Abstract
Objective
The putative effect of lesion-induced brain damage on post-stroke upper limb motor impairment can be estimated by overlaying a patient's lesion or its surrogate with key motor areas. We assessed the predictive value of imaging-based brain damage measures for cross-sectional upper limb motor impairment and subsequent upper limb motor outcome after stroke.
Methods
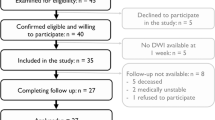
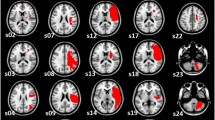
In 47 stroke patients, upper limb motor impairment was evaluated with the Upper-Extremity Fugl-Meyer Assessment (UE-FMA) at 2 weeks (2W) and 3 months (3M) post-stroke. Given each patient’s lesion identified at 2W, we considered the disconnectome, estimated as an ensemble of structural and functional connections passing through the lesion, as a surrogate of the lesion. The lesion load and the disconnectome load were measured by overlaying the lesion and disconnectome with the corticospinal tract (CST) and motor cortex (MC), and their association with the UE-FMA score at 2W and 3M was assessed.
Results
Whereas the disconnectome loads on the CST and MC were better in predicting the UE-FMA score at 2W, the lesion load on the CST was better in predicting the UE-FMA score at 3M. Furthermore, when the CST lesion load was combined with the UE-FMA score at 2W, the UE-FMA score at 3M was better predicted, with smaller generalization error, than by using either measure alone.
Conclusions
The combination of the CST lesion load and baseline upper limb motor impairment would provide a tailored fusion of imaging and clinical measures for more accurate motor outcome prediction.


Similar content being viewed by others
References
Chen C-L, Tang F-T, Chen H-C, Chung C-Y, Wong M-K (2000) Brain lesion size and location: effects on motor recovery and functional outcome in stroke patients. Arch Phys Med Rehabil 81(4):447–452. https://doi.org/10.1053/mr.2000.3837
Zhu LL, Lindenberg R, Alexander MP, Schlaug G (2010) Lesion load of the corticospinal tract predicts motor impairment in chronic stroke. Stroke 41(5):910–915. https://doi.org/10.1161/STROKEAHA.109.577023
Feng W, Wang J, Chhatbar PY, Doughty C, Landsittel D, Lioutas VA et al (2015) Corticospinal tract lesion load: an imaging biomarker for stroke motor outcomes. Ann Neurol 78(6):860–870. https://doi.org/10.1002/ana.24510
Park C, Kou N, Ward NS (2016) The contribution of lesion location to upper limb deficit after stroke. J Neurol Neurosurg Psychiatry 87(12):1283–1286. https://doi.org/10.1136/jnnp-2015-312738
Rondina JM, Park C, Ward NS (2017) Brain regions important for recovery after severe post-stroke upper limb paresis. J Neurol Neurosurg Psychiatry 88(9):737–743. https://doi.org/10.1136/jnnp-2016-315030
Foulon C, Cerliani L, Kinkingnéhun S, Levy R, Rosso C, Urbanski M et al (2018) Advanced lesion symptom map** analyses and implementation as BCBtoolkit. Gigascience 7(3):1–17. https://doi.org/10.1093/gigascience/giy004
Kuceyeski A, Navi BB, Kamel H, Raj A, Relkin N, Toglia J et al (2016) Structural connectome disruption at baseline predicts 6-months post-stroke outcome. Hum Brain Mapp 37(7):2587–2601. https://doi.org/10.1002/hbm.23198
Kruschke J (2014) Doing Bayesian Data Analysis: a tutorial with R, JAGS, and Stan, Second Edition. Academic Press
Prabhakaran S, Zarahn E, Riley C, Speizer A, Chong JY, Lazar RM et al (2008) Inter-individual variability in the capacity for motor recovery after ischemic stroke. Neurorehabil Neural Repair 22(1):64–71. https://doi.org/10.1177/1545968307305302
Winters C, van Wegen EE, Daffertshofer A, Kwakkel G (2015) Generalizability of the proportional recovery model for the upper extremity after an ischemic stroke. Neurorehabil Neural Repair 29(7):614–622. https://doi.org/10.1177/1545968314562115
Mori S, Oishi K, Jiang H, Jiang L, Li X, Akhter K et al (2008) Stereotaxic white matter atlas based on diffusion tensor imaging in an ICBM template. Neuroimage 40(2):570–582. https://doi.org/10.1016/j.neuroimage.2007.12.035
Hammers A, Allom R, Koepp MJ, Free SL, Myers R, Lemieux L et al (2003) Three-dimensional maximum probability atlas of the human brain, with particular reference to the temporal lobe. Hum Brain Mapp 19(4):224–247. https://doi.org/10.1002/hbm.10123
James G, Witten D, Hastie T, Tibshirani R (2013) An introduction to statistical learning: with applications in R. Springer
Stinear CM (2017) Prediction of motor recovery after stroke: advances in biomarkers. Lancet Neurol 16(10):826–836. https://doi.org/10.1016/S1474-4422(17)30283-1
Stinear CM, Ward NS (2013) How useful is imaging in predicting outcomes in stroke rehabilitation? Int J Stroke 8(1):33–37. https://doi.org/10.1111/j.1747-4949.2012.00970.x
Puig J, Blasco G, Schlaug G, Stinear CM, Daunis-i-Estadella P, Biarnes C et al (2017) Diffusion tensor imaging as a prognostic biomarker for motor recovery and rehabilitation after stroke. Neuroradiology 59(4):343–351. https://doi.org/10.1007/s00234-017-1816-0
Grefkes C, Ward NS (2014) Cortical reorganization after stroke: how much and how functional? Neuroscientist 20(1):56–70. https://doi.org/10.1177/1073858413491147
Puig J, Pedraza S, Blasco G, Daunis-I-Estadella J, Prados F, Remollo S et al (2011) Acute damage to the posterior limb of the internal capsule on diffusion tensor tractography as an early imaging predictor of motor outcome after stroke. Am J Neuroradiol 32(5):857–863. https://doi.org/10.3174/ajnr.A2400
Schiemanck SK, Kwakkel G, Post MW, Kappelle JL, Prevo AJ (2008) Impact of internal capsule lesions on outcome of motor hand function at one year post-stroke. J Rehabil Med 40(2):96–101. https://doi.org/10.2340/16501977-0130
Dinomais M, Hertz-Pannier L, Groeschel S, Chabrier S, Delion M, Husson B et al (2015) Long term motor function after neonatal stroke: lesion localization above all. Hum Brain Mapp 36(12):4793–4807. https://doi.org/10.1002/hbm.22950
Doughty C, Wang J, Feng W, Hackney D, Pani E, Schlaug G (2016) Detection and predictive value of fractional anisotropy changes of the corticospinal tract in the acute phase of a stroke. Stroke 47(6):1520–1526. https://doi.org/10.1161/STROKEAHA.115.012088
Lin DJ, Cloutier AM, Erler KS, Cassidy JM, Snider SB, Ranford J et al (2019) Corticospinal tract injury estimated from acute stroke imaging predicts upper extremity motor recovery after stroke. Stroke 50(12):3569–3577. https://doi.org/10.1161/STROKEAHA.119.025898
Salvalaggio A, De Filippo De Grazia M, Zorzi M, de Schotten MT, Corbetta M (2020) Post-stroke deficit prediction from lesion and indirect structural and functional disconnection. Brain 143(7):2173–88. https://doi.org/10.1093/brain/awaa156
Park C, Chang WH, Ohn SH, Kim ST, Bang OY, Pascual-Leone A et al (2011) Longitudinal changes of resting-state functional connectivity during motor recovery after stroke. Stroke 42(5):1357–1362. https://doi.org/10.1161/STROKEAHA.110.596155
Hope TMH, Friston K, Price CJ, Leff AP, Rotshtein P, Bowman H (2018) Recovery after stroke: not so proportional after all? Brain 142(1):15–22. https://doi.org/10.1093/brain/awy302
Hawe RL, Scott SH, Dukelow SP (2019) Taking proportional out of stroke recovery. Stroke 50(1):204–211. https://doi.org/10.1161/STROKEAHA.118.023006
Bonkhoff AK, Hope T, Bzdok D, Guggisberg AG, Hawe RL, Dukelow SP et al (2020) Bringing proportional recovery into proportion: Bayesian modelling of post-stroke motor impairment. Brain 143(7):2189–2206. https://doi.org/10.1093/brain/awaa146
Buch ER, Rizk S, Nicolo P, Cohen LG, Schnider A, Guggisberg AG (2016) Predicting motor improvement after stroke with clinical assessment and diffusion tensor imaging. Neurology 86(20):1924–1925. https://doi.org/10.1212/WNL.0000000000002675
Byblow WD, Stinear CM, Barber PA, Petoe MA, Ackerley SJ (2015) Proportional recovery after stroke depends on corticomotor integrity. Ann Neurol 78(6):848–859. https://doi.org/10.1002/ana.24472
Guggisberg AG, Nicolo P, Cohen LG, Schnider A, Buch ER (2017) Longitudinal structural and functional differences between proportional and poor motor recovery after stroke. Neurorehabil Neural Repair 31(12):1029–1041. https://doi.org/10.1177/1545968317740634
Stinear CM, Byblow WD, Ackerley SJ, Smith MC, Borges VM, Barber PA (2017) Proportional motor recovery after stroke: implications for trial design. Stroke 48(3):795–798. https://doi.org/10.1161/STROKEAHA.116.016020
Funding
This work was supported by the National Research Foundation of Korea grants funded by the Korean government (2019R1H1A2039678 and 2020R1I1A1A01061768 to C.P.).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Park, Ch., Ohn, S.H. The predictive value of lesion and disconnectome loads for upper limb motor impairment after stroke. Neurol Sci 43, 3097–3104 (2022). https://doi.org/10.1007/s10072-021-05600-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-021-05600-9