Abstract
Background
Cognitive impairment is a frequent disabling feature of Parkinson’s disease (PD). Orthostatic hypotension (OH) is treatable and may be a risk factor for cognitive impairment.
Objective
We conducted a systematic review and meta-analysis to examine the relationship between OH with PD-associated minimal cognitive impairment (PD-MCI) and dementia (PDD) and assess the mitigating effects of potential confounding factors.
Methods
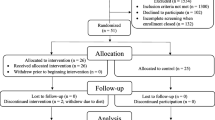
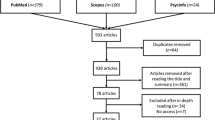
Observational studies published in English, Spanish, French, or Portuguese up to January 2022 were searched for in PubMed, EBSCO, and SciELO databases. The primary aim of this study was to revise the association between OH with PD-MCI and PDD. Alongside, we assessed OH as related to cognitive rating scales. Fixed and random models were fitted. Meta-regression was used to assess the mitigating effects of confounding variables.
Results
We identified 18 studies that reported OH association with PDD or PD-MCI, 15 of them reporting OH association with cognitive rating scales. OH was significantly associated with PDD/PD-MCI (OR, 95% CI: 3.31, 2.16–5.08; k = 18, n = 2251; p < 0.01). OH association with PDD (4.64, 2.68–8.02; k = 13, n = 1194; p < 0.01) was stronger than with PD-MCI (1.82, 0.92–3.58; k = 5, n = 1056; p = NS). The association between OH and PD-MCI/PDD was stronger in studies with a higher proportion of women and in those with a lower frequency of supine hypertension. Global cognition rating scale scores were lower in patients with OH (SMD, 95% CI: − 0.55, − 0.83/ − 0.26; k = 12, n = 1427; p < 0.01).
Conclusions
Orthostatic hypotension shows as a significant risk factor for cognitive impairment in PD, especially in women and patients not suffering from hypertension.





Similar content being viewed by others
Data Availability
Data is available upon request to the authors.
Change history
17 January 2023
A Correction to this paper has been published: https://doi.org/10.1007/s10072-023-06612-3
References
Aarsland D, Batzu L, Halliday GM et al (2021) Parkinson disease-associated cognitive impairment. Nat Rev Dis Primers 7:1–21. https://doi.org/10.1038/s41572-021-00280-3
Hely MA, Reid WG, Adena MA, Halliday GM, Morris JG (2008) The Sydney multicenter study of Parkinson’s disease: the inevitability of dementia at 20 years. Mov Disord 23:837–844
Williams-Gray CH (2009) The distinct cognitive syndromes of Parkinson’s disease: 5 year follow-up of the CamPaIGN cohort. Brain 132:2958–2969
Leroi I, McDonald K, Pantula H, Harbishettar V (2012) Cognitive impairment in Parkinson disease: impact on quality of life, disability, and caregiver burden. J Geriatr Psychiatry Neurol 25:208–214. https://doi.org/10.1177/0891988712464823
Vossius C, Larsen JP, Janvin C, Aarsland D (2011) The economic impact of cognitive impairment in Parkinson’s disease. Mov Disord 26:1541–1544. https://doi.org/10.1002/MDS.23661
Fanciulli A, Leys F, Falup-Pecurariu C, Thijs R, Wenning GK (2020) Management of orthostatic hypotension in Parkinson’s disease. J Parkinsons Dis 10:S57–S64. https://doi.org/10.3233/JPD-202036
Page MJ, McKenzie JE, Bossuyt PM et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:71. https://doi.org/10.1136/BMJ.N71
Bell CC (1994) DSM-IV: Diagnostic and Statistical Manual of Mental Disorders. JAMA 272:828–829. https://doi.org/10.1001/JAMA.1994.03520100096046
Emre M, Aarsland D, Brown RG et al (2007) Clinical diagnostic criteria for dementia associated with Parkinson’s disease. Mov Disord 22:1689–1707. https://doi.org/10.1002/MDS.21507
Dubois B, Burn D, Goetz CG et al (2007) Diagnostic procedures for Parkinson’s disease dementia: recommendations from the movement disorder society task force. Mov Disord 22:2314–2324. https://doi.org/10.1002/MDS.21844
Litvan I, Aarsland D, Adler CH et al (2011) MDS Task Force on Mild Cognitive Impairment in Parkinson’s disease: critical review of PD-MCI. Mov Disord 26:1814. https://doi.org/10.1002/MDS.23823
Freeman R, Wieling W, Axelrod FB et al (2011) Consensus statement on the definition of orthostatic hypotension, neurally mediated syncope and the postural tachycardia syndrome. Clin Auton Res 21:69–72. https://doi.org/10.1007/S10286-011-0119-5
Schatz IJ, Bannister R, Freeman RL et al (1996) Consensus statement on the definition of orthostatic hypotension, pure autonomic failure, and multiple system atrophy. Neurology 46:1470. https://doi.org/10.1212/WNL.46.5.1470
Sterne JA, Hernán MA, Reeves BC et al (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355:i4919. https://doi.org/10.1136/BMJ.I4919
Balduzzi S, Rücker G, Schwarzer G (2019) How to perform a meta-analysis with R: a practical tutorial. Evid Based Ment Health 22:153–160. https://doi.org/10.1136/EBMENTAL-2019-300117
Higgins JPT, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560. https://doi.org/10.1136/BMJ.327.7414.557
Kim J-S, Oh Y-S, Lee K-S, Kim Y-I, Yang D-W, Goldstein DS (2012) Association of cognitive dysfunction with neurocirculatory abnormalities in early Parkinson disease. Neurology 79:1323–1331. https://doi.org/10.1212/WNL.0b013e31826c1acd
Li L, Guo P, Ding D et al (2019) Parkinson’s disease with orthostatic hypotension: analyses of clinical characteristics and influencing factors. Neurol Res 41:734–741. https://doi.org/10.3389/fneur.2019.00363.10(1080/01616412),pp.1610224,2019
Peralta C, Stampfer-Kountchev M, Karner E et al (2007) Orthostatic hypotension and attention in Parkinson’s disease with and without dementia. J Neural Transm (Vienna) 114:585–588. https://doi.org/10.1007/s00702-006-0615-2
Pilleri M, Facchini S, Gasparoli E et al (2013) Cognitive and MRI correlates of orthostatic hypotension in Parkinson’s disease. J Neurol 260:253–259. https://doi.org/10.1007/s00415-012-6627-y
Tanaka R, Yamashiro K, Ogawa T et al (2020) The absence of orthostatic heart rate increase is associated with cognitive impairment in Parkinson’s disease. PLoS One 15:e0240491. https://doi.org/10.1371/JOURNAL.PONE.0240491
Umehara T, Oka H, Nakahara A, Matsuno H, Toyoda C (2018) High norepinephrinergic orthostatic hypotension in early Parkinson’s disease. Parkinsonism Relat Disord 55:97–102. https://doi.org/10.1016/j.clinph.2018.05.003.10.1016/j.parkreldis.2018.05.025
Anang JB, Gagnon JF, Bertrand JA et al (2014) Predictors of dementia in Parkinson disease: a prospective cohort study. Neurology 83:1253–1260. https://doi.org/10.1212/WNL.0000000000000842
Hussain MW, Camicioli R (2018) Nonmotor symptoms of Parkinson’s disease as predictors of dementia. Can J Neurol Sci 45:97–99. https://doi.org/10.1016/j.parkreldis.2017.10.014.10.1017/cjn.2017.239
Idiaquez J, Benarroch EE, Rosales H, Milla P, Rios L (2007) Autonomic and cognitive dysfunction in Parkinson’s disease. Clin Auton Res 17:93–98. https://doi.org/10.1007/s10286-007-0410-7
Centi J, Freeman R, Gibbons CH, Neargarder S, Canova AO, Cronin-Golomb A (2017) Effects of orthostatic hypotension on cognition in Parkinson disease. Neurology 88:17–24. https://doi.org/10.1212/wnl.0000000000003452
Daida K, Tanaka R, Yamashiro K et al (2018) The presence of cerebral microbleeds is associated with cognitive impairment in Parkinson’s disease. Parkinsons Dis 393:39–44. https://doi.org/10.1155/2018/3136415
Fanciulli A, Gobel G, Ndayisaba JP et al (2016) Supine hypertension in Parkinson’s disease and multiple system atrophy. Clin Auton Res 26:97–105. https://doi.org/10.1007/s10286-015-0336-4
Allcock LM, Kenny RA, Mosimann UP et al (2006) Orthostatic hypotension in Parkinson’s disease: association with cognitive decline? Int J Geriatr Psychiatry 21:778–783. https://doi.org/10.1002/gps.1562
Bae HJ, Lim JH, Cheon SM (2014) Orthostatic hypotension and cognitive impairment in de novo patients with Parkinson’s disease. J Mov Disord 7:102–4. https://doi.org/10.14802/jmd.14016
Chen SW, Wang YK, Dou RH et al (2020) Characteristics of the 24-h ambulatory blood pressure monitoring in patients with Parkinson’s disease - the SFC BP multicentre study in China. J Hypertens 38:2270–2278. https://doi.org/10.1097/HJH.0000000000002536
Dadar M, Fereshtehnejad SM, Zeighami Y, Dagher A, Postuma RB, Collins DL (2020) White matter hyperintensities mediate impact of dysautonomia on cognition in Parkinson’s disease. Mov Disord Clin Pract 7:639–647. https://doi.org/10.1002/mdc3.13003
Longardner K, Bayram E, Litvan I (2020) Orthostatic hypotension is associated with cognitive decline in Parkinson disease. Front Neurol 11:897. https://doi.org/10.3389/FNEUR.2020.00897
Oka H, Umehara T, Nakahara A, Matsuno H (2020) Comparisons of cardiovascular dysautonomia and cognitive impairment between de novo Parkinson’s disease and de novo dementia with Lewy bodies. BMC Neurol 20:350. https://doi.org/10.1186/S12883-020-01928-5
Shin NY, Park YW, Yoo SW et al (2021) Adverse effects of hypertension, supine hypertension, and perivascular space on cognition and motor function in PD. NPJ Parkinsons Dis 7:69. https://doi.org/10.1038/S41531-021-00214-6
Yoo SW, Oh YS, Yoo JY et al (2020) Intervening effects of orthostatic blood pressure change on subcortical atrophy and cognition in de novo and drug-naive Parkinson’s disease. J Parkinsons Dis 10:153–160. https://doi.org/10.3233/JPD-191748
Kang SH, Chung SJ, Lee J, Koh SB (2022) Independent effect of neurogenic orthostatic hypotension on mild cognitive impairment in Parkinson’s disease. Clin Auton Res 32:43–50. https://doi.org/10.1007/s10286-021-00841-2
Longardner K, Merola A, Litvan I et al (2022) Differential impact of individual autonomic domains on clinical outcomes in Parkinson’s disease. J Neurol 269:5510–5520. https://doi.org/10.1007/s00415-022-11221-9
Yin K, Zhou C, Zhu Y et al (2022) REM sleep behavioral disorder may be an independent risk factor for orthostatic hypotension in Parkinson’s disease. Aging Clin Exp Res 34:159–166. https://doi.org/10.1007/s40520-021-01887-y
Guo Y, Liu FT, Hou XH et al (2021) Predictors of cognitive impairment in Parkinson’s disease: a systematic review and meta-analysis of prospective cohort studies. J Neurol 268:2713–2722. https://doi.org/10.1007/S00415-020-09757-9
Guo Y, Xu W, Liu F-T et al (2019) Modifiable risk factors for cognitive impairment in Parkinson's disease: a systematic review and meta-analysis of prospective cohort studies. Mov Disord 34:876–883. https://doi.org/10.1002/mds.27665
Lam RW, Kennedy SH, McIntyre RS, Khullar A (2014) Cognitive dysfunction in major depressive disorder: effects on psychosocial functioning and implications for treatment. Can J Psychiatry 59:649. https://doi.org/10.1177/070674371405901206
Raz L, Knoefel J, Bhaskar K (2016) The neuropathology and cerebrovascular mechanisms of dementia. J Cereb Blood Flow Metab 36:172–186. https://doi.org/10.1038/JCBFM.2015.164
Pilotto A, Romagnolo A, Scalvini A et al (2021) Association of orthostatic hypotension with cerebral atrophy in patients with Lewy body disorders. Neurology 97:e814–e824. https://doi.org/10.1212/WNL.0000000000012342
De Anda-Duran I, Woltz SG, Bell CN, Bazzano LA (2022) Hypertension and cognitive function: a review of life-course factors and disparities. Curr Opin Cardiol 37:326–333. https://doi.org/10.1097/HCO.0000000000000975
Blanken AE, Nation DA (2020) Does gender influence the relationship between high blood pressure and dementia? Highlighting areas for further investigation. J Alzheimers Dis 78:23–48. https://doi.org/10.3233/JAD-200245
Jiménez-Sánchez L, Hamilton OKL, Clancy U et al (2021) Sex differences in cerebral small vessel disease: a systematic review and meta-analysis. Front Neurol 12:756887. https://doi.org/10.3389/FNEUR.2021.756887
Cani I, Sambati L, Bartiromo F et al (2022) Cognitive profile in idiopathic autonomic failure: relation with white matter hyperintensities and neurofilament levels. Ann Clin Transl Neurol 9:864–876. https://doi.org/10.1002/acn3.51567
Author information
Authors and Affiliations
Contributions
Research project = SPLL, OJP.
Data collection and evaluation = DL, RB.
Data analysis = SPLL, SB, LG.
Manuscript preparation = SPLL.
Academic editing (grammar and style) and proofreading: MOL.
Manuscript revision = DL, RB, SB, LG, FC, MOL, OJP.
Corresponding author
Ethics declarations
Conflict of interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: The above article was published with error. The author Francisco Capani contains only two affiliations instead of four. This has been corrected here.
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Loureiro, D., Bilbao, R., Bordet, S. et al. A systematic review and meta-analysis on the association between orthostatic hypotension and mild cognitive impairment and dementia in Parkinson’s disease. Neurol Sci 44, 1211–1222 (2023). https://doi.org/10.1007/s10072-022-06537-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-022-06537-3