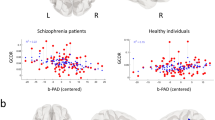
The aim of the present study was, within the framework of the concept of “clinical high risk for psychosis,” to identify functional characteristics of the brain (based on resting-state fMRI data) and neuropsychological characteristics in 27 patients with non-psychotic mental disorders, with attenuated schizophrenia symptoms which had not converted during a long observation period, as compared with 24 patients with first-episode schizophrenia, and 27 mentally healthy subjects. The main group was characterized by higher levels pf BOLD coherence in the visual cortex of the right hemisphere and higher functional connectivity between the occipital component of the visual network and a salience network component in the right prefrontal cortex (as compared with schizophrenia patients). Both groups of patients showed decreased productivity in verbal fluency tests. The neuroimaging and neuropsychological peculiarities of patients in the main group identified here can be regarded as reflecting an impact of “protective” and “pathological” mechanisms in patients at high risk for schizophrenia.
Similar content being viewed by others
References
Adamek, P., Langova, V., and Horacek, J., “Early-stage visual perception impairment in schizophrenia, bottom-up and back again,” Schizophrenia (Heidelb.), 8, No. 1, 27 (2022), https://doi.org/10.1038/s41537-022-00237-9.
Addington, J., Farris, M., Stowkowy, J., et al., “Predictors of transition to psychosis in individuals at clinical high risk,” Curr. Psychiatry Rep., 21, No. 6, 39 (2019), https://doi.org/10.1007/s11920-019-1027-y.
Addington, J., Piskulic, D., Liu, L., et al., “Comorbid diagnoses for youth at clinical high risk of psychosis,” Schizophr. Res., 190, 90–95 (2017), https://doi.org/https://doi.org/10.1016/j.schres.2017.03.043.
Aita, S. L., Beach, J. D., Taylor, S. E., et al., “Executive, language, or both? An examination of the construct validity of verbal fluency measures,” Appl. Neuropsychol. Adult, 26, No. 5, 441–451 (2019), https://doi.org/https://doi.org/10.1080/23279095.2018.1439830.
Akhutina, T. V. (ed.) Methods for Neuropsychological Investigation of Children Aged 6–9 Years, V. Sekachev, Moscow (2016).
Andreou, C. and Borgwardt, S., “Structural and functional imaging markers for susceptibility to psychosis,” Mol. Psychiatry, 25, No. 11, 2773–2785 (2020), https://doi.org/https://doi.org/10.1038/s41380-020-0679-7.
Anticevic, A., Haut, K., Murray, J. D., et al., “Association of thalamic dysconnectivity and conversion to psychosis in youth and young adults at elevated clinical risk,” JAMA Psychiatry, 72, No. 9, 882–891 (2015), https://doi.org/https://doi.org/10.1001/jamapsychiatry.2015.0566.
Bolt, L. K., Amminger, G. P., Farhall, J., et al., “Neurocognition as a predictor of transition to psychotic disorder and functional outcomes in ultra-high risk participants: Findings from the NEURAPRO randomized clinical trial,” Schizophr. Res., 206, 67–74 (2019), https://doi.org/https://doi.org/10.1016/j.schres.2018.12.013.
Bosanac, P. and Castle, D. J., “Schizophrenia and depression,” Med. J. Aust., 199, No. S6, S36–39 (2013), https://doi.org/https://doi.org/10.5694/mja12.10516.
Cao, H., Chen, O. Y., Chung, Y., et al., “Cerebello-thalamo-cortical hyperconnectivity as a state-independent functional neural signature for psychosis prediction and characterization,” Nat. Commun., 9, No. 1, 3836 (2018), https://doi.org/10.1038/s41467-018-06350-7.
Catalan, A., Salazar de Pablo, G., Aymerich, C., et al., “Neurocognitive functioning in individuals at clinical high risk for psychosis: A systematic review and meta-analysis,” JAMA Psychiatry, (2021), https://doi.org/10.1001/jamapsychiatry.2021.1290.
Chai, X. J., Castanon, A. N., Ongur, D., and Whitfield-Gabrieli, S., “Anticorrelations in resting state networks without global signal regression,” NeuroImage, 59, No. 2, 1420–1428 (2012), https://doi.org/https://doi.org/10.1016/j.neuroimage.2011.08.048.
Chechko, N., Cieslik, E. C., Muller, V. I., et al., “Differential resting-state connectivity patterns of the right anterior and posterior dorsolateral prefrontal cortices (DLPFC) in schizophrenia,” Front. Psychiatry, 9, 211 (2018), https://doi.org/https://doi.org/10.3389/fpsyt.2018.00211.
Collin, G., Seidman, L. J., Keshavan, M. S., et al., “Functional connectome organization predicts conversion to psychosis in clinical high-risk youth from the SHARP program,” Mol. Psychiatry, 25, No. 10, 2431–2440 (2020), https://doi.org/https://doi.org/10.1038/s41380-018-0288-x.
Delis, D. C., Kaplan, E., and Kramer, J. H., Delis-Kaplan Executive Function System: Examiner’s Manual, The Psychological Corporation, San Antonio, TX (2001).
Ellis, J. K., Walker, E. F., and Goldsmith, D. R., “Selective review of neuroimaging findings in youth at clinical high risk for psychosis: On the path to biomarkers for conversion,” Front. Psychiatry, 11, 567534 (2020), https://doi.org/https://doi.org/10.3389/fpsyt.2020.567534.
Filimonenko, Yu. I. and Timofeev, V. I., Handbook for Investigations of Intelligence in Adults using the D. Wechsler Scale (WAIS), IMATON, St. Petersburg (1995).
Gottesman, I. I. and Gould, T. D., “The endophenotype concept in psychiatry: etymology and strategic intentions,” Am. J. Psychiatry, 160, No. 4, 636–645 (2003), https://doi.org/https://doi.org/10.1176/appi.ajp.160.4.636.
Grill-Spector, K. and Malach, R., “The human visual cortex,” Annu. Rev. Neurosci., 27, 649–677 (2004), https://doi.org/https://doi.org/10.1146/annurev.neuro.27.0702-03.144220.
Gustavson, D. E., Panizzon, M. S., Franz, C. E., et al., “Integrating verbal fluency with executive functions: Evidence from twin studies in adolescence and middle age,” J. Exp. Psychol. Gen., 148, No. 12, 2104–2119 (2019), https://doi.org/https://doi.org/10.1037/xge0000589.
Hafner, H., “From onset and prodromal stage to a life-long course of schizophrenia and its symptom dimensions: How sex, age, and other risk factors influence incidence and course of illness,” Psychiatry J., 2019, 9804836 (2019), https://doi.org/https://doi.org/10.1155/2019/9804836.
Hamilton, M., “A rating scale for depression,” J. Neurol. Neurosurg., 23, 56–62 (1960), https://doi.org/https://doi.org/10.1136/jnnp.23.1.56.
Hedges, E. P., Dickson, H., Tognin, S., et al., “Verbal memory performance predicts remission and functional outcome in people at clinical high-risk for psychosis,” Schizophr. Res. Cogn., 28, 100222 (2022), https://doi.org/https://doi.org/10.1016/j.scog.2021.100222.
Kapur, S., “Psychosis as a state of aberrant salience: a framework linking biology, phenomenology, and pharmacology in schizophrenia,” Am. J. Psychiatry, 160, No. 1, 13–23 (2003), https://doi.org/https://doi.org/10.1176/appi.ajp.160.1.13.
Kay, S. R., Fiszbein, A., and Opler, L. A., “The positive and negative syndrome scale (PANSS) for schizophrenia,” Schizophr. Bull., 13, No. 2, 261–276 (1987), https://doi.org/https://doi.org/10.1093/schbul/13.2.261.
Keri, S. and Benedek, G., “Visual contrast sensitivity alterations in inferred magnocellular pathways and anomalous perceptual experiences in people at high-risk for psychosis,” Vis. Neurosci., 24, No. 2, 183–189 (2007), https://doi.org/https://doi.org/10.1017/S0952523807070253.
Kim, D., Kim, J. W., Koo, T. H., et al., “Shared and distinct neurocognitive endophenotypes of schizophrenia and psychotic bipolar disorder,” Clin. Psychopharmacol. Neurosci., 13, No. 1, 94–102 (2015), https://doi.org/https://doi.org/10.9758/cpn.2015.13.1.94.
Kronke, K. M., Wolff, M., Shi, Y., et al., “Functional connectivity in a triple-network saliency model is associated with real-life self-control,” Neuropsychologia, 149, 107667 (2020), https://doi.org/https://doi.org/10.1016/j.neuropsychologia.2020.-107667.
Liang, S., Deng, W., Wang, Q., et al., “Performance of verbal fluency as an endophenotype in patients with familial versus sporadic schizophrenia and their parents,” Sci. Rep., 6, 32597 (2016), https://doi.org/https://doi.org/10.1038/srep32597.
Lombardo, M. V., Pramparo, T., Gazestani, V., et al., “Large-scale associations between the leukocyte transcriptome and BOLD responses to speech differ in autism early language outcome subtypes,” Nat. Neurosci., 21, No. 12, 1680–1688 (2018), https://doi.org/https://doi.org/10.1038/s41593-018-0281-3.
Miller, T. J., McGlashan, T. H., Woods, S. W., et al., “Symptom assessment in schizophrenic prodromal states,” Psychiatr Q., 70, No. 4, 273–287 (1999), https://doi.org/https://doi.org/10.1023/a:1022034115078.
Montchal, M. E., Reagh, Z. M., and Yassa, M. A., “Precise temporal memories are supported by the lateral entorhinal cortex in humans,” Nat. Neurosci., 22, No. 2, 284–288 (2019), https://doi.org/https://doi.org/10.1038/s41593-018-0303-1.
Morosini, P. L., Magliano, L., Brambilla, L., et al., “Development, reliability and acceptability of a new version of the DSM-IV Social and Occupational Functioning Assessment Scale (SOFAS) to assess routine social funtioning,” Acta Psychiatr. Scand., 101, No. 4, 323–329 (2000), https://doi.org/https://doi.org/10.1034/j.1600-0447.2000.10100-4323x.
Murphy, K., Birn, R. M., Handwerker, D. A., et al., “The impact of global signal regression on resting state correlations: are anti-correlated networks introduced?” NeuroImage, 44, No. 3, 893–905 (2009), https://doi.org/https://doi.org/10.1016/j.neuroimage.2008.09.036.
Newton, R., Rouleau, A., et al., “Diverse definitions of the early course of schizophrenia-a targeted literature review,” NPJ Schizophr., 4, No. 1, 21 (2018), https://doi.org/10.1038/s41537-018-0063-7.
Omelchenko, M. A., “Clinical prerequisites for a high risk of develo** endogenous psychosis: issues of diagnosis and therapy,” Psikhiatriya, 18, No. 2, 82–91 (2020), https://doi.org/10.30629/2618-6667-2020-18-2-82-91.
Panikratova, Y. R., Vlasova, R. M., Akhutina, T. V., et al., “Functional connectivity of the dorsolateral prefrontal cortex contributes to different components of executive functions,” Int. J. Psychophysiol., 151, 70–79 (2020), https://doi.org/https://doi.org/10.1016/j.ijpsycho.2020.02.013.
Patel, K. R., Cherian, J., Gohil, K., and Atkinson, D., “Schizophrenia: Overview and treatment options,” Pharm. Ther., 39, No. 9, 638–645 (2014).
Riecher-Rossler, A., Pflueger, M. O., Aston, J., et al., “Efficacy of using cognitive status in predicting psychosis: a 7-year follow-up,” Biol. Psychiatry, 66, No. 11, 1023–1030 (2009), https://doi.org/https://doi.org/10.1016/j.biopsych.2009.07.020.
Shao, Z., Janse, E., Visser, K., and Meyer, A. S., “What do verbal fluency tasks measure? Predictors of verbal fluency performance in older adults,” Front. Psychol., 5, 772 (2014), https://doi.org/https://doi.org/10.3389/fpsyg.2014.00772.
Smieskova, R., Fusar-Poli, P., Riecher-Rossler, A., and Borgwardt, S., “Neuroimaging and resilience factors–staging of the at-risk mental state?” Curr. Pharm. Des., 18, No. 4, 416–421 (2012), https://doi.org/https://doi.org/10.2174/138161212799316046.
van der Werf, M., Hanssen, M., Kohler, S., et al., “Systematic review and collaborative recalculation of 133,693 incident cases of schizophrenia,” Psychol. Med., 44, No. 1, 9–16 (2014), https://doi.org/https://doi.org/10.1017/S0033291712002796.
van Os, J. and Guloksuz, S., “A critique of the “ultra-high risk” and “transition” paradigm,” World Psychiatry, 16, No. 2, 200–206 (2017), https://doi.org/https://doi.org/10.1002/wps.20423.
Wang, C., Lee, J., Ho, N. F., et al., “Large-scale network topology reveals heterogeneity in individuals with at risk mental state for psychosis: findings from the Longitudinal Youth-at-Risk Study,” Cereb. Cortex, 28, No. 12, 4234–4243 (2018), https://doi.org/https://doi.org/10.1093/cercor/bhx278.
Wang, L., Mruczek, R. E., Arcaro, M. J., and Kastner, S., “Probabilistic maps of visual topography in human cortex,” Cereb. Cortex, 25, No. 10, 3911–3931 (2015), https://doi.org/https://doi.org/10.1093/cercor/bhu277.
Williams, D., “Hierarchical Bayesian models of delusion,” Conscious. Cogn., 61, 129–147 (2018), https://doi.org/https://doi.org/10.1016/j.concog.2018.03.003.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lebedeva, I.S., Panikratova, Y.R., Abdullina, E.G. et al. Neuroimaging (Resting-State fMRI) and Neuropsychological Characteristics of Non-Converted Patients from a Group at Clinical High Risk for Schizophrenia. Neurosci Behav Physi 53, 1449–1458 (2023). https://doi.org/10.1007/s11055-023-01538-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11055-023-01538-x