Abstract
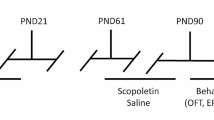
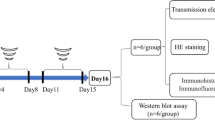
Therapeutic hypothermia (TH) is the standard treatment for neonatal hypoxia-ischemia (HI) with a time window limited up to 6 h post injury. However, influence of sexual dimorphism in the therapeutic window for TH has not yet been elucidated in animal models of HI. Therefore, the aim of this study was to investigate the most effective time window to start TH in male and female rats submitted to neonatal HI. Wistar rats (P7) were divided into the following groups: NAÏVE and SHAM (control groups), HI (submitted to HI) and TH (submitted to HI and TH; 32ºC for 5 h). TH was started at 2 h (TH-2 h group), 4 h (TH-4 h group), or 6 h (TH-6 h group) after HI. At P14, animals were subjected to behavioural tests, volume of lesion and reactive astrogliosis assessments. Male and female rats from the TH-2 h group showed reduction in the latency of behavioral tests, and decrease in volume of lesion and intensity of GFAP immunofluorescence. TH-2 h females also showed reduction of degenerative cells and morphological changes in astrocytes. Interestingly, females from the TH-6 h group showed an increase in volume of lesion and in number of degenerative hippocampal cells, associated with worse behavioral performance. Together, these results indicate that TH neuroprotection is time- and sex-dependent. Moreover, TH started later (6 h) can worsen volume of brain lesion in females. These data indicate the need to develop specific therapeutic protocols for each sex and reinforce the importance of early onset of the hypothermic treatment.
Graphical Abstract








Similar content being viewed by others
Data Availability
“The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request”.
References
Abate BB, Bimerew M, Gebremichae B et al (2021) Effects of therapeutic hypothermia on death among asphyxiated neonates with hypoxicischemic encephalopathy: A systematic review and meta-analysis of randomized control trials. PLoS ONE 16:1–20. https://doi.org/10.1371/journal.pone.0247229
Ahn SY, Chang YS, Sung DK et al (2018) Hypothermia broadens the therapeutic time window of mesenchymal stem cell transplantation for severe neonatal hypoxic ischemic encephalopathy. Sci Rep 8:1–10. https://doi.org/10.1038/s41598-018-25902-x
Arteni NS, Pereira LO, Rodrigues AL et al (2010) Lateralized and sex-dependent behavioral and morphological effects of unilateral neonatal cerebral hypoxia-ischemia in the rat. Behav Brain Res 210:92–98. https://doi.org/10.1016/j.bbr.2010.02.015
Askalan R, Gabarin N, Armstrong EA et al (2015) Mechanisms of neurodegeneration after severe hypoxic-ischemic injury in the neonatal rat brain. Brain Res 1629:94–103. https://doi.org/10.1016/j.brainres.2015.10.020
Bezzi P, Volterra A (2001) A neuron–glia signalling network in the active brain. Curr Opin Neurobiol 11:387–394. https://doi.org/10.1016/S0959-4388(00)00223-3
Burnsed JC, Chavez-Valdez R, Hossain MS et al (2015) Hypoxia-ischemia and therapeutic hypothermia in the neonatal mouse brain - A longitudinal study. PLoS ONE 10:1–20. https://doi.org/10.1371/journal.pone.0118889
Catherine RC, Ballambattu VB, Adhisivam B et al (2021) Effect of Therapeutic Hypothermia on the Outcome in Term Neonates with Hypoxic Ischemic Encephalopathy—A Randomized Controlled Trial. J Trop Pediatr 67:1–6. https://doi.org/10.1093/tropej/fmaa073
Cho KHT, Davidson JO, Dean JM et al (2020) Cooling and immunomodulation for treating hypoxic-ischemic brain injury. Pediatr Int 62:770–778. https://doi.org/10.1111/ped.14215
Davidson JO, Wassink G, van den Heuij LG et al (2015) Therapeutic Hypothermia for Neonatal Hypoxic–Ischemic Encephalopathy – Where to from Here? Front Neurol 6. https://doi.org/10.3389/fneur.2015.00198
Davies A, Wassink G, Bennet L et al (2019) Can we further optimize therapeutic hypothermia for hypoxic-ischemic encephalopathy? Neural Regeneration Research 14:1678–1683. https://doi.org/10.4103/1673-5374.257512
de Fraga LS, Tassinari ID, Jantsch J et al (2021) “A picture is worth a thousand words”: the use of microscopy for imaging neuroinflammation. Clin Experimental Immunol 00:1–21. https://doi.org/10.1111/cei.13669
Degucchi K, Oguchi K, Takashima S (1997) Characteristic Neuropathology of Leukomalacia in Extremely Low Birth Weight Infants. Pediatr Neurol 16:290–300
Dhikav V, Anand K (2012) Hippocampus in health and disease: An overview. Ann Indian Acad Neurol 15:239. https://doi.org/10.4103/0972-2327.104323
Escartin C, Galea E, Lakatos A et al (2021) Reactive astrocyte nomenclature, definitions, and future directions. Nat Neurosci 24:312–325. https://doi.org/10.1038/s41593-020-00783-4
Fabres RB, da Rosa LA, de Souza SK et al (2018) Effects of progesterone on the neonatal brain following hypoxia-ischemia. Metab Brain Dis 1–9. https://doi.org/10.1007/s11011-018-0193-7
Fabres RB, Montes NL, de Camboim Y et al (2020a) Long-Lasting Actions of Progesterone Protect the Neonatal Brain Following Hypoxia-Ischemia. Cell Mol Neurobiol. https://doi.org/10.1007/s10571-020-00827-0
Fabres RB, Montes NL, de Camboim Y et al (2020b) Long-Lasting Actions of Progesterone Protect the Neonatal Brain Following Hypoxia-Ischemia. Cell Mol Neurobiol. https://doi.org/10.1007/s10571-020-00827-0
Fang AY, Gonzalez FF, Sheldon RA, Ferriero DM (2013) Effects of combination therapy using hypothermia and erythropoietin in a rat model of neonatal hypoxia-ischemia. Pediatr Res 73:12–17. https://doi.org/10.1038/pr.2012.138
Gunn AJ, Gunn TR, De Haan HH et al (1997) Dramatic neuronal rescue with prolonged selective head cooling after ischemia in fetal lambs. J Clin Invest 99:248–256. https://doi.org/10.1172/JCI119153
Haim L, Ben, Carrillo-de Sauvage MA, Ceyzériat K, Escartin C (2015) Elusive roles for reactive astrocytes in neurodegenerative diseases. Front Cell Neurosci 9:1–27. https://doi.org/10.3389/fncel.2015.00278
Hermans RHM, Hunter DE, Mcgivern RF et al (1992) Behavioral sequelae in young rats of acute intermittent antenatal hypoxia. Neurotoxicol Teratol 14:119–129. https://doi.org/10.1016/0892-0362(92)90060-N
Heyser CJ (2003) Assessment of Developmental Milestones in Rodents. Curr Protoc Neurosci 25:1–15. https://doi.org/10.1002/0471142301.ns0818s25
Jatana M, Singh I, Singh AK, Jenkins D (2006) Combination of systemic hypothermia and N-acetylcysteine attenuates hypoxic-ischemic brain injury in neonatal rats. Pediatr Res 59:684–689. https://doi.org/10.1203/01.pdr.0000215045.91122.44
Joly LM, Mucignat V, Mariani J et al (2004) Caspase Inhibition after Neonatal Ischemia in the Rat Brain. J Cereb Blood Flow Metab 24:124–131. https://doi.org/10.1097/01.WCB.0000100061.36077.5F
Lehmann J, Pryce CR, Bettschen D, Feldon J (1999) The Maternal Separation Paradigm and Adult Emotionality and Cognition in Male and Female Wistar Rats. Pharmacol Biochem Behav 64:705–715. https://doi.org/10.1016/S0091-3057(99)00150-1
Li J, Feng L, **ng Y et al (2014) Radioprotective and antioxidant effect of resveratrol in hippocampus by activating Sirt1. Int J Mol Sci 15:5928–5939. https://doi.org/10.3390/ijms15045928
Liddelow SA, Guttenplan KA, Clarke LE et al (2017) Neurotoxic reactive astrocytes are induced by activated microglia. Nature 541:481–487. https://doi.org/10.1038/nature21029
Lubics A, Reglodi D, Tamás A et al (2005) Neurological reflexes and early motor behavior in rats subjected to neonatal hypoxic-ischemic injury. Behav Brain Res 157:157–165. https://doi.org/10.1016/j.bbr.2004.06.019
Mari C, Odorcyk FK, Sanches EF et al (2019) International Journal of Developmental Neuroscience Arundic acid administration protects astrocytes, recovers histological damage and memory de fi cits induced by neonatal hypoxia ischemia in rats. Int J Dev Neurosci 76:41–51. https://doi.org/10.1016/j.ijdevneu.2019.06.003
Mestriner RG, Pagnussat AS, Boisserand LSB et al (2011) Skilled reaching training promotes astroglial changes and facilitated sensorimotor recovery after collagenase-induced intracerebral hemorrhage. Exp Neurol 227:53–61. https://doi.org/10.1016/j.expneurol.2010.09.009
Mirza MA, Ritzel R, Xu Y et al (2015) Sexually dimorphic outcomes and inflammatory responses in hypoxic-ischemic encephalopathy. J Neuroinflamm 12:1–10. https://doi.org/10.1186/s12974-015-0251-6
Nelson KB, Lynch JK (2004) Stroke in newborn infants. Lancet Neurol 3:150–158. https://doi.org/10.1016/S1474-4422(04)00679-9
Netto CA, Sanches E, Odorcyk FK et al (2017) Sex-dependent consequences of neonatal brain hypoxia-ischemia in the rat. J Neurosci Res 95:409–421
Nie X, Lowe DW, Rollins LG et al (2016) Sex-specific effects of N-acetylcysteine in neonatal rats treated with hypothermia after severe hypoxia-ischemia. Neurosci Res 108:24–33. https://doi.org/10.1016/j.neures.2016.01.008
Owoeye O, Malomo AO (2015) Launaea taraxacifolia leaf extract protected against gamma radiation – induced haematological, behavioural and histological alterations in the hippocampus and cerebellum of rats. archives Basic & Appied Medicine 3:21–28
Park WS, Sung SI, Ahn SY et al (2015) Hypothermia augments neuroprotective activity of mesenchymal stem cells for neonatal hypoxic-ischemic encephalopathy. PLoS ONE 10:1–13. https://doi.org/10.1371/journal.pone.0120893
Paxinos G, Watson C (2007) The Rat Brain in Stereotaxic Coordinates, Elsevier S. SanDiego, CA
Peterson BL, Won S, Geddes RI et al (2015) Sex-related differences in effects of progesterone following neonatal hypoxic brain injury. Behav Brain Res. https://doi.org/10.1016/j.bbr.2015.03.005
Reddy SD, Wu X, Kuruba R et al (2020) Magnetic resonance imaging analysis of long-term neuropathology after exposure to the nerve agent soman: correlation with histopathology and neurological dysfunction. Ann N Y Acad Sci 1–20. https://doi.org/10.1111/nyas.14431
Reinboth BS, Köster C, Abberger H et al (2016) Endogenous hypothermic response to hypoxia reduces brain injury: Implications for modeling hypoxic-ischemic encephalopathy and therapeutic hypothermia in neonatal mice. Exp Neurol 283:264–275. https://doi.org/10.1016/j.expneurol.2016.06.024
Sabir H, Osredkar D, Maes E et al (2016) Xenon combined with therapeutic hypothermia is not neuroprotective after severe hypoxia-ischemia in neonatal rats. PLoS ONE 11:1–10. https://doi.org/10.1371/journal.pone.0156759
Sabir H, Scull-Brown E, Liu X, Thoresen M (2012) Immediate hypothermia is not neuroprotective after severe hypoxia-ischemia and is deleterious when delayed by 12 hours in neonatal rats. Stroke 43:3364–3370. https://doi.org/10.1161/STROKEAHA.112.674481
Sabir H, Walløe L, Dingley J et al (2014) Combined treatment of Xenon and hypothermia in newborn rats - Additive or synergistic effect? PLoS ONE 9:1–7. https://doi.org/10.1371/journal.pone.0109845
Saegusa Y, Fujimoto H, Woo GH et al (2012) Transient aberration of neuronal development in the hippocampal dentate gyrus after developmental exposure to brominated flame retardants in rats. Arch Toxicol 86:1431–1442. https://doi.org/10.1007/s00204-012-0824-4
Saegusa Y, Woo GH, Fujimoto H et al (2010) Sustained production of Reelin-expressing interneurons in the hippocampal dentate hilus after developmental exposure to anti-thyroid agents in rats. Reprod Toxicol 29:407–414. https://doi.org/10.1016/j.reprotox.2010.03.006
Sanches EF, Arteni NS, Nicola F et al (2013a) Early hypoxia-ischemia causes hemisphere and sex-dependent cognitive impairment and histological damage. https://doi.org/10.1016/j.neuroscience.2013.01.066. Neuroscience
Sanches EF, Arteni NS, Scherer EB et al (2013b) Are the consequences of neonatal hypoxia–ischemia dependent on animals’ sex and brain lateralization? Brain Res 1507:105–114. https://doi.org/10.1016/j.brainres.2013.02.040
Schneider T, Przewłocki R (2005) Behavioral alterations in rats prenatally to valproic acid: Animal model of autism. Neuropsychopharmacology 30:80–89. https://doi.org/10.1038/sj.npp.1300518
Shankaran S, Laptook AR, Ehrenkranz RA et al (2005) Whole-Body Hypothermia for Neonates with Hypoxic–Ischemic Encephalopathy. N Engl J Med 353:1574–1584. https://doi.org/10.1056/NEJMcps050929
Sheikhbahaei S, Morris B, Collina J et al (2018) Morphometric analysis of astrocytes in brainstem respiratory regions. J Comp Neurol 526:2032–2047. https://doi.org/10.1002/cne.24472
Sizonenko SV, Camm EJ, Dayer A, Kiss JZ (2008) Glial responses to neonatal hypoxic-ischemic injury in the rat cerebral cortex. Int J Dev Neurosci 26:37–45. https://doi.org/10.1016/j.ijdevneu.2007.08.014
Smith A, Garbus H, Rosenkrantz T, Fitch R (2015) Sex Differences in Behavioral Outcomes Following Temperature Modulation During Induced Neonatal Hypoxic Ischemic Injury in Rats. Brain Sci 5:220–240. https://doi.org/10.3390/brainsci5020220
Smith AL, Rosenkrantz TS, Fitch RH (2016) Effects of sex and mild intrainsult hypothermia on neuropathology and neural reorganization following neonatal hypoxic ischemic brain injury in rats. Neural Plasticity 2016:. https://doi.org/10.1155/2016/2585230
Sofroniew MV (2015) Astrogliosis. Cold Spring Harbor Perspectives in Biology 7:a020420. https://doi.org/10.1101/cshperspect.a020420
Soltesz I, Losonczy A (2018) CA1 pyramidal cell diversity enabling parallel information processing in the hippocampus. Nat Neurosci 21:484–493. https://doi.org/10.1038/s41593-018-0118-0
Sun H-S, Xu B, Chen W et al (2015) Neuronal KATP channels mediate hypoxic preconditioning and reduce subsequent neonatal hypoxic–ischemic brain injury. Exp Neurol 263:161–171. https://doi.org/10.1016/j.expneurol.2014.10.003
Tassinari IDÁ, Andrade MKG, da Rosa LA, Neuroscience et al (2020) https://doi.org/10.1016/j.neuroscience.2020.09.006
Thoresen M, Bågenholm R, Løberg EM et al (1996) Posthypoxic cooling of neonatal rats provides protection against brain injury. Arch Dis Child 74:0–5. https://doi.org/10.1136/fn.74.1.f3
Thoresen M, Hobbs CE, Wood T et al (2009) Cooling combined with immediate or delayed xenon inhalation provides equivalent long-term neuroprotection after neonatal hypoxia-ischemia. J Cereb Blood Flow Metab 29:707–714. https://doi.org/10.1038/jcbfm.2008.163
Thoresen M, Tooley J, Liu X et al (2013) Time Is Brain: Starting Therapeutic Hypothermia within Three Hours after Birth Improves Motor Outcome in Asphyxiated Newborns. Neonatology 104:228–233. https://doi.org/10.1159/000353948
Waddell J, Hanscom M, Shalon Edwards N et al (2016) Sex differences in cell genesis, hippocampal volume and behavioral outcomes in a rat model of neonatal HI. Exp Neurol 275:285–295. https://doi.org/10.1016/j.expneurol.2015.09.003
Wagner BP, Nedelcu J, Martin E (2002) Delayed postischemic hypothermia improves long-term behavioral outcome after cerebral hypoxia-ischemia in neonatal rats. Pediatr Res 51:354–360. https://doi.org/10.1203/00006450-200203000-00015
Wood T, Osredkar D, Puchades M et al (2016) Treatment temperature and insult severity influence the neuroprotective effects of therapeutic hypothermia. Sci Rep 6:23430. https://doi.org/10.1038/srep23430
**ong M, Yang Y, Chen G, Zhou W (2009) Post-ischemic hypothermia for 24 h in P7 rats rescues hippocampal neuron: Association with decreased astrocyte activation and inflammatory cytokine expression. Brain Res Bull 79:351–357. https://doi.org/10.1016/j.brainresbull.2009.03.011
Yuan X, Ghosh N, McFadden B et al (2015) Hypothermia modulates cytokine responses after neonatal rat hypoxic-ischemic injury and reduces brain damage. ASN Neuro 6. https://doi.org/10.1177/1759091414558418
Funding
This study was supported in part by grants from Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq), Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES) and, Financiadora de Estudos e Projetos (FINEP). We would also like to thank the Laboratório de Análises de Amostras Biológicas por Fluorescência (LabFluor - UFRGS) for the support in all analysis.
Author information
Authors and Affiliations
Contributions
All authors contributed in this work. RBF, LSF, CAN and planned the study design. RBF, RRN, MMM, MKGA, APRM, IDT and ESF conducted the experiments. RBF performed data analysis and wrote the manuscript. RBF and IDT prepared the figures. RBF, EFS, LFS and CAN revised critically the manuscript. LSF and CAN were recipient of funding used to support the study.
Corresponding author
Ethics declarations
Competing interests
The authors declare that they have no conflict of interest.
Ethics approval
All procedures involving animals were in accordance with the precepts of the National and International Guidelines, especially Law 11,794 of November 8, 2008, Decree 6899 of July 15, 2009, and as edited by the National Council for the Control of Animal Experimentation (CONCEA), was approved by the Institutional Animal Care and Use Committee of Federal University of Rio Grande do Sul (UFRGS, #31442).
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fabres, R.B., Nunes, R.R., de Medeiros de Mattos, M. et al. Therapeutic hypothermia for the treatment of neonatal hypoxia-ischemia: sex-dependent modulation of reactive astrogliosis. Metab Brain Dis 37, 2315–2329 (2022). https://doi.org/10.1007/s11011-022-01030-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11011-022-01030-4