Abstract
Urinary tract stones are a common clinical condition that affect millions of individuals worldwide. The management of these stones has evolved significantly over the past 70 years, and ultrasound imaging has emerged as a valuable tool for diagnosis, treatment planning, and follow-up. This review aims to provide an overview of the application of ultrasound imaging in the treatment of urinary tract stones, highlighting its advantages, limitations, and current advancements in the field.


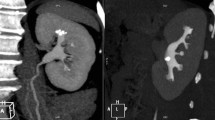
Source: Reproduced from [32]







Source: Reproduced from [84]

Similar content being viewed by others
Data availability
Data sharing is not applicable to this article.
References
Alelign T, Petros B. Kidney stone disease: an update on current concepts. Adv Urol. 2018. https://doi.org/10.1155/2018/3068365.
Sakamoto S, Miyazawa K, Yasui T, et al. Chronological changes in the epidemiological characteristics of upper urinary tract urolithiasis in Japan. Int J Urol. 2018;25:373–8.
Uribarri J, Oh MS, Carroll HJ. The first kidney stone. Ann Intern Med. 1989;111:1006–9.
Kluner C, Hein PA, Gralla O, et al. Does ultra-low-dose CT with a radiation dose equivalent to that of KUB suffice to detect renal and ureteral calculi? J Comput Assist Tomogr. 2006;30:44–50.
Caoili EM, Cohan RH, Korobkin M, et al. Urinary tract abnormalities: initial experience with multi-detector row CT urography. Radiology. 2002;222:353–60.
Van Der Molen AJ, Cowan NC, Mueller-Lisse UG, et al. CT urography: definition, indications and techniques. A guideline for clinical practice. Eur Radiol. 2008;18:4–17.
Niemann T, Kollmann T, Bongartz G. Diagnostic performance of low-dose CT for the detection of urolithiasis: a meta-analysis. AJR Am J Roentgenol. 2008;191:396–401.
Zilberman DE, Tsivian M, Lipkin ME, et al. Low dose computerized tomography for detection of urolithiasis-its effectiveness in the setting of the urology clinic. J Urol. 2011;185:910–4.
Fulgham PF, Assimos DG, Pearle MS, et al. Clinical effectiveness protocols for imaging in the management of ureteral calculous disease: AUA technology assessment. J Urol. 2013;189:1203–13.
Bhanot R, Hameed ZBM, Shah M, et al. ALARA in Urology: Steps to minimise radiation exposure during all parts of the endourological journey. Curr Urol Rep. 2022;23:255–9.
Tasian GE, Copelovitch L, et al. Evaluation and medical management of kidney stones in children. J Urol. 2014;192:1329–36.
Schlegel JU, Diggdon P, Cuellar J. The use of ultrasound for localizing renal calculi. J Urol. 1961;86:367–9.
Cook JH III, Lytton S. Intraoperative localization of renal calculi during nephrolithotomy by ultrasound scanning. J Urol. 1977;117:543–6.
Turk C, Petrik A, Sarica K, et al. EAU guidelines on interventional treatment for urolithiasis. Eur Urol. 2016;69:475–82.
Assimos D, Krambeck A, Miller NL, et al. Surgical management of stones: American urological association/Endourological society guideline. PART I J Urol. 2016;196:1153–60.
Smith A, Averch TD, Shahrour K, et al. A nephrolithometric nomogram to predict treatment success of percutaneous nephrolithotomy. J Urol. 2013;190:149–56.
El-Nahas AR, El-Assmy AM, Mansour O, et al. A prospective multivariate analysis of factors predicting stone disintegration by extracorporeal shock wave lithotripsy: the value of high-resolution noncontrast computed tomography. Eur Urol. 2007;51:1693–4.
Ferrandino MN, Bagrodia A, Pierre SA, et al. Radiation exposure in the acute and short-term management of urolithiasis at 2 academic centers. J Urol. 2009;181:668–73.
Ripolles T, Agramunt M, Errando J, et al. Suspected ureteral colic: plain film and sonography vs unenhanced helical CT. A prospective study in 66 patients. Eur Radiol. 2004;14:129–36.
Smith-Bindman R, Aubin C, Bailitz J, et al. Ultrasonography versus computed tomography for suspected nephrolithiasis. N Engl J Med. 2014;371:1100–10.
Stothers L, Lee LM. Renal colic in pregnancy. J Urol. 1992;148:1383–7.
Patel SJ, Reede DL, Katz DS, et al. Imaging the pregnant patient for nonobstetric conditions: algorithms and radiation dose considerations. Radiographics. 2007;27:1705–22.
Cheung KL, Lafayette RA. Renal physiology of pregnancy. Adv Chronic Kidney Dis. 2013;20:209–14.
King WE 3rd, Kimme-Smith C, Winter J. Renal stone shadowing: an investigation of contributing factors. Radiology. 1985;154:191–6.
Wood BG, Urban MW. Detecting kidney stones using twinkling artifacts: survey of kidney stones with varying composition and size. Ultrasound Med Biol. 2020;46:155–66.
Rahmouni A, Bargoin R, Herment A, et al. Color Doppler twinkling artifact in hyperechoic regions. Radiology. 1996. https://doi.org/10.1148/radiology.199.1.8633158.
Winkel RR, Kalhauge A, Fredfeldt KE. The usefulness of ultrasound color Doppler twinkling artefact for detecting urolithiasis compared with low dose nonenhanced computerized tomography. Ultrasound Med Biol. 2012;38:1180–7.
Abdel-Gawad M, Kadasne RD, Elsobky E, et al. A prospective comparative study of color Doppler ultrasound with twinkling and noncontrast computerized tomography for the evaluation of acute renal colic. J Urol. 2016;196:757–62.
Gliga ML, Chirila CN, Podeanu DM, et al. Twinkle, twinkle little stone: an artifact improves the ultrasound performance! Med Ultrason. 2017;19:272–5.
Masch WR, Cohan RH, Ellis JH, et al. Clinical effectiveness of prospectively reported sonographic twinkling artifact for the diagnosis of renal calculus in patients without known urolithiasis. Am J Roentgenol. 2016. https://doi.org/10.2214/AJR.15.14998.
Sternberg KM, Eisner B, Larson T, et al. Ultrasonography significantly overestimates stone size when compared to; ow-dose, noncontrast computed tomography. Urology. 2016;95:67–71.
Ganesan V, De S, Greene D, et al. Accuracy of ultrasonography for renal stone detection and size determination: is it good enough for management decisions? BJU Int. 2017;119:464–9.
Ray AA, Ghiculete D, Pace KT, et al. Limitations to ultrasound in the detection and measurement of urinary tract calculi. Urology. 2010;76:295–300.
Dunmire B, Lee FC, Hsi RS, et al. Tools to improve the accuracy of kidney stone sizing with ultrasound. J Endourol. 2015;29:147–52.
Dunmire B, Harper JD, Cunitz BW, et al. Use of the acoustic shadow width to determine kidney stone size with ultrasound. J Urol. 2016;195:171–7.
Dai JC, Dunmire B, Sternberg KM, et al. Retrospective comparison of measured stone size and posterior acoustic shadow width in clinical ultrasound images. World J Urol. 2018;36:727–32.
Ellenbogen PH, Scheible FW, Talner LB, et al. Sensitivity of gray scale ultrasound in detecting urinary tract obstruction. AJR Am J Roentgenol. 1978;130:731–3.
Wong C, Teitge B, Ross M, et al. The accuracy and prognostic value of point-of-care ultrasound for nephrolithiasis in the emergency department: a systematic review and meta-analysis. Acad Emerg Med. 2018;25:684–498.
Hamamoto S, Okada S, Inoue T, et al. Prospective evaluation and classification of endoscopic findings for ureteral calculi. Sci Rep. 2020. https://doi.org/10.1038/s41598-020-699158-w.
Degirmenci T, Gunlusoy B, Kozacioglu Zm, et al. Outcomes of ureteroscopy for the management of impacted ureteral calculi with different localizations. Urology. 2012;80:811–5.
Yamashita S, Inoue T, Kohjimoto Y, et al. Comprehensive endoscopic management of impacted ureteral stones: literature review and expert opinions. Int J Urol. 2022;29:799–806.
Legemate JD, Wijnstok NJ, Matsuda T, et al. Characteristics and outcomes of ureteroscopic treatment in 2650 patients with impacted ureteral stones. World J Urol. 2017;35:1497.
Taguchi K, Hamamoto S, Osaga S, et al. Comparison of antegrade and retrograde ureterolithotripsy for proximal ureteral stones: a systematic review and meta-analysis. Trans Adnrol Urol. 2021;10:1179–91.
De Sio M, Autorino R, Quarto G, et al. Modified supine versus prone position in percutaneous nephrolithotomy for renal stones treatable with a single percutaneous access: a prospective randomized trial. Eur Urol. 2008;54:196–203.
Yuan D, Liu Y, Rao H, et al. Supine versus prone position in percutaneous nephrolithotomy for kidney calculi: a meta-analysis. J Endourol. 2016;30:754–63.
Hamamoto S, Okada S, Inoue T, et al. Comparison of the safety and efficacy between the prone split-leg and Galdakao-modified supine Valdivia positions during endoscopic combined intrarenal surgery: a multi-institutional analysis. Int J Urol. 2021;28:1129–35.
Munver R, Delvecchio FC, Newman GE, et al. Critical analysis of supracostal access for percutaneous renal surgery. J Urol. 2001;166:1242–6.
Amaresh M, Hegde P, Chawla A, et al. Safety and efficacy of superior calyceal access versus inferior calyceal access for pelvic and/or lower calyceal renal calculi—a prospective observational comparative study. World J Urol. 2021;39:2155–61.
Pearle MS, Lingeman JE, Leveillee R, et al. Prospective randomized trial comparing shock wave lithotripsy and ureteroscopy for lower pole caliceal calculi 1 cm or less. J Urol. 2005;173:2005–9.
Drake T, Grivas N, Dabestani S, et al. What are the benefits and harms of ureteroscopy compared with shock-wave lithotripsy in the treatment of upper ureteral stones? A systematic review. Eur Urol. 2017;72:772–86.
Sorensen MD, Bailey MR, Shah AR, et al. Quantitative assessment of shockwave lithotripsy accuracy and the effect of respiratory motion. J Endourol. 2012;26:1070–4.
Chen CJ, Hsu HC, Chung WS, Yu HJ. Clinical experience with ultrasound-based real-time tracking lithotripsy in the single renal stone treatment. J Endourol. 2009;23:1811–5.
Isogai M, Hamamoto S, Kawase K, et al. Efficacy of ultrasound monitoring during extracorporeal shock wave lithotripsy: a multi-institutional propensity score-matched study. Int J Urol. 2022;29:1054–60.
Besien JV, Uvin P, Hermie I, et al. Ultrasonography is not inferior to fluoroscopy to guide extracorporeal shock waves during treatment of renal and upper ureteric calculi: a randomized prospective study. Biomed Res Int. 2017;2017:7802672.
Drach GW, Dretler S, Fair W. Report of the United States cooperative study of extracorporeal shock wave lithotripsy. J Urol. 1986;35:1127–33.
Sumino Y, Mimata H, Tasaki Y, et al. Predictors of lower pole renal stone clearance after extracorporeal shock wave lithotripsy. J Urol. 2002;168:1344–7.
Elbahnasy AM, Clayman RV, Shalhav AL, et al. Lower pole calyceal stone clearance after SWL, percutaneous nephrolithotomy, and flexible URS; impact of radiographic spatial anatomy. J Endourol. 1998;12:113–9.
Sampaio FJ, Aragao AH. Inferior pole collecting system anatomy; its probable role in extracorporeal shock wave lithotripsy. J Urol. 1992;147:322–4.
Shah A, Owen N, Lu W, et al. Novel ultrasound method to reposition kidney stones. Urol Res. 2010;38:491–5.
Harper JD, Cunitz BW, Dunmire B, et al. First in human clinical trial of ultrasonic propulsion of kidney stones. J Urol. 2016;195:956–64.
May PC, Bailey MR, Harper JD. Ultrasonic propulsion of kidney stones. Curr Opin Urol. 2016;26:264–70.
Harper JD, Sorensen MD, Cunitz BW, et al. Focused ultrasound to expel calculi from the kidney: safety and efficacy of a clinical prototype device. J Urol. 2013;190:1090–5.
Candau C, Saussine C, Lang H, et al. Natural history of residual renal stone fragments after ESWL. Eur Urol. 2000;37:18–22.
Sahin C, Tuncer M, Yazici O, et al. Do the residual fragments after shock wave lithotripsy affect the quality of life? Urology. 2014;84:549–54.
Chew BH, Brotherhood HL, Sur RL, et al. Natural history, complications and re-intervention rates of asymptomatic residual stone fragments after ureteroscopy: a report from the EDGE Research Consortium. J Urol. 2016;195:982–6.
Maxwell AD, Cunitz BW, Kreider W, et al. Fragmentation of urinary calculi in vitro by burst wave lithotripsy. J Urol. 2015;193:338–44.
Dai JC, Bailey MR, Sorensen MD, et al. Innovations in ultrasound technology in the management of kidney stones. Urol Clin North Am. 2019;46:273–85.
Harper JD, Lingeman JE, Sweet RM, et al. Fragmentation of stones by burst wave lithotripsy in the first 19 humans. J Urol. 2022;207:1067–76.
Hall MK, Thiel J, Dunmire B, et al. First series using ultrasonic propulsion and burst wave lithotripsy to treat ureteral stones. J Urol. 2022;208:1075–82.
Chung DY, Kang DH, Cho KS, et al. Comparison of stone-free rates following shock wave lithotripsy, percutaneous nephrolithotomy, and retrograde intrarenal surgery for treatment of renal stones: a systematic review and network meta-analysis. PLoS ONE. 2019;14: e0211316.
Seitz C, Desai M, Häcker A, et al. Incidence, prevention, and management of complications following percutaneous nephrolitholapaxy. Eur Urol. 2012;61:146–58.
El-Nahas AR, Shokeir AA, El-Assmy AM, et al. Post-percutaneous nephrolithotomy extensive hemorrhage: a study of risk factors. J Urol. 2007;177:576–9.
Wickham JE, Kellett MJ. Percutaneous nephrolithotomy. Br J Urol. 1981;53:297–9.
Desai M, Ridhorkar V, Patel S, et al. Pediatric percutaneous nephrolithotomy: assessing impact of technical innovations on safety and efficacy. J Endourol. 1999;13:359–64.
Agarwal M, Agrawal MS, Jaiswal A, et al. Safety and efficacy of ultrasonography as an adjunct to fluoroscopy for renal access in percutaneous nephrolithotomy (PCNL). BJU Int. 2011;108:1346–9.
Corrales M, Doizi S, Barghouthy Y, et al. Ultrasound or fluoroscopy for percutaneous nephrolithotomy access, is there really a difference? A review of literature. J Endourol. 2021;35:241–8.
Usawachintachit M, Masic S, Allen IE, et al. Adopting ultrasound guidance for prone percutaneous nephrolithotomy: evaluating the learning curve for the experienced surgeon. J Endourol. 2016;30:856–63.
de la Rosette JJ, Laguna MP, Rassweiler et al. Training in percutaneous nephrolithotomy—a critical review. Eur Urol. 2008;54:994.
Tzeng BC, Wang CJ, Huang SW, et al. Doppler ultrasound-guided percutaneous nephrolithotomy: a prospective randomized study. Urology. 2011;78:535–9.
Lu MH, Pu XY, Gao X, et al. A comparative study of clinical value of single B-mode ultrasound guidance and B-mode combined with color doppler ultrasound guidance in mini-invasive percutaneous nephrolithotomy to decrease hemorrhagic complications. Urology. 2010;76:815–20.
Meola M, Ibeas J, Lasalle G, et al. Basics for performing a high-quality color Doppler sonography of the vascular access. J Vasc Access. 2021;22:18–31.
Inoue T, Kinoshita H, Okada S, et al. Wideband Doppler ultrasound-guided mini-endoscopic combined intrarenal surgery as an effective and safe procedure for management of large renal stones: a preliminary report. Urology. 2016;95:60–6.
Miyagawa T, Ishikawa S, Kimura T, et al. Real-time virtual sonography for navigation during targeted prostate biopsy using magnetic resonance imaging data. Int J Urol. 2010;10:855–60.
Haber GP, Colombo JR, Remer E, et al. Synchronized real-time ultrasonography and three-dimensional computed tomography scan navigation during percutaneous renal cryoablation in a porcine model. J Endourol. 2010;24:333–7.
Hamamoto S, Unno R, Taguchi K, et al. A new navigation system of renal puncture for endoscopic combined intrarenal surgery: real-time virtual sonography-guided renal access. Urology. 2017;109:44–50.
Rule AD, Lieske JC, Li X, et al. The ROKS nomogram for predicting a second symptomatic stone episode. J Am Soc Nephrol. 2014;25:2878–86.
D’Costa MR, Haley WE, Mara KC, et al. Symptomatic and radiographic manifestations of kidney stone recurrence and their prediction by risk factors: a prospective cohort study. J Am Soc Nephrol. 2019;30:1251–60.
Tzelves L, Geraghty R, Lombardo R, et al. Duration of follow-up and timing of discharge from imaging follow-up, in adult patients with urolithiasis after surgical or medical intervention: a systematic review and meta-analysis from the European Association of Urology Guideline Panel on Urolithiasis. Eur Urol Focus. 2023;9:188–98.
Poletti PA, Platon A, Rutschmann OT, et al. Low-dose versus standard-dose CT protocol in patients with clinically suspected renal colic. AJR Am J Roentgenol. 2007;188:927–33.
Moore CL, Carpenter CR, Heilbrun ME, et al. Imaging in suspected renal colic: systematic review of the literature and multispecialty consensus. J Urol. 2019;202:475–83.
Mitterberger M, **gera GM, Pallwein L, et al. Plain abdominal radiography with transabdominal native tissue harmonic imaging ultrasonography vs unenhanced computed tomography in renal colic. BJU Int. 2007;100:887–90.
Fahmy NM, Elkoushy MA, Andonian S. Effective radiation exposure in evaluation and follow-up of patients with urolithiasis. Urology. 2012;79:43–7.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there are no conflicts of interest.
Ethical approval
All procedures performed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and the Helsinki Declaration of 1964 and later versions. Informed consent was obtained from all patients for inclusion in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Hamamoto, S., Inoue, T., Okada, S. et al. Application of ultrasound imaging in the treatment of urinary tract stones. J Med Ultrasonics (2023). https://doi.org/10.1007/s10396-023-01343-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10396-023-01343-6