Abstract
Background
To predict the outflow tract ventricular arrhythmias (OTVA) site of origin (SOO) before the ablation procedure has important practical implications. The present study sought to prospectively evaluate the accuracy of a clinical and electrocardiographic hybrid algorithm (HA) for the prediction of OTVAs-SOO, and at the same time to develop and to prospectively validate a new score with improved discriminatory capacity.
Methods
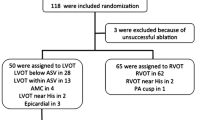
In this multicenter study, we prospectively enrolled consecutive patients referred for OTVA ablation (N = 202), and we divided them in a derivation sample and a validation cohort. Surface ECGs during OTVA were analyzed to compare previous published ECG-only criteria and to develop a new score.
Results
In the derivation sample (N = 105), the correct prediction rate of HA and ECG-only criteria ranged from 74 to 89%. R-wave amplitude in V3 was the best ECG parameter for discriminating LVOT origin in V3 precordial transition (V3PT) patients, and was incorporated to the novel weighted hybrid score (WHS). WHS correctly classified 99 (94.2%) patients, presenting 90% sensitivity and 96% specificity (AUC 0.97) in the entire population; WHS mantained a 87% sensitivity and 91% specificity (AUC 0.95) in patients with V3PT subgroup. The high discriminatory capacity was confirmed in the validation sample (N = 97): the WHS exhibited an AUC (0.93), and a WHS ≥ 2 allowed a correct prediction of LVOT origin in 87 (90.0%) cases, yielding a sensitivity of 87% and specificity of 90%; moreover, the V3PT subgroup showed an AUC of 0.92, and a punctuation ≥ 2 predicted an LVOT origin with a sensitivity of 94% and specificity of 78%.
Conclusions
The novel hybrid score has proved to accurately anticipate the OTVA’s origin, even in those with a V3 precordial transition.
Graphical Abstract
A Weighted hybrid score. B Typical examples of the use of the weighted hybrid score. C ROC analysis of WHS and previous ECG criteria for prediction of LVOT origin in the derivation cohort. D ROC analysis of WHS and previous ECG criteria for prediction of LVOT origin in the V3 precordial transition OTVA subgroup





Similar content being viewed by others
Data Availability
Data could be available upon request.
References
Mont L, Seixas T, Brugada P, Brugada J, Simonis F, Rodriguez LM, et al. Clinical and electrophysiologic characteristics of exercise-related idiopathic ventricular tachycardia. Am J Cardiol. 1991;68(9):897–900.
Holmqvist F, Kesek M, Englund A, Blomstrom-Lundqvist C, Karlsson LO, Kenneback G, Poci D, et al. A decade of catheter ablation of cardiac arrhythmias in Sweden: Ablation practices and outcomes. Eur Heart J. 2019;40(10):820–30.
Penela D, Van Huls Van Taxis C, Aguinaga L, Fernandez-Armenta J, Mont L, Castel MA, et al. Neurohormonal, structural, and functional recovery pattern after premature ventricular complex ablation is independent of structural heart disease status in patients with depressed left ventricular ejection fraction: A prospective multicenter study. J Am Coll Cardiol. 2013;62(13):1195–202.
Peichl P, Wichterle D, Pavlu L, Cihak R, Aldhoon B, Kautzner J. Complications of catheter ablation of ventricular tachycardia: A single-center experience. Circ Arrhythm Electrophysiol. 2014;7(4):684–90.
Betensky BP, Park RE, Marchlinski FE, Hutchinson MD, Garcia FC, Dixit S, et al. The V(2) transition ratio: A new electrocardiographic criterion for distinguishing left from right ventricular outflow tract tachycardia origin. J Am Coll Cardiol. 2011;57(22):2255–62.
Ouyang F, Fotuhi P, Ho SY, Hebe J, Volkmer M, Goya M, et al. Repetitive monomorphic ventricular tachycardia originating from the aortic sinus cusp: electrocardiographic characterization for guiding catheter ablation. J Am Coll Cardiol. 2002;39(3):500–8.
Yoshida N, Yamada T, McElderry HT, Inden Y, Shimano M, Murohara T, et al. A novel electrocardiographic criterion for differentiating a left from right ventricular outflow tract tachycardia origin: The V2s/V3r index. J Cardiovasc Electrophysiol. 2014;25(7):747–53.
**e S, Kubala M, Liang JJ, Hayashi T, Park J, Padros IL, et al. Lead I R-wave amplitude to differentiate idiopathic ventricular arrhythmias with left bundle branch block right inferior axis originating from the left versus right ventricular outflow tract. J Cardiovasc Electrophysiol. 2018;29(11):1515–22.
Yoshida N, Inden Y, Uchikawa T, Kamiya H, Kitamura K, Shimano M, et al. Novel transitional zone index allows more accurate differentiation between idiopathic right ventricular outflow tract and aortic sinus cusp ventricular arrhythmias. Heart Rhythm. 2011;8(3):349–56.
Penela D, De Riva M, Herczku C, Catto V, Pala S, Fernandez-Armenta J, et al. An easy-to-use, operator-independent, clinical model to predict the left vs. right ventricular outflow tract origin of ventricular arrhythmias. Europace. 2015;17(7):1122–8.
Gabriels JK, Abdelrahman M, Nambiar L, Kim J, Ip JE, Thomas G, Liu CF, et al. Reappraisal of electrocardiographic criteria for localization of idiopathic outflow region ventricular arrhythmias. Heart Rhythm. 2021;18(11):1959–65.
Priori SG, Blomstrom-Lundqvist C, Mazzanti A, Blom N, Borggrefe M, Camm J, et al. Esc Guidelines for the Management of Patients with Ventricular Arrhythmias and the Prevention of Sudden Cardiac Death: The Task Force for the Management of Patients with Ventricular Arrhythmias and the Prevention of Sudden Cardiac Death of the European Society of Cardiology (Esc). Endorsed By: Association for European Paediatric and Congenital Cardiology (Aepc). Eur Heart J. 2015;36(41):2793–867.
Jauregui B, Penela D, Fernandez-Armenta J, Acosta J, Teres C, Soto-Iglesias D, et al. Impact of a predefined pacemap** protocol use for ablation of infrequent premature ventricular complexes: a prospective, multicenter study. Heart Rhythm. 2021;18(10):1709–16.
Tanaka Y, Tada H, Ito S, Naito S, Higuchi K, Kumagai K, et al. Gender and age differences in candidates for radiofrequency catheter ablation of idiopathic ventricular arrhythmias. Circ J. 2011;75(7):1585–91.
Acosta J, Penela D, Herczku C, Macias Y, Andreu D, Fernandez-Armenta J, et al. Impact of earliest activation site location in the septal right ventricular outflow tract for identification of left vs right outflow tract origin of idiopathic ventricular arrhythmias. Heart Rhythm. 2015;12(4):726–34.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by Ethics Committee of each center.
Conflict of interest
A. Berruezo is stockholder of Galgo Medical. D. Soto-Iglesias is an employee of Biosense Webster. A. Berruezo received speaker fees from Biosense and research grants from Biotronik. P. Francia received speaker fees, research and educational grants from Boston Scientific and Abbott. The other authors have no other relevant affiliations or financial involvement with any organization or entity with a financial interest in or financial conflict with the subject matter or materials discussed in the manuscript apart from those disclosed.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key messages
• To anticipate the OTVA’s site of origin has relevant implications for ablation. Several ECG algorithms had been proposed but, until now, baseline clinical information has been disregarded for this purpose. .
• This study supports that patients with LVOT-OTVA have a different clinical profile than those with RVOT-OTVA. The present study translates this different clinical profile into a practical tool for choosing the first chamber to be mapped during catheter ablation procedures.
• A simple-to-use score combining electrocardiographic and clinical information correctly classified 99 (94.2%) patients, presenting 90% sensitivity and 96% specificity (AUC 0.97), maintaining his discriminatory capacity in V3 precordial transition subgroup (AUC 0.95).
• This is the first study that prospectively evaluates the usefulness of a predefined algorithm for identifying the site of origin, and hence for choosing the vascular access, in consecutive patients referred for OTVA ablation.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Penela, D., Falasconi, G., Carreño, J.M. et al. A hybrid clinical and electrocardiographic score to predict the origin of outflow tract ventricular arrhythmias. J Interv Card Electrophysiol 66, 1877–1888 (2023). https://doi.org/10.1007/s10840-023-01507-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-023-01507-x