Abstract
Background
While ethanol infusion into the vein of Marshall (VOM) as an adjunct to atrial fibrillation ablation has shown promise, adoption has been limited by the technical expertise required, unclear antiarrhythmic mechanism, and complication risk. Delayed pericardial effusions have been associated with ethanol infusion into the VOM in prior studies. Very little is known about how the procedural approach itself can impact the risk of delayed effusions. We sought to understand the incidence and influence of procedural technique on complications including delayed pericardial effusions from VOM ethanol infusion at a large single medical center.
Methods
A total of 275 atrial ablation cases wherein VOM ethanol infusion was attempted were identified from the time of the program’s inception in 2019 at Maine Medical Center (Portland, ME) until October of 2023. Cases were classified into phase I cases (early experience) and phase II cases (later experience) based upon temporal programmatic changes in the ethanol dose and infusion rate as well as the use of routine VOM venography. Procedural details and complications were adjudicated from the medical record.
Results
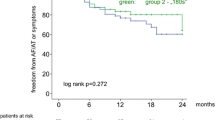
The overall VOM ethanol infusion success was 91.4%. Nine complications (3.3%) occurred in eight patients (2.9% of patients). These were more frequent in phase I (5.8%) compared to phase II (1.3%, p = 0.047). This difference was driven by a difference in delayed presentations of tamponade, which occurred in four patients in phase I (3.3%) and in no patients in phase II (0%, p = 0.037). Twelve-month estimated atrial arrhythmia freedom did not differ between groups (73.8% phase I vs 70.4% phase II, p = 0.24).
Conclusion
In our single-center experience, adjustments to the procedural approach with lower ethanol infusion rate and dosage, combined with utilizing selective VOM venography, associated with a lowering of complication rates and in particular, delayed pericardial tamponade.
Graphical Abstract







Similar content being viewed by others
References
Clarnette JA, Brooks AG, Mahajan R, Elliott AD, Twomey DJ, Pathak RK, Kumar S, Munawar DA, Young GD, Kalman JM, Lau DH, Sanders P. Outcomes of persistent and long-standing persistent atrial fibrillation ablation: a systematic review and meta-analysis. Europace : European pacing, arrhythmias, and cardiac electrophysiology : journal of the working groups on cardiac pacing, arrhythmias, and cardiac cellular electrophysiology of the European Society of Cardiology. 2018;20:f366–76.
Verma A, Jiang CY, Betts TR, et al. Approaches to catheter ablation for persistent atrial fibrillation. N Engl J Med. 2015;372:1812–22.
Valderrabano M, Peterson LE, Swarup V, et al. Effect of catheter ablation with vein of marshall ethanol infusion vs catheter ablation alone on persistent atrial fibrillation: the VENUS randomized clinical trial. JAMA. 2020;324:1620–8.
Pambrun T, Denis A, Duchateau J, Sacher F, Hocini M, Jais P, Haissaguerre M, Derval N. MARSHALL bundles elimination, Pulmonary veins isolation and Lines completion for ANatomical ablation of persistent atrial fibrillation: MARSHALL-PLAN case series. J Cardiovascular Electrophysiol. 2019;30:7–15.
Derval N, Duchateau J, Denis A, et al. Marshall bundle elimination, Pulmonary vein isolation, and Line completion for ANatomical ablation of persistent atrial fibrillation (Marshall-PLAN): prospective, single-center study. Heart Rhythm. 2021;18:529–37.
Leyton-Mange JS, Tandon K, Sze EY, Carpenter CM, Sesselberg HW. The Maine vein of Marshall ethanol experience: learning curve and safety. J Interventional Cardiac Electrophysiol: Int J arrhythmias Pacing. 2023;66:661–71.
Kamakura T, Derval N, Duchateau J, et al. Vein of Marshall ethanol infusion: feasibility, pitfalls, and complications in over 700 patients. Circul Arrhythmia Electrophysiol. 2021;14:e010001.
Krisai P, Pambrun T, Nakatani Y, et al. How to perform ethanol ablation of the vein of Marshall for treatment of atrial fibrillation. Heart Rhythm. 2021;18:1083–7.
Motoki K, Harada T, Hosokawa S, Hara T, Yamamoto K, Kishi K. Very delayed pericarditis associated with ethanol ablation of the vein of Marshall for treatment of atrial fibrillation. HeartRhythm Case Reports. 2023;9:255–7.
Hussein A, Das M, Riva S, et al. Use of ablation index-guided ablation results in high rates of durable pulmonary vein isolation and freedom from arrhythmia in persistent atrial fibrillation patients: the PRAISE study results. Circulation Arrhythmia Electrophysiol. 2018;11:e006576.
Valderrabano M, Morales PF, Rodriguez-Manero M, Lloves C, Schurmann PA, Dave AS. The human left atrial venous circulation as a vascular route for atrial pharmacological therapies: effects of ethanol infusion. JACC Clin Electrophysiol. 2017;3:1020–32.
Zhang HD, Ding L, Yu FY, Mi LJ, Zhang K, Weng SX, Jiang ZH, Tang M. Angiographic assessment of vein of Marshall in atrial fibrillation: implications for identification and cannulation. Heliyon. 2023;9:21266.
Landra F, Nesti M, Garibaldi S, et al. A proposed index of myocardial staining for vein of Marshall ethanol infusion: an Italian single-center experience. Journal of interventional cardiac electrophysiology : an international journal of arrhythmias and pacing Jan 11 2024.
Lador A, Peterson LE, Swarup V, et al. Determinants of outcome impact of vein of Marshall ethanol infusion when added to catheter ablation of persistent atrial fibrillation: a secondary analysis of the VENUS randomized clinical trial. Heart Rhythm. 2021;18:1045–54.
Davong B, Adelino R, Delasnerie H, Albenque JP, Combes N, Cardin C, Voglimacci-Stephanopoli Q, Combes S, Boveda S. Pulsed-field ablation on mitral isthmus in persistent atrial fibrillation: preliminary data on efficacy and safety. JACC Clin Electrophysiol. 2023;9:1070–81.
Reddy VY, Peichl P, Anter E, et al. A focal ablation catheter toggling between radiofrequency and pulsed field energy to treat atrial fibrillation. JACC Clin Electrophysiol. 2023;9:1786–801.
Reddy VY, Petru J, Funasako M, Kopriva K, Hala P, Chovanec M, Janotka M, Kralovec S, Neuzil P. Coronary arterial spasm during pulsed field ablation to treat atrial fibrillation. Circulation. 2022;146:1808–19.
Acknowledgements
The authors would like to acknowledge our colleagues and our EP lab staff for their assistance in reviewing this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. J.L.M. and A.D.H. performed the data collection. J.L.M. performed the analysis and preparation of the first draft of the manuscript. All authors commented on subsequent versions as well as read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval
This study was approved by the Maine Medical Center Institutional Review Board and performed in accordance with the Declaration of Helsinki.
Consent to participate
This is a retrospective study performed by chart review, and as such, informed consent was waived by the Institutional Review Board.
Conflict of interest
J.L.M. has received prior speaking fees from Sanofi Aventis and consulting Fees from Biosense Webster. The remaining authors have no relevant financial or non-financial interests to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Leyton-Mange, J.S., Haskell, A.D., Tandon, K. et al. Protocol modifications reduce risk of delayed pericardial effusions after vein of Marshall ethanol infusion: follow-up from the Maine experience. J Interv Card Electrophysiol (2024). https://doi.org/10.1007/s10840-024-01842-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10840-024-01842-7