Abstract
Background
Several preoperative systemic inflammation indices have been proven to be correlated with the prognosis of patients diagnosed with non-metastatic renal cell carcinoma (RCC). However, these indices are currently not included in the main prognostic models, and few studies have compared the prognostic efficacy of different preoperative systemic inflammation indices.
Patients and methods
This retrospective study reviewed patients diagnosed with non-metastatic RCC who underwent nephrectomy at West China Hospital of Sichuan University from 2011 to 2013. Different preoperative systemic inflammation indices (neutrophil-to-lymphocyte ratio [NLR], platelet-to-lymphocyte ratio [PLR], monocyte-to-lymphocyte ratio [MLR], systemic immune-inflammation index [SII], and systemic inflammation response index [SIRI]) were calculated. Logistic regression was used to explore the relationship between systemic inflammation indices and clinical characteristics, and Cox regression was used to identify independent prognostic factors of overall survival (OS). The concordance index (c-index) was also calculated.
Results
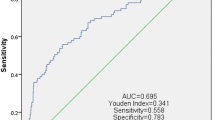
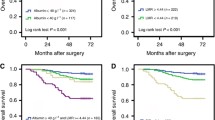
A total of 820 patients were included in the study, with a median follow-up of 78 months. Higher levels of NLR (> 3.04), PLR (> 147), MLR (> 0.32), SII (> 700), and SIRI (> 1.27) were found to be associated with more advanced tumor stage, higher Furman grade, and larger tumor size. In multivariate Cox regression, NLR, PLR, MLR, SII, and SIRI were identified as independent prognostic factors, and SII had the highest and most significant hazard ratio and the largest c-index.
Conclusion
In conclusion, various systemic inflammation indices were found to be associated with poorer OS. Among them, SII exhibited the highest predictive efficacy, suggesting its potential inclusion as a component in future prognostic models.



Similar content being viewed by others
Availability of data and materials
Data for this study will be provided by the corresponding author for reasonable reasons.
References
Sung H et al (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 Countries. CA Cancer J Clin 71(3):209–249
Ljungberg B et al (2022) European Association of urology guidelines on renal cell carcinoma: the 2022 update. Eur Urol 82(4):399–410
Frank I et al (2002) An outcome prediction model for patients with clear cell renal cell carcinoma treated with radical nephrectomy based on tumor stage, size, grade and necrosis: the SSIGN score. J Urol 168(6):2395–2400
Leibovich BC et al (2018) Predicting oncologic outcomes in renal cell carcinoma after surgery. Eur Urol 73(5):772–780
Zisman A et al (2002) Risk group assessment and clinical outcome algorithm to predict the natural history of patients with surgically resected renal cell carcinoma. J Clin Oncol 20(23):4559–4566
Bensalah K et al (2006) Prognostic value of thrombocytosis in renal cell carcinoma. J Urol 175(3 Pt 1):859–863
Chen Z et al (2019) Systemic inflammation response index predicts prognosis in patients with clear cell renal cell carcinoma: a propensity score-matched analysis. Cancer Manag Res 11:909–919
de Martino M et al (2013) Prognostic impact of preoperative neutrophil-to-lymphocyte ratio in localized nonclear cell renal cell carcinoma. J Urol 190(6):1999–2004
Hu X et al (2020) Preoperative systemic immune-inflammation index predicts prognosis of patients with non-metastatic renal cell carcinoma: a propensity score-matched analysis. Cancer Cell Int 20:222
Hutterer GC et al (2014) Low preoperative lymphocyte-monocyte ratio (LMR) represents a potentially poor prognostic factor in nonmetastatic clear cell renal cell carcinoma. Urol Oncol 32(7):1041–1048
Obata J et al (2016) Plasma fibrinogen level: an independent prognostic factor for disease-free survival and cancer-specific survival in patients with localised renal cell carcinoma. BJU Int 118(4):598–603
Wang Z et al (2018) Platelet-lymphocyte ratio acts as an independent predictor of prognosis in patients with renal cell carcinoma. Clin Chim Acta 480:166–172
Mantovani A et al (2008) Cancer-related inflammation. Nature 454(7203):436–444
Roxburgh CS, McMillan DC (2010) Role of systemic inflammatory response in predicting survival in patients with primary operable cancer. Future Oncol 6(1):149–163
Grivennikov SI, Greten FR, Karin M (2010) Immunity, inflammation, and cancer. Cell 140(6):883–899
Shaul ME, Fridlender ZG (2019) Tumour-associated neutrophils in patients with cancer. Nat Rev Clin Oncol 16(10):601–620
Tan KW et al (2013) Neutrophils contribute to inflammatory lymphangiogenesis by increasing VEGF-A bioavailability and secreting VEGF-D. Blood 122(22):3666–3677
Gay LJ, Felding-Habermann B (2011) Contribution of platelets to tumour metastasis. Nat Rev Cancer 11(2):123–134
Labelle M, Begum S, Hynes RO (2011) Direct signaling between platelets and cancer cells induces an epithelial-mesenchymal-like transition and promotes metastasis. Cancer Cell 20(5):576–590
Ruffell B, Coussens LM (2015) Macrophages and therapeutic resistance in cancer. Cancer Cell 27(4):462–472
Saroha S et al (2013) Lymphopenia is an independent predictor of inferior outcome in clear cell renal carcinoma. J Urol 189(2):454–461
Buti S et al (2017) Validation of a new prognostic model to easily predict outcome in renal cell carcinoma: the GRANT score applied to the ASSURE trial population. Ann Oncol 28(11):2747–2753
Allenet C et al (2022) Can pre-operative neutrophil-to-lymphocyte ratio (NLR) help predict non-metastatic renal carcinoma recurrence after nephrectomy? (UroCCR-61 Study). Cancers (Basel) 14(22)
Zhang W et al (2019) Systemic immune-inflammation index predicts prognosis of bladder cancer patients after radical cystectomy. Ann Transl Med 7(18):431
Jan HC, Yang WH, Ou CH (2019) Combination of the preoperative systemic immune-inflammation index and monocyte-lymphocyte ratio as a novel prognostic factor in patients with upper-tract urothelial carcinoma. Ann Surg Oncol 26(2):669–684
Funding
None.
Author information
Authors and Affiliations
Contributions
All listed authors contributed to data collection, collation, analysis, and writing of the manuscript and approved the submission of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethics approval and consent to participate
The ethical standards set by the ethics committee of Sichuan University West China Hospital were followed during all human participant studies. This study was approved by the ethics committee of Sichuan University West China Hospital, and the requirement for informed consent was waived by the board.
Consent for publication
All listed authors agree to publish.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tang, Y., Shao, Y., Hu, X. et al. Validation and comparison of prognostic value of different preoperative systemic inflammation indices in non-metastatic renal cell carcinoma. Int Urol Nephrol 55, 2799–2807 (2023). https://doi.org/10.1007/s11255-023-03724-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-023-03724-9