Abstract
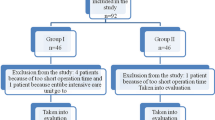
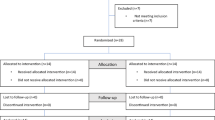
Hypothermia is common occurrence in patients undergoing colonic surgeries. We hypothesized that the underbody forced air warming blankets will be better than conventional over-body forced air warming blankets for prevention of hypothermia during laparoscopic colon surgeries. After ethics approval, sixty patients undergoing elective laparoscopic colon surgeries were randomly divided into two groups to receive warming by underbody forced air warming blanket (n = 30) or over-body forced air warming blanket (n = 30). In the operating room, epidural catheter was inserted and thereafter warming was started with the forced air warmer with temperature set at 44 °C. Intraoperatively core temperature (using nasopharyngeal probe), vitals, incidence of postoperative shivering and time to reach Aldrete Score of 10 in the postoperative period were recorded. The core temperature was higher with an underbody blanket at 60 min (36.1 ± 0.5 °C vs. 35.7 ± 0.5 °C, P = 0.005), 90 min (35.9 ± 0.5 °C vs. 35.6 ± 0.5 °C, P = 0.009), 120 min (35.9 ± 0.5 °C vs. 35.5 ± 0.4 °C, P = 0.007), and 150 min (35.9 ± 0.5 °C vs. 35.6 ± 0.4 °C, P = 0.011). In the post anesthesia care unit, the time to reach an Aldrete score of 10 was also less in the underbody blanket group (14.3 ± 2.5 min vs. 16.8 ± 3.6 min) (P = 0.003). However, there were no clinically meaningful differences in any outcome. Underbody and over-body blankets were comparably effective in preventing hypothermia in patients undergoing laparoscopic colorectal surgery under general anaesthesia.
Trial registration CTRI (2019/06/019,576). Date of Registration: June 2019, Prospectively registered.


Similar content being viewed by others
Data availability
Data is available.
References
Matsukawa T, Sessler DI, Sessler AM, Schroeder M, Ozaki M, Kurz A, et al. Heat flow and distribution during induction of general anesthesia. Anesthesiology. 1995;82(3):662–73.
Kurz A, Sessler DI, Lenhardt R. Perioperative normothermia to reduce the incidence of surgical-wound infection and shorten hospitalization. Study of Wound Infection and Temperature Group. N Engl J Med. 1996;334(19):1209–15.
Winkler M, Akça O, Birkenberg B, Hetz H, Scheck T, Arkiliç CF, et al. Aggressive warming reduces blood loss during hip arthroplasty. Anesth Analg. 2000;91(4):978–84.
Schmied H, Kurz A, Sessler DI, Kozek S, Reiter A. Mild hypothermia increases blood loss and transfusion requirements during total hip arthroplasty. Lancet Lond Engl. 1996;347(8997):289–92.
Frank SM, Fleisher LA, Breslow MJ, Higgins MS, Olson KF, Kelly S, et al. Perioperative maintenance of normothermia reduces the incidence of morbid cardiac events. A randomized clinical trial. JAMA. 1997;277(14):1127–34.
Lenhardt R, Marker E, Goll V, Tschernich H, Kurz A, Sessler DI, et al. Mild intraoperative hypothermia prolongs postanesthetic recovery. Anesthesiology. 1997;87(6):1318–23.
Just B, Trévien V, Delva E, Lienhart A. Prevention of intraoperative hypothermia by preoperative skin-surface warming. Anesthesiology. 1993;79(2):214–8.
Frank SM, Beattie C, Christopherson R, Norris EJ, Rock P, Parker S, et al. Epidural versus general anesthesia, ambient operating room temperature, and patient age as predictors of inadvertent hypothermia. Anesthesiology. 1992;77(2):252–7.
Pei L, Huang Y, Xu Y, Zheng Y, Sang X, Zhou X, et al. Effects of ambient temperature and forced-air warming on intraoperative core temperature: a factorial randomized trial. Anesthesiology. 2018;128(5):903–11.
Matika R, Ibrahim M, Patwardhan A. The importance of body temperature: an anesthesiologist’s perspective. Temperature 2016;4(1):9–12.
Moola S, Lockwood C. Effectiveness of strategies for the management and/or prevention of hypothermia within the adult perioperative environment. Int J Evid Healthc. 2011;9(4):337–45.
Hynson JM, Sessler DI. Intraoperative warming therapies: a comparison of three devices. J Clin Anesth. 1992;4(3):194–9.
Taguchi A, Ratnaraj J, Kabon B, Sharma N, Lenhardt R, Sessler DI, et al. Effects of a circulating-water garment and forced-air warming on body heat content and core temperature. Anesthesiology. 2004;100(5):1058–64.
Grocott HP, Mathew JP, Carver EH, Phillips-Bute B, Landolfo KP, Newman MF, et al. A randomized controlled trial of the Arctic Sun Temperature Management System versus conventional methods for preventing hypothermia during off-pump cardiac surgery. Anesth Analg. 2004;98(2):298–302.
Madrid E, Urrútia G, Roqué i Figuls M, Pardo-Hernandez H, Campos JM, Paniagua P, Maestre L, Alonso-Coello P. Active body surface warming systems for preventing complications caused by inadvertent perioperative hypothermia in adults. Cochrane Database Syst Rev. 2016;4:009016.
Miyazaki R, Hayamizu K, Hoka S. Underbody forced-air warmer blanket is superior to overbody blanket in preventing hypothermia during laparoscopic donor nephrectomy. Middle East J Anesthesiol. 2017;24:43–8.
Teodorczyk JE, Heijmans JH, van Mook WNKA, Bergmans DCJJ, Roekaerts PMHJ. Effectiveness of an underbody forced warm-air blanket during coronary artery bypass surgery in the prevention of postoperative hypothermia: a prospective controlled randomized clinical trial. Open J Anesthesiol. 2012;02:65–9.
Pu Y, Cen G, Sun J, Gong J, Zhang Y, Zhang M, et al. Warming with an underbody warming system reduces intraoperative hypothermia in patients undergoing laparoscopic gastrointestinal surgery: a randomized controlled study. Int J Nurs Stud. 2014;51:181–9.
Insler SR, Bakri MH, Nageeb F, Mascha E, Mihaljevic T, Sessler DI. An evaluation of a full-access underbody forced-air warming system during near-normothermic, on-pump cardiac surgery. Anesth Analg. 2008;106(3):746–50.
Alparslan V, Kus A, Hosten T, Ertargin M, Ozdamar D, Toker K, et al. Comparison of forced-air warming systems in prevention of intraoperative hypothermia. J Clin Monit Comput. 2018;32(2):343–9.
Funding
No external funding of any sort is involved.
Author information
Authors and Affiliations
Contributions
AG contributed to literature search, data acquisition, manuscript preparation and editing. NG contributed to concepts, design, literature search, manuscript editing and review. VK contributed to concept, manuscript editing and review. SB contributed to manuscript editing and review. RKM contributed to data analysis and statistics. RG, SJB, SM and SB contributed to manuscript editing and review. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
No conflict of interest is involved in the present study.
Ethics approval
Institutional ethical approval was obtained before start of the study (IEC-474/09.2018).
Informed consent
Written informed consent was obtained from all the patients prior to their inclusion in the study. We give our full free and voluntary consent to the Journal for the publication and copyright of the article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gulia, A., Gupta, N., Kumar, V. et al. Comparison of two forced air warming systems for prevention of intraoperative hypothermia in carcinoma colon patients: a prospective randomized study. J Clin Monit Comput 36, 215–220 (2022). https://doi.org/10.1007/s10877-020-00639-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-020-00639-z