Abstract
Several surgical modalities are available for maxillofacial reconstruction as locoregional or microvascular free flaps.
Purpose
(a) Evaluate the reliability of the supraclavicular flap in cervico-orofacial region; (b) investigate the role of computed tomography angiography (CTA) in predicting the post-operative viability of the flap; (c) assess the speech, feeding, and esthetics after reconstruction using this flap.
Methods
Eleven patients included in this study underwent either conventional or delayed harvesting of the supraclavicular flap (SCF). All the patients had diagnostic computed tomography angiography (CTA) of the supraclavicular flap before the surgery.
Results
The mean harvesting time of the flap was 45.45 ± 4.16 min. The average length of the flap was 22.64 ± 1.12 cm, whereas the mean width of the flap was 6.14 ± 1.14 cm. The flap survived in 9 patients, while two patients had complete flap loss. After the surgery, three patients complained of speech difficulties. Two patients had swallowing problems. After the surgery, three patients complained of speech difficulties. Two patients had swallowing problems. Only two patients complained of weakness in the donor site. None of the patients reported that the weakness or pain at the donor site affected their daily activities or quality of life.
Conclusion
The pedicled SCF represents a safe and feasible option that can be used to reconstruct a wide array of maxillofacial oncologic defects. However, a study with a larger sample size is recommended to achieve more reliable clinical results for the modified delayed technique modification in terms of their effect on the survival of the supraclavicular flap.





Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Jiang C, Huang J, Lin L et al (2022) Digitally reconstructed severe trauma-induced oro-maxillofacial defects with free vascularised composite tissue flaps. Br J Oral Maxillofac Surg 60:773–778. https://doi.org/10.1016/j.bjoms.2021.11.006
Zirk M, Zalesski A, Peters F et al (2018) Prevention and management of bacterial infections of the donor site of flaps raised for reconstruction in head and neck surgery. J Cranio-Maxillofac Surg 46:1669–1673. https://doi.org/10.1016/j.jcms.2018.06.011
Ren Z-H, Wu H-J, Wang K et al (2014) Anterolateral thigh myocutaneous flaps as the preferred flaps for reconstruction of oral and maxillofacial defects. J Cranio-Maxillofac Surg 42:1583–1589. https://doi.org/10.1016/j.jcms.2014.04.012
Andrades P, Militsakh O, Hanasono MM et al (2011) Current strategies in reconstruction of maxillectomy defects. Arch Otolaryngol-Head Neck Surg 137:806–812. https://doi.org/10.1001/archoto.2011.132
Mücke T, Hölzle F, Loeffelbein DJ et al (2011) Maxillary reconstruction using microvascular free flaps. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 111:51–57. https://doi.org/10.1016/j.tripleo.2010.03.042
Yehya AA, Gamaan I, Monem MAE et al (2017) Outcomes of facial artery musculomucosal flap for closure of small and medium sized fistula after clefts. Egypt J Ear Nose Throat Allied Sci 18:231–235. https://doi.org/10.1016/j.ejenta.2017.08.003
Karabulut B (2020) Supraclavicular flap reconstruction in head and neck oncologic surgery. J Craniofac Surg 31:e372–e375. https://doi.org/10.1097/scs.0000000000006315
Alves HRN, de Faria JCM, Busnardo F et al (2017) Forehead reconstruction using supraclavicular flap with microsurgical technique: free flap and a pedicle supercharged flap. JPRAS Open 14:33–38. https://doi.org/10.1016/j.jpra.2017.08.001
Min S-H, Choe SH, Kim WS et al (2022) Effects of ischemic conditioning on head and neck free flap oxygenation: a randomized controlled trial. Sci Rep 12:8130. https://doi.org/10.1038/s41598-022-12374-3
Pratt GF, Rozen WM, Chubb D et al (2012) Preoperative imaging for perforator flaps in reconstructive surgery: a systematic review of the evidence for current techniques. Ann Plast Surg 69:3–9. https://doi.org/10.1097/SPA.0b013e318222b7b7
Tschumi C, Seyed Jafari SM, Rothenberger J et al (2015) Post-operative monitoring of free muscle transfers by Laser Doppler Imaging: a prospective study. Microsurgery 35:528–535. https://doi.org/10.1002/micr.22469
Adams AS, Wright MJ, Johnston S et al (2012) The use of multislice CT angiography preoperative study for supraclavicular artery island flap harvesting. Ann Plast Surg 69
Khoong YM, Huang X, Gu S et al (2021) Imaging for thinned perforator flap harvest: current status and future perspectives. Burns Trauma 9. https://doi.org/10.1093/burnst/tkab042
Li Y, Zhao Z, Wu D et al (2019) Clinical application of supraclavicular flap for head and neck reconstruction. Eur Arch Otorhinolaryngol 276:2319–2324. https://doi.org/10.1007/s00405-019-05483-9
Rosner B (2011) Fundamentals of biostatistics. 7th edn. Boston, Mass
Prasad KN, Cole WC, Haase GM (2004) Radiation protection in humans: extending the concept of as low as reasonably achievable (ALARA) from dose to biological damage. Br J Radiol 77:97–99. https://doi.org/10.1259/bjr/88081058
Thakker JS, Fernandes R (2014) Evaluation of reconstructive techniques for anterior and middle skull base defects following tumor ablation. J Oral Maxillofac Surg 72:198–204. https://doi.org/10.1016/j.joms.2013.05.017
Khareng M, Awang J, Machae R et al (2016) Roles of freedom of religion: in supporting the formation of openness attitude among the southern of Thailand society. Global Journal Al-Thaqafah 6:59–71
Bauer F, Koerdt S, Rommel N et al (2015) Reconstruction of facial defects with local flaps–a training model for medical students? Head Face Med 11:30. https://doi.org/10.1186/s13005-015-0087-4
Mahieu R, Colletti G, Bonomo P et al (2016) Head and neck reconstruction with pedicled flaps in the free flap era. Acta Otorhinolaryngol Ital 36:459–468. https://doi.org/10.14639/0392-100x-1153
Sittitrai P, Ruenmarkkaew D, Klibngern H (2022) Pedicled flaps versus free flaps for oral cavity cancer reconstruction: a comparison of complications, hospital costs, and functional outcomes. Int Arch Otorhinolaryngol 11:e32-e42. https://doi.org/10.1055/s-0042-1751001
Teli Z, Kantharia R, Kantharia S et al (2021) Oral cavity reconstruction with pedicled and free flaps: a single institutional experience. Oncol J India 5:60–66. https://doi.org/10.4103/oji.oji_10_21
Akhundzada I, Kerimov RA, Aliyev AY et al (2016) Supraclavicular flap for reconstruction of the face. AMAJ 2:45–49
Razdan SN, Albornoz CR, Ro T et al (2015) Safety of the supraclavicular artery island flap in the setting of neck dissection and radiation therapy. J Reconstr Microsurg 31:378–383. https://doi.org/10.1055/s-0035-1546294
Loghmani S, Eidy M, Mohammadzadeh M et al (2013) The supraclavicular flap for reconstruction of post-burn mentosternal contractures. Iran Red Crescent Med J 15:292–297. https://doi.org/10.5812/ircmj.1600
Rashid M, Zia-Ul-Islam M, Sarwar SU et al (2006) The ‘expansile’ supraclavicular artery flap for release of post-burn neck contractures. J Plast Reconstr Aesthet Surg 59:1094–1101. https://doi.org/10.1016/j.bjps.2005.12.058
Fang S-L, Zhang D-M, Chen W-L et al (2016) Reconstruction of full-thickness cheek defects with a folded extended supraclavicular fasciocutaneous island flap following ablation of advanced oral cancer. J Cancer Res Ther 12:888–891. https://doi.org/10.4103/0973-1482.177497
You Y-h, Chen W-l, Zhang D-m (2013) Closure of large oropharyngocutaneous fistulas using a folded extensive supraclavicular fasciocutaneous island flap. J Oral Maxillofac Surg Med Pathol 25:310–313. https://doi.org/10.1016/j.ajoms.2012.09.012
Valentini V, Cassoni A, Marianetti TM et al (2008) Diabetes as main risk factor in head and neck reconstructive surgery with free flaps. J Craniofac Surg 19:1080–1084. https://doi.org/10.1097/SCS.0b013e3181763531
Zhang W, Li X, Li X (2021) A systematic review and meta-analysis of perforator flaps in plantar defects: risk analysis of complications. Int Wound J 18:525–535. https://doi.org/10.1111/iwj.13552
Mills E, Eyawo O, Lockhart I et al (2011) Smoking cessation reduces postoperative complications: a systematic review and meta-analysis. Am J Med 124:144-154.e8. https://doi.org/10.1016/j.amjmed.2010.09.013
Garip M, Van Dessel J, Grosjean L et al (2021) The impact of smoking on surgical complications after head and neck reconstructive surgery with a free vascularised tissue flap: a systematic review and meta-analysis. Br J Oral Maxillofac Surg 59:e79–e98. https://doi.org/10.1016/j.bjoms.2020.07.020
Kokot N, Mazhar K, Reder LS et al (2013) The supraclavicular artery island flap in head and neck reconstruction: applications and limitations. JAMA Otolaryngol-Head Neck Surg 139:1247–1255. https://doi.org/10.1001/jamaoto.2013.5057
Hwang K, Son JS, Ryu WK (2018) Smoking and flap survival. Plast Surg 26:280–285. https://doi.org/10.1177/2292550317749509. (Oakv)
Colletti G, Autelitano L, Tewfik K et al (2012) Autonomized flaps in secondary head and neck reconstructions. Acta Otorhinolaryngol Ital 32:329–335
Wang H, Li Z, Liu X (2008) Effects of various protocols of ischemic preconditioning on rat tram flaps. Microsurgery 28:37–43. https://doi.org/10.1002/micr.20436
Murry CE, Jennings RB, Reimer KA (1986) Preconditioning with ischemia: a delay of lethal cell injury in ischemic myocardium. Circulation 74:1124–1136. https://doi.org/10.1161/01.cir.74.5.1124
Shenoy A, Patil VS, Prithvi BS et al (2013) Supraclavicular artery flap for head and neck oncologic reconstruction: an emerging alternative. Int J Surg Oncol 2013:658989. https://doi.org/10.1155/2013/658989
Chiu ES, Liu PH, Friedlander PL (2009) Supraclavicular artery island flap for head and neck oncologic reconstruction: indications, complications, and outcomes. Plast Reconstr Surg 124:115–123. https://doi.org/10.1097/PRS.0b013e3181aa0e5d
Alves HR, Ishida LC, Ishida LH et al (2012) A clinical experience of the supraclavicular flap used to reconstruct head and neck defects in late-stage cancer patients. J Plast Reconstr Aesthet Surg 65:1350–1356. https://doi.org/10.1016/j.bjps.2012.04.050
Boschetti CE, Pollice A, Fragola R et al (2022) The revival of the supraclavicular artery island flap (SCAIF) during the COVID-19 pandemic. Adv Oral Maxillofac Surg 100358. https://doi.org/10.1016/j.adoms.2022.100358
Vinh VQ, Van Anh T, Ogawa R et al (2009) Anatomical and clinical studies of the supraclavicular flap: analysis of 103 flaps used to reconstruct neck scar contractures. Plast Reconstr Surg 123:1471–1480. https://doi.org/10.1097/PRS.0b013e3181a205ba
Kokot N, Mazhar K, Reder LS et al (2014) Use of the supraclavicular artery island flap for reconstruction of cervicofacial defects. Otolaryngol Head Neck Surg 150:222–228. https://doi.org/10.1177/0194599813514205
Ismail H, Elshobaky A (2016) Supraclavicular artery perforator flap in management of post-burn neck reconstruction: clinical experience. Ann Burns Fire Disasters 29:209–214
Balakrishnan TM, Sivarajan N (2012) Anatomical study of supraclavicular perforator artery and its clinical application as sensate supraclavicular artery propeller flap in the reconstruction of post burns scar contracture neck. Indian J Sci Technol 5:3137–3141
More A, Sivakumar A, Gaurav GK (2020) Supraclavicular flap for large anterior chest wall defects-a road less travelled. Indian J Plast Surg 53:427–430. https://doi.org/10.1055/s-0040-1716457
Hunt JP, Buchmann LO (2014) The supraclavicular artery flap for lateral skull and scalp defects: effective and efficient alternative to free tissue transfer. J Neurol Surg Rep 75:e5–e10. https://doi.org/10.1055/s-0033-1358376
Gupta SK, Rana AS, Gupta D et al (2010) Unusual causes of reduced mouth opening and it’s suitable surgical management: our experience. Natl J Maxillofac Surg 1:86–90. https://doi.org/10.4103/0975-5950.69150
Louise Kent M, Brennan MT, Noll JL et al (2008) Radiation-induced trismus in head and neck cancer patients. Support Care Cancer 16:305–309. https://doi.org/10.1007/s00520-007-0345-5
Weber C, Dommerich S, Pau HW et al (2010) Limited mouth opening after primary therapy of head and neck cancer. Oral Maxillofac Surg 14:169–173. https://doi.org/10.1007/s10006-010-0220-2
Scott B, Butterworth C, Lowe D et al (2008) Factors associated with restricted mouth opening and its relationship to health-related quality of life in patients attending a Maxillofacial Oncology clinic. Oral Oncol 44:430–438. https://doi.org/10.1016/j.oraloncology.2007.06.015
Abboud WA, Hassin-Baer S, Alon EE et al (2020) Restricted mouth opening in head and neck cancer: etiology, prevention, and treatment. JCO Oncol Pract 16:643–653. https://doi.org/10.1200/op.20.00266
Granzow JW, Suliman A, Roostaeian J et al (2013) Supraclavicular artery island flap (SCAIF) vs free fasciocutaneous flaps for head and neck reconstruction. Otolaryngol-Head Neck Surg 148:941–948. https://doi.org/10.1177/0194599813476670
Atallah S, Guth A, Chabolle F et al (2015) Supraclavicular artery island flap in head and neck reconstruction. Eur Ann Otorhinolaryngol Head Neck Dis 132:291–294. https://doi.org/10.1016/j.anorl.2015.08.021
Sandu K, Monnier P, Pasche P (2012) Supraclavicular flap in head and neck reconstruction: experience in 50 consecutive patients. Eur Arch Otorhinolaryngol 269:1261–1267. https://doi.org/10.1007/s00405-011-1754-0
Herr MW, Bonanno A, Montalbano LA et al (2014) Shoulder function following reconstruction with the supraclavicular artery island flap. Laryngoscope 124:2478–2483. https://doi.org/10.1002/lary.24761
Spiegel JL, Pilavakis Y, Canis M et al (2018) Shoulder morbidity in patients after head and neck reconstruction with the pedicled supraclavicular island flap. Plast Reconstr Surg – Global Open 6:e1711. https://doi.org/10.1097/gox.0000000000001711
Spiegel JL, Pilavakis Y, Canis M et al (2018) Shoulder morbidity in patients after head and neck reconstruction with the pedicled supraclavicular island flap. Plast Reconstr Surg Glob Open 6:e1711. https://doi.org/10.1097/gox.0000000000001711
Welz C, Canis M, Schwenk-Zieger S et al (2017) Oral cancer reconstruction using the supraclavicular artery island flap: comparison to free radial forearm flap. J Oral Maxillofac Surg 75:2261–2269. https://doi.org/10.1016/j.joms.2017.02.017
Wong S, Brennan M, Nishikawa S et al (2019) Supraclavicular artery island flap in head and neck reconstruction: a case series and literature review. Perm J 23. https://doi.org/10.7812/tpp/19.006
Marshall CD, Hu MS, Leavitt T et al (2018) Cutaneous scarring: basic science, current treatments, and future directions. Adv Wound Care 7:29–45. https://doi.org/10.1089/wound.2016.0696. (New Rochelle)
Edriss AS, Mesták J (2005) Management of keloid and hypertrophic scars. Ann Burns Fire Disasters 18:202–210
Gauglitz GG, Korting HC, Pavicic T et al (2011) Hypertrophic scarring and keloids: pathomechanisms and current and emerging treatment strategies. Mol Med 17:113–125. https://doi.org/10.2119/molmed.2009.00153
Otene CI, Olaitan PB, Ogbonnaya IS et al (2011) Donor site morbidity following harvest of split-thickness skin grafts in South Eastern Nigeria. J West Afr Coll Surg 1:86–96
Dusseldorp JR, Pennington DG (2014) Quantifying blood flow in the DIEP flap: an ultrasonographic study. Plast Reconstr Surg Glob Open 2:e228. https://doi.org/10.1097/gox.0000000000000191
Collet C, Onuma Y, Andreini D et al (2018) Coronary computed tomography angiography for heart team decision-making in multivessel coronary artery disease. Eur Heart J 39:3689–3698. https://doi.org/10.1093/eurheartj/ehy581
Suzuki Y, Shimizu Y, Kasai S et al (2019) Indocyanine green fluorescence videoangiography for reliable variations of supraclavicular artery flaps. Arch Plast Surg 46:318–323. https://doi.org/10.5999/aps.2018.01536
Tayfur V, Magden O, Edizer M et al (2010) Supraclavicular artery flap. J Craniofac Surg 21:1938–1940. https://doi.org/10.1097/SCS.0b013e3181f4ee38
Pallua N, Demir E (2008) Postburn head and neck reconstruction in children with the fasciocutaneous supraclavicular artery island flap. Ann Plast Surg 60:276–282. https://doi.org/10.1097/SAP.0b013e3180db2775
Weiglein AH, Moriggl B, Schalk C et al (2005) Arteries in the posterior cervical triangle in man. Clin Anat 18:553–557. https://doi.org/10.1002/ca.20143
Vinh VQ, Ogawa R, Van Anh T et al (2007) Reconstruction of neck scar contractures using supraclavicular flaps: retrospective study of 30 cases. Plast Reconstr Surg 119:130–135. https://doi.org/10.1097/01.prs.0000244843.49596.e5
Ross RJ, Baillieu CE, Shayan R et al (2014) The anatomical basis for improving the reliability of the supraclavicular flap. J Plast Reconstr Aesthet Surg 67:198–204. https://doi.org/10.1016/j.bjps.2013.10.006
Wilson MK, Collyar D, Chingos DT et al (2015) Outcomes and endpoints in cancer trials: bridging the divide. Lancet Oncol 16:e43-52. https://doi.org/10.1016/s1470-2045(14)70380-8
Paydarfar JA, Patel UA (2011) Submental island pedicled flap vs radial forearm free flap for oral reconstruction: comparison of outcomes. Arch Otolaryngol Head Neck Surg 137:82–87. https://doi.org/10.1001/archoto.2010.204
Zhang S, Chen W, Cao G et al (2015) Pedicled supraclavicular artery island flap versus free radial forearm flap for tongue reconstruction following hemiglossectomy. J Craniofac Surg 26:e527–e530. https://doi.org/10.1097/scs.0000000000002031
Author information
Authors and Affiliations
Contributions
A.Z. and M.K. wrote the main manuscript text and A.Z. prepared figures 1-5. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of the University Faculty of Dentistry, Alexandria University (IRB No. 001056–IORG 0008839-0280-09/2021).
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
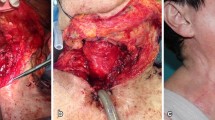
The authors affirm that human research participants provided informed consent for publication of the images in Figures 1p and 3a.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zaitoun, A., Fata, M., Shafei, M.E. et al. Application of supraclavicular island flap in oral and maxillofacial reconstruction. Oral Maxillofac Surg 28, 893–908 (2024). https://doi.org/10.1007/s10006-024-01225-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10006-024-01225-2