with intrahepatic cholangiocarcinoma: systematic review and meta-analysis. JAMA Surg 2014;149:565–574.
Sakamoto Y, Kokudo N, Matsuyama Y, et al. Proposal of a new staging system for intrahepatic cholangiocarcinoma: Analysis of surgical patients from a nationwide survey of the Liver Cancer Study Group of Japan. Cancer 2016;122:61–70.
Sapisochin G, Facciuto M, Rubbia-Brandt L, et al. Liver transplantation for “very early” intrahepatic cholangiocarcinoma: International retrospective study supporting a prospective assessment. Hepatology 2016;64:1178–88.
Adachi T, Eguchi S. Lymph node dissection for intrahepatic cholangiocarcinoma: a critical review of the literature to date. J Hepatobiliary Pancreat Sci 2014;21:162–8.
Jutric Z, Johnston WC, Hoen HM, et al. Impact of lymph node status in patients with intrahepatic cholangiocarcinoma treated by major hepatectomy: a review of the National Cancer Database. HPB 2016;18(1):79–87.
Bagante F, Gani F, Spolverato G, et al.: Intrahepatic cholangiocarcinoma: Prognosis of patients who did not undergo lymphadenectomy. J Am Coll Surg 2015;221:1031–1040.
Guglielmi A, Ruzzenente A, Campagnaro T, et al. Patterns and prognostic significance of lymph node dissection for surgical treatment of perihilar and intrahepatic cholangiocarcinoma. J Gastrointest Surg 2013;17(11):1917–28.
Murakami Y, Uemura K, Sudo T, Hashimoto Y, Nakashima A, Sueda T. Intrahepatic cholangiocarcinoma: clinicopathological differences between peripheral type and hilar type. J Gastrointest Surg 2012;16:540–8
Shirabe K, Mano Y, Taketomi A, Soejima Y, Uchiyama H, Aishima S. Clinicopathological prognostic factors after hepatectomy for patients with mass-forming type intrahepatic cholangiocarcinoma: relevance of the lymphatic invasion index. Ann Surg Oncol 2010;17:1816–22
Hyder O, Marques H, Pulitano C, Marsh JW, Alexandrescu S, Bauer TW et al. A nomogram to predict long-term survival after resection for intrahepatic cholangiocarcinoma: an Eastern and Western experience. JAMA Surg 2014;149:432–438.
Zhang XF, Chakedis J, Bagante F, Chen Q, Beal EV, Lv Y, et al. Trends in use of lymphadenectomy in surgery with curative intent for intrahepatic cholangiocarcinoma. Br J Surg 2018;105(7):857–866.
Amini N., Ejaz A., Spolverato G., Maithel S.K., Kim Y., Pawlik T.M. Management of lymph nodes during resection of hepatocellular carcinoma and intrahepatic cholangiocarcinoma: a systematic review. J Gastrointest Surg 2014;18:2136–2148.
Nakagawa T, Kamiyama T, Kurauchi N, Matsushita M, Nakanishi K, Kamachi H et al. Number of lymph node metastases is a significant prognostic factor in intrahepatic cholangiocarcinoma. World J Surg 2005;29(6):728–33.
Dhanasekaran R, Hemming AW, Zendejas I, George T, Nelson DR, Soldevila-Pico C, et al. Treatment outcomes and prognostic factors of intra-hepatic cholangiocarcinoma. Oncol Rep 2013;29:1259–1267.
Guglielmi A, Ruzzenente A, Campagnaro T, Pachera S, Valdegamberi A, Nicoli P, Cappellani A, Malfermoni G, Iacono C. Intrahepatic cholangiocarcinoma: prognostic factors after surgical resection. World J Surg 2009;33(6):1247–54.
Wang Y, Li J, **a Y, et al. Prognostic nomogram for intrahepatic cholangiocarcinoma after partial hepatectomy. J Clin Oncol 2013;31(9):1188–1195
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Data collection and analysis were performed according to the institutional guidelines and were conformed to the ethical standards of the World Medical Association (Declaration of Helsinki). The study was approved by each local ethical committee, and signed consent was obtained from all the subjects included in the study.
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
Figure S1
Overall survival between Large-ICC and Small-ICC according to the different LN Status: A, N0 (p = 0.028); B, N+ (p = 0.048); C, NX (p = 0.985). (PPTX 3715 kb)
Figure S2
Overall survival between Large-ICC and Small-ICC according to the different LN Status (N0, N+ and NX) (p = 0.001). (PPTX 1272 kb)
Rights and permissions
About this article
Cite this article
Ruzzenente, A., Conci, S., Viganò, L. et al. Role of Lymph Node Dissection in Small (≤ 3 cm) Intrahepatic Cholangiocarcinoma. J Gastrointest Surg 23, 1122–1129 (2019). https://doi.org/10.1007/s11605-019-04108-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-019-04108-0