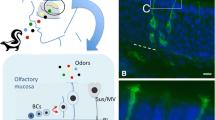
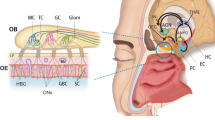
This article analyzes published data and shows that the functioning of the olfactory system is impaired in schizophrenia. Structural and functional anomalies extend from the cortex to the peripheral apparatus of the olfactory sensory system. As the olfactory sensory system is anatomically the most tightly linked with the temporal-limbic and frontal lobes, which are the most involved in schizophrenia and underlie the social, emotional, and cognitive anomalies in this pathology, studies of olfaction may provide a suitable tool for assessing the structural and functional integrity of these pathomorphological neural substrates. Because of this link, olfactory dysfunction can be used as a sensitive indicator both for the early diagnosis of schizophrenia and for differential diagnosis, especially in people with high genetic risk of illness. The relationship between one of the leading pathogenetic components of schizophrenia – a defect in postanal neurogenesis – with formation of anomalies in the olfactory system is of particular interest. Studies of schizophrenia have in recent years started to use biopsies of the olfactory neuroepithelium, allowing the molecular mechanisms of the pathogenesis the disease to be observed in model cultures. Thus, the olfactory neuroepithelium can be used as a model not only facilitating identification of preclinical biomarkers but also linking them with the specific mechanisms of the disease.
Similar content being viewed by others
References
V. E. Golimbet, A. I. Kryukov, G. P. Kostyuk, et al., “The olfactory neuroepithelium as a model for studies of the molecular mechanisms of schizophrenia,” Zh. Nevrol. Psikhiat., No. 6, 111–114.
B. Atanasova et al., “Olfaction: a potential cognitive marker of psychiatric disorders,” Neurosci. Biobehav. Rev., 32, No. 7, 1315–25 (2008).
D. N. Abrous, M. Koehl, and M. Le Moal, “Adult neurogenesis, from precursors to network and physiology,” Physiol. Rev., 85, No. 2, 523–69 (2005).
A. K. Anderson et al., “Dissociated neural representations of intensity and valence in human olfaction,” Nat. Neurosci., 6, 196–202 (2003).
S. E. Arnold and L. Rioux, “Challenges, status, and opportunities for studying developmental neuropathology in adult schizophrenia,” Schizophr. Bull., 27, No. 3, 395–416 (2001).
S. E. Arnold et al., “Dysregulation of olfactory receptor neuron lineage in schizophrenia,” Arch. Gen. Psychiatry, 58, No. 9, 829–35 (2001).
K. E. Borgmann-Winter et al., “Altered G protein coupling in olfactory neuroepithelial cells from patients with schizophrenia,” Schizophr. Bull., 42, No. 2, 377–85 (2016).
J. Bossy, “Development of olfactory and related structures in staged human embryos,” Anat. Embryol. (Berl.), 161, No. 2, 225–36 (1980).
W. J. Brewer et al., “Impairment of olfactory identification ability in individuals at ultra-high risk for psychosis who later develop schizophrenia,” Am. J. Psychiatry, 160, No. 10, 1790–4 (2003).
T. W. Buchanan, D. Tranel, and R. Adolphs, “A specific role for the human amygdala in olfactory memory,” Learn. Mem., 10, No. 5, 319–25 (2003).
T. M. Cabrera-Vera et al., “Insights into G protein structure, function and regulation,” Endocrine Rev., 24, No. 5, 765–781 (2003).
J. G. Chi, E. C. Dooling, and F. H. Gilles, “Gyral development of the human brain,” Ann. Neurol., 1, 86–93 (1977).
C. Corcoran et al., “Olfactory deficits, cognition and negative symptoms in early onset psychosis,” Schizophr. Res., 80, No. 1, 95–106 (2005).
E. Courtiol and D. A. Wilson, “Thalamic olfaction, characterizing odor processing in the mediodorsal thalamus of the rat,” J. Neurophysiol., 111, No. 6, 1274–85 (2014).
B. Crespo-Facorroa et al., “Temporal pole morphology and psychopathology in males with schizophrenia,” Psychiatry Res. Neuroimaging, 132, 107–115 (2004).
A. M. Cunningham, P. B. Manis, R. R. Reed, and G. V. Ronnet, “Olfactory receptor neurons exist as distinct subclasses of immature and mature cells in primary culture,” Neurosci., 93, No. 4, 1301–1312 (1999).
L. Dahmani et al., “An intrinsic association between olfactory identification and spatial memory in humans,” Nat. Comm., 9, 4162 (2018).
G. Daval, J. Leveteau, and P. Macleod, “Analyse topographique de l’electro-olfactogramme chez la grenouille,” J. Physiol. Paris, 76, No. 6, 559–567 (1980).
R. L. Doty, P. Shaman, and M. Dann, “Development of the University of Pennsylvania Smell Identification Test, a standardized microencapsulated test of olfactory function,” Physiol. Behav., 32, No. 3, 489–502 (1984).
A. Drobyshevsky et al., “Antenatal insults modify newborn olfactory function by nitric oxide produced from neuronal nitric oxide synthase,” Exp. Neurol., 237, No. 2, 427–34 (2012).
C. N. Egbujo et al., “Molecular evidence for decreased synaptic efficacy in the postmortem olfactory bulb of individuals with schizophrenia,” Schizophr. Res., 168, 554–562 (2015).
J. A. English et al., “Reduced protein synthesis in schizophrenia patient-derived olfactory cells,” Transl. Psychiatry, 5, e663 (2015).
R. Faigle and H. Song, “Signaling mechanisms regulating adult neural stem cells and neurogenesis,” Biochim. Biophys. Acta, 1830, No. 2, 2435–48 (2013).
B. J. Gallagher, J. A. McFalls, B. J. Jones, and A. M. Pisa, “Prenatal illness and subtypes of schizophrenia, the winter pregnancy phenomenon,” J. Clin. Psychol., 55, 915–922 (1999).
N. J. Gamo and A. Sawa, “Human stem cells and surrogate tissues for basic and translational study of mental disorders,” Biol. Psychiatry, 75, No. 12, 918–919 (2015).
C. L. Godoy et al., “Olfaction in neurologic and neurodegenerative diseases, a literature review,” Arch. Otorhinolaryngol., 19, 176–179 (2015).
W. F. Goette, A. E. Werry, and A. L. Schmitt, “The relationship between smell identification and neuropsychological domains: Results from a sample of community-dwelling adults suspected of dementia,” J. Clin. Exp. Neuropsychol., 40, No. 6, 595–605 (2018).
Q. Gong, “Culture of mouse olfactory sensory neurons,” Curr. Protoc. Neurosci., Unit 3, 24 (2012).
J. D. Howard et al., “Odor quality coding and categorization in human posterior piriform cortex,” Nat. Neurosci., 12, 932–938 (2009).
A. Y. Hsia, J. D. Vincent, and P. M. Lledo, “Dopamine depresses synaptic inputs into the olfactory bulb,” J. Neurophysiol., 82, No. 2, 1082–5 (1999).
V. Kamath, J. S. Bedwell, and M. T. Compton, “Is the odour identification deficit in schizophrenia influenced by odour hedonics?” Cogn. Neuropsychiatry, 16, No. 5, 448–60 (2011).
V. Kamath et al., “Olfactory processing in schizophrenia, non-ill first-degree family members, and young people at-risk for psychosis,” World J. Biol. Psychiatry, 15, No. 3, 209–18 (2014).
S. Kiparizoska and T. Ikuta, “Disrupted olfactory integration in schizophrenia: Functional connectivity study,” Int. J. Neuropsychopharmacol., 20, No. 9, 740–746 (2017).
L. C. Kopala et al., “Olfactory function in monozygotic twins discordant for schizophrenia,” Am. J. Psychiatry, 155, 134–136 (1998).
L. C. Kopala et al., “Impaired olfactory identification in relatives of patients with familial schizophrenia,” Am. J. Psychiatry, 158, No. 8, 1286–90 (2001).
T. Kovács, “Mechanisms of olfactory dysfunction in aging and neurodegenerative disorders,” Ageing Res. Rev., 3, 215–232 (2004).
J. Lavoie, A. Sawa, and K. Ishizuka, “Application of olfactory tissue and its neural progenitors to schizophrenia and psychiatric research,” Curr. Opin. Psychiatry, 30, No. 3, 176–183 (2017).
S. G. Leinwand and S. H. Chalasani, “Olfactory networks: from sensation to perception,” Curr. Opin. Genet. Dev., 21, No. 6, 806–11 (2011).
P. F. Liddle, “Schizophrenic syndromes, cognitive performance and neurological dysfunction,” Psychol. Med., 17, No. 1, 49–57 (1987).
D. A. Lim and A. Alvarez-Buylla, “The adult ventricular-subventricular zone (V-SVZ) and olfactory bulb (OB) neurogenesis,” Cold Spring Harb. Perspect. Biol., 8, No. 5, a018820 (2016).
N. Mandairon, F. Jourdan, and A. Didier, “Deprivation of sensory inputs to the olfactory bulb up-regulates cell death and proliferation in the subventricular zone of adult mice,” Neurosci., 119, 507–516 (2003).
C. Martin, J. Beshel, and L. M. Kay, “An olfacto-hippocampal network is dynamically involved in odor-discrimination learning,” J. Neurophysiol., 98, No. 4, 2196–2205 (2007).
N. A. Martínez et al., “Clinical importance of olfactory function in neurodegenerative diseases,” Rev. Med. Hosp. Gen. Méx., 81, No. 4, 268–275 (2018).
B. P. Menco, “Pre-natal development of rat nasal epithelia. IV. Freeze-fracturing on apices, microvilli and primary and secondary cilia of olfactory and respiratory epithelial cells, and on olfactory axons,” Anat. Embryol. (Berl.), 178, No. 4, 309–26 (1988).
A. Menini, “Calcium signalling and regulation in olfactory neurons,” Curr. Opin. Neurobiol., 9, 419–426 (1999).
J. K. Millar et al., “DISC1 and PDE4B are interacting genetic factors in schizophrenia that regulate cAMP signaling,” Science, 310, 1187–1191 (2005).
P. J. Moberg et al., “Olfactory dysfunction in schizophrenia: a qualitative and quantitative review,” Neuropsychopharmacology, 21, No. 3, 325–40 (1999).
P. J. Moberg, D. R. Roalf, R. E. Gur, and B. I. Turetsky, “Smaller nasal volumes as stigmata of aberrant neurodevelopment in schizophrenia,” Am. J. Psychiatry, 161, 2314–2316 (2004).
S. Nagayama et al., “Differential axonal projection of mitral and tufted cells in the mouse main olfactory system,” Front. Neural Circuits, 4, 120 (2010).
A. D. Nguyen, M. E. Shenton, and J. J. Levitt, “Olfactory dysfunction in schizophrenia: a review of neuroanatomy and psychophysiological measurements,” Harv. Rev. Psychiatry, 18, No. 5, 279–92 (2010).
O. O. Okusaga, “Accelerated aging in schizophrenia patients: the potential role of oxidative stress,” Aging Dis., 5, No. 4, 256–62 (2013).
H. Pantazopoulos et al., “Proteoglycan abnormalities in olfactory epithelium tissue from subjects diagnosed with schizophrenia,” Spec. Sect. Negat. Sympt., 150, 366–372 (2013).
B. M. Pause et al., “Increased processing speed for emotionally negative odors in schizophrenia,” Int. J. Psychophysiol., 70, No. 1, 16–22 (2008).
G. D. Pearlson et al., “Medial and superior temporal gyral volumes and cerebral asymmetry in schizophrenia versus bipolar disorder,” Biol. Psychiatry, 41, 1–14 (1997).
J. Plailly et al., “Left temporo-limbic and orbital dysfunction in schizophrenia during odor familiarity and hedonicity judgments,” NeuroImage, 29, 302–313 (2006).
L. Rioux et al., “Characterization of olfactory bulb glomeruli in schizophrenia,” Schizophr. Res., 77, No. 2–3, 229–239 (2005).
D. R. Roalf et al., “Unirhinal olfactory function in schizophrenia patients and first-degree relatives,” Neuropsych. Clin. Neurosci., 8, 389–396 (2016).
J. P. Royet et al., “Functional anatomy of perceptual and semantic processing for odors,” J. Cogn. Neurosci., 11, No. 1, 94–109 (1999).
I. Savic, “Imaging of brain activation by odorants in humans,” Curr. Opin. Neurobiol., 12, No. 4, 455–61 (2002).
R. Sattler, et al., “Human nasal olfactory epithelium as a dynamic marker for CNS therapy development,” Exp. Neurol., 232, No. 2, 203–11 (2011).
M. Schecklmann et al., “A systematic review on olfaction in child and adolescent psychiatric disorders,” J. Neural Transm. (Vienna), 120, No. 1, 121–30 (2013).
L. J. Seidman et al., “Experimental and clinical neuropsychological measures of prefrontal dysfunction in schizophrenia,” Neuropsychology, 9, No. 4 (1995).
K. Sim et al., “Hippocampal and parahippocampal volumes in schizophrenia, a structural MRI study,” Schizophr. Bull., 32, No. 2, 332–40 (2006).
P. Sirota et al., “Increased olfactory sensitivity in first episode psychosis and the effect of neuroleptic treatment on olfactory sensitivity in schizophrenia,” Psychiatry Res., 86, No. 2, 143–53 (1999).
P. Taupin, “Adult neurogenesis in the mammalian central nervous system, functionality and potential clinical interest,” Med. Sci. Monit., 11, No. 7, RA247–252 (2005).
J. Y. Tee, R. Sutharsan, Y. Fan, and A. Mackay-Sim, “Cell migration in schizophrenia, patient-derived cells do not regulate motility in response to extracellular matrix,” Mol. Cell. Neurosci., 80, 111–122 (2017).
B. Turetsky et al., “Frontal and temporal lobe brain volumes in schizophrenia. Relationship to symptoms and clinical subtype,” Arch. Gen. Psychiatry, 52, No. 12, 1061–70 (1995).
B. I. Turetsky et al., “Olfactory bulb volume is reduced in patients with schizophrenia,” Am. J. Psychiatry, 157, 828–830 (2000).
B. I. Turetsky et al., “Low olfactory bulb volume in 1st-degree relatives of patients with schizophrenia,” Am. J. Psychiatry, 160, 703–708 (2003).
B. I. Turetsky et al., “Physiological impairment of olfactory stimulus processing in schizophrenia,” Biol. Psychiatry, 53, 403–41 (2003).
B. I. Turetsky et al., “Decrements in volume of anterior ventromedial temporal lobe and olfactory dysfunction in schizophrenia,” Arch. Gen. Psychiatry, 60, No. 12, 1193–200 (2003).
B. I. Turetsky et al., “Reduced posterior nasal cavity volume: a gender-specific neurodevelopmental abnormality in schizophrenia,” Schizophr. Res., 93, 237–244 (2007).
B. I. Turetsky, C. G. Hahn, S. E. Arnold, and P. J. Moberg, “Olfactory receptor neuron dysfunction in schizophrenia,” Neuropsychopharmacology, 34, No. 3, 767–774 (2009).
B. I. Turetsky, C. G. Hahn, K. Borgmann-Winter, and P. J. Moberg, “Scents and nonsense: olfactory dysfunction in schizophrenia,” Schizophr. Bull., 35, No. 6, 1117–1131 (2009).
B. I. Turetsky and P. J. Moberg, “An odor-specific threshold deficit implicates abnormal intracellular cyclic AMP signaling in schizophrenia,” Am. J. Psychiatry, 166, No. 2, 226–33 (2009).
R. Vassar et al., “Topographic organization of sensory projections to the olfactory bulb,” Cell, 79, 981–991 (1994).
C. S. Weickert and D. Weinberger, “A candidate molecule approach to defining developmental pathology in schizophrenia,” Schizophr. Bull., 24, No. 2, 303–316 (1998).
D. W. Wesson, D. A. Wilson, and R. A. Nixon, “Should olfactory dysfunction be used as a biomarker of Alzheimer’s disease?” Expert Rev. Neurother., 10, No. 5, 633–635 (2010).
Y. Yılmaz et al., “Clinical assessment and implication of olfactory dysfunction in neuropsychiatric disorders of childhood and adulthood: A review of literature,” Neurobehav. Sci., 1, 7–30 (2015).
D. H. Zald and J. V. Pardo, “Emotion, olfaction, and the human amygdala, amygdala activation during aversive olfactory stimulation,” Proc. Natl. Acad. Sci. USA, 94, No. 8, 4119–24 (1997).
Author information
Authors and Affiliations
Corresponding author
Additional information
Translated from Uspekhi Fiziologicheskikh Nauk, Vol. 52, No. 2, pp. 93–104, April–June, 2021.
Rights and permissions
About this article
Cite this article
Bigdai, E.V., Samoilov, V.O. & Sinegubov, A.A. Complex Impairments to the Olfactory Sensory System in Schizophrenia. Neurosci Behav Physi 52, 598–606 (2022). https://doi.org/10.1007/s11055-022-01280-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11055-022-01280-w