Abstract
Purpose
HER2-low triple-negative breast cancer (TNBC) accounted for up to 34%–39% of primary TNBC and 22.2%–32% of metastatic TNBC. Our study aims to explore the relationship between HER2 expression and clinicopathological characteristics, analyze the impact of HER2 expression on the pathological complete response (pCR) to neoadjuvant chemotherapy (NAC) in TNBC.
Methods
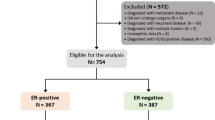
This study involved 191 patients with TNBC who underwent operation after NAC from October 2021 to August 2022. Clinicopathological characteristics and the frequency of pCR were compared between HER2-low and HER2-0 TNBC.
Results
42.2% (81/191) patients in our cohort were HER2-low. They exhibited differences in menopausal status, body mass index (BMI), androgen receptor (AR) expression, and histological grade (P < 0.05). Particularly, in HER2-low TNBC, AR was associated with tumor size, lymph node metastase, histological grade, and the incidence of multifocal disease (P < 0.05). The total pCR rate of entire cohor was 39.8%. Tumor size (P = 0.025), AR status (P = 0.033) and histological grade (P = 0.007) were significantly associated with the pCR rate of them, while the HER2 status did not exert a similar association. The multivariate analysis revealed that BMI (P = 0.004) and histological grade (P < 0.001) were associated with pCR of HER2-low TNBC, while tumor size (P = 0.034) and AR (P = 0.034) were associated with pCR of HER2-0 TNBC, respectively.
Conclusions
In our cohort, HER2-low TNBC patients exhibits specific clinical characteristics and response features to NAC.
Similar content being viewed by others
Data availability
Enquiries about data availability should be directed to the authors.
References
Bianchini G, De Angelis C, Licata L, Gianni L (2022) Treatment landscape of triple-negative breast cancer—expanded options, evolving needs. Nat Rev Clin Oncol 19:91–113. https://doi.org/10.1038/s41571-021-00565-2
Corti C, Giugliano F, Nicolò E, Tarantino P, Criscitiello C, Curigliano G (2023) HER2-low breast cancer: a new subtype? Curr Treat Options Oncol 24:468–478. https://doi.org/10.1007/s11864-023-01068-1
Wolff AC, Hammond MEH, Allison KH, Harvey BE, Mangu PB, Bartlett JMS et al (2018) Human epidermal growth factor receptor 2 testing in breast cancer: American Society of Clinical Oncology/College of American Pathologists Clinical practice guideline focused update. Arch Pathol Lab Med 142:1364–1382. https://doi.org/10.5858/arpa.2018-0902-SA
Tarantino P, Hamilton E, Tolaney SM, Cortes J, Morganti S, Ferraro E et al (2020) HER2-low breast cancer: pathological and clinical landscape. J Clin Oncol 38:1951–1962. https://doi.org/10.1200/JCO.19.02488
Denkert C, Seither F, Schneeweiss A, Link T, Blohmer JU, Just M et al (2021) Clinical and molecular characteristics of HER2-low-positive breast cancer: pooled analysis of individual patient data from four prospective, neoadjuvant clinical trials. Lancet Oncol 22:1151–1161. https://doi.org/10.1016/S1470-2045(21)00301-6
Gampenrieder SP, Dezentjé V, Lambertini M, De Nonneville A, Marhold M, Le Du F et al (2023) Influence of HER2 expression on prognosis in metastatic triple-negative breast cancer—results from an international, multicenter analysis coordinated by the AGMT Study Group. ESMO Open 8:100747. https://doi.org/10.1016/j.esmoop.2022.100747
Fehrenbacher L, Cecchini RS, Geyer CE, Rastogi P, Costantino JP, Atkins JN et al (2020) NSABP B-47/NRG oncology phase III randomized trial comparing adjuvant chemotherapy with or without trastuzumab in high-risk invasive breast cancer negative for HER2 by FISH and With IHC 1+ or 2+. J Clin Oncol 38:444–453. https://doi.org/10.1200/JCO.19.01455
Modi S, Jacot W, Yamashita T, Sohn J, Vidal M, Tokunaga E et al (2022) Trastuzumab deruxtecan in previously treated HER2-low advanced breast cancer. N Engl J Med 387:9–20. https://doi.org/10.1056/NEJMoa2203690
Chick RC, Clifton GT, Hale DF, Vreeland TJ, Hickerson AT, Kemp Bohan PM et al (2021) Subgroup analysis of nelipepimut-S plus GM-CSF combined with trastuzumab versus trastuzumab alone to prevent recurrences in patients with high-risk, HER2 low-expressing breast cancer. Clin Immunol 225:108679. https://doi.org/10.1016/j.clim.2021.108679
Venema CM, Bense RD, Steenbruggen TG, Nienhuis HH, Qiu SQ, Van Kruchten M et al (2019) Consideration of breast cancer subtype in targeting the androgen receptor. Pharmacol Ther 200:135–147. https://doi.org/10.1016/j.pharmthera.2019.05.005
Cortazar P, Zhang L, Untch M, Mehta K, Costantino JP, Wolmark N et al (2014) Pathological complete response and long-term clinical benefit in breast cancer: the CTNeoBC pooled analysis. Lancet 384:164–172. https://doi.org/10.1016/S0140-6736(13)62422-8
Hu XE, Yang P, Chen S, Wei G, Yuan L, Yang Z et al (2023) Clinical and biological heterogeneities in triple-negative breast cancer reveals a non-negligible role of HER2-low. Breast Cancer Res 25:34. https://doi.org/10.1186/s13058-023-01639-y
Ma Y, Jiao D, Zhang J, Lv M, Chen X, Liu Z (2023) HER2-low status was associated with better breast cancer-specific survival in early-stage triple-negative breast cancer. Oncologist. https://doi.org/10.1093/oncolo/oyad275
Leon-Ferre RA, Goetz MP (2023) Advances in systemic therapies for triple negative breast cancer. BMJ 381:e071674. https://doi.org/10.1136/bmj-2022-071674
Thomas A, Teicher BA, Hassan R (2016) Antibody–drug conjugates for cancer therapy. Lancet Oncol 17:e254–e262. https://doi.org/10.1016/S1470-2045(16)30030-4
(2022) T-DXd: new standard for HER2-low breast cancer. Cancer Discov 12:1828. https://doi.org/10.1158/2159-8290.Cd-nb2022-0043
Narayan P, Dilawari A, Osgood C, Feng Z, Bloomquist E, Pierce WF et al (2023) US Food and Drug Administration approval summary: fam-trastuzumab deruxtecan-nxki for human epidermal growth factor receptor 2-low unresectable or metastatic breast cancer. J Clin Oncol 41:2108–2116. https://doi.org/10.1200/JCO.22.02447
Schreiber AR, O’bryant CL, Kabos P, Diamond JR (2023) The emergence of targeted therapy for HER2-low triple-negative breast cancer: a review of fam-trastuzumab deruxtecan. Expert Rev Anticancer Ther 23:1061–1069. https://doi.org/10.1080/14737140.2023.2257885
Li Y, Tsang JY, Tam F, Loong T, Tse GM (2023) Comprehensive characterization of HER2-low breast cancers: implications in prognosis and treatment. EBioMedicine 91:104571. https://doi.org/10.1016/j.ebiom.2023.104571
Jacot W, Maran-Gonzalez A, Massol O, Sorbs C, Mollevi C, Guiu S et al (2021) Prognostic value of HER2-low expression in non-metastatic triple-negative breast cancer and correlation with other biomarkers. Cancers 13:6059. https://doi.org/10.3390/cancers13236059
Lehmann BD, Bauer JA, Chen X, Sanders ME, Chakravarthy AB, Shyr Y et al (2011) Identification of human triple-negative breast cancer subtypes and preclinical models for selection of targeted therapies. J Clin Invest 121:2750–2767. https://doi.org/10.1172/JCI45014
Choupani E, Gomari MM, Zanganeh S, Nasseri S, Haji-Allahverdipoor K, Rostami N et al (2023) Newly developed targeted therapies against the androgen receptor in triple-negative breast cancer: a review. Pharmacol Rev 75:309–327. https://doi.org/10.1124/pharmrev.122.000665
Wardley A, Cortes J, Provencher L, Miller K, Chien AJ, Rugo HS et al (2021) The efficacy and safety of enzalutamide with trastuzumab in patients with HER2+ and androgen receptor-positive metastatic or locally advanced breast cancer. Breast Cancer Res Treat 187:155–165. https://doi.org/10.1007/s10549-021-06109-7
De Moura LL, Cesca MG, Tavares MC, Santana DM, Saldanha EF, Guimarães PT et al (2021) HER2-low status and response to neoadjuvant chemotherapy in HER2 negative early breast cancer. Breast Cancer Res Treat 190:155–163. https://doi.org/10.1007/s10549-021-06365-7
Domergue C, Martin E, Lemarié C, Jézéquel P, Frenel JS, Augereau P et al (2022) Impact of HER2 status on pathological response after neoadjuvant chemotherapy in early triple-negative breast cancer. Cancers 14:2509. https://doi.org/10.3390/cancers14102509
Ergun Y, Akagunduz B, Karacin C, Turker S, Ucar G (2023) The effect of HER2-low status on pathological complete response and survival in triple-negative breast cancer: a systemic review and meta-analysis. Clin Breast Cancer 23:567–575. https://doi.org/10.1016/j.clbc.2023.05.015
Masuda N, Lee SJ, Ohtani S, Im YH, Lee ES, Yokota I et al (2017) Adjuvant capecitabine for breast cancer after preoperative chemotherapy. N Engl J Med 376:2147–2159. https://doi.org/10.1056/NEJMoa1612645
Sanomachi T, Okuma HS, Kitadai R, Kawachi A, Yazaki S, Tokura M et al (2023) Low HER2 expression is a predictor of poor prognosis in stage I triple-negative breast cancer. Front Oncol 13:1157789. https://doi.org/10.3389/fonc.2023.1157789
Yi X, Hu S, Ma M, Huang D, Zhang Y (2023) Effect of HER2-low expression on neoadjuvant efficacy in operable breast cancer. Clin Transl Oncol. https://doi.org/10.1007/s12094-023-03318-y
Horisawa N, Adachi Y, Takatsuka D, Nozawa K, Endo Y, Ozaki Y et al (2022) The frequency of low HER2 expression in breast cancer and a comparison of prognosis between patients with HER2-low and HER2-negative breast cancer by HR status. Breast Cancer 29:234–241. https://doi.org/10.1007/s12282-021-01303-3
Wei T, Wang D, Gao S, Wang X, Yue J, Kang Y et al (2023) Clinicopathologic characteristics and prognostic significance of HER2-low expression in patients with early breast cancer: a systematic review and meta-analysis. Front Oncol 13:1100332. https://doi.org/10.3389/fonc.2023.1100332
Funding
This article is funded by Education Department Foundation of Liaoning Province of China, LJKMZ20221227, Youth Science Program of the First Affiliated Hospital of **zhou Medical University, FYQKR-202201.
Author information
Authors and Affiliations
Contributions
Yue Shi contributed to conceptualization, data curation, investigation, project administration, validation, writing-original draft. Heng Lu contributed to formal analysis, investigation, methodology, resources, visualization. Yiqi Zhang contributed to conceptualization, resources, supervision, funding acquisition, writing – review & editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shi, Y., Lu, H. & Zhang, Y. Impact of HER2 status on clinicopathological characteristics and pathological complete response to neoadjuvant chemotherapy in triple-negative breast cancer. Breast Cancer Res Treat 206, 387–395 (2024). https://doi.org/10.1007/s10549-024-07317-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-024-07317-7