Abstract
Purpose
To assess child and family engagement in the selection of patient-reported outcomes for clinical studies/clinical settings and development of patient-reported outcome measures (PROMs)/patient-reported experience measures (PREMs) across the pediatric literature.
Methods
Databases were reviewed: EMBASE, MEDLINE, and PsycINFO. Articles published from December 2009 to September 2018 pertaining to the selection of outcomes or development of PROMs/PREMs for children or families were included. The International Association for Public Participation (IAP2) Spectrum of Public Participation was used to classify levels of engagement across each article; IAP2 plots engagement on a spectrum across five stages (from minimal to most engagement): Inform, Consult, Involve, Collaborate, and Empower.
Results
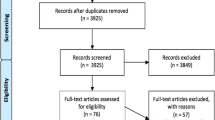
9019 non-duplicate articles were screened; 36 articles met inclusion criteria, seven studies focused on the selection of outcomes, and 29 studies pertained to PROM/PREM development. Twenty-three articles adhered to ‘Involve’ level of engagement. Four articles were categorized as ‘Collaborate,’ seven articles were classified as ‘Consult,’ and three articles were categorized as ‘Inform’.
Conclusion
Children and families were sparsely engaged as co-conductors or equal partners in the selection or development of PRO research; involvement remained on the mid-low end of the IAP2 Spectrum. Engaging with children and families as collaborators can improve the patient-centredness, rigour, and applicability of PROM/PREM research.


Similar content being viewed by others
References
Braithwaite, J., Testa, L., Lamprell, G., Herkes, J., Ludlow, K., McPherson, E., et al. (2017). Built to last? The sustainability of health system improvements, interventions and change strategies: A study protocol for a systematic review. British Medical Journal Open, 7(11), e018568. https://doi.org/10.1136/bmjopen-2017-018568
Thomson, S., Foubister, T., Figueras, J., Kutzin, J., Permanand, G., & Bryndová, L. (2009). Addressing financial sustainability in health systems. World Health Organization. Retrieved September 2020 from https://www.euro.who.int/__data/assets/pdf_file/0018/76041/E93058.pdf.
Serebrisky, D., & Wiznia, A. (2019). Pediatric asthma: A global epidemic. Annals of Global Health, 85(1), 6. https://doi.org/10.5334/aogh.2416
Cohen, E., & Patel, H. (2014). Responding to the rising number of children living with complex chronic conditions. Canadian Medical Association Journal, 186(16), 1199–1200. https://doi.org/10.1503/cmaj.141036
Male, L., Noble, A., Atkinson, J., & Marson, T. (2017). Measuring patient experience: A systematic review to evaluate psychometric properties of patient reported experience measures (PREMs) for emergency care service provision. International Journal for Quality in Health Care: Journal of the International Society for Quality in Health Care, 29(3), 314–326. https://doi.org/10.1093/intqhc/mzx027
Allard, A., Fellowes, A., Shilling, V., Janssens, A., Beresford, B., & Morris, C. (2014). Key health outcomes for children and young people with neurodisability: Qualitative research with young people and parents. British Medical Journal Open, 4, 1–11. https://doi.org/10.1136/bmjopen-2013-004611
Morris, C., Janssens, A., Shilling, V., Allard, A., Fellowes, A., Tomlinson, R., et al. (2015). Meaningful health outcomes for paediatric neurodisability: Stakeholder prioritisation and appropriateness of patient reported outcome measures. Health and Quality of Life Outcomes, 13, 87. https://doi.org/10.1186/s12955-015-0284-7
Bevans, K. B., Moon, J., Becker, B. D., Carle, A., & Forrest, C. B. (2020). Development of patient-reported outcome measures of children’s oral health aesthetics. Community Dentistry and Oral Epidemiology, 48(5), 423–432. https://doi.org/10.1111/cdoe.12555
Sinha, I., Jones, L., Smyth, R. L., & Williamson, P. R. (2008). A systematic review of studies that aim to determine which outcomes to measure in clinical trials in children. PLoS Medicine, 5(4), e96. https://doi.org/10.1371/journal.pmed.0050096
Edbrooke-childs, J., Wolpert, M., & Deighton, J. (2016). Using patient reported outcome measures to improve service effectiveness (UPROMISE): Training clinicians to use outcome measures in child mental health. Administration and Policy in Mental Health and Mental Health Services Research, 43(3), 302–308. https://doi.org/10.1007/s10488-014-0600-2
Fayed, N., de Camargo, O. K., Elahi, I., Dubey, A., Fernandes, R. M., Houtrow, A., et al. (2014). Patient-important activity and participation outcomes in clinical trials involving children with chronic conditions. Quality of Life Research, 23(3), 751–757. https://doi.org/10.1007/s11136-013-0483-9
Jain, P., Smith, M. L., Speechley, K., Ferro, M., Connolly, M., Ramachandrannair, R., et al. (2020). Seizure freedom improves health-related quality of life after epilepsy surgery in children. Developmental Medicine & Child Neurology, 62(5), 600–608.
Fortunato, J. E., Troy, A. L., Cuffari, C., Davis, J. E., Loza, M. J., Oliva-Hemker, M., et al. (2010). Outcome after percutaneous endoscopic gastrostomy in children and young adults. Journal of Pediatric Gastroenterology and Nutrition, 50(4), 390–393.
Mahant, S., Friedman, J. N., Connolly, B., Goia, C., & Macarthur, C. (2009). Tube feeding and quality of life in children with severe neurological impairment. Archives of Disease in Childhood, 94(9), 668–673.
Nelson, K. E., Rosella, L. C., Mahant, S., Cohen, E., & Guttmann, A. (2019). Survival and health care use after feeding tube placement in children with neurologic impairment. Pediatrics, 143(2), e20182863.
Roth, J., Carlson, C., Devinsky, O., Harter, D. H., MacAllister, W. S., & Weiner, H. L. (2014). Safety of staged epilepsy surgery in children. Neurosurgery, 74(2), 154–162. https://doi.org/10.1227/NEU.0000000000000231
Marshall, S., Haywood, K., & Fitzpatrick, R. (2006). Impact of patient-reported outcome measures on routine practice: A structured review. Journal of Evaluation in Clinical Practice, 12(5), 559–568. https://doi.org/10.1111/j.1365-2753.2006.00650.x
Stover, A. M., Haverman, L., van Oers, H. A., Greenhalgh, J., Potter, C. M., Ahmed, S., et al. (2020). Using an implementation science approach to implement and evaluate patient-reported outcome measures (PROM) initiatives in routine care settings. Quality of Life Research. https://doi.org/10.1007/s11136-020-02564-9
Fayed, N., Gardecki, M., & Cohen, E. (2018). Partnering with families of children with medical complexity to evaluate interventions. Canadian Medical Association Journal. https://doi.org/10.1503/cmaj.180372
Janvier, A., Farlow, B., Baardsnes, J., Pearce, R., & Barrington, K. J. (2016). Measuring and communicating meaningful outcomes in neonatology: A family perspective. In Seminars in perinatology (Vol. 40, No. 8, pp. 571–577). Philadelphia: WB Saunders.
Fayed, N. (2011). Content issues in child health status and quality of life instruments: Addressing the challenges with new methods (Doctoral dissertation).
Rosenbaum, P. L., Livingston, M. H., Palisano, R. J., Galuppi, B. E., & Russell, D. J. (2007). Quality of life and health-related quality of life of adolescents with cerebral palsy. Developmental Medicine & Child Neurology, 49(7), 516–521.
Raphael, D., Brown, I., Renwick, R., & Rootman, I. (1996). Assessing the quality of life of persons with developmental disabilities: Description of a new model, measuring instruments, and initial findings. International Journal of Disability, Development and Education, 43(1), 25–42. https://doi.org/10.1080/0156655960430103
Crudgington, H., Collingwood, A., Bray, L., Lyle, S., Martin, R., Gringras, P., et al. (2020). Map** epilepsy-specific patient-reported outcome measures for children to a proposed core outcome set for childhood epilepsy. Epilepsy & Behavior, 112, 107372.
Morris, C., Simkiss, D., Busk, M., Morris, M., Allard, A., Denness, J., et al. (2015). Setting research priorities to improve the health of children and young people with neurodisability: A British Academy of Childhood Disability-James Lind Alliance Research Priority Setting Partnership. British Medical Journal Open, 5(1), e006233. https://doi.org/10.1136/bmjopen-2014-006233
U.S. Department of Health and Human Services Food and Drug Administration. (2009). Guidance for industry patient-reported outcome measures: Use in medical product development to support labeling claims. Rockville: U.S. Department of Health and Human Services Food and Drug Administration.
European Medicines Agency. (2005). Regulatory guidance for the use of health-related quality of life (Hrql) measures in the evaluation of medicinal products reproduction. Amsterdam: European Medicines Agency.
International Association for Public Participation. (2004). Public participation spectrum. Retrieved September 2018 from https://iap2canada.ca/Resources/Documents/0702-Foundations-Spectrum-MW-rev2%20(1).pdf.
Frank, L., Forsythe, L., Ellis, L., Schrandt, S., Sheridan, S., Gerson, J., et al. (2015). Conceptual and practical foundations of patient engagement in research at the patient-centered outcomes research institute. Quality of Life Research, 24(5), 1033–1041.
Esposito, D., Heeringa, J., Bradley, K., Croake, S., & Kimmey, L. (2015). PCORI dissemination and implementation framework. MATHEMATICA Policy Research. Washington, DC, US. Retrieved from http://pcori.org/sites/default/files/PCORI-Dissemination-Implementation-Framework.pdf.
Frank, L., Basch, E., & Selby, J. (2014). Viewpoint: The PCORI perspective on patient-centered outcomes research. Journal of the American Medical Association, 312(15), 1513–1514.
Moher D, Liberati A, Tetzlaff J, Altman DG, The PRISMA Group. (2009). Preferred reporting items for systematic reviews and meta-analyses: The PRISMA Statement. PLoS Medicine, 6(7), e1000097. https://doi.org/10.1371/journal.pmed.1000097
Covidence. (2020). Retrieved September 2018 from, https://www.covidence.org/about-us/.
Arbuckle, R., Abetz, L., Durmer, J. S., Ivanenko, A., Owens, J. A., Croenlein, J., et al. (2010). Development of the Pediatric Restless Legs Syndrome Severity Scale (P-RLS-SS): A patient-reported outcome measure of pediatric RLS symptoms and impact. Sleep Medicine, 11(9), 897–906. https://doi.org/10.1016/j.sleep.2010.03.016
Basra, M. K. A., Salek, M. S., Fenech, D., & Finlay, A. Y. (2018). Conceptualization, development and validation of T-QoL© (Teenagers’ Quality of Life): A patient-focused measure to assess quality of life of adolescents with skin diseases. The British Journal of Dermatology, 178(1), 161–175. https://doi.org/10.1111/bjd.15853
Bemister, T. B., Brooks, B. L., & Kirton, A. (2014). Development, reliability, and validity of the Alberta Perinatal Stroke Project Parental Outcome Measure. Pediatric Neurology, 51(1), 43–52. https://doi.org/10.1016/j.pediatrneurol.2014.01.052
Bevans, K. B., Gardner, W., Pajer, K., Riley, A. W., & Forrest, C. B. (2013). Qualitative development of the PROMIS(R) pediatric stress response item banks. Journal of Pediatric Psychology, 38(2), 173–191. https://doi.org/10.1093/jpepsy/jss107
Bramhagen, A.-C., Eriksson, M., Ericsson, E., Nilsson, U., Harden, S., & Idvall, E. (2016). Self-reported post-operative recovery in children: Development of an instrument. Journal of Evaluation in Clinical Practice, 22(2), 180–188. https://doi.org/10.1111/jep.12451
Caty, G., Gilles, C., Arnould, C., Thonnard, J. L., & Lejuene, T. (2008). ABILOCO-Kids: A Rasch-built 10-item questionnaire for assessing locomotion ability in children with cerebral palsy. Journal of Rehabilitation Medicine, 40(10), 823–830.
Chang, K. W., Austin, A., Yeaman, J., Phillips, L., Kratz, A., Yang, L., et al. (2017). Health-related quality of life components in children with neonatal brachial plexus palsy: A qualitative study. PM&R, 9(4), 383–391.
Chien, C.-W., Rodger, S., & Copley, J. (2015). Development and psychometric evaluation of a new measure for children’s participation in hand-use life situations. Archives of Physical Medicine and Rehabilitation, 96(6), 1045–1055. https://doi.org/10.1016/j.apmr.2014.11.013
de Kleuver, M., Faraj, S., Holewijn, R. M., Germscheid, N. M., Adobor, R. D., Andersen, M., et al. (2017). Defining a core outcome set for adolescent and young adult patients with a spinal deformity. Acta Orthopaedica, 88(6), 612–618. https://doi.org/10.1080/17453674.2017.1371371
Dickin, K. L., Lent, M., Lu, A. H., Sequeira, J., & Dollahite, J. S. (2012). Develo** a measure of behavior change in a program to help low-income parents prevent unhealthful weight gain in children. Journal of Nutrition Education and Behavior, 44(1), 12–21. https://doi.org/10.1016/j.jneb.2011.02.015
Doi, T., Inoue, H., Arai, Y., Shirado, O., Doi, T., Yamazaki, K., et al. (2018). Reliability and validity of a novel quality of life questionnaire for female patients with adolescent idiopathic scoliosis: Scoliosis Japanese Questionnaire-27: A multicenter, cross-sectional study. BMC Musculoskeletal Disorders, 19(1), 99. https://doi.org/10.1186/s12891-018-2025-7
Dyson, M. P., Shave, K., Gates, A., Fernandes, R. M., Scott, S. D., & Hartling, L. (2017). Which outcomes are important to patients and families who have experienced paediatric acute respiratory illness? Findings from a mixed methods sequential exploratory study. British Medical Journal Open, 7(12), e018199. https://doi.org/10.1136/bmjopen-2017-018199
Eapen, V., Crncec, R., Walter, A., & Tay, K. P. (2014). Conceptualisation and development of a quality of life measure for parents of children with autism spectrum disorder. Autism Research and Treatment, 2014(101576459), 160783. https://doi.org/10.1155/2014/160783
Fabricant, P. D., Robles, A., Downey-Zayas, T., Do, H. T., Marx, R. G., Widmann, R. F., et al. (2013). Development and validation of a pediatric sports activity rating scale: The Hospital for Special Surgery Pediatric Functional Activity Brief Scale (HSS Pedi-FABS). The American Journal of Sports Medicine, 41(10), 2421–2429. https://doi.org/10.1177/0363546513496548
Fiume, A., Deveber, G., Jang, S.-H., Fuller, C., Viner, S., & Friefeld, S. (2018). Development and validation of the Pediatric Stroke Quality of Life Measure. Developmental Medicine and Child Neurology, 60(6), 587–595. https://doi.org/10.1111/dmcn.13684
Franciosi, J. P., Hommel, K. A., DeBrosse, C. W., Greenberg, A. B., Greenler, A. J., Abonia, J. P., et al. (2012). Quality of life in paediatric eosinophilic oesophagitis: What is important to patients? Child: Care Health and Development, 38(4), 477–483. https://doi.org/10.1111/j.1365-2214.2011.01265.x
Geister, T. L., Quintanar-Solares, M., Martin, M., Aufhammer, S., & Asmus, F. (2014). Qualitative development of the “Questionnaire on Pain caused by Spasticity (QPS)”, a pediatric patient-reported outcome for spasticity-related pain in cerebral palsy. Quality of Life Research: An International Journal of Quality of Life Aspects of Treatment, Care and Rehabilitation, 23(3), 887–896. https://doi.org/10.1007/s11136-013-0526-2
Gore, C., Griffin, R., Rothenberg, T., Tallett, A., Hopwood, B., Sizmur, S., et al. (2016). New patient-reported experience measure for children with allergic disease: Development, validation and results from integrated care. Archives of Disease in Childhood, 101(10), 935–943. https://doi.org/10.1136/archdischild-2015-309598
Heyworth, B., Cohen, L., von Heideken, J., Kocher, M. S., & Iversen, M. D. (2018). Validity and comprehensibility of outcome measures in children with shoulder and elbow disorders: Creation of a new Pediatric and Adolescent Shoulder and Elbow Survey (Pedi-ASES). Journal of Shoulder and Elbow Surgery, 27(7), 1162–1171. https://doi.org/10.1016/j.jse.2017.11.009
Klingels, K., Mayhew, A. G., Mazzone, E. S., Duong, T., Decostre, V., Werlauff, U., et al. (2017). Development of a patient-reported outcome measure for upper limb function in Duchenne muscular dystrophy: DMD Upper Limb PROM. Developmental Medicine and Child Neurology, 59(2), 224–231. https://doi.org/10.1111/dmcn.13277
Kramer, J. M., & Schwartz, A. E. (2018). Development of the Pediatric Disability Inventory-Patient Reported Outcome (PEDI-PRO) measurement conceptual framework and item candidates. Scandinavian Journal of Occupational Therapy, 25(5), 335–346. https://doi.org/10.1080/11038128.2018.1502344
Liu, H., Hays, R. D., Marcus, M., et al. (2016). Patient-reported oral health outcome measurement for children and adolescents. BMC Oral Health, 16, 95.
Morris, C., Dunkley, C., Gibbon, F. M., Currier, J., Roberts, D., Rogers, M., et al. (2017). Core health outcomes in childhood epilepsy (CHOICE): Protocol for the selection of a core outcome set. Trials, 18(1), 572. https://doi.org/10.1186/s13063-017-2323-7
Newcombe, P. A., Sheffield, J. K., Petsky, H. L., Marchant, J. M., Willis, C., & Chang, A. B. (2016). A child chronic cough-specific quality of life measure: Development and validation. Thorax, 71(8), 695–700. https://doi.org/10.1136/thoraxjnl-2015-207473
Oluboyede, Y., Hulme, C., & Hill, A. (2017). Development and refinement of the WAItE: A new obesity-specific quality of life measure for adolescents. Quality of Life Research: An International Journal of Quality of Life Aspects of Treatment, Care and Rehabilitation, 26(8), 2025–2039. https://doi.org/10.1007/s11136-017-1561-1
O’Sullivan, E. J., & Rasmussen, K. M. (2017). Development, construct validity, and reliability of the questionnaire on infant feeding: A tool for measuring contemporary infant-feeding behaviors. Journal of the Academy of Nutrition and Dietetics, 117(12), 1983-1990.e1984. https://doi.org/10.1016/j.jand.2017.05.006
Punpanich, W., Hays, R. D., Detels, R., Chokephaibulkit, K., Chantbuddhiwet, U., Leowsrisook, P., et al. (2011). Development of a culturally appropriate health-related quality of life measure for human immunodeficiency virus-infected children in Thailand. Journal of Paediatrics and Child Health, 47(1–2), 27–33. https://doi.org/10.1111/j.1440-1754.2010.01886.x
Roorda, L. D., Scholtes, V. A., van der Lee, J. H., Becher, J., & Dallmeijer, A. J. (2010). Measuring mobility limitations in children with cerebral palsy: Development, scalability, unidimensionality, and internal consistency of the mobility questionnaire, MobQues47. Archives of Physical Medicine and Rehabilitation, 91(8), 1194–1209. https://doi.org/10.1016/j.apmr.2010.05.009
Santucci, N. R., Hyman, P. E., Karpinski, A., Rosenberg, A., Garguilo, D., Rein, L. E., et al. (2018). Development and validation of a childhood self-efficacy for functional constipation questionnaire. Neurogastroenterology and Motility, 30(3), e13222.
Shaikh, N., Martin, J. M., Casey, J. R., Pichichero, M. E., Wald, E. R., Colborn, D. K., et al. (2009). Development of a patient-reported outcome measure for children with streptococcal pharyngitis. Pediatrics, 124(4), e557-563. https://doi.org/10.1542/peds.2009-0331
Tadic, V., Cooper, A., Cumberland, P., Lewando-Hundt, G., Rahi, J. S., & Vision-related Quality of Life Group. (2013). Development of the functional vision questionnaire for children and young people with visual impairment: The FVQ_CYP. Ophthalmology, 120(12), 2725–2732. https://doi.org/10.1016/j.ophtha.2013.07.055
Tsakos, G., Blair, Y., Yusuf, H., Wright, W., Watt, R., & Macpherson, L. (2012). Develo** a new self-reported scale of oral health outcomes for 5-year-old children (SOHO-5). Health and Quality of Life Outcomes, 10, 62.
Verschuren, O., Ketelaar, M., Keefer, D., Wright, V., Butler, J., Ada, L., et al. (2011). Identification of a core set of exercise tests for children and adolescents with cerebral palsy: A Delphi survey of researchers and clinicians. Developmental Medicine and Child Neurology, 53(5), 449–456. https://doi.org/10.1111/j.1469-8749.2010.03899.x
Wray, J., Hobden, S., Knibbs, S., & Oldham, G. (2018). Hearing the voices of children and young people to develop and test a patient-reported experience measure in a specialist paediatric setting. Archives of Disease in Childhood, 103(3), 272–279. https://doi.org/10.1136/archdischild-2017-313032
Wright, W. G., Spiro, A., 3rd., Jones, J. A., Rich, S. E., & Garcia, R. I. (2017). Development of the teen oral health-related quality of life instrument. Journal of Public Health Dentistry, 77(2), 115–124. https://doi.org/10.1111/jphd.12181
Varni, J. W., Seid, M., & Rode, C. A. (1999). The PedsQL™: Measurement model for the pediatric quality of life inventory. Medical Care, 37, 126–139.
Landgraf, J. M., Abetz, L., & Ware, J. E. (1999). Child health questionnaire (CHQ): A user’s manual. Boston, MA: Landgraf & Ware.
Berry, J. G., Graham, D. A., Graham, R. J., Zhou, J., Putney, H. L., O’Brien, J. E., et al. (2009). Predictors of clinical outcomes and hospital resource use of children after tracheotomy. Pediatrics, 124(2), 563–572.
Eapen, V., Črnčec, R., & Walter, A. (2013). Clinical outcomes of an early intervention program for preschool children with Autism Spectrum Disorder in a community group setting. BMC Pediatrics. https://doi.org/10.1186/1471-2431-13-3
Wilkinson, J. D., Lowe, A. M., Salbert, B. A., Sleeper, L. A., Colan, S. D., Cox, G. F., et al. (2012). Outcomes in children with Noonan syndrome and hypertrophic cardiomyopathy: A study from the Pediatric Cardiomyopathy Registry. American Heart Journal, 164(3), 442–448.
Biederman, J., Monuteaux, M. C., Doyle, A. E., Seidman, L. J., Wilens, T. E., Ferrero, F., et al. (2004). Impact of executive function deficits and attention-deficit/hyperactivity disorder (ADHD) on academic outcomes in children. Journal of Consulting and Clinical Psychology, 72(5), 757–766. https://doi.org/10.1037/0022-006X.72.5.757
Langley, K., Fowler, T., Ford, T., Thapar, A. K., Van Den Bree, M., Harold, G., et al. (2010). Adolescent clinical outcomes for young people with attention-deficit hyperactivity disorder. The British Journal of Psychiatry, 196(3), 235–240.
Wiering, B., de Boer, D., & Delnoij, D. (2017). Patient involvement in the development of patient-reported outcome measures: The developers’ perspective. BMC Health Services Research, 17(1), 635. https://doi.org/10.1186/s12913-017-2582-8
Mader, L. B., Harris, T., Kläger, S., Wilkinson, I. B., & Hiemstra, T. F. (2018). Inverting the patient involvement paradigm: Defining patient led research. Research Involvement and Engagement, 4(1), 21. https://doi.org/10.1186/s40900-018-0104-4
El-Damanawi, R., Lee, M., Harris, T., Mader, L. B., Bond, S., Pavey, H., et al. (2018). Randomised controlled trial of high versus ad libitum water intake in patients with autosomal dominant polycystic kidney disease: Rationale and design of the DRINK feasibility trial. British Medical Journal Open, 8(5), e022859. https://doi.org/10.1136/bmjopen-2018-022859
Acknowledgements
The author would like to thank Sandra McKeown for her knowledge and insight on creating database search strategies.
Funding
The research was funded through the Ontario Child Health Support Unit through OSSU (the Ontario SPOR [Strategy for Patient-Oriented Research] SUPPORT [Support for People and Patient-Oriented Research and Trials] Unit).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There are no conflicts of interest or competing interests to report.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
McNeill, M., Noyek, S., Engeda, E. et al. Assessing the engagement of children and families in selecting patient-reported outcomes (PROs) and develo** their measures: a systematic review. Qual Life Res 30, 983–995 (2021). https://doi.org/10.1007/s11136-020-02690-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-020-02690-4