Abstract
Introduction
Considering the extension of working life due to socioeconomic and political factors, many people may experience cognitive complaints (CC) at their workplace, with severe consequences on their quality of life. The identification of workers reporting significative SCC is crucial to eventually address them to an objective neuropsychological evaluation and implement cognitive interventions to guarantee workers’ well-being. Since no Italian questionnaires for detecting CC were designed for occupational settings, the aim of the study was to validate the Italian version of the Cognitive Function at Work Questionnaire (CFWQ) and to provide its normative data.
Materials and methods
Internal consistency, convergent and divergent validity, and factorial structure of the CFWQ were evaluated. A regression-based procedure served to compute percentiles of CFWQ and its subscales.
Results
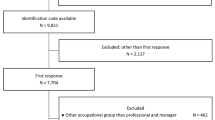
Four hundred twenty-one participants without psychiatric and/or neurological disorders completed the survey. We found that the Italian CFWQ included 26 items, with a good internal consistency (Cronbach’s alpha = 0.897) and a six-factor structure (memory, language, processing speed, abstract thinking/behavioral control, behavioral inertia, planning ability). CFWQ score did not correlate with empathy but correlated strongly with memory scores and moderately with anxiety and depression scores.
Conclusions
The Italian CFWQ showed good psychometric properties, in analogy with the original English scale. Therefore, it can be successfully employed in organizational contexts to possibly identify workers with CC and therefore with possible co-occurrent psychological, behavioral, and cognitive consequences.
Similar content being viewed by others
Data availability
The dataset analyzed during the current study is available from the corresponding author upon reasonable request.
References
Mendonça MD, Alves L, Bugalho P (2016) From subjective cognitive complaints to dementia: who is at risk?: a systematic review. Am J Alzheimers Dis Other Demen 31:105–114. https://doi.org/10.1177/1533317515592331
Edmonds EC, Delano-Wood L, Galasko DR et al (2014) Subjective cognitive complaints contribute to misdiagnosis of mild cognitive impairment. J Int Neuropsychol Soc 20:836–847. https://doi.org/10.1017/S135561771400068X
Rijs KJ, den Kommer TNV, Comijs HC, Deeg DJH (2015) Prevalence and incidence of memory complaints in employed compared to non-employed aged 55–64 years and the role of employment characteristics. PLoS One 10:e0119192. https://doi.org/10.1371/journal.pone.0119192
Taylor CA, Bouldin ED, McGuire LC (2018) Subjective cognitive decline among adults aged ≥45 years - United States, 2015–2016. MMWR Morb Mortal Wkly Rep 67:753–757. https://doi.org/10.15585/mmwr.mm6727a1
van Harten AC, Mielke MM, Swenson-Dravis DM et al (2018) Subjective cognitive decline and risk of MCI: the Mayo Clinic Study of Aging. Neurology 91:e300–e312. https://doi.org/10.1212/WNL.0000000000005863
Markova H, Nikolai T, Mazancova AF et al (2019) Differences in subjective cognitive complaints between non-demented older adults from a memory clinic and the community. Journal of Alzheimer’s Disease 70:61–73. https://doi.org/10.3233/JAD-180630
Jessen F, Amariglio RE, van Boxtel M et al (2014) A conceptual framework for research on subjective cognitive decline in preclinical Alzheimer’s disease. Alzheimers Dement 10:844–852. https://doi.org/10.1016/j.jalz.2014.01.001
Jessen F, Amariglio RE, Buckley RF et al (2020) The characterisation of subjective cognitive decline. Lancet Neurol 19:271–278. https://doi.org/10.1016/S1474-4422(19)30368-0
Brown MJ, Hill NL, Haider MR (2022) Age and gender disparities in depression and subjective cognitive decline-related outcomes. Aging Ment Health 26:48–55. https://doi.org/10.1080/13607863.2020.1861214
Cheng G-R, Liu D, Huang L-Y et al (2023) Prevalence and risk factors for subjective cognitive decline and the correlation with objective cognition among community-dwelling older adults in China: results from the Hubei memory and aging cohort study. Alzheimer’s Dement. https://doi.org/10.1002/alz.13047
Cheng Y-W, Chen T-F, Chiu M-J (2017) From mild cognitive impairment to subjective cognitive decline: conceptual and methodological evolution. Neuropsychiatr Dis Treat 13:491–498. https://doi.org/10.2147/NDT.S123428
Si T, **ng G, Han Y (2020) Subjective cognitive decline and related cognitive deficits. Front Neurol 11. https://doi.org/10.3389/fneur.2020.00247
Comijs HC, Deeg DJH, Dik MG et al (2002) Memory complaints; the association with psycho-affective and health problems and the role of personality characteristics. A 6-year follow-up study. J Affect Disord 72:157–165. https://doi.org/10.1016/s0165-0327(01)00453-0
Slavin MJ, Brodaty H, Kochan NA et al (2010) Prevalence and predictors of “subjective cognitive complaints” in the Sydney Memory and Ageing Study. Am J Geriatr Psychiatry 18:701–710. https://doi.org/10.1097/jgp.0b013e3181df49fb
Hohman TJ, Beason-Held LL, Resnick SM (2011) Cognitive complaints, depressive symptoms, and cognitive impairment: are they related? J Am Geriatr Soc 59:1908–1912. https://doi.org/10.1111/j.1532-5415.2011.03589.x
Stogmann E, Moser D, Klug S et al (2016) Activities of daily living and depressive symptoms in patients with subjective cognitive decline, mild cognitive impairment, and Alzheimer’s disease. J Alzheimers Dis 49:1043–1050. https://doi.org/10.3233/JAD-150785
Raimo S, Trojano L, Siciliano M et al (2016) Psychometric properties of the Italian version of the multifactorial memory questionnaire for adults and the elderly. Neurol Sci 37:681–691. https://doi.org/10.1007/s10072-016-2562-5
Mol MEM, van Boxtel MPJ, Willems D et al (2009) Subjective forgetfulness is associated with lower quality of life in middle-aged and young-old individuals: a 9-year follow-up in older participants from the Maastricht Aging Study. Aging Ment Health 13:699–705. https://doi.org/10.1080/13607860902845541
Bassett SS, Folstein MF (1993) Memory complaint, memory performance, and psychiatric diagnosis: a community study. J Geriatr Psychiatry Neurol 6:105–111. https://doi.org/10.1177/089198879300600207
Jessen F, Feyen L, Freymann K et al (2006) Volume reduction of the entorhinal cortex in subjective memory impairment. Neurobiol Aging 27:1751–1756. https://doi.org/10.1016/j.neurobiolaging.2005.10.010
Jungwirth S, Fischer P, Weissgram S et al (2004) Subjective memory complaints and objective memory impairment in the Vienna-Transdanube aging community. J Am Geriatr Soc 52:263–268. https://doi.org/10.1111/j.1532-5415.2004.52066.x
Allison SL, Rodebaugh TL, Johnston C et al (2019) Develo** a spatial navigation screening tool sensitive to the preclinical Alzheimer disease continuum. Arch Clin Neuropsychol 34:1138–1155. https://doi.org/10.1093/arclin/acz019
Crowe M, Andel R, Wadley V et al (2006) Subjective cognitive function and decline among older adults with psychometrically defined amnestic MCI. Int J Geriat Psychiatry 21:1187–1192. https://doi.org/10.1002/gps.1639
Santangelo G, Baldassarre I, Barbaro A et al (2021) Subjective cognitive failures and their psychological correlates in a large Italian sample during quarantine/self-isolation for COVID-19. Neurol Sci 42:2625–2635. https://doi.org/10.1007/s10072-021-05268-1
Russo A, Silvestro M, Garramone F et al (2020) A subjective cognitive impairments scale for migraine attacks: validation of the Italian version of the MIG-SCOG. Neurol Sci 41:1139–1143. https://doi.org/10.1007/s10072-019-04200-y
Youn JC, Kim KW, Lee DY et al (2009) Development of the subjective memory complaints questionnaire. Dement Geriatr Cogn Disord 27:310–317. https://doi.org/10.1159/000205512
Ávila-Villanueva M, Rebollo-Vázquez A, Ruiz-Sánchez de León JM et al (2016) Clinical relevance of specific cognitive complaints in determining mild cognitive impairment from cognitively normal states in a study of healthy elderly controls. Front Aging Neurosci 8:233. https://doi.org/10.3389/fnagi.2016.00233
Gifford KA, Liu D, Romano RR et al (2015) Development of a subjective cognitive decline questionnaire using item response theory: a pilot study. Alzheimer’s Dement 1:429–439. https://doi.org/10.1016/j.dadm.2015.09.004
La Joie R, Perrotin A, Egret S et al (2016) Qualitative and quantitative assessment of self-reported cognitive difficulties in nondemented elders: association with medical help seeking, cognitive deficits, and β-amyloid imaging. Alzheimer’s Dement 5:23–34. https://doi.org/10.1016/j.dadm.2016.12.005
Lubitz AF, Eid M, Niedeggen M (2018) Complainer profile identification (CPI): properties of a new questionnaire on subjective cognitive complaints. Aging Neuropsychol Cogn 25:99–121. https://doi.org/10.1080/13825585.2016.1267325
Wallace JC, Chen G (2005) Development and validation of a work-specific measure of cognitive failure: implications for occupational safety. J Occup Organ Psychol 78:615–632. https://doi.org/10.1348/096317905X37442
Heikkinen A-L, Hänninen T, Kuikka P et al (2021) The Cognitive Function at Work Questionnaire (CFWQ): a new scale for measuring cognitive complaints in occupational population. Appl Neuropsychol Adult 1–12. https://doi.org/10.1080/23279095.2021.1970553
Kuikka P, Ritva A, Veijo P, Juhani S (2011) Miksi muisti pätkii? Pekka Kuikka, Ritva Akila, Veijo Pulliainen, Juhani Salo. Työterveyslaitos
Das M, Ester P, Kaczmirek L (2011) Social and behavioral research and the internet: advances in applied methods and research strategies. Routledge, New York
Hunter RF, Gough A, O’Kane N et al (2018) Ethical issues in social media research for public health. Am J Public Health 108:343–348. https://doi.org/10.2105/AJPH.2017.304249
Beaton DE, Bombardier C, Guillemin F, Ferraz MB (2000) Guidelines for the process of cross-cultural adaptation of self-report measures. Spine (Phila Pa 1976) 25:3186–3191. https://doi.org/10.1097/00007632-200012150-00014
Spitzer RL, Kroenke K, Williams JBW, Löwe B (2006) A brief measure for assessing generalized anxiety disorder: the GAD-7. Arch Intern Med 166:1092–1097. https://doi.org/10.1001/archinte.166.10.1092
Mazzotti E, Fassone G, Picardi A et al (2003) II Patient Health Questionnaire (PHQ) per lo screening dei disturbi psichiatrici: Uno studio di validazione nei confronti della Intervista Clinica Strutturata per il DSM-IV asse I (SCID-I). Ital J Psychopathol 9:235–242
Chiorri C (2016) Competing factor structures for the Toronto Empathy Questionnaire. The Neurobiology and Psychology of Empathy. Nova Science Publishers Inc, New York, pp 399–432
Altieri M, Maggi G, Rippa V, Santangelo G (2023) Evaluation of apathy in non-clinical populations: validation, psychometric properties, and normative data of the Italian version of Apathy-Motivation Index (AMI). Neurol Sci. https://doi.org/10.1007/s10072-023-06774-0
Maggi G, Altieri M, Ilardi CR, Santangelo G (2022) Validation of a short Italian version of the Barratt Impulsiveness Scale (BIS-15) in non-clinical subjects: psychometric properties and normative data. Neurol Sci 43:4719–4727. https://doi.org/10.1007/s10072-022-06047-2
Maggi G, D’Iorio A, Aiello EN et al (2023) Psychometrics and diagnostics of the Italian version of the Beck Depression Inventory-II (BDI-II) in Parkinson’s disease. Neurol Sci. https://doi.org/10.1007/s10072-023-06619-w
George D, Mallery P (2019) IBM SPSS Statistics 26 step by step: a simple guide and reference, 16th edn. Routledge, New York
Nucci M, Mapelli D, Mondini S (2012) Cognitive reserve index questionnaire (CRIq): a new instrument for measuring cognitive reserve. Aging Clin Exp Res 24:218–226. https://doi.org/10.3275/7800
Rabin LA, Smart CM, Crane PK et al (2015) Subjective cognitive decline in older adults: an overview of self-report measures used across 19 international research studies. J Alzheimers Dis 48(Suppl 1):S63-86. https://doi.org/10.3233/JAD-150154
Liew TM (2019) Depression, subjective cognitive decline, and the risk of neurocognitive disorders. Alzheimer’s Res Ther 11:70. https://doi.org/10.1186/s13195-019-0527-7
Liew TM (2020) Subjective cognitive decline, anxiety symptoms, and the risk of mild cognitive impairment and dementia. Alzheimers Res Ther 12:107. https://doi.org/10.1186/s13195-020-00673-8
Molinuevo JL, Rabin LA, Amariglio R et al (2017) Implementation of subjective cognitive decline criteria in research studies. Alzheimers Dement 13:296–311. https://doi.org/10.1016/j.jalz.2016.09.012
Belloni M, Carrino L, Meschi E (2022) The impact of working conditions on mental health: novel evidence from the UK. Labour Econ 76:102176. https://doi.org/10.1016/j.labeco.2022.102176
McCarthy JM, Trougakos JP, Cheng BH (2016) Are anxious workers less productive workers? It depends on the quality of social exchange. J Appl Psychol 101:279–291. https://doi.org/10.1037/apl0000044
Mendes T, Ginó S, Ribeiro F et al (2008) Memory complaints in healthy young and elderly adults: reliability of memory reporting. Aging Ment Health 12:177–182. https://doi.org/10.1080/13607860701797281
Schliep KC, Barbeau WA, Lynch KE et al (2022) Overall and sex-specific risk factors for subjective cognitive decline: findings from the 2015–2018 behavioral risk factor surveillance system survey. Biol Sex Differ 13:16. https://doi.org/10.1186/s13293-022-00425-3
Sundermann EE, Edmonds EC, Delano-Wood L et al (2018) Sex influences the accuracy of subjective memory complaint reporting in older adults. J Alzheimers Dis 61:1163–1178. https://doi.org/10.3233/JAD-170425
Stern Y (2009) Cognitive reserve. Neuropsychologia 47:2015–2028. https://doi.org/10.1016/j.neuropsychologia.2009.03.004
Gu L, Xu H (2022) Effect of cognitive reserve on cognitive function in Parkinson’s disease. Neurol Sci 43:4185–4192. https://doi.org/10.1007/s10072-022-05985-1
Lavrencic LM, Churches OF, Keage HA (2018) Cognitive reserve is not associated with improved performance in all cognitive domains - PubMed. Appl Neuropsychol Adult 25:473–485. https://doi.org/10.1080/23279095.2017.1329146
Santangelo G, Altieri M, Enzinger C et al (2019) Cognitive reserve and neuropsychological performance in multiple sclerosis: a meta-analysis. Neuropsychology 33:379–390. https://doi.org/10.1037/neu0000520
Santangelo G, Altieri M, Gallo A, Trojano L (2019) Does cognitive reserve play any role in multiple sclerosis? A meta-analytic study. Mult Scler Relat Disord 30:265–276. https://doi.org/10.1016/j.msard.2019.02.017
de Souza-Talarico JN, Caramelli P, Nitrini R, Chaves EC (2007) The influence of schooling on working memory performance in elderly individuals without cognitive decline. Dement Neuropsychol 1:276. https://doi.org/10.1590/S1980-57642008DN10300009
Szajer J, Murphy C (2013) Education level predicts retrospective metamemory accuracy in healthy aging and Alzheimer’s disease. J Clin Exp Neuropsychol 35:971–982. https://doi.org/10.1080/13803395.2013.844771
Angel L, Guerrerro-Sastoque L, Bernardo M et al (2022) Metamemory mediates the protective effect of cognitive reserve on episodic memory during aging. Acta Psychol (Amst) 228:103627. https://doi.org/10.1016/j.actpsy.2022.103627
Ohtani K, Hisasaka T (2018) Beyond intelligence: a meta-analytic review of the relationship among metacognition, intelligence, and academic performance. Metacognition Learn 13:179–212. https://doi.org/10.1007/s11409-018-9183-8
Teodoro T, Koreki A, Chen J et al (2023) Functional cognitive disorder affects reaction time, subjective mental effort and global metacognition. Brain 146:1615–1623. https://doi.org/10.1093/brain/awac363
Bhome R, McWilliams A, Price G et al (2022) Metacognition in functional cognitive disorder. Brain Commun 4:fcac041. https://doi.org/10.1093/braincomms/fcac041
Bhome R, McWilliams A, Huntley JD et al (2019) Metacognition in functional cognitive disorder- a potential mechanism and treatment target. Cogn Neuropsychiatry 24:311–321. https://doi.org/10.1080/13546805.2019.1651708
Jenkins A, Tree J, Tales A (2021) Distinct profile differences in subjective cognitive decline in the general public are associated with metacognition, negative affective symptoms, neuroticism, stress, and poor quality of life. J Alzheimers Dis 80:1231–1242. https://doi.org/10.3233/JAD-200882
Norman E (2020) Why metacognition is not always helpful. Front Psychol 11. https://doi.org/10.3389/fpsyg.2020.01537
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
The study was approved by the ethics committee of University of Campania “Luigi Vanvitelli,” and it was performed in accordance with the Declaration of Helsinki and its later amendments.
Consent to participate
Each participant provided a written informed consent to the study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Altieri, M., Maggi, G., Giacobbe, C. et al. Psychometric properties and normative data of the Italian version of the Cognitive Function at Work Questionnaire: a screening tool for detecting subjective cognitive complaints at work. Neurol Sci 45, 2593–2603 (2024). https://doi.org/10.1007/s10072-023-07265-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-023-07265-y