Abstract
Introduction
Re-operation is advised for patients with T1b or greater incidental gallbladder cancer (GBCA). The presence of residual disease (RD) impacts resectability, chemotherapy, and survival. This study created a preoperative model to predict RD at re-operation.
Methods
Patients with re-operation for incidental GBCA from 1992–2015 were included. The relationship between pathology data from initial cholecystectomy and RD at re-operation was assessed with logistic regression and classification and regression tree (CART) analysis.
Results
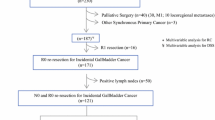
Two hundred fifty-four patients were included and 188 underwent definitive re-resection (74.0%). Distant RD was identified in 69 (27.2%) patients and locoregional only RD in 82 (32.3%). On multivariate analysis, T3 (OR 22.7, 95% CI 5.5–94.4) and poorly differentiated tumors (OR 4.3, 95% CI 1.4–13.3) were associated with RD (p < 0.001–0.012). AUC of multivariate model was 0.78 (95% CI 0.72–0.83). CART analysis split patients into groups based on percentage with RD: 87% RD with T3, 67% RD with T1b/T2 and poorly differentiated, and 35% RD with T1b/T2 and well/moderate differentiated tumors.
Conclusion
Based on T stage and grade from cholecystectomy, this study developed a model for predicting RD at re-operation in incidental GBCA. This model delineates patient groups with variable percentages of RD and could be used to stratify high-risk patients for prospective trials.



Similar content being viewed by others
References
Hueman MT, Vollmer CM Jr, Pawlik TM. Evolving treatment strategies for gallbladder cancer. Annals of surgical oncology. 2009; 16(8):2101–15.
Fong Y, Jarnagin W, Blumgart LH. Gallbladder cancer: comparison of patients presenting initially for definitive operation with those presenting after prior noncurative intervention. Annals of surgery. 2000; 232(4):557–69.
Fuks D, Regimbeau JM, Le Treut YP, et al. Incidental gallbladder cancer by the AFC-GBC-2009 Study Group. World journal of surgery. 2011; 35(8):1887–97.
Goetze TO, Paolucci V. Benefits of reoperation of T2 and more advanced incidental gallbladder carcinoma: analysis of the German registry. Annals of surgery. 2008; 247(1):104–8.
Aloia TA, Jarufe N, Javle M, et al. Gallbladder cancer: expert consensus statement. HPB: the official journal of the International Hepato Pancreato Biliary Association. 2015; 17(8):681–90.
D'Angelica M, Dalal KM, DeMatteo RP, et al. Analysis of the Extent of Resection for Adenocarcinoma of the Gallbladder. Annals of surgical oncology. 2009; 16(4):806–16.
Pawlik TM, Gleisner AL, Vigano L, et al. Incidence of finding residual disease for incidental gallbladder carcinoma: implications for re-resection. Journal of gastrointestinal surgery: official journal of the Society for Surgery of the Alimentary Tract. 2007; 11(11):1478–86; discussion 86-7.
Butte JM, Kingham TP, Gönen M, et al. Residual Disease Predicts Outcomes after Definitive Resection for Incidental Gallbladder Cancer. Journal of the American College of Surgeons. 2014; 219(3):416–29.
Butte JM, Waugh E, Meneses M, et al. Incidental Gallbladder Cancer: Analysis of Surgical Findings and Survival. Journal of surgical oncology. 2010; 102(6):620–5.
Ito H, Ito K, D'Angelica M, et al. Accurate Staging for Gallbladder Cancer Implications for Surgical Therapy and Pathological Assessment. Annals of surgery. 2011; 254(2):320–5.
Ethun CG, Postlewait LM, Le N, et al. A Novel Pathology-Based Preoperative Risk Score to Predict Locoregional Residual and Distant Disease and Survival for Incidental Gallbladder Cancer: A 10-Institution Study from the U.S. Extrahepatic Biliary Malignancy Consortium. Annals of surgical oncology. 2017; 24(5):1343–50.
Jarnagin WR, Ruo L, Little SA, et al. Patterns of initial disease recurrence after resection of gallbladder carcinoma and hilar cholangiocarcinoma: implications for adjuvant therapeutic strategies. Cancer. 2003; 98(8):1689–700.
Li W, Qin J, Sun YH, Liu TS. Neoadjuvant chemotherapy for advanced gastric cancer: a meta-analysis. World journal of gastroenterology. 2010; 16(44):5621–8.
Blazer M, Wu C, Goldberg RM, et al. Neoadjuvant modified (m) FOLFIRINOX for locally advanced unresectable (LAPC) and borderline resectable (BRPC) adenocarcinoma of the pancreas. Annals of surgical oncology. 2015; 22(4):1153–9.
Butte JM, Gonen M, Allen PJ, et al. The role of laparoscopic staging in patients with incidental gallbladder cancer. Hpb. 2011; 13(7):463–72.
Maker AV, Butte JM, Oxenberg J, et al. Is port site resection necessary in the surgical management of gallbladder cancer? Annals of surgical oncology. 2012; 19(2):409–17.
Hastie T, Tibshirani R, Friedman JH. The elements of statistical learning: data mining, inference, and prediction. 2nd ed. New York: Springer; 2009. xxii, 745 p.
Zhang H, Singer B, Zhang H. Recursive partitioning and applications. 2nd ed. New York: Springer; 2010. xiv, 259 p.
Valle J, Wasan H, Palmer DH, et al. Cisplatin plus gemcitabine versus gemcitabine for biliary tract cancer. The New England journal of medicine. 2010; 362(14):1273–81.
Rubin DB. Inference and Missing Data. Biometrika. 1976; 63(3):581–90.
Vach W, Blettner M. Missing data in epidemiologic studies. Encyclopedia of biostatistics. New York: John Wiley and Sons; 1998. 2641 p.
Burton A, Altman DG. Missing covariate data within cancer prognostic studies: a review of current reporting and proposed guidelines. British journal of cancer. 2004; 91(1):4–8.
College of American Patholgists. Cancer protocols 2012 [cited September 30, 2016]. Available from: http://www.cap.org/web/hom/resources/cancer-reporting-tools/cancer-protocols.
Ausania F, Tsirlis T, White SA, et al. Incidental pT2-T3 gallbladder cancer after a cholecystectomy: outcome of staging at 3 months prior to a radical resection. HPB: the official journal of the International Hepato Pancreato Biliary Association. 2013; 15(8):633–7.
Duffy A, Capanu M, Abou-Alfa GK, et al. Gallbladder cancer (GBC): 10-year experience at Memorial Sloan-Kettering Cancer Centre (MSKCC). Journal of surgical oncology. 2008; 98(7):485–9.
Bartlett DL, Fong Y, Fortner JG, et al. Long-term results after resection for gallbladder cancer. Implications for staging and management. Annals of surgery. 1996; 224(5):639–46.
Author information
Authors and Affiliations
Contributions
All authors met criteria for authorship based on contributions to the manuscript in submission.
Corresponding author
Ethics declarations
Funding
This work was supported in part by the NIH/NCI P30 CA008748 Cancer Center Support Grant.
Conflict of Interest
The authors declare that they have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Creasy, J.M., Goldman, D.A., Gonen, M. et al. Predicting Residual Disease in Incidental Gallbladder Cancer: Risk Stratification for Modified Treatment Strategies. J Gastrointest Surg 21, 1254–1261 (2017). https://doi.org/10.1007/s11605-017-3436-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-017-3436-8