Abstract
Background
Peripheral arterial disease (PAD) is highly prevalent among individuals of higher age or those with one or more cardiovascular risk factors. Screening for PAD is recommended, since it is often linked to atherothrombotic manifestations in the coronary or carotid circulation and associated with a substantial increase in all-cause and cardiovascular mortality. We aimed to assess patients with newly diagnosed, suspected and confirmed PAD in the primary care setting with regards to clinical characteristics, diagnostic and therapeutic management (including referral to specialists), and medium-term outcomes.
Methods
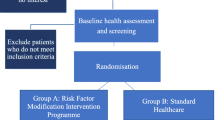
This was a multicentre, prospective, observational cohort study with a cross-sectional and a longitudinal part. A total of 2,781 general practitioners across Germany were cluster randomised to document five consecutive patients each in one of the strata: (1) patients with intermittent claudication (IC) or other typical PAD-related complaints (group A) or (2) patients >55 years of age with one or more risk factors (group B) for PAD (current smoking, diabetes, previous myocardial infection and/or previous stroke). Patients with confirmed PAD will be followed up for diagnostic procedures, therapy and vascular events over 18 months.
Results
In group A, a total of 2,131 patients with suspected PAD (80.1% confirmed, 75.9% with referral to specialists) and in group B 9,921 patients were included (44.6% confirmed, 54.6% referral). The ankle-brachial index was calculated in 41.3% and 33.5% only. Mean age was 66.6 years (group A) and 68.4 years (group B), respectively. Vascular risk factors were prevalent in both groups, in particular smoking (group A 44.6%, group B 44.4%), hypertension (73.2 and 78.1%), hypercholesterolaemia (64.6 and 70.6%) and diabetes mellitus (41.7 and 60.6%). Concomitant atherothrombotic morbidities were frequent in both groups. In patients with the respective diseases, antihypertensive, antidiabetic, lipid-lowering and antithrombotic therapies were prescribed in group A in 96.6, 96.0, 91.1 and 89.7% and in group B in 98.3, 97.4, 94.1 and 91.2%.
Conclusion
The cross-sectional part of the study indicates a substantial burden of disease in PAD patients in primary care. Treatment rates appear to have improved compared to earlier surveys. In the follow-up period, outcomes of these patients and their association with disease stages, guideline-oriented treatment or patient compliance and disease-co** strategies, among other factors, will be determined.

Similar content being viewed by others
References
(1996) A randomised, blinded, trial of clopidogrel versus aspirin in patients at risk of ischaemic events (CAPRIE) CAPRIE Steering Committee. Lancet 348:1329–1339
Antithrombotic Trialists’ Collaboration (2002) Collaborative meta-analysis of randomised trials of antiplatelet therapy for prevention of death, myocardial infarction, and stroke in high risk patients. BMJ 324:71–86
Arbeitsgruppe Epidemiologische Methoden der Deutschen Arbeitsgemeinschaft Epidemiologie (DAE) Leitlinien und Empfehlungen zur Sicherung von Guter Epidemiologischer Praxis (GEP). Available via http://www.gmds.de/texte/onlinedocs/empfehlungen/empf_gep_langfassung.htm. Accessed 18 Jul 2008
Belch JJF, Topol EJ, Agnelli G, Bertrand M, Califf RM, Clement DL, Creager MA, Easton JD, Gavin I, James R, Greenland P, Hankey G, Hanrath P, Hirsch AT, Meyer J, Smith SC, Sullivan F, Weber MA (2003) Critical issues in peripheral arterial disease detection and management: a call to action. Arch Intern Med 163:884–892
Bhatt DL, Steg PG, Ohman EM, Hirsch AT, Ikeda Y, Mas J-L, Goto S, Liau C-S, Richard AJ, Rother J, Wilson PWF, REACH Registry Investigators (2006) International prevalence, recognition, and treatment of cardiovascular risk factors in outpatients with atherothrombosis. JAMA 295:180–189
Criqui MH, Denenberg JO, Bird CE, Fronek A, Klauber MR, Langer RD (1996) The correlation between symptoms and non-invasive test results in patients referred for peripheral arterial disease testing. Vasc Med 1:65–71
Diehm C, Heidrich H, Schulte K, Spengel FA, Theiss W, für Deutsche Gesellschaft für Angiologie, Gesellschaft für Gefäßmedizin (2001) Leitlinien zur Diagnostik und Therapie der arteriellen Verschlusskrankheit der Becken-Beinarterien. VASA 30(Suppl 57):1–20
Diehm C, Schuster A, Allenberg H, Darius H, Haberl R, Lange S, Pittrow D, von Stritzky B, Tepohl G, Trampisch H (2004) High prevalence of peripheral arterial disease and co-morbidity in 6880 primary care patients: cross-sectional study. Atherosclerosis 172:95–105
Dillman D (1991) The design and administration of mail surveys. Annu Rev Sociol 17:225–249
Feringa HH, van Waning VH, Bax JJ, Elhendy A, Boersma E, Schouten O, Galal W, Vidakovic RV, Tangelder MJ, Poldermans D (2006) Cardioprotective medication is associated with improved survival in patients with peripheral arterial disease. J Am Coll Cardiol 47:1182–1187
Grumbach K, Selby JV, Damberg C, Bindman AB, Quesenberry C Jr, Truman A, Uratsu C (1999) Resolving the gatekeeper conundrum: what patients value in primary care and referrals to specialists. JAMA 282:261–266
Heald CL, Fowkes FG, Murray GD, Price JF (2006) Risk of mortality and cardiovascular disease associated with the ankle-brachial index: systematic review. Atherosclerosis 189:61–69
Heart Protection Study Collaborative Group (2002) MRC/BHF Heart Protection Study of cholesterol lowering with simvastatin in 20,536 high-risk individuals: a randomised placebo-controlled trial. Lancet 360:7–22
Hirsch AT, Gotto AM Jr (2002) Undertreatment of dyslipidemia in peripheral arterial disease and other high-risk populations: an opportunity for cardiovascular disease reduction. Vasc Med 7:323–331
Hirsch AT, Criqui MH, Treat-Jacobson D, Regensteiner JG, Creager MA, Olin JW, Krook SH, Hunninghake DB, Comerota AJ, Walsh ME, McDermott MM, Hiatt WR (2001a) Peripheral arterial disease detection, awareness, and treatment in primary care. JAMA 286:1317–1324
Hirsch AT, Halverson SL, Treat-Jacobson D, Hotvedt PS, Lunzer MM, Krook S, Rajala S, Hunninghake DB (2001b) The Minnesota Regional Peripheral Arterial Disease Screening Program: toward a definition of community standards of care. Vasc Med 6:87–96
Hirsch AT, Haskal Z, Hertzer N et al (2006) ACC/AHA guidelines for the management of patients with peripheral arterial disease (lower extremity, renal, mesenteric, and abdominal aortic): a collaborative report from the American Association for Vascular Surgery/Society for Vascular Surgery, Society for Cardiovascular Angiography and Interventions, Society for Vascular Medicine and Biology, Society of Interventional Radiology, and the ACC/AHA Task Force on Practice Guidelines (Writing Committee to Develop Guidelines for the Management of Patients With Peripheral Arterial Disease): endorsed by the American Association of Cardiovascular and Pulmonary Rehabilitation; National Heart, Lung, and Blood Institute; Society for Vascular Nursing; TransAtlantic Inter-Society Consensus; and Vascular Disease Foundation. Circulation 113:e463–e654
Holland-Letz T, Endres HG, Biedermann S, Mahn M, Kunert J, Groh S, Pittrow D, von Bilderling P, Sternitzky R, Diehm C (2007) Reproducibility and reliability of the ankle-brachial index as assessed by vascular experts, family physicians and nurses. Vasc Med 12:105–112
Kaiser V, Kester A, Stoffers H, Kitslaar P, Knottnerus J (1999) The influence of experience on the reproducibility of the ankle-brachial systolic pressure ratio in peripheral arterial occlusive disease. Eur J Vasc Endovasc Surg 18:25–29
Khan S, Flather M, Mister R, Delahunty N, Fowkes G, Bradbury A, Stansby G (2007) Characteristics and treatments of patients with peripheral arterial disease referred to UK vascular clinics: results of a prospective registry. Eur J Vasc Endovasc Surg 33:442–450
Liles DR, Kallen MA, Petersen LA, Bush RL (2006) Quality of life and peripheral arterial disease. J Surg Res 136:294–301
Norgren L, Hiatt W, Dormandy J, Nehler M, Harris K, Fowkes F et al (2007) Inter-Society Consensus for the Management of Peripheral Arterial Disease (TASC II). Eur J Vasc Endovasc Surg 33(Suppl 1):S1–S75
Ostergren J, Sleight P, Dagenais G, Danisa K, Bosch J, Qilong Y, Yusuf S, HOPE study investigators (2004) Impact of ramipril in patients with evidence of clinical or subclinical peripheral arterial disease. Eur Heart J 25:17–24
Pittrow D, Lange S, Trampisch H, Darius H, Tepohl G, Allenberg J, v. Stritzky B, Haberl R, Diehm C (2003) The German Trial on Ankle Brachial Index (getABI): high prevalence and evidence for antiplatelet undertreatment of peripheral arterial disease in primary care (abstract). Int J Clin Pharmacol Ther 41 (445(P27))
Statistisches Bundesamt (2006) Ten leading causes of mortality in Germany in 2006 (in German). Available via http://www.destatis.de/jetspeed/portal/cms/Sites/destatis/Internet/DE/Content/Statistiken/Gesundheit/Todesursachen/Tabellen/Content75/SterbefaelleInsgesamt,templateId=renderPrint.psml. Accessed 18 Jul 2008
van Elderen T, Maes S, Dusseldorp E (1999) Co** with coronary heart disease: a longitudinal study. J Psychosom Res 47:175–183
Yao ST, Hobbs JT, Irvine WT (1969) Ankle systolic pressure measurements in arterial disease affecting the lower extremities. Br J Surg 56:676–679
Yusuf S, Sleight P, Pogue J, Bosch J, Davies R, Dagenais G (2000) Effects of an angiotensin-converting-enzyme inhibitor, ramipril, on cardiovascular events in high-risk patients. The Heart Outcomes Prevention Evaluation Study Investigators. N Engl J Med 342:145–153
Yusuf S, Hawken S, Ounpuu S, Dans T, Avezum A, Lanas F, McQueen M, Budaj A, Pais P, Varigos J, Lisheng L, INTERHEART Study Investigators (2004) Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): case-control study. Lancet 364:937–952
Acknowledgements
The study is supported by an unrestricted educational grant from Sanofi-Aventis Pharma. We thank Anja Neumann for her a strong commitment in the project office. Further, we appreciate the help of the participating GPs for collecting the data for the study and their practice staff for their assistance.
Conflict of interest
The authors confirm that there are no relevant associations that might pose a conflict of interest.
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
The study group was supported by an advisory board founded in 2003 with the following members: Hans Jürgen Ahrens, Curt Diehm, Leonhard Hansen (until 2004), Klaus-Dieter Kossow.
Rights and permissions
About this article
Cite this article
Neumann, A., Jahn, R., Diehm, C. et al. Presentation and medical management of peripheral arterial disease in general practice: rationale, aims, design and baseline results of the PACE-PAD Study. J Public Health 17, 127–135 (2009). https://doi.org/10.1007/s10389-008-0223-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10389-008-0223-8