Abstract
Purpose
Learning how to use barbed sutures and perform Barbed Pharyngoplasty (BP) is challenging due to limited surgical training opportunities. This work aims to design, develop, and validate a new 3D surgical simulator to train ENT residents and specialists in performing BP.
Methods
The Barbed Pharyngoplasty Simulator (BPS) was designed using diagnostic images of the facial mass and testing different materials to replicate the mucosal and bony tissues. ENT specialists with experience in BP and ENT residents were included in the validation study and were asked to perform the Alianza BP. After the simulation, they compiled the Face and Content Validity Questionnaires.
Results
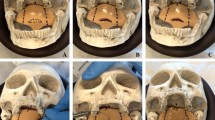
The BPS consists of a reusable cranial structure that contains the disposable palatopharyngeal structure, replicating the palatal structures and the tongue. Fifteen experienced ENT specialists and nine residents were included in the study. Findings demonstrated that the BPS faithfully replicated the muscular and fibrous-bony palatopharyngeal structures, with only 11% of residents having a negative opinion of the mucosal tissue. All the participants positively rated the sensation of using surgical instruments on the simulator. Also, ENT residents rated all aspects of the content validity test from normal to excellent, while specialists rated the BPS as a general training tool from normal to excellent; for lateral pharyngoplasty, BP, and Alianza, only 6.7% of participants disagreed with its usefulness, and 13.3% disagreed with it for anterior pharyngoplasty.
Conclusion
The BPS proposed in this preliminary study can potentially be a valuable tool in BP surgical training for residents and young otolaryngologists.





Similar content being viewed by others
Data availability
The data that support the findings of this study are not openly available due to reasons of sensitivity and are available from the corresponding author upon reasonable request.
References
Mantovani M, Rinaldi V, Salamanca F, Torretta S, Carioli D, Gaffuri M, Pignataro L (2014) Should We Stop Performing Uvulopalatopharyngoplasty? In Indian J Otolaryngology Head Neck Surgery 67(1):161–162. https://doi.org/10.1007/s12070-014-0800-9. (Springer India)
Casale M, Moffa A, Pierri M, Baptista P, & Giorgi L (2023). High-Definition 3D Exoscope-Assisted Barbed Pharyngoplasty for OSAS and Snoring: Better Than Live. Healthcare 11(4). https://doi.org/10.3390/HEALTHCARE11040596
Moffa A, Rinaldi V, Mantovani M, Pierri M, Fiore V, Costantino A, Pignataro L, Baptista P, Cassano M, Casale M (2020) Different barbed pharyngoplasty techniques for retropalatal collapse in obstructive sleep apnea patients: a systematic review. In Sleep and Breathing 24(3):1115–1127. https://doi.org/10.1007/s11325-020-02088-z. (Springer)
Moffa A, Giorgi L, Carnuccio L, Cassano M, Lugo R, Baptista P, Casale M (2023). Barbed Pharyngoplasty for Snoring: Does It Meet the Expectations? A Systematic Review. Healthcare (Basel, Switzerland), 11(3). https://doi.org/10.3390/HEALTHCARE11030435
Vicini C, Meccariello G, Montevecchi F, De Vito A, Frassineti S, Gobbi R, Pelucchi S, Iannella G, Magliulo G, Cammaroto G (2020) Effectiveness of barbed repositioning pharyngoplasty for the treatment of obstructive sleep apnea (OSA): a prospective randomized trial. Sleep and Breathing 24(2):687–694. https://doi.org/10.1007/s11325-019-01956-7
Casale M, Moffa A, Giorgi L, Sabatino L, Pierri M, Lugo R, Baptista P, Rinaldi V (2022) No-cutting remodelling intra-pharyngeal surgery can avoid CPAP in selected OSA patients: myth or reality? Eur Arch Otorhinolaryngol 279(10):5039–5045. https://doi.org/10.1007/s00405-022-07261-6
Rinaldi V, Mancini G, de Apodaca PMR, Vicini C, Carrasco M (2023) “Pharyngolab”: a new surgical simulator for pharyngoplasties. Eur Arch Oto-Rhino-Laryngol 280(3):1339–13
Rinaldi V, Costantino A, Moffa A, Baptista P, Sabatino L, Casale M (2019) “Barbed snore surgery” simulator: a low-cost surgical model. Eur Arch Oto-Rhino-Laryngology 276(8):2345–2348. https://doi.org/10.1007/S00405-019-05497-3
Low CM, Morris JM, Matsumoto JS, Stokken JK, O’Brien EK, Choby G (2019) Use of 3D-Printed and 2D-Illustrated International Frontal Sinus Anatomy Classification Anatomic Models for Resident Education. Otolaryngology - Head and Neck Surgery (United States) 161(4):705–713. https://doi.org/10.1177/0194599819860832
Rinaldi V, Costantino A, Moffa A, Casale M (2019) Ex-vivo surgical model for “Barbed Snore Surgery”: a feasibility study. Eur Arch Otorhinolaryngol 276(12):3539–3542. https://doi.org/10.1007/s00405-019-05660-w
Awad Z, Ahmed S, Taghi AS, Ghufoor K, Wareing MJ, Patel N, Tolley NS (2014) Feasibility of a synthetic temporal bone for training in mastoidectomy: Face, content, and concurrent validity. Otol Neurotol 35(10):1813–1818. https://doi.org/10.1097/MAO.0000000000000511
Steehler MK, Pfisterer MJ, Na H, Hesham HN, Pehlivanova M, Malekzadeh S (2012) Face, Content, and Construct Validity of a Low-Cost Sinus Surgery Task Trainer. Otolaryngology-Head and Neck Surgery 146(3):504–509. https://doi.org/10.1177/0194599811430187
Vicini C, Hendawy E, Campanini A, Eesa M, Bahgat A, AlGhamdi S, Meccariello G, DeVito A, Montevecchi F, Mantovani M (2015) Barbed reposition pharyngoplasty (BRP) for OSAHS: a feasibility, safety, efficacy and teachability pilot study. “We are on the giant’s shoulders.” Eur Arch Oto-Rhino-Laryngology 272(10):3065–3070. https://doi.org/10.1007/s00405-015-3628-3
Alwani MM, Svenstrup TJ, Bandali EH, Sharma D, Higgins TS, Wu AW, Shipchandler TZ, Illing EA, Ting JY (2020) Validity testing of a three-dimensionally printed endoscopic sinonasal surgery simulator. Laryngoscope 130(12):2748–2753. https://doi.org/10.1002/lary.28356
Sonnadara RR, Mui C, McQueen S, Mironova P, Nousiainen M, Safir O, Kraemer W, Ferguson P, Alman B, Reznick R (2014) Reflections on Competency-Based Education and Training for Surgical Residents. J Surg Educ 71(1):151–158. https://doi.org/10.1016/J.JSURG.2013.06.020
James J, Irace ALA, Drusin M, Kim AH, Gudis DA, Overdevest JB (2022) Thinking Beyond the Temporal Bone Lab: A Systematic Process for Expanding Surgical Simulation in Otolaryngology Training. Ann Otology Rhinol Laryngology 132(7):828–836. https://doi.org/10.1177/00034894221115753
Musbahi O, Aydin A, Al Omran Y, Skilbeck CJ, Ahmed K (2017) Current Status of Simulation in Otolaryngology: A Systematic Review. J Surg Educ 74(2):203–215. https://doi.org/10.1016/J.JSURG.2016.09.007
Cote V, Schwartz M, Arbouin Vargas JF, Canfarotta M, Kavanagh KR, Hamdan U, Valdez TA (2018) 3-Dimensional printed haptic simulation model to teach incomplete cleft palate surgery in an international setting. Int J Pediatr Otorhinolaryngol 113:292–297. https://doi.org/10.1016/J.IJPORL.2018.08.016
Alrasheed AS, Nguyen LHP, Mongeau L, Funnell WRJ, Tewfik MA (2017) Development and validation of a 3D-printed model of the ostiomeatal complex and frontal sinus for endoscopic sinus surgery training. Int Forum Allerg Rhinology 7(8):837–841. https://doi.org/10.1002/alr.21960
Ranjan R, Kumar D, Kundu M, Chandra Moi S (2022) A critical review on Classification of materials used in 3D printing process. Materials Today: Proceedings. https://doi.org/10.1016/j.matpr.2022.03.308
Crafts TD, Ellsperman SE, Wannemuehler TJ, Bellicchi TD, Shipchandler TZ, Mantravadi AV (2017) Three-Dimensional Printing and Its Applications in Otorhinolaryngology-Head and Neck Surgery. Otolaryngology - Head and Neck Surgery (United States) 156(6):999–1010. https://doi.org/10.1177/0194599816678372
Martelli N, Serrano C, van den Brink H, Pineau J, Prognon P, Borget I, El Batti S (2016) Advantages and disadvantages of 3-dimensional printing in surgery: A systematic review. Surgery 159(6):1485–1500. https://doi.org/10.1016/j.surg.2015.12.017
Kostas JC, Lee AS, Arunkumar A, Han C, Lee M, Goel AN, Alrassi J, Crosby T, Clark CM, Amin M, Abu-Ghanem S, Kirke D, Rameau A (2023) Validation of a 3D-Printed Percutaneous Injection Laryngoplasty Simulator: A Randomized Controlled Trial. Laryngoscope. https://doi.org/10.1002/LARY.30878
Garaycochea O, Baptista P, Calvo-Imirizaldu M, Terrasa D, Moffa A, Casale M, Alcalde J, O’Connor-Reina C, Plaza G, Fernández S (2022) Surgical anatomy of the lingual nerve for palate surgery: where is located and how to avoid it. Eur Arch Otorhinolaryngol 279(11):5347. https://doi.org/10.1007/S00405-022-07432-5
Olszewska E, Woodson BT (2019) Palatal anatomy for sleep apnea surgery. Laryngoscope Investigative Otolaryngology 4(1):181. https://doi.org/10.1002/LIO2.238
Chen G, Jiang M, Coles-Black J, Mansour K, Chuen J, Amott D (2020) Three-dimensional printing as a tool in otolaryngology training: A systematic review. J Laryngol Otol 134(1):14–19. https://doi.org/10.1017/S0022215119002585
Nadagouda MN, Ginn M, Rastogi V (2020) A review of 3D printing techniques for environmental applications. Curr Opin Chem Eng 28:173–178. https://doi.org/10.1016/j.coche.2020.08.002
Acknowledgements
Thanks to “MediLife Innovation and Technology,” which supported our team in the design and manufacturing process of the 3D-surgical simulator.
Funding
No funding was received for this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
The study was conducted by the Declaration of Helsinki and approved by the Fondazione Policlinico Universitario Campus Bio-Medico Ethics Committee. Appoval Code: PAR 96.23 OSS. Approval Date: 19/04/2023.
Informed consent
Informed consent was obtained from all participants in the study.
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Giorgi, L., Moffa, A., Pericone, G. et al. Barbed Pharyngoplasty simulation using a 3D-printed model: design and validation study. Sleep Breath (2024). https://doi.org/10.1007/s11325-024-03067-4
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11325-024-03067-4