Abstract
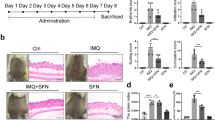
Psoriasis is a common immune-mediated skin disease characterized by abnormally reactive inflammation and epidermal hyperplasia. Previous studies have shown melatonin (MLT) has powerful anti-inflammatory effects. The mechanisms that MLT regulates psoriasis-associated skin inflammation remain unclear. Here, in imiquimod-induced psoriasis-like mice, MLT supplementation reduced skin inflammation and corrected the Th17/Treg cell imbalance. Network pharmacology and proteome sequencing analyses revealed that MLT attenuates the inflammatory response in the skin of psoriatic mice by inhibiting the PI3K/Akt signaling pathway. Overall, the data suggest that MLT has a protective effect against psoriasis-like inflammation.





Similar content being viewed by others
Availability of Data and Materials
The data that support the findings of this study are available on request from the corresponding author, HY, upon reasonable request.
Abbreviations
- IMQ:
-
Imiquimod
- MLT:
-
Melatonin
- MTX:
-
Methotrexate
- RT-qPCR:
-
Real-time quantitative PCR
- Ki67:
-
Antigen KI67
- Th:
-
T helper type
- Treg:
-
Regulatory T cell
- PI3K:
-
Phosphatidylinositol 3-kinase
- Akt:
-
Protein kinase B
- CON:
-
Control
- PS:
-
Psoriasis
- MLTL:
-
Low-dose of melatonin
- MLTH:
-
High-dose of melatonin
- LY294002:
-
PI3k/Akt inhibitor
- H&E:
-
Hematoxylin and eosin
- PASI:
-
Psoriasis severity index
- PBS:
-
Phosphate-buffered saline
- KEGG:
-
Kyoto Encyclopedia of Genes and Genomes
References
Michalek, I.M., B. Loring, and S.M. John. 2017. A systematic review of worldwide epidemiology of psoriasis. Journal of the European Academy of Dermatology and Venereology 31 (205–212): 674. https://doi.org/10.1111/jdv.13854.
Greb, Jacqueline E., Ari M. Goldminz, James T. Elder, Mark G. Lebwohl, Dafna D. Gladman, Jashin J. Wu, Nehal N. Mehta, Andrew Y. Finlay, and Alice B. Gottlieb. 2016. Psoriasis. Nature Reviews Disease Primers 2: 16082. https://doi.org/10.1038/nrdp.2016.82.
Karamehic, Jasenko, Lamija Zecevic, Halima Resic, Majda Jukic, Tomislav Jukic, Ognjen Ridjic, Mirsad Panjeta, and Jozo Coric. 2014. Immunophenotype lymphocyte of peripheral blood in patients with psoriasis. Medical Archives 68 (236): 20. https://doi.org/10.5455/medarh.2014.68.236-238.
Keijsers, R.R.M.C., H.M.J. Van Der Velden, P.E.J. Van Erp, R.T. De Boer-van Huizen, I. Joosten, H.J.P.M. Koenen, and P.C.M. Van De Kerkhof. 2013. Balance of Treg vs. T-helper cells in the transition from symptomless to lesional psoriatic skin: balance of Treg vs. T-helper cells in psoriasis. British Journal of Dermatology 168 (1294–1302): 41. https://doi.org/10.1111/bjd.12236.
Zhang, L., Y. Li, X. Yang, J. Wei, S. Zhou, Z. Zhao, J. Cheng, et al. 2016. Characterization of Th17 and FoxP3+ Treg cells in paediatric psoriasis patients. Scandinavian Journal of Immunology 83 (174–180): 56. https://doi.org/10.1111/sji.12404.
Zhang, L., X.-Q. Yang, J. Cheng, R.-S. Hui, and T.-W. Gao. 2010. Increased Th17 cells are accompanied by FoxP3+ Treg cell accumulation and correlated with psoriasis disease severity. Clinical Immunology 135 (108–117): 177. https://doi.org/10.1016/j.clim.2009.11.008.
Ando, N., Y. Nakamura, R. Aoki, K. Ishimaru, H. Ogawa, K. Okumura, S. Shibata, S. Shimada, and A. Nakao. 2015. Circadian gene clock regulates psoriasis-like skin inflammation in mice. Journal of Investigative Dermatology 135 (3001–3008): 51. https://doi.org/10.1038/jid.2015.316.
Németh, V., S. Horváth, Á. Kinyó, R. Gyulai, and Z. Lengyel. 2021. Expression patterns of clock gene mRNAs and clock proteins in human psoriatic skin samples. International Journal of Molecular Sciences 23: 121.5. https://doi.org/10.3390/ijms23010121.
Li, W.-Q., A.A. Qureshi, E.S. Schernhammer, and J. Han. 2013. Rotating night-shift work and risk of psoriasis in US women. Journal of Investigative Dermatology 133 (565–567): 56. https://doi.org/10.1038/jid.2012.285.
Nguyen, S., H. Bahakeem, A. Alkhalifah, M. Cavalié, F. Boukari, H. Montaudié, J.-P. Lacour, and T. Passeron. 2017. Topical corticosteroids application in the evening is more effective than in the morning in psoriasis: results of a prospective comparative study. Journal of the European Academy of Dermatology and Venereology 31: e263-e264.5. https://doi.org/10.1111/jdv.14027.
Kartha, L.B., L. Chandrashekar, M. Rajappa, V. Menon, D.M. Thappa, and P.H. Ananthanarayanan. 2014. Serum melatonin levels in psoriasis and associated depressive symptoms. Clinical Chemistry and Laboratory Medicine (CCLM) 52: 21. https://doi.org/10.1515/cclm-2013-0957.
Zhang, L., J.-T. Zhang, Y. Huang, G.-K. Zhou, Y. Zhou, J.-P. Yang, and T. Liu. 2022. Melatonin attenuates acute and chronic itch in mice: the antioxidant and anti-inflammatory effects of melatonin receptors. Annals of Translational Medicine 10: 972–972. https://doi.org/10.21037/atm-22-3804.
Chen, S., H. Kesheng Han, J.C. Li, Y. Yang, W. Hezhen, and Q. Wei. 2017. Isogarcinol extracted from Garcinia mangostana L. ameliorates imiquimod-induced psoriasis-like skin lesions in mice. Journal of Agricultural and Food Chemistry 65: 846-857.21. https://doi.org/10.1021/acs.jafc.6b05207.
Fischer, Tobias W., Konrad Kleszczyński, Lena H. Hardkop, Nathalie Kruse, and Detlef Zillikens. 2013. Melatonin enhances antioxidative enzyme gene expression (CAT, GPx, SOD), prevents their UVR-induced depletion, and protects against the formation of DNA damage (8-hydroxy-2’-deoxyguanosine) in ex vivo human skin. Journal of Pineal Research 54: 303–312. https://doi.org/10.1111/jpi.12018.
Tiirikainen, M.L., A. Woetmann, H. Norsgaard, L.F. Santamaria-Babí, and P. Lovato. 2020. Ex vivo culture of lesional psoriasis skin for pharmacological testing. Journal of Dermatological Science 97: 109-116.2. https://doi.org/10.1016/j.jdermsci.2019.12.010.
Wang, J., C. Wang, L. Liu, S. Hong, R. Yi, X. Sun, J. Chen, et al. 2023. Adverse events associated with anti-IL-17 agents for psoriasis and psoriatic arthritis: a systematic sco** review. Frontiers in Immunology 14: 993057. https://doi.org/10.3389/fimmu.2023.993057.
Pinilla Martín, B., A. Sánchez Velázquez, C. Vico Alonso, and R. Rivera Díaz. 2021. De un anti-IL-17 a otro: dar una segunda oportunidad o cambiar de diana. Actas Dermo-Sifiliográficas 112: 473-475.0. https://doi.org/10.1016/j.ad.2019.12.008.
Fagiani, F., D. Di Marino, A. Romagnoli, C. Travelli, D. Voltan, L. Di Cesare, M.R. Mannelli, S. Govoni, and C. Lanni. 2022. Molecular regulations of circadian rhythm and implications for physiology and diseases. Signal Transduction and Targeted Therapy 7: 41–74. https://doi.org/10.1038/s41392-022-00899-y.
Yu, X., D. Rollins, K.A. Ruhn, J.J. Stubblefield, C.B. Green, M. Kashiwada, P.B. Rothman, J.S. Takahashi, and L.V. Hooper. 2013. T H 17 cell differentiation is regulated by the circadian clock. Science 342: 727-730.339. https://doi.org/10.1126/science.1243884.
Luengas-Martinez, Andrea, Ralf Paus, Mudassar Iqbal, Laura Bailey, David W. Ray, and Helen S. Young. 2022. Circadian rhythms in psoriasis and the potential of chronotherapy in psoriasis management. Experimental Dermatology 31: 1800-1809.9. https://doi.org/10.1111/exd.14649.
Ren, W., G. Liu, S. Chen, J. Yin, J. Wang, B. Tan, W. Guoyao, et al. 2017. Melatonin signaling in T cells: functions and applications. Journal of Pineal Research 62: e12394. https://doi.org/10.1111/jpi.12394.
Reiter, R.J., S. Rosales-Corral, D.X. Tan, M.J. Jou, A. Galano, and X. Bing. 2017. Melatonin as a mitochondria-targeted antioxidant: one of evolution’s best ideas. Cellular and Molecular Life Sciences 74: 3863-3881.24. https://doi.org/10.1007/s00018-017-2609-7.
Houshang, N., K. Reza, S. Masoud, E. Ali, R. Mansour, and A. Vaisi-Raygani. 2014. Antioxidant status in patients with psoriasis: antioxidant in patients with psoriasis. Cell Biochemistry and Function 32: 268-273.72. https://doi.org/10.1002/cbf.3011.
Kizilyel, O., and N Akdeni̇Z, M Sami Meti̇N, Ö Faruk Elmas. 2019. Investigation of oxidant and antioxidant levels in patients with psoriasis. Turkish Journal of Medical Sciences 49: 1085–108811. https://doi.org/10.3906/sag-1807-257.
Zhang, Z.Q., S.B. Tang, Y.Y. Jiang, F.Y. Long, F. He, J. Liu, G. ShouYong, L. Yan, and Z.Q. Yin. 2022. Oxidative stress induces meiotic defects of oocytes in a mouse psoriasis model. Cell Death & Disease 13: 474.2. https://doi.org/10.1038/s41419-022-04948-w.
Scuderi, S.A., L. Cucinotta, A. Filippone, M. Lanza, M. Campolo, I. Paterniti, and E. Esposito. 2022. Effect of melatonin on psoriatic phenotype in human reconstructed skin model. Biomedicines 10: 752.2. https://doi.org/10.3390/biomedicines10040752.
Farez, M.F., I.D. Mascanfroni, S.P. Méndez-Huergo, A. Yeste, G. Murugaiyan, L.P. Garo, M.E. Balbuena Aguirre, et al. 2015. Melatonin contributes to the seasonality of multiple sclerosis relapses. Cell 162: 1338-1352.245. https://doi.org/10.1016/j.cell.2015.08.025.
Juntilla, M.M., and G.A. Koretzky. 2008. Critical roles of the PI3K/Akt signaling pathway in T cell development. Immunology Letters 116 (104–110): 134. https://doi.org/10.1016/j.imlet.2007.12.008.
Herrero-Sánchez, M.C., C. Rodríguez-Serrano, J. Almeida, L.S. Segundo, S. Inogés, Á. Santos-Briz, J. García-Briñón, et al. 2016. Targeting of PI3K/AKT/mTOR pathway to inhibit T cell activation and prevent graft-versus-host disease development. Journal of Hematology & Oncology 9: 113.54. https://doi.org/10.1186/s13045-016-0343-5.
Iacobas, D., J. Wen, S. Iacobas, N. Schwartz, and C. Putterman. 2021. Remodeling of neurotransmission, chemokine, and PI3K-AKT signaling genomic fabrics in neuropsychiatric systemic lupus erythematosus. Genes 12: 251.7. https://doi.org/10.3390/genes12020251.
Alzahrani, A.S. 2019. PI3K/Akt/mTOR inhibitors in cancer: at the bench and bedside. Seminars in Cancer Biology 59: 125-132.503. https://doi.org/10.1016/j.semcancer.2019.07.009.
Chamcheu, J.C., S. Esnault, V.M. Adhami, A.L. Noll, S. Banang-Mbeumi, T. Roy, S.S. Singh, S. Huang, K.G. Kousoulas, and H. Mukhtar. 2019. Fisetin, a 3,7,3’,4’-tetrahydroxyflavone inhibits the PI3K/Akt/mTOR and MAPK pathways and ameliorates psoriasis pathology in 2D and 3D organotypic human inflammatory skin models. Cells 8: 108949. https://doi.org/10.3390/cells8091089.
Chamcheu, J.C., M.-I. Chaves-Rodriquez, V.M. Adhami, I.A. Siddiqui, G.S. Wood, B. Jack Longley, and H. Mukhtar. 2016. Upregulation of PI3K/AKT/mTOR, FABP5 and PPARβ/δ in human psoriasis and imiquimod-induced murine psoriasiform dermatitis model. Acta Dermato-Venereologica 96: 854-856.45. https://doi.org/10.2340/00015555-2359.
Varshney, P., and N. Saini. 2018. PI3K/AKT/mTOR activation and autophagy inhibition plays a key role in increased cholesterol during IL-17A mediated inflammatory response in psoriasis. Biochimica Et Biophysica Acta. Molecular Basis of Disease 1864: 1795-1803.79. https://doi.org/10.1016/j.bbadis.2018.02.003.
Chen, K., P. Zhu, W. Chen, K. Luo, X.-J. Shi, and W. Zhai. 2021. Melatonin inhibits proliferation, migration, and invasion by inducing ROS-mediated apoptosis via suppression of the PI3K/Akt/mTOR signaling pathway in gallbladder cancer cells. Aging 13: 22502-22515.15. https://doi.org/10.18632/aging.203561.
Chen, Y.-T., C.-R. Huang, C.-L. Chang, J.Y. Chiang, C.-W. Luo, H.-H. Chen, and H.-K. Yip. 2020. Jagged2 progressively increased expression from stage I to III of bladder cancer and melatonin-mediated downregulation of Notch/Jagged2 suppresses the bladder tumorigenesis via inhibiting PI3K/AKT/mTOR/MMPs signaling. International Journal of Biological Sciences 16: 2648-2662.14. https://doi.org/10.7150/ijbs.48358.
Reitamo, S., P. Spuls, B. Sassolas, M. Lahfa, A. Claudy, and C. Griffiths. 2001. Efficacy of sirolimus (rapamycin) administered concomitantly with a subtherapeutic dose of cyclosporin in the treatment of severe psoriasis: a randomized controlled trial. The British Journal of Dermatology 145: 138. https://doi.org/10.1046/j.1365-2133.2001.04376.x.
Funding
This study was supported by the Natural Science Foundation of Chongqing Municipality (no. CSTB2023NSCQ-MSX0168 to HY), the joint project of Chongqing Municipal Health Commission and Chongqing Municipal Science and Technology Bureau (No. 2020MSXM070 to HY), the second batch of Class A reserve talents of the Children’s Hospital Affiliated to Chongqing Medical University (No. RC05036 to HY), and the program for Youth Innovation in Future Medicine, Chongqing Medical University (W0177 to XL).
Author information
Authors and Affiliations
Contributions
Zhanting Shen: formal analysis, methodology, validation, visualization, and writing—original draft. **qiu Jiang: methodology. **aoying Zhou: methodology. Qingqing Tan: methodology. Shi Yan: methodology. Xuege Wu: methodology. Jiangshan Pi: methodology. Hua Wang: conceptualization, supervision, and writing—review and editing. Huan Yang: conceptualization, formal analysis, funding acquisition, investigation, project administration, supervision, visualization, writing—original draft, and writing—review and editing. **aoyan Luo: conceptualization, funding acquisition, investigation, supervision, and writing—review and editing.
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
Study procedures were performed in accordance with the Declaration of Helsinki ethical principles for medical research involving human subjects. This study was approved by the Institutional Ethics Committee of Children’s Hospital of Chongqing Medical University (No. 2023388). Informed consent was obtained from all participants before study inclusion.
Consent for Publication
The consent of all coauthors was collected before submission.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shen, Z., Jiang, J., Zhou, X. et al. Melatonin Attenuates Imiquimod-Induced Psoriasis-Like Inflammation and Restores the Th17/Treg Immune Balance. Inflammation (2024). https://doi.org/10.1007/s10753-024-02023-4
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10753-024-02023-4