Abstract
Purpose
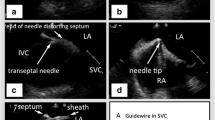
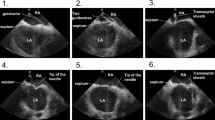
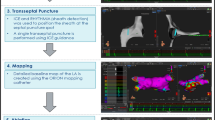
There is growing interest in performing fluoroless radiofrequency ablation (RFA) for atrial fibrillation (AF) due to the increasing awareness of risk associated with radiation exposure of patients and professional staff. The present study aimed to evaluate the feasibility, safety, and efficacy of a stepwise transesophageal echocardiography (TEE)–guided zero-fluoroscopy approach (ZFA) for RFA.
Methods
Consecutive patients (n = 111) referred for AF-ablation were prospectively enrolled with intention to RFA with ZFA. Procedural outcomes were compared with historical controls (HCs) after 1:1 propensity score matching. ZFA success was considered when no X-ray was utilized to perform the whole procedure.
Results
ZFA success was achieved in 80 (72%) procedures. BMI > 35 kg/m2 resulted in the only independent predictor of ZFA failure (OR = 6.10, 95% CI 1.15–46.49, p = 0.04). In comparison to HCs, a significant reduction in radiation exposure was observed in the ZFA group: fluoroscopy time (3 vs. 63 s, p < 0.001), total emitted fluoroscopy dose (0.2 vs. 6.0 mGy, p < 0.001), dose area product (0.04 vs. 1.4 Gy*cm2, p < 0.001), and effective dose (0.8 vs. 27.2 mSv*100, p < 0.001). Complete pulmonary vein isolation was achieved in all procedures. No difference was observed between the groups in in-hospital complication rate (0.9% vs. 1.8%, p = 0.99).
Conclusions
This is the largest study proving procedural feasibility, safety, and efficacy of TEE-guided AF-ablation with a complete or near-complete avoidance of radiological exposure, without using intracardiac echocardiography.




Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author, upon reasonable request.
References
Calkins H, Hindricks G, Cappato R, Kim YH, Saad EB, Aguinaga L, Akar JG, Badhwar V, Brugada J, Camm J, Chen PS, Chen SA, Chung MK, Nielsen JC, Curtis AB, Davies DW, Day JD, d’Avila A, de Groot Nmsn, Di Biase L, Duytschaever M, Edgerton JR, Ellenbogen KA, Ellinor PT, Ernst S, Fenelon G, Gerstenfeld EP, Haines DE, Haissaguerre M, Helm RH, Hylek E, Jackman WM, Jalife J, Kalman JM, Kautzner J, Kottkamp H, Kuck KH, Kumagai K, Lee R, Lewalter T, Lindsay BD, Macle L, Mansour M, Marchlinski FE, Michaud GF, Nakagawa H, Natale A, Nattel S, Okumura K, Packer D, Pokushalov E, Reynolds MR, Sanders P, Scanavacca M, Schilling R, Tondo C, Tsao HM, Verma A, Wilber DJ, Yamane T. 2017 Hrs/Ehra/Ecas/Aphrs/Solaece expert consensus statement on catheter and surgical ablation of atrial fibrillation: executive summary. Heart Rhythm. 2017;14(10):e445–94.
Lickfett L, Mahesh M, Vasamreddy C, Bradley D, Jayam V, Eldadah Z, Dickfeld T, Kearney D, Dalal D, Luderitz B, Berger R, Calkins H. Radiation exposure during catheter ablation of atrial fibrillation. Circulation. 2004;110(19):3003–10.
Di Cori A, Zucchelli G, Segreti L, Barletta V, Viani S, Paperini L, Della Tommasina V, Cellamaro T, Vecchi A, Soldati E, Bongiorni MG. Predictors of zero X ray procedures in supraventricular arrhythmias ablation. Int J Cardiovasc Imaging. 2020;36(9):1599–607.
Cha MJ, Lee E, Oh S. Zero-fluoroscopy catheter ablation for atrial fibrillation: a transitional period experience. J Arrhythm. 2020;36(6):1061–7.
Scaglione M, Ebrille E, Caponi D, Battaglia A, Di Donna P, Anselmino M, Peyracchia M, Mazzucchi P, Cerrato N, Ferraris F, Castagno D, Lamberti F, Gaita F. Zero-fluoroscopy atrial fibrillation ablation in the presence of a patent foramen ovale: a multicentre experience. J Cardiovasc Med (Hagerstown). 2020;21(4):292–8.
Hindricks G, Potpara T, Dagres N, Arbelo E, Bax JJ, Blomstrom-Lundqvist C, Boriani G, Castella M, Dan GA, Dilaveris PE, Fauchier L, Filippatos G, Kalman JM, La Meir M, Lane DA, Lebeau JP, Lettino M, Lip GYH, Pinto FJ, Thomas GN, Valgimigli M, Van Gelder IC, Van Putte BP, Watkins CL, E. S. C. Scientific Document Group. 2020 ESC Guidelines for the diagnosis and management of atrial fibrillation developed in collaboration with the European Association for Cardio-Thoracic Surgery (Eacts). Eur Heart J. 2021;42(5):373–498.
Teres C, Soto-Iglesias D, Penela D, Jauregui B, Ordonez A, Chauca A, Huguet M, Ramirez C, Oller G, Jornet A, Palet J, Santana D, Panaro A, Maldonado G, de Leon G, Gualis B, Jimenez-Britez G, Evangelista A, Carballo J, Ortiz-Perez JT, Berruezo A. Left atrial wall thickness of the pulmonary vein reconnection sites during atrial fibrillation redo procedures. Pacing Clin Electrophysiol (2021)
Gabriels J, Donnelly J, Khan M, Anca D, Beldner S, Willner J, Epstein LM, Patel A. High-frequency, low tidal volume ventilation to improve catheter stability during atrial fibrillation ablation. JACC Clin Electrophysiol. 2019;5(10):1224–6.
Pambrun T, Combes S, Sousa P, Bloa ML, El Bouazzaoui R, Grand-Larrieu D, Thompson N, Martin R, Combes N, Boveda S, Haissaguerre M, Albenque JP. Contact-force guided single-catheter approach for pulmonary vein isolation: feasibility, outcomes, and cost-effectiveness. Heart Rhythm. 2017;14(3):331–8.
Pani A, Giuseppina B, Bonanno C, GraziaBongiorni M, Bottoni N, Brambilla R, Ceglia S, Della Bella P, Vito G, Malaspina D, Menardi E, Napoli V, Negroni MS, Ocello S, Orsida D, Pandozi C, Pedretti S, Penela D, Pepi P, Rossi L, Rovaris G, Scopinaro A, Vincenti A, Viola G, Zaca V, Zoppo F, Vergara P. Predictors of zero X-ray ablation for supraventricular tachycardias in a nationwide multicenter experience. Circ Arrhythm Electrophysiol. 2018;11(3):e005592.
Limacher MC, Douglas PS, Germano G, Laskey WK, Lindsay BD, McKetty MH, Moore ME, Park JK, Prigent FM, Walsh MN. ACC expert consensus document. Radiation Safety in the Practice of Cardiology. American College of Cardiology. J Am Coll Cardiol. 1998;31(4):892–913.
Casella M, Dello Russo A, Pelargonio G, Del Greco M, Zingarini G, Piacenti M, Di Cori A, Casula V, Marini M, Pizzamiglio F, Zucchetti M, Riva S, Russo E, Narducci ML, Soldati E, Panchetti L, Startari U, Bencardino G, Perna F, Santangeli P, Di Biase L, Cichocki F, Fattore G, Bongiorni M, Picano E, Natale A, Tondo C. Near zerO fluoroscopic exPosure during catheter ablAtion of supRavenTricular ArrhYthmias: the NO-PARTY multicentre randomized trial. Europace. 2016;18(10):1565–72.
Sommer P, Bertagnolli L, Kircher S, Arya A, Bollmann A, Richter S, Rolf S, Hindricks G. Safety profile of near-zero fluoroscopy atrial fibrillation ablation with non-fluoroscopic catheter visualization: experience from 1000 consecutive procedures. Europace. 2018;20(12):1952–8.
Haegeli LM, Stutz L, Mohsen M, Wolber T, Brunckhorst C, On CJ, Duru F. Feasibility of zero or near zero fluoroscopy during catheter ablation procedures. Cardiol J. 2019;26(3):226–32.
Shoemaker MB, Muhammad R, Farrell M, Parvez B, White BW, Streur M, Stubblefield T, Rytlewski J, Parvathaneni S, Nagarakanti R, Roden DM, Saavedra P, Ellis C, Whalen SP, Darbar D. Relation of morbid obesity and female gender to risk of procedural complications in patients undergoing atrial fibrillation ablation. Am J Cardiol. 2013;111(3):368–73.
Russo G, Taramasso M, Maisano F. Transseptal puncture: procedural guidance, challenging situations and complications management. EuroIntervention (2021)
Clark J, Bockoven JR, Lane J, Patel CR, Smith G. Use of three-dimensional catheter guidance and trans-esophageal echocardiography to eliminate fluoroscopy in catheter ablation of left-sided accessory pathways. Pacing Clin Electrophysiol. 2008;31(3):283–9.
Sciahbasi A, Ferrante G, Fischetti D, Miklin DJ, Sarandrea A, Schirripa V, Guarracini F, Arya A, Loreni G, Bruni A, Rigattieri S, Marini M, Vagnarelli S, Scevola G, Reimers B, Hindricks G, Cohen M. Radiation dose among different cardiac and vascular invasive procedures: the RODEO study. Int J Cardiol. 2017;240:92–6.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Giulio Falasconi, Diego Penela, and David Soto-Iglesias. The first draft of the manuscript was written by Giulio Falasconi, and all authors commented on the previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the local Ethics Committee.
Conflict of interest
Dr. Berruezo is a stockholder of ADAS 3D Medical. Dr. Soto-Iglesias is an employee of Biosense Webster. The other authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file2 (MP4 6542 KB)
Supplementary file3 (MP4 3483 KB)
Supplementary file4 (MP4 10801 KB)
Rights and permissions
About this article
Cite this article
Falasconi, G., Penela, D., Soto-Iglesias, D. et al. A standardized stepwise zero-fluoroscopy approach with transesophageal echocardiography guidance for atrial fibrillation ablation. J Interv Card Electrophysiol 64, 629–639 (2022). https://doi.org/10.1007/s10840-021-01086-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-021-01086-9