Abstract
Background
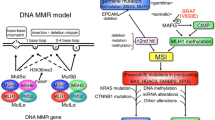
In cancer research, one of the most significant findings was to characterize the DNA repair deficiency as carcinogenic. Amongst the various repair mechanisms, mismatch repair (MMR) and direct reversal of DNA damage systems are designated as multilevel safeguards in the human genome. Defects in these elevate the rate of mutations and results in dire consequences like cancer. Of the several molecular signatures in human genome, tandem repeats (TRs) appear at various frequencies in the exonic, intronic, and regulatory regions of the DNA. Hypervariability among these repeats in the coding and non-coding regions of the genes is well characterized for solid tumours, but its significance in haematologic malignancies remains to be explored. The purpose of our study was to elucidate the role of nucleotide repeat instability in the coding and non-coding regions of 10 different repair genes in myeloid and lymphoid cell lines compared to the control samples.
Methods and Results
We selected MMR deficient extensively studied microsatellite instable colorectal cancer (HCT116), and MMR proficient breast cancer (MCF-7) cells along with underemphasized haematologic cancer cell lines to decipher the hypermutability of tandem repeats. A statistically significant TR variation was observed for MSH2 and MSH6 genes in 4 and 3 of the 6 cell lines respectively. KG1 (AML) and Daudi (Burkitt’s lymphoma) were found to have compromised DNA repair competency with highly unstable nucleotide repeats.
Conclusion
Taken together, the results suggest that mutable TRs in intronic and non-intronic regions of repair genes in blood cancer might have a tumorigenic role. Since this is a pilot study on cell lines, high throughput research in large cohorts can be undertaken to reveal novel diagnostic markers for unexplained blood cancer patients with normal karyotypes or otherwise with karyotypic defects.



Similar content being viewed by others
References
Yang G, Zheng RY, ** ZS (2019) Correlations between microsatellite instability and the biological behaviour of tumours. J Cancer Res Clin Oncol 145:2891–2899. https://doi.org/10.1007/s00432-019-03053-4
Bhattacharya P, Patel TN (2018) Microsatellite instability and promoter hypermethylation of DNA repair genes in hematologic malignancies: a forthcoming direction toward diagnostics. Hematology 23:77–82. https://doi.org/10.1080/10245332.2017.1354428
Vieira ML, Santini L, Diniz AL, Munhoz Cde F (2016) Microsatellite markers: what they mean and why they are so useful. Genet Mol Biol 39:312–328. https://doi.org/10.1590/1678-4685-GMB-2016-0027
Sulovari A, Li R, Audano PA, Porubsky D, Vollger MR, Logsdon GA et al (2019) Human-specific tandem repeat expansion and differential gene expression during primate evolution. Proc Natl Acad Sci USA 116:23243–23253. https://doi.org/10.1073/pnas.1912175116
Bolton KA, Ross JP, Grice DM, Bowden NA, Holliday EG, Avery-Kiejda KA et al (2013) STaRRRT: a table of short tandem repeats in regulatory regions of the human genome. BMC Genomics 14:795. https://doi.org/10.1186/1471-2164-14-795
Li YC, Korol AB, Fahima T, Nevo E (2004) Microsatellites within genes: structure, function, and evolution. Mol Biol Evol 21:991–1007. https://doi.org/10.1093/molbev/msh073
Li K, Luo H, Huang L, Luo LH, Zhu X (2020) Microsatellite instability: a review of what the oncologist should know. Cancer Cell Int 20:16. https://doi.org/10.1186/s12935-019-1091-8
Pećina-Šlaus N, Kafka A, Salamon I, Bukovac A (2020) Mismatch repair pathway, genome stability and cancer. Front Mol Biosci 7:122. https://doi.org/10.3389/fmolb.2020.00122
Modrich P, Lahue R (1996) Mismatch repair in replication fidelity, genetic recombination, and cancer biology. Annu Rev Biochem 65:101–133. https://doi.org/10.1146/annurev.bi.65.070196.000533
Chikan NA, Bukhari S, Shabir N, Amin A, Shafi S, Qadri RA et al (2015) Atomic insight into the altered O6-methylguanine-DNA methyltransferase protein architecture in gastric cancer. PLoS ONE 10:e0127741. https://doi.org/10.1371/journal.pone.0127741
Rye PT, Delaney JC, Netirojjanakul C, Sun DX, Liu JZ, Essigmann JM (2008) Mismatch repair proteins collaborate with methyltransferases in the repair of O(6)-methylguanine. DNA Repair (Amst) 7:170–176. https://doi.org/10.1016/j.dnarep.2007.09.003
Akagi K, Oki E, Taniguchi H, Nakatani K, Aoki D, Kuwata T et al (2020) Nationwide large-scale investigation of microsatellite instability status in more than 18,000 patients with various advanced solid cancers. J Clin Oncol 38:803–803. https://doi.org/10.1200/JCO.2020.38.4_suppl.803
Magalhães M, Farre L, Bittencourt A (2011) Microsatellite instability in the smoldering form of adult T-cell leukemia/lymphoma (ATL) in Brazil. Retrovirology 8:A148. https://doi.org/10.1186/1742-4690-8-S1-A148
Miyashita K, Fujii K, Taguchi K, Shimokawa M, Yoshida MA, Abe Y et al (2017) A specific mode of microsatellite instability is a crucial biomarker in adult T-cell leukaemia/lymphoma patients. J Cancer Res Clin Oncol 143:399–408. https://doi.org/10.1007/s00432-016-2294-1
Sanz-Vaqué L, Colomer D, Bosch F, López-Guillermo A, Dreyling MH, Bosch F et al (2001) Microsatellite instability analysis in typical and progressed mantle cell lymphoma and B-cell chronic lymphocytic leukemia. Haematologica 86:181–186
Walker CJ, Eisfeld AK, Genutis LK, Bainazar M, Kohlschmidt J, Mrózek K et al (2017) No evidence for microsatellite instability in acute myeloid leukemia. Leukemia 31:1474–1476. https://doi.org/10.1038/leu.2017.97
Losso GM, Moraes Rda S, Gentili AC, Messias-Reason IT (2012) Microsatellite instability—MSI markers (BAT26, BAT25, D2S123, D5S346, D17S250) in rectal cancer. Arq Bras Cir Dig 25:240–244. https://doi.org/10.1590/s0102-67202012000400006
Liengswangwong U, Nitta T, Kashiwagi H, Kikukawa H, Kawamoto T, Todoroki T et al (2003) Infrequent microsatellite instability in liver fluke infection-associated intrahepatic cholangiocarcinomas from Thailand. Int J Cancer 107:375–380. https://doi.org/10.1002/ijc.11380
Lu Y, Soong TD, Elemento O (2013) A novel approach for characterizing microsatellite instability in cancer cells. PLoS ONE 8:e63056. https://doi.org/10.1371/journal.pone.0063056
Nugoli M, Chuchana P, Vendrell J, Orsetti B, Ursule L, Nguyen C et al (2003) Genetic variability in MCF-7 sublines: evidence of rapid genomic and RNA expression profile modifications. BMC Cancer 3:13. https://doi.org/10.1186/1471-2407-3-13
Zhang J, Kuo CC, Chen L (2011) GC content around splice sites affects splicing through pre-mRNA secondary structures. BMC Genomics 12:90. https://doi.org/10.1186/1471-2164-12-90
Evrard C, Tachon G, Randrian V, Karayan-Tapon L, Tougeron D (2019) Microsatellite instability: diagnosis, heterogeneity, discordance, and clinical impact in colorectal cancer. Cancers 11:1567. https://doi.org/10.3390/cancers11101567
Nojadeh JN, Behrouz Sharif S, Sakhinia E (2018) Microsatellite instability in colorectal cancer. Excli J 17:159–168. https://doi.org/10.17179/excli2017-948
Adem C, Soderberg CL, Cunningham JM, Reynolds C, Sebo TJ, Thibodeau SN et al (2003) Microsatellite instability in hereditary and sporadic breast cancers. Int J Cancer 107:580–582. https://doi.org/10.1002/ijc.11442
Rimsza LM, Kopecky KJ, Ruschulte J, Chen IM, Slovak ML, Karanes C et al (2000) Microsatellite instability is not a defining genetic feature of acute myeloid leukemogenesis in adults: results of a retrospective study of 132 patients and review of the literature. Leukemia 14:1044–1051. https://doi.org/10.1038/sj.leu.2401699
Nomdedéu JF, Perea G, Estivill C, Lasa A, Carnicer MJ, Brunet S et al (2005) Microsatellite instability is not an uncommon finding in adult de novo acute myeloid leukemia. Ann Hematol 84:368–375. https://doi.org/10.1007/s00277-005-1035-3
Inokuchi K, Ikejima M, Watanabe A, Nakajima E, Orimo H, Nomura T et al (1995) Loss of expression of the human MSH3 gene in hematological malignancies. Biochem Biophys Res Commun 214:171–179. https://doi.org/10.1006/bbrc.1995.2271
Edelmann W, Umar A, Yang K, Heyer J, Kucherlapati M, Lia M et al (2000) The DNA mismatch repair genes Msh3 and Msh6 cooperate in intestinal tumor suppression. Cancer Res 60:803–807
Morimoto H, Tsukada J, Kominato Y, Tanaka Y (2005) Reduced expression of human mismatch repair genes in adult T-cell leukemia. Am J Hematol 78:100–107. https://doi.org/10.1002/ajh.20259
Matheson EC, Hogarth LA, Case MC, Irving JA, Hall AG (2007) DHFR and MSH3 co-amplification in childhood acute lymphoblastic leukaemia, in vitro and in vivo. Carcinogenesis 28:1341–1346. https://doi.org/10.1093/carcin/bgl235
Nuuri K, Arroyo-Berdugo Y, Esposito MT (2020) Analysis of expression of MSH2 and MSH3 genes in Mixed Lineage Leukemia (MLL)–Acute Lymphoblastic Leukemia (ALL) human cell lines. J Young Investig 37:38–48
Rajewska M, Wegrzyn K, Konieczny I (2012) AT-rich region and repeated sequences—the essential elements of replication origins of bacterial replicons, FEMS. Microbiol Rev 36:408–434. https://doi.org/10.1111/j.1574-6976.2011.00300.x
Yang Y, Jain RK, Glenn ST, Xu B, Singh PK, Wei L et al (2020) Complete response to anti-PD-L1 antibody in a metastatic bladder cancer associated with novel MSH4 mutation and microsatellite instability. J Immunother Cancer 8:e000128. https://doi.org/10.1136/jitc-2019-000128
Clark N, Wu X, Her C (2013) MutS homologues hMSH4 and hMSH5: genetic variations, functions, and implications in human diseases. Curr Genomics 14:81–90. https://doi.org/10.2174/1389202911314020002
Sekine H, Ferreira RC, Pan-Hammarström Q, Graham RR, Ziemba B, de Vries SS et al (2007) Role for Msh5 in the regulation of Ig class switch recombination. Proc Natl Acad Sci U S A 104:7193–7198. https://doi.org/10.1073/pnas.0700815104
de Valles-Ibáñez G, Esteve-Solé A, Piquer M, González-Navarro EA, Hernandez-Rodriguez J et al (2018) Evaluating the genetics of common variable immunodeficiency: monogenetic model and beyond. Front immunol 9:636. https://doi.org/10.3389/fimmu.2018.00636
Graham RP, Kerr SE, Butz ML, Thibodeau SN, Halling KC, Smyrk TC et al (2015) Heterogenous MSH6 loss is a result of microsatellite instability within MSH6 and occurs in sporadic and hereditary colorectal and endometrial carcinomas. Am J Surg Pathol 39:1370–1376. https://doi.org/10.1097/PAS.0000000000000459
Ollikainen M, Hannelius U, Lindgren CM, Abdel-Rahman WM, Kere J, Peltomäki P (2007) Mechanisms of inactivation of MLH1 in hereditary nonpolyposis colorectal carcinoma: a novel approach. Oncogene 26:4541–4549. https://doi.org/10.1038/sj.onc.1210236
Hutter P, Wijnen J, Rey-Berthod C, Thiffault I, Verkuijlen P, Farber D et al (2002) An MLH1 haplotype is over-represented on chromosomes carrying an HNPCC predisposing mutation in MLH1. J Med Genet 39:323–327. https://doi.org/10.1136/jmg.39.5.323
Limpaiboon T, Krissadarak K, Sripa B, Jearanaikoon P, Bhuhisawasdi V, Chau-in S et al (2002) Microsatellite alterations in liver fluke related cholangiocarcinoma are associated with poor prognosis. Cancer Lett 181:215–222. https://doi.org/10.1016/s0304-3835(02)00052-6
Leeksma OC, de Miranda NF, Veelken H (2017) Germline mutations predisposing to diffuse large B-cell lymphoma. Blood Cancer J 7:e532 (Erratum in: Blood. Cancer. J. 7 (2017) e541. DOI: 10.1038/bcj.2017.15)
Bakry D, Aronson M, Durno C, Rimawi H, Farah R, Alharbi QK et al (2014) Genetic and clinical determinants of constitutional mismatch repair deficiency syndrome: report from the constitutional mismatch repair deficiency consortium. Eur J Cancer 50:987–996. https://doi.org/10.1016/j.ejca.2013.12.005
Loukola A, Vilkki S, Singh J, Launonen V, Aaltonen LA (2000) Germline and somatic mutation analysis of MLH3 in MSI-positive colorectal cancer. Am J Pathol 157:347–352. https://doi.org/10.1016/S0002-9440(10)64546-4
Bacher JW, Clipson L, Steffen LS, Halberg RB (2016) Microsatellite instability and its significance to hereditary and sporadic cancer. Microsatellite markers. IntechOpen, London. https://doi.org/10.5772/65065
Geisler JP, Goodheart MJ, Sood AK, Holmes RJ, Hatterman-Zogg MA, Buller RE (2003) Mismatch repair gene expression defects contribute to microsatellite instability in ovarian carcinoma. Cancer 98:2199–2206. https://doi.org/10.1002/cncr.11770
Sugano K, Nakajima T, Sekine S, Taniguchi H, Saito S, Takahashi M et al (2016) Germline PMS2 mutation screened by mismatch repair protein immunohistochemistry of colorectal cancer in Japan. Cancer Sci 107:1677–1686. https://doi.org/10.1111/cas.13073
Pink RC, Wicks K, Caley DP, Punch EK, Jacobs L, Carter DR (2011) Pseudogenes: pseudo-functional or key regulators in health and disease? RNA 17:792–798. https://doi.org/10.1261/rna.2658311
Whitehall VL, Walsh MD, Young J, Leggett BA, Jass JR (2001) Methylation of O-6-methylguanine DNA methyltransferase characterizes a subset of colorectal cancer with low-level DNA microsatellite instability. Cancer Res 61:827–830
Fox EJ, Leahy DT, Geraghty R, Mulcahy HE, Fennelly D, Hyland JM et al (2006) Mutually exclusive promoter hypermethylation patterns of hMLH1 and O6-methylguanine DNA methyltransferase in colorectal cancer. J Mol Diagn 8:68–75. https://doi.org/10.2353/jmoldx.2006.050084
Amit M, Donyo M, Hollander D, Goren A, Kim E, Gelfman S et al (2012) Differential GC content between exons and introns establishes distinct strategies of splice-site recognition. Cell Rep 1:543–556. https://doi.org/10.1016/j.celrep.2012.03.013
Zhao P, Li L, Jiang X, Li Q (2019) Mismatch repair deficiency/microsatellite instability-high as a predictor for anti-PD-1/PD-L1 immunotherapy efficacy. J Hematol Oncol 12:54. https://doi.org/10.1186/s13045-019-0738-1
Kelley MR, Logsdon D, Fishel ML (2014) Targeting DNA repair pathways for cancer treatment: what’s new? Future Oncol 10:1215–1237. https://doi.org/10.2217/fon.14.60
Acknowledgements
We are extremely grateful to Penn State Cancer Institute, Hershey, PA 17033, USA.for generous donation of HCT116 cell lines.
Funding
We are thankful to Vellore Institute of Technology for providing the facilities and fund for research student without which the work would have not be completed.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declares that they have no conflict of interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bhattacharya, P., Patel, T.N. Looking beyond the cytogenetics in haematological malignancies: decoding the role of tandem repeats in DNA repair genes. Mol Biol Rep 49, 10293–10305 (2022). https://doi.org/10.1007/s11033-022-07761-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-022-07761-y