Abstract
Purpose
Lung cancer incidences tend to be higher among males than females in both China and the United States, yet secular incidence patterns are different due to distinct population and environmental exposures. We examined long-term and future trends of lung cancer incidence, as well as the associations of age, period, and cohort effects with gender disparities.
Methods
Using data from the Cancer Incidence in Five Continents from 1978 to 2012, we calculated age-standardized, age-specific incidence, and male-to-female incidence rate ratios (IRR), and conducted an age-period-cohort analysis. The average annual percentage change (AAPC) of the trends was obtained by Joinpoint Regression. Bayesian age-period-cohort analysis was also conducted to project incidences to 2032.
Results
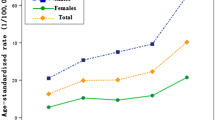
In China, age-standardized incidence revealed a decreasing trend among males, but showed increasing trends among the younger age groups (30–54 years) in females. Age-standardized incidence rates of males decreased but remained stable among females from 1972 to 2012 in the United States. Male-to-female incidence rate ratios narrowed in both countries and reversed among younger birth cohorts in the United States. Gender disparities are expected to continue to diminish in both countries, and incidence among females appears to exceed that of males in the United States by around 2023–2027.
Conclusion
Gender disparities in lung cancer incidence persist and will continue into the future in both countries, but our findings suggested that smoking may play different roles in gender disparities in lung cancer incidence between the two countries. Further population-based epidemiological studies among females in China are imperative.






Similar content being viewed by others
Data availability
The data underlying this article will be shared on reasonable request to the corresponding author.
References
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 71(3):209–249. https://doi.org/10.3322/caac.21660
Lewis DR, Check DP, Caporaso NE, Travis WD, Devesa SS (2014) US lung cancer trends by histologic type. Cancer 120(18):2883–2892. https://doi.org/10.1002/cncr.28749
Jemal A, Miller KD, Ma J, Siegel RL, Fedewa SA, Islami F, Devesa SS, Thun MJ (2018) higher lung cancer incidence in young women than young men in the United States. N Engl J Med 378(21):1999–2009. https://doi.org/10.1056/NEJMoa1715907
Chen WQ, Zheng RS, Zeng HM (2011) Bayesian age-period-cohort prediction of lung cancer incidence in China. Thoracic Cancer 2(4):149–155. https://doi.org/10.1111/j.1759-7714.2011.00062.x
Chen W, Zhang S, Zou X (2010) Evaluation on the incidence, mortality and tendency of lung cancer in China. Thorac Cancer 1(1):35–40. https://doi.org/10.1111/j.1759-7714.2010.00011.x
Siemiatycki J, Karp I, Sylvestre MP, Pintos J (2014) Estimating the proportion of cases of lung cancer legally attributable to smoking: a novel approach for class actions against the tobacco industry. Am J Public Health 104(8):e60–e66. https://doi.org/10.2105/AJPH.2014.302040
de Groot P, Munde RF (2012) Lung cancer epidemiology, risk factors, and prevention. Radiol Clin North Am 50(5):863–876. https://doi.org/10.1016/j.rcl.2012.06.006
Muir C S, Waterhouse J, Mack T, Powell J, Whelan S L (1987) Cancer incidence in five continents, Vol. V. IARC Scientific Publications, No. 88. IARC, Lyon
Parkin D M, Muir C S, Whelan S L, Gao Y-T, Ferlay J, Powell J (1992) Cancer incidence in five continents, Vol. VI. IARC Scientific Publications, No. 120. IARC, Lyon
Parkin D M, Whelan S L, Ferlay J, Raymond L, Young J (1997) Cancer incidence in five continents, Vol. VII. IARC Scientific Publications, No. 143, IARC, Lyon
Parkin D M, Whelan S L, Ferlay J, Teppo L T, homas D B (2002) Cancer incidence in five continents, Vol. VIII. IARC Scientific Publications, No. 155. IARC, Lyon
Curado M P, Edwards B, Shin H R, Storm H, Ferlay J, Heanue M, Boyle P (2007) Cancer incidence in five continents, Vol. IX. IARC Scientific Publications, No. 160. IARC, Lyon
Forman D, Bray F, Brewster D H, Gombe Mbalawa C, Kohler B, Piñeros M, Steliarova-Foucher E, Swaminathan R, Ferlay J (2014) Cancer incidence in five continents, Vol. X. IARC Scientific Publication No. 164. International Agency for Research on Cancer, Lyon
Bray F, Colombet M, Mery L, Piñeros M, Znaor A, Zanetti R, Ferlay J (2017) Cancer incidence in five continents, Vol.XI (electronic version). International Agency for Research on Cancer, Lyon https://ci5.iarc.fr. Accessed 8 Sept 2021
United Nations, Department of Economic and Social Affairs, Population Division (2019) World population prospects 2019, Online Edition. https://population.un.org/wpp/. Accessed 8 Sept 2021
Segi M (1960) Cancer mortality for selected sites in 24 countries (1950–57). Department of Public Health, Tohoku University of Medicine, Sendai
Kim HJ, Fay MP, Feuer EJ, Midthune DN (2000) Permutation tests for joinpoint regression with applications to cancer rates. Stat Med 19(3):335–351. https://doi.org/10.1002/(SICI)1097-0258(20000215)19:3%3c335::AID-SIM336%3e3.0.CO;2-Z
Robertson C, Boyle P (1998) Age-period-cohort analysis of chronic disease rates. I: Modelling approach. Stat Med 17(12):1305–1323. https://doi.org/10.1002/(sici)1097-0258(19980630)17:12%3c1305::aid-sim853%3e3.0.co;2-w
Alder SC (2005) Monitoring the health of populations: statistical principles and methods for public health surveillance. Am J Epidemiol 161(2):205–205. https://doi.org/10.1093/aje/kwi024
Riebler A, Held L (2017) Projecting the future burden of cancer: Bayesian age-period-cohort analysis with integrated nested laplace approximations. Biom J 59(3):531–549. https://doi.org/10.1002/bimj.201500263
Rue H, Martino S, Chopin N (2009) Approximate Bayesian inference for latent gaussian models by using integrated nested laplace approximations. J Royal Stat Soc Series B (Statistical Methodology) 71(2):319–392. https://doi.org/10.1111/j.1467-9868.2008.00700.x
Huang J, Deng Y, Tin MS, Lok V, Ngai CH, Zhang L, Lucero-Prisno DE 3rd, Xu W, Zheng ZJ, Elcarte E, Withers M, Wong MCS (2022) Distribution, risk factors, and temporal trends for lung cancer incidence and mortality: a global analysis. Chest 161(4):1101–1111. https://doi.org/10.1016/j.chest.2021.12.655
Zhang Y, Luo G, Etxeberria J, Hao Y (2021) Global patterns and trends in lung cancer incidence: a population-based study. J Thorac Oncol 16(6):933–944. https://doi.org/10.1016/j.jtho.2021.01.1626
Zheng R, Zhang S, Zeng H, Wang S, Sun K, Chen R, Li L, Wei W, He J (2022) Cancer incidence and mortality in China, 2016. J Natl Cancer Center. https://doi.org/10.1016/j.jncc.2022.02.002
Ferlay J, Ervik M, Lam F, Colombet M, Mery L, Piñeros M, Znaor A, Soerjomataram I, Bray F (2020) Global cancer observatory: Cancer Today. International Agency for Research on Cancer, Lyon https://gco.iarc.fr/today. Accessed 3 Sept 2021
Jeon J, Holford TR, Levy DT, Feuer EJ, Cao P, Tam J, Clarke L, Clarke J, Kong CY, Meza R (2018) Smoking and lung cancer mortality in the United States From 2015 to 2065: a comparative modeling approach. Ann Intern Med 169(10):684–693. https://doi.org/10.7326/M18-1250
Harris JE (1983) Cigarette smoking among successive birth cohorts of men and women in the United States during 1900–80. J Natl Cancer Inst 71(3):473–479
Wynder EL, Muscat JE (1995) The changing epidemiology of smoking and lung cancer histology. Environ Health Perspect 103(Suppl 8):143–148. https://doi.org/10.1289/ehp.95103s8143
Burns D, Lee L, Zhen L A (1997) Cigarette smoking behavior in the United States. Changes in cigarette-related disease risks and their implication for prevention and control; Monograph 8
Lung cancer: what are the risk factors? Centers for Disease Control and Prevention. Centers for Disease Control and Prevention. https://www.cdc.gov/cancer/lung/basic_info/risk_factors.htm. Accessed 3 Sept 2021
Jemal A, Ward E, Thun MJ (2005) Contemporary lung cancer trends among US women. Cancer Epidemiol Biomark Prev 14(3):582–585. https://doi.org/10.1158/1055-9965.EPI-04-0554
Pierce JP, Lee L, Gilpin EA (1994) Smoking initiation by adolescent girls, 1944 through 1988. An association with targeted advertising. JAMA 271(8):608–611
Jemal A, Thun MJ, Ries LA, Howe HL, Weir HK, Center MM, Ward E, Wu XC, Eheman C, Anderson R et al (2008) Annual report to the nation on the status of cancer, 1975–2005, featuring trends in lung cancer, tobacco use, and tobacco control. J Natl Cancer Inst 100(23):1672–1694. https://doi.org/10.1093/jnci/djn389
Khuder SA, Mutgi AB (2001) Effect of smoking cessation on major histologic types of lung cancer. Chest 120(5):1577–1583. https://doi.org/10.1378/chest.120.5.1577
Li S, Meng L, Chiolero A, Ma C, ** B (2016) Trends in smoking prevalence and attributable mortality in China, 1991–2011. Prev Med 93:82–87. https://doi.org/10.1016/j.ypmed.2016.09.027
Yu SZ, Zhao N (1996) Combined analysis of case-control studies of smoking and lung cancer in China. Lung Cancer 14(Suppl 1):S161–S170. https://doi.org/10.1016/s0169-5002(96)90221-4
Zhang M, Wang LM, Li YC, Li XY, Jiang Y, Hu N, **ao L, Li Q, Yang Y, Yang GH (2012) Cross-sectional survey on smoking and smoking cessation behaviors among Chinese adults in 2010. Zhonghua Yu Fang Yi Xue Za Zhi 46(5):404–408
Fidler-Benaoudia MM, Torre LA, Bray F, Ferlay J, Jemal A (2020) Lung cancer incidence in young women vs. young men: a systematic analysis in 40 countries. Int J Cancer 147(3):811–819. https://doi.org/10.1002/ijc.32809
Du Y, Cui X, Sidorenkov G, Groen HJM, Vliegenthart R, Heuvelmans MA, Liu S, Oudkerk M, de Bock GH (2020) Lung cancer occurrence attributable to passive smoking among never smokers in China: a systematic review and meta-analysis. Transl Lung Cancer Res 9(2):204–217. https://doi.org/10.21037/tlcr.2020.02.11
Current cigarette smoking among adults in the United States. Centers for Disease Control and Prevention. Centers for Disease Control and Prevention. https://www.cdc.gov/tobacco/data_statistics/fact_sheets/adult_data/cig_smoking/. Accessed 3 Sept 2021
Centers for Disease Control and Prevention (2008) Disparities in secondhand smoke exposure-United States, 1988-1994 and 1999-2004. JAMA 300(9):1019–1020. https://doi.org/10.1001/jama.300.9.1019
Schauer C, Niessner R, Poschl U (2003) Polycyclic aromatic hydrocarbons in urban air particulate matter: decadal and seasonal trends, chemical degradation, and sampling artifacts. Environ Sci Technol 37(13):2861–2868. https://doi.org/10.1021/es034059s
Deng Y, Peng L, Li N, Zhai Z, **ang D, Ye X, Hu J, Zheng Y, Yao J, Wang S et al (2021) Tracheal, bronchus, and lung cancer burden and related risk factors in the United States and China. Am J Transl Res 13(4):1928–1951
Guo Y, Zeng H, Zheng R, Li S, Barnett AG, Zhang S, Zou X, Huxley R, Chen W, Williams G (2016) The association between lung cancer incidence and ambient air pollution in China: a spatiotemporal analysis. Environ Res 144(Pt A):60–65. https://doi.org/10.1016/j.envres.2015.11.004
Lissowska J, Bardin-Mikolajczak A, Fletcher T, Zaridze D, Szeszenia-Dabrowska N, Rudnai P, Fabianova E, Cassidy A, Mates D, Holcatova I et al (2005) Lung cancer and indoor pollution from heating and cooking with solid fuels: the IARC international multicentre case-control study in Eastern/Central Europe and the United Kingdom. Am J Epidemiol 162(4):326–333. https://doi.org/10.1093/aje/kwi204
Hosgood HD 3rd, Boffetta P, Greenland S, Lee YC, McLaughlin J, Seow A, Duell EJ, Andrew AS, Zaridze D, Szeszenia-Dabrowska N et al (2010) In-home coal and wood use and lung cancer risk: a pooled analysis of the international lung cancer consortium. Environ Health Perspect 118(12):1743–1747. https://doi.org/10.1289/ehp.1002217
Yin P, Brauer M, Cohen AJ, Wang H, Li J, Burnett RT, Stanaway JD, Causey K, Larson S, Godwin W et al (2020) The effect of air pollution on deaths, disease burden, and life expectancy across China and its provinces, 1990–2017: an analysis for the Global Burden of Disease Study 2017. Lancet Planet Health 4(9):e386–e398. https://doi.org/10.1016/S2542-5196(20)30161-3
Wang M, Qin S, Zhang T, Song X, Zhang S (2015) The effect of fruit and vegetable intake on the development of lung cancer: a meta-analysis of 32 publications and 20,414 cases. Eur J Clin Nutr 69(11):1184–1192. https://doi.org/10.1038/ejcn.2015.64
Vieira AR, Abar L, Vingeliene S, Chan DS, Aune D, Navarro-Rosenblatt D, Stevens C, Greenwood D, Norat T (2016) Fruits, vegetables and lung cancer risk: a systematic review and meta-analysis. Ann Oncol 27(1):81–96. https://doi.org/10.1093/annonc/mdv381
Lam WK (2005) Lung cancer in Asian women-the environment and genes. Respirology 10(4):408–417. https://doi.org/10.1111/j.1440-1843.2005.00723.x
Ragavan M, Patel MI (2022) The evolving landscape of sex-based differences in lung cancer: a distinct disease in women. Eur Respir Rev. https://doi.org/10.1183/16000617.0100-2021
Cote ML, Liu M, Bonassi S, Neri M, Schwartz AG, Christiani DC, Spitz MR, Muscat JE, Rennert G, Aben KK et al (2012) Increased risk of lung cancer in individuals with a family history of the disease: a pooled analysis from the international lung cancer consortium. Eur J Cancer 48(13):1957–1968. https://doi.org/10.1016/j.ejca.2012.01.038
Yin X, Chan CPY, Seow A, Yau WP, Seow WJ (2021) Association between family history and lung cancer risk among Chinese women in Singapore. Sci Rep 11(1):21862. https://doi.org/10.1038/s41598-021-00929-9
Weiss JM, Lacey Jr JV, Shu XO, Ji BT, Hou L, Yang G, Li H, Rothman N, Blair A, Gao YT, Chow WH, Zheng W (2008) Menstrual and reproductive factors in association with lung cancer in female lifetime nonsmokers. Am J Epidemiol 168(11):1319–1325. https://doi.org/10.1093/aje/kwn257
Rodriguez-Lara V, Avila-Costa MR (2021) An overview of lung cancer in women and the impact of estrogen in lung carcinogenesis and lung cancer treatment. Front Med (Lausanne) 8:600121. https://doi.org/10.3389/fmed.2021.600121
Chen WQ, Zheng RS, Zeng HM (2011) Bayesian age-period-cohort prediction of lung cancer incidence in China. Thorac Cancer 2(4):149–155. https://doi.org/10.1111/j.1759-7714.2011.00062.x
**e L, Qian Y, Liu Y, Li Y, Jia S, Yu H, Wang C, Qian B, Bao P (2020) Distinctive lung cancer incidence trends among men and women attributable to the period effect in Shanghai: an analysis spanning 42 years. Cancer Med 9(8):2930–2939. https://doi.org/10.1002/cam4.2917
Xu X, Zhang X, Hu TW, Miller LS, Xu M (2019) Effects of global and domestic tobacco control policies on cigarette consumption per capita: an evaluation using monthly data in China. BMJ Open 9(6):e025092. https://doi.org/10.1136/bmjopen-2018-025092
The 1964 report on smoking and health: documents. The reports of the surgeon general. NIH. https://profiles.nlm.nih.gov/ps/retrieve/Narrative/NN/p-nid/60/p-docs/true. Accessed 2 Sept 2021
Levy DT, Meza R, Zhang Y, Holford TR (2016) Gauging the effect of U.S. tobacco control policies from, 1965 through 2014 using simsmoke. Am J Prev Med 50(4):535–542. https://doi.org/10.1016/j.amepre.2015.10.001
Travis WD, Brambilla E, Riely GJ (2013) New pathologic classification of lung cancer: relevance for clinical practice and clinical trials. J Clin Oncol 31(8):992–1001. https://doi.org/10.1200/JCO.2012.46.9270
Bishop JA, Teruya-Feldstein J, Westra WH, Pelosi G, Travis WD, Rekhtman N (2012) p40 (DeltaNp63) is superior to p63 for the diagnosis of pulmonary squamous cell carcinoma. Mod Pathol 25(3):405–415. https://doi.org/10.1038/modpathol.2011.173
Funding
This study was supported by funding from the National Key R&D Program of China (Grant No. 2016YFC1302505-2).
Author information
Authors and Affiliations
Contributions
CZ, MJ, and MX: study conceptualization and design. MX, ML, and LJ: literature search. MX, ML, JP, and LJ: acquisition and preparation of data. MX, ML, and JP: statistical analysis and interpretation of study findings. MX and CW: manuscript preparation. CW and CZ: language polishing. CZ and MJ: supervision. CZ and MJ: funding acquisition. All authors: final approval of the paper.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All data used in the present study have been retrieved from publicly accessible sources and this study does not require ethics approval.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Xu, M., Li, M., Pei, J. et al. Gender disparities in incidence and projections of lung cancer in China and the United States from 1978 to 2032: an age-period-cohort analysis. Cancer Causes Control 33, 1247–1259 (2022). https://doi.org/10.1007/s10552-022-01597-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-022-01597-4