Abstract
Background
Ulcerative proctitis (UP), though associated with high symptom burden and poor quality of life, is excluded from most of the randomized controlled trials in UC, including the OCTAVE trials. We aimed to analyse the effectiveness of tofacitinib in UP, and compare it to that in left sided colitis (LSC) and pancolitis (PC).
Methods
This was a prospective cohort study. Patients with either steroid-dependent or refractory ulcerative colitis, who received tofacitinib, were divided into three groups based on the disease extent [UP, LSC and PC]. The primary outcome was comparison of proportion of patients in clinical remission in the three groups, at weeks 8, 16 and 48. Safety outcomes were reported using incidence rate per patient year of exposure.
Results
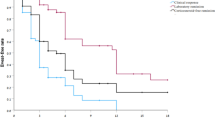
Clinical remission was achieved in 47%(15/32), 24%(23/94), and 43%(23/54) of patients at week 8, 56%(18/32), 37%(35/94), and 56%(30/54) of patients at week 16, and 59%(19/32), 38%(36/94), and 24%(13/54) of patients at week 48 in groups UP, LSC and PC, respectively. Corticosteroid-free clinical remission rates were significantly higher in patients in groups UP at week 48. Five (15%) patients with UP were primary non-responders to tofacitinib at week 16, while three (9%) patients had secondary loss of response at week 48. The probability of sustained clinical response was highest in patients with UP. Patients with UP had the lowest incidence of adverse effects.
Conclusion
The effectiveness of tofacitinib in inducing and maintaining clinical remission is greater in patients with UP compared to LSC and PC.
Graphical Abstract





Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author, [AS], upon reasonable request.
References
Silverberg MS, Satsangi J, Ahmad T et al. Toward an integrated clinical, molecular and serological classification of inflammatory bowel disease: report of a Working Party of the 2005 Montreal World Congress of Gastroenterology. Can J Gastroenterol,. 2005;19:5 Suppl A-36A. https://doi.org/10.1155/2005/269076.
Satsangi J, Silverberg MS, Vermeire S, Colombel J. The Montreal classification of inflammatory bowel disease: controversies, consensus, and implications. Gut. 2006;55:749–753. https://doi.org/10.1136/gut.2005.082909.
Dubois E, Moens A, Geelen R, Sabino J, Ferrante M, Vermeire S. Long-term outcomes of patients with ulcerative proctitis: analysis from a large referral centre cohort. United Eur Gastroenterol J. 2020;8:933–941. https://doi.org/10.1177/2050640620941345.
Meucci G, Vecchi M, Astegiano M et al. The natural history of ulcerative proctitis: a multicenter, retrospective study. Gruppo di Studio per le Malattie Infiammatorie Intestinali (GSMII). Am J Gastroenterol. 2000;95:469–473. https://doi.org/10.1111/j.1572-0241.2000.t01-1-01770.x.
Rutgeerts P, Sandborn WJ, Feagan BG et al. Infliximab for induction and maintenance therapy for ulcerative colitis. N Engl J Med. 2005;353:2462–2476. https://doi.org/10.1056/NEJMoa050516.
Feagan BG, Rutgeerts P, Sands BE et al. Vedolizumab as induction and maintenance therapy for ulcerative colitis. N Engl J Med. 2013;369:699–710. https://doi.org/10.1056/NEJMoa1215734.
Sands BE, Sandborn WJ, Panaccione R et al. Ustekinumab as induction and maintenance therapy for ulcerative colitis. N Engl J Med. 2019;381:1201–1214. https://doi.org/10.1056/NEJMoa1900750.
Reinisch W, Sandborn WJ, Hommes DW et al. Adalimumab for induction of clinical remission in moderately to severely active ulcerative colitis: results of a randomised controlled trial. Gut. 2011;60:780–787. https://doi.org/10.1136/gut.2010.221127.
Sandborn WJ, van Assche G, Reinisch W et al. Adalimumab induces and maintains clinical remission in patients with moderate-to-severe ulcerative colitis. Gastroenterology. 2012;142:257–265. https://doi.org/10.1053/j.gastro.2011.10.032.
Sandborn WJ, Su C, Sands BE et al. Tofacitinib as induction and maintenance therapy for ulcerative colitis. N Engl J Med. 2017;376:1723–1736. https://doi.org/10.1056/NEJMoa1606910.
Lucaciu LA, Constantine-Cooke N, Plevris N et al. Real-world experience with tofacitinib in ulcerative colitis: a systematic review and meta-analysis. Therap Adv Gastroenterol. 2021;14:17562848211064004. https://doi.org/10.1177/17562848211064004.
Ma C, Panaccione R, **ao Y et al. REMIT-UC: real world effectiveness and safety of tofacitinib for moderate-to-severely active ulcerative colitis. Am J Gastroenterol. 2022. https://doi.org/10.14309/ajg.0000000000002129.
Chaparro M, Garre A, Mesonero F et al. Tofacitinib in ulcerative colitis: real-world evidence from the ENEIDA Registry. J Crohns Colitis. 2021;15:35–42. https://doi.org/10.1093/ecco-jcc/jjaa145.
Honap S, Chee D, Chapman TP et al. Real-world effectiveness of tofacitinib for moderate to severe ulcerative colitis: a multicentre UK experience. J Crohns Colitis. 2020;14:1385–1393. https://doi.org/10.1093/ecco-jcc/jjaa075.
Lair-Mehiri L, Stefanescu C, Vaysse T et al. Real-world evidence of tofacitinib effectiveness and safety in patients with refractory ulcerative colitis. Dig Liver Dis. 2020;52:268–273. https://doi.org/10.1016/j.dld.2019.10.003.
Raine T, Bonovas S, Burisch J et al. ECCO guidelines on therapeutics in ulcerative colitis: medical treatment. J Crohns Colitis. 2022;16:2–17. https://doi.org/10.1093/ecco-jcc/jjab178.
Sahami S, Wildenberg ME, Koens L et al. Appendectomy for Therapy-Refractory Ulcerative Colitis Results in Pathological Improvement of Colonic Inflammation: Short-Term Results of the PASSION Study. J Crohns Colitis. 2019;13:165–171. https://doi.org/10.1093/ecco-jcc/jjy127.
Amiot A, Bouguen G, Bonnaud G et al. Clinical guidelines for the management of inflammatory bowel disease: Update of a French national consensus. Dig Liver Dis. 2021;53:35–43. https://doi.org/10.1016/j.dld.2020.10.018.
Sood A, Ahuja V, Midha V et al. Colitis and Crohn’s Foundation (India) consensus statements on use of 5-aminosalicylic acid in inflammatory bowel disease. Intest Res. 2020;18:355–378. https://doi.org/10.5217/ir.2019.09176.
Singh A, Mahajan R, Kedia S et al. Use of thiopurines in inflammatory bowel disease: an update. Intest Res. 2022;20:11–30. https://doi.org/10.5217/ir.2020.00155.
Lewis JD, Chuai S, Nessel L, Lichtenstein GR, Aberra FN, Ellenberg JH. Use of the noninvasive components of the Mayo score to assess clinical response in ulcerative colitis. Inflamm Bowel Dis. 2008;14:1660–1666. https://doi.org/10.1002/ibd.20520.
Schroeder KW, Tremaine WJ, Ilstrup DM. Coated oral 5-aminosalicylic acid therapy for mildly to moderately active ulcerative colitis. A randomized study. N Engl J Med 1987;317:1625–1629. https://doi.org/10.1056/NEJM198712243172603.
Deepak P, Alayo QA, Khatiwada A et al. Safety of tofacitinib in a real-world cohort of patients with ulcerative colitis. Clin Gastroenterol Hepatol. 2021;19:1592-1601.e3. https://doi.org/10.1016/j.cgh.2020.06.050.
Viscido A, Valvano M, Stefanelli G et al. Systematic review and meta-analysis: the advantage of endoscopic Mayo score 0 over 1 in patients with ulcerative colitis. BMC Gastroenterol. 2022;22:92. https://doi.org/10.1186/s12876-022-02157-5.
Ayres RC, Gillen CD, Walmsley RS, Allan RN. Progression of ulcerative proctosigmoiditis: incidence and factors influencing progression. Eur J Gastroenterol Hepatol. 1996;8:555–558. https://doi.org/10.1097/00042737-199606000-00011.
Chaparro M, Acosta D, Rodríguez C et al. Real-world evidence of tofacinitib in ulcerative colitis: short-term and long-term effectiveness and safety. Am J Gastroenterol. 2023. https://doi.org/10.14309/ajg.0000000000002145.
Long MD, Afzali A, Fischer M et al. Tofacitinib response in ulcerative colitis (TOUR): early response after initiation of tofacitinib therapy in a real-world setting. Inflamm Bowel Dis. 2022. https://doi.org/10.1093/ibd/izac121.
Pineton de Chambrun G, Amiot A, Bouguen G et al. Efficacy of tumor necrosis factor antagonist treatment in patients with refractory ulcerative proctitis. Clin Gastroenterol Hepatol. 2020;18:620-627.e1. https://doi.org/10.1016/j.cgh.2019.05.060.
Bouguen G, Roblin X, Bourreille A et al. Infliximab for refractory ulcerative proctitis. Aliment Pharmacol Ther 2010;31:1178–1185. https://doi.org/10.1111/j.1365-2036.2010.04293.x.
Cooney RM, Warren BF, Altman DG, Abreu MT, Travis SPL. Outcome measurement in clinical trials for Ulcerative Colitis: towards standardisation. Trials. 2007;8:17. https://doi.org/10.1186/1745-6215-8-17.
Funding
Nil.
Author information
Authors and Affiliations
Contributions
Guarantor of article: AS. Specific author contributions—ArS: Conception and design of the study, acquisition of data, interpretation of data, drafting the article, revising it critically for important intellectual content, final approval of the version to be submitted. VM: Conceptualization, Supervision, Project administration, Drafting the article, revising it critically for important intellectual content, final approval of the version to be submitted. KK: Project administration, supervision, Revising the article critically for important intellectual content, final approval of the version to be submitted. RM: Revising the article critically for important intellectual content, final approval of the version to be submitted. DS: Acquisition of data, final approval of the version to be submitted. RK: Acquisition of data, final approval of the version to be submitted. SG: Revising the article critically for important intellectual content, final approval of the version to be submitted. KA: Revising the article critically for important intellectual content, final approval of the version to be submitted. NB: Interpretation of data, final approval of the version to be submitted. AS: Conception and design of the study, acquisition of data, interpretation of data, drafting the article, revising it critically for important intellectual content, final approval of the version to be submitted.
Corresponding author
Ethics declarations
Conflict of interest
Ajit Sood is on the advisory board of Janssen Pharmaceuticals (Asia–Pacific) and received honorarium for speaker events from Pfizer India and Takeda India. The remaining authors disclose no conflicts.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Singh, A., Mahajan, R., Midha, V. et al. Effectiveness of Tofacitinib in Ulcerative Proctitis Compared to Left Sided Colitis and Pancolitis. Dig Dis Sci 69, 1389–1402 (2024). https://doi.org/10.1007/s10620-024-08276-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-024-08276-1