Abstract
Purpose
To evaluate the accuracy of prenatal diagnosis of congenital heart defect at the referral level in our institution.
Methods
One hundred and thirty-two cases were referred for prenatal diagnosis of congenital heart defect (CHD). Cases having CHDs were divided into isolated and complex CHDs, and the prenatal and postnatal diagnoses were compared.
Results
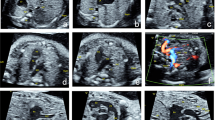
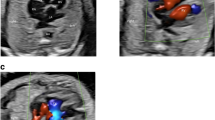
Thirty-nine cases were diagnosed with CHDs. The remaining 93 cases were diagnosed as normal. Postnatal diagnosis confirmed that 39 cases had CHDs; there were 19 cases of isolated CHD and 20 cases of complex CHD. Among the 19 cases of isolated CHD, all four cases with a false negative diagnosis had ventricular septal defects of an outlet or muscular type with a small defect. Cases with a false positive diagnosis had coarctation of the aorta (3 cases) or total anomalous pulmonary venous connection (1 case). Among the 20 cases of complex CHD, the prenatal diagnoses in two cases were not the same as the postnatal diagnosis and the prognosis was worse than expected. In one case with a single ventricle, pulmonary stenosis, and pulmonary venous atresia, the prenatal diagnosis was hypoplastic left heart syndrome with a suboptimal study at 38 weeks’ gestation. In the other case, the diagnosis of corrected transposition of the great arteries had been missed because of misinterpretation of the anatomically right and left ventricles in utero.
Conclusions
There were three possible causes of misdiagnosis or overdiagnosis of CHD: disease orientation, timing of diagnosis, and skill of the examiners. This information may be helpful for the improvement of diagnosis.

Similar content being viewed by others
References
Gembruch U. Prenatal diagnosis of congenital heart disease. Prenat Diagn. 1997;17:1283–98.
Ferencz C, Rubin JD, McCarter RJ, et al. Congenital heart disease: prevalence at livebirth. The Baltimore–Washington Infant Study. Am J Epidemiol. 1985;121:31–6.
Hoffman JI. Incidence of congenital heart disease: II. Prenatal incidence. Pediatr Cardiol. 1995;16:155–65.
Young ID, Clarke M. Lethal malformations and perinatal mortality: a 10 year review with comparison of ethnic differences. Br Med J (Clin Res Ed). 1987;295:89–91.
Saari-Kemppainen A, Karjalainen O, Ylostalo P, Heinonen OP. Ultrasound screening and perinatal mortality: controlled trial of systematic one-stage screening in pregnancy. The Helsinki Ultrasound Trial. Lancet. 1990;336:387–91.
Leivo T, Tuominen R, Saari-Kemppainen A, Ylostalo P, Karjalainen O, Heinonen OP. Cost-effectiveness of one-stage ultrasound screening in pregnancy: a report from the Helsinki ultrasound trial. Ultrasound Obstet Gynecol. 1996;7:309–14.
Bakiler AR, Ozer EA, Kanik A, Kanit H, Aktas FN. Accuracy of prenatal diagnosis of congenital heart disease with fetal echocardiography. Fetal Diagn Ther. 2007;22:241–4.
Satomi G, Kawataki M, Nishibataka M, et al. The guideline for fetal echocardiography. Pediatr Cardiol Card Surg. 2006;22:591–613 (in Japanese)
Yoshikane Y, Yoshizato T, Maeno Y, et al. Impact and issues of detecting fetal congenital heart defects in Kyushu, Japan. J Obstet Gynaecol Res. 2011;37:775–81.
Chao R, Ho E, Hsieh K. Fluctuations of interventricular shunting in a fetus with an isolated ventricular septal defect. Am Heart J. 1994;127:955–8.
Lethor JP, Marson F, de Moor M, King MEE. Physiology of ventricular septal defect shunt flow in the fetus examined by color Doppler M-mode. Circulation. 2000;101:e93–4.
Axt-Fliedner R, Schwarze A, Smrcek J, Germer U, Krapp M, Gembruch U. Isolated ventricular septal defects detected by color Doppler imaging: evolution during fetal and first year of postnatal life. Ultrasound Obstet Gynecol. 2006;27:266–73.
Brown KL, Ridout DA, Hoskote A, Verhulst L, Ricci M, Bull C. Delayed diagnosis of congenital heart disease worsens preoperative condition and outcome of surgery in neonates. Heart. 2006;92:1298–302.
Wren C, Reinhardt Z, Khawaja K. Twenty-year trends in diagnosis of life-threatening neonatal cardiovascular malformations. Arch Dis Child Fetal Neonatal Ed. 2008;93:F33–5.
Hornberger LK, Weintraub RG, Pesonen E, et al. Echocardiographic study of the morphology and growth of the aortic arch in the human fetus. Observations related to the prenatal diagnosis of coarctation. Circulation. 1992;86:741–7.
Nomiyama M, Ueda Y, Toyota Y, Kawano H. Fetal aortic isthmus growth and morphology in late gestation. Ultrasound Obstet Gynecol. 2002;19:153–7.
Sharland GK, Chan KY, Allan LD. Coarctation of the aorta: difficulties in prenatal diagnosis. Br Heart J. 1994;71:70–5.
Hornberger LK, Sahn DJ, Kleinman CS, Copel J, Silverman NH. Antenatal diagnosis of coarctation of the aorta: a multicenter experience. J Am Coll Cardiol. 1994;23:417–23.
Jung E, Won HS, Lee RP, Kim A, Park LS. Clinical implication of isolated right dominant heart in the fetus. Prenat Diagn. 2007;27:695–8.
Matsui H, Mellander M, Roughton M, Jicinska H, Gardiner HM. Morphological and physiological predictors of fetal aortic coarctation. Circulation. 2008;118:1793–801.
Pasquini L, Mellander M, Seale A, et al. Z-scores of the fetal aortic isthmus and duct: an aid to assessing arch hypoplasia. Ultrasound Obstet Gynecol. 2007;29:628–33.
Conflict of interest
There are no conflicts of interest or competing financial interests related to this work.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Yoshikane, Y., Yoshizato, T., Otake, Y. et al. Four-year experience with prenatal diagnosis of congenital heart defects at a single referral center in Japan with focus on inaccurately diagnosed cases. J Med Ultrasonics 39, 235–240 (2012). https://doi.org/10.1007/s10396-012-0362-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10396-012-0362-y