Abstract
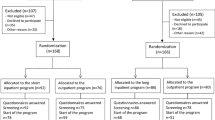
Purpose Mental health symptoms (MHSs) may affect people’s work capacity and lead to sickness absence and disability. Expectations and perceptions of illness have been shown to influence return to work (RTW) across health conditions, but we know little about illness perceptions and RTW-expectations in MHSs. The aim of this study was to investigate the association between illness perceptions and RTW-expectations in a group struggling with work participation due to MHSs. Methods Cross-sectional associations between illness perceptions and return to work expectations at baseline were analyzed for 1,193 participants who reported that MHSs affected their work participation. The study was part of a randomized controlled trial evaluating the effect of job focused Cognitive Behavioral Therapy (CBT) combined with supported employment (IPS). Participants were from a working age population with diverse job status. Results There was a strong and salient relationship between illness perceptions and RTW-expectations. When adjusting for demographic and clinical variables, the components consequences, personal control, identity and illness concern remained significantly associated with uncertain and negative RTW-expectations. Less illness understanding remained significantly associated with uncertain RTW-expectations, while timeline and emotional representations remained significantly associated with negative RTW-expectations. In the fully adjusted model only the consequences component (believing that illness has more severe consequences) remained significantly associated with RTW-expectations. Openly asked, participants reported work, personal relationships and stress as main causes of their illness. Conclusions In people with MHSs who struggle with work participation, perceptions and beliefs about their problems are strongly associated with their expectations to return to work.

Similar content being viewed by others
References
OECD. Sick on the Job? Myths and realities about mental health and work: OECD2012.
National Institute of Mental Health. Statistics—any disorder among adults. 2007.
Kessler RC, Demler O, Frank RG, Olfson M, Pincus HA, Walters EE, et al. Prevalence and treatment of mental disorders, 1990 to 2003. N Eng J Med. 2005;352(24):2515–23.
Prinz C, Andersson P, Förster M, Sickness DaW, 1 BtBV, 2006 O. Sickness, Disability and Work BREAKING THE BARRIERS Norway, Poland and Switzerland: Organisation for Economic Co-operation and Development 2006.
Dekkers-Sanchez PM, Hoving JL, Sluiter JK, Frings-Dresen MH. Factors associated with long-term sick leave in sick-listed employees: a systematic review. Occup Environ Med. 2008;65(3):153–7.
Waghorn G, Chant D. Employment restrictions among persons with ICD-10 anxiety disorders: characteristics from a population survey. J Anxiety D. 2005;19(6):642–57.
Leventhal H, Benyamini Y, Brownlee S, Diefenbach M, Leventhal EA, Patrick-Miller L, et al. Illness representations: theoretical foundations. In: Weinman JA, Petrie KJ, editors. Perceptions of health and illness. Amsterdam: Harwood Academic Publishers; 1997. p. 19–47.
Petrie KJ, Weinman J. Why illness perceptions matter. Clin Med. 2006;6(6):536–9.
Broadbent E, Kydd R, Sanders D, Vanderpyl J. Unmet needs and treatment seeking in high users of mental health services: role of illness perceptions. Aust NZ J P. 2008;42(2):147–53.
Petrie KJ, Cameron LD, Ellis CJ, Buick D, Weinman J. Changing illness perceptions after myocardial infarction: an early intervention randomized controlled trial. Psychos Med. 2002;64(4):580–6.
Hoving JL, van der Meer M, Volkova AY, Frings-Dresen MH. Illness perceptions and work participation: a systematic review. Int Arch Occup. 2010;83(6):595–605.
Petrie KJ, Broadbent E, Kydd R. Illness perceptions in mental health: issues and potential applications. J Ment Health. 2008;17(6):559–64.
Hoving JL, van der Meer M, Volkova AY, Frings-Dresen MHW. Illness perceptions and work participation: a systematic review. Int Arch Occup. 2010;83(6):595–605.
Sampere M, Gimeno D, Serra C, Plana M, Carlos Lopez J, Miguel Martinez J, et al. Return to work expectations of workers on long-term non-work-related sick leave. J Occup Rehabil. 2012;22(1):15–26.
Nieuwenhuijsen K, Verbeek JH, de Boer AG, Blonk RW, van Dijk FJ. Predicting the duration of sickness absence for patients with common mental disorders in occupational health care. Scand J Work Environ Health. 2006;32(1):67–74.
Mondloch MV, Cole DC, Frank JW. Does how you do depend on how you think you’ll do? A systematic review of the evidence for a relation between patients’ recovery expectations and health outcomes. Can Med Assoc J. 2001;165(2):174–9.
Laisne F, Lecomte C, Corbiere M. Biopsychosocial predictors of prognosis in musculoskeletal disorders: a systematic review of the literature. Disabil Rehabil. 2012;34(5):355–82.
Reme SE, Hagen EM, Eriksen HR. Expectations, perceptions, and physiotherapy predict prolonged sick leave in subacute low back pain. BMC Musculoskelet Disord. 2009;10(1):139.
Nijrolder I, van der Windt D, van der Horst H. Prediction of outcome in patients presenting with fatigue in primary care. Br J Gen Pract. 2009;59(561):e101–9.
Fleten N, Johnsen R, Førde OH. Length of sick leave—why not ask the sick-listed? Sick-listed individuals predict their length of sick leave more accurately than professionals. BMC Public Health. 2004. doi:10.1186/1471-2458-4-46.
Bandura A. Self-efficacy—toward a unifying theory of behavioral change. Psychol Rev. 1077;84(2):191–215.
Bandura A. Self-efficacy: the exercise of control. New York: WH Freeman; 1997.
Lagerveld SE, Blonk RWB, Brenninkmeijer V, Schaufeli WB. Return to work among employees with mental health problems: development and validation of a self-efficacy questionnaire. Work Stress. 2010;24(4):359–75.
Shaw WS, Reme SE, Linton SJ, Huang Y-H, Pransky G. 3(rd) place, PREMUS best paper competition: development of the return-to-work self-efficacy (RTWSE-19) questionnaire—psychometric properties and predictive validity. Scand J Work Environ Health. 2011;37(2):109–19.
Vaez M, Rylander G, Nygren Å, Åsberg M, Alexanderson K. Sickness absence and disability pension in a cohort of employees initially on long-term sick leave due to psychiatric disorders in Sweden. Soc Psychiatry Psychiatr Epidemiol. 2007;42(5):381–8.
Nielsen MBD, Madsen IEH, Bultmann U, Christensen U, Diderichsen F, Rugulies R. Predictors of return to work in employees sick-listed with mental health problems: findings from a longitudinal study. Eur J Public Health. 2011;21(6):806–11.
Andersen MF, Nielsen KM, Brinkmann S. Meta-synthesis of qualitative research on return to work among employees with common mental disorders. Scand J Work Environ Health. 2012;38(2):93–104.
Cornelius LR, van der Klink JJL, Groothoff JW, Brouwer S. Prognostic factors of long term disability due to mental disorders: a systematic review. J Occup Rehabil. 2011;21(2):259–74.
Cole DC, Mondloch MV, Hogg-Johnson S. Listening to injured workers: how recovery expectations predict outcomes—a prospective study. Can Med Assoc J. 2002;166(6):749–54.
Lagerveld SE, Blonk RWB, Brenninkmeijer V, Wijngaards-de Meij L, Schaufeli WB. Work-focused treatment of common mental disorders and return to work: a comparative outcome study. J Occup Health Psych. 2012;17(2):220–34.
Broadbent E, Petrie KJ, Main J, Weinman J. The brief illness perception questionnaire. J Psychosom Res. 2006;60(6):631–7.
Zigmond A, Snaith R. The hospital anxiety and depression scale. Acta Psychiatr Scand. 1983;676:361–70.
Eriksen HR, Ihlebaek C, Ursin H. A scoring system for subjective health complaints (SHC). Scand J Public Health. 1999;27(1):63–72.
Petrie KJ, Weinman J, Sharpe N, Buckley J. Role of patients’ view of their illness in predicting return to work and functioning after myocardial infarction: longitudinal study. BMJ. 1996;312(7040):1191–4.
Giri P, Poole J, Nightingale P, Robertson A. Perceptions of illness and their impact on sickness absence. Occup Med-Oxf. 2009;59(8):550–5.
Foster NE, Bishop A, Thomas E, Main C, Horne R, Weinman J. Illness perceptions of low back pain patients in primary care: what are they, do they change and are they associated with outcome? Pain. 2008;136(1–2):177–87.
Boot CRL, Heijmans M, van der Gulden JWJ, Rijken M. The role of illness perceptions in labor participation of the chronically ill. Int Arch Occup Environ Health. 2008;82(1):13–20.
Norrmen G, Svardsudd K, Andersson DK. The association of patient’s family, leisure time, and work situation with sickness certification in primary care in Sweden. Scand J Prim Health Care. 2010;28(2):76–81.
Stefansson C-G. Chapter 5.5: major public health problems - mental ill-health. Scand J Public Health. 2006;34(Suppl 67):87–103.
Ratcliffe D, MacLeod A, Sensky T. Anxiety in patients who have had a myocardial infarction: the maintaining role of perceived physical sensations and causal attributions. Behav Cogn Psychother. 2006;34(2):201–17.
Bratberg E, Dahl SA, Risa AE. ‘The double burden’—do combinations of career and family obligations increase sickness absence among women? Eur Sociol Rev. 2002;18(2):233–49.
Reme SE, Hagen EM, Eriksen HR. Expectations, perceptions, and physiotherapy predict prolonged sick leave in subacute low back pain. BMC Musculoskelet Disord. 2009;10. doi:10.1186/1471-2474-10-139.
Ihlebaek C, Brage S, Eriksen HR. Health complaints and sickness absence in Norway, 1996–2003. Occup Med (Lond). 2007;57(1):43–9.
Waddell G, Burton K, Aylward M. Work and common health problems. J Insur Med. 2007;39(2):109–20.
Petrie KJ, Broadbent E, Kydd R. Illness perceptions in mental health: issues and potential applications. J Ment Health. 2008;17(6):559–64.
Acknowledgments
This research was funded by the Norwegian Labor and Welfare Administration. Ingrid Blø Olsen helped to develop a framework for categorization of the causal item on the Brief Illness Perception Questionnaire and with the categorization of responses to this item.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Løvvik, C., Øverland, S., Hysing, M. et al. Association Between Illness Perceptions and Return-to-Work Expectations in Workers with Common Mental Health Symptoms. J Occup Rehabil 24, 160–170 (2014). https://doi.org/10.1007/s10926-013-9439-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10926-013-9439-8