Abstract
Objectives
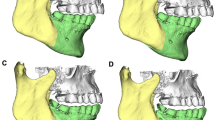
This study aimed to find out the correlation between different anatomical parameters of the mandible and the occurrence of a bad split in patients who had undergone bilateral split sagittal ramus osteotomy (BSSRO).
Materials and method
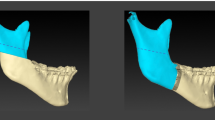
At both the distal roots of the first molar (1) and the retromolar area (2), we measured the distance from the buccal margin of the inferior dental canal (IDC) to the buccal margin of the cortical bone (MCBC), the thickness of both buccal cortical (WBCB) and cancellous bone (WBCA), distance from the superior border of IDC to the alveolar crest (MCAC), buccolingual thickness (BLT), and thickness of cancellous bone (WCA). At the ramus, the distances between the sigmoid notch to the upper part of the lingula (SL) and the inferior border of the mandible (SIBM), the thickness of the ramus at the level of the lingula (BLTR), and the anteroposterior width of the ramus (APWR) were measured. The paired and independent t-tests were used when applicable, and a P-value < 0.05 was considered significant.
Results
MCBC1 showed a significant difference between bad and non-bad split sides (P = 0.037). Both WBCA1 and WBCA2 show the same significant difference (P = 0.023, 0.024). Similarly, WCA1 and WCA2 showed a statistical difference between the bad and non-bad split sides (P = 0.027, 0.036). There were no statistically significant differences between the compared sides of WBCB1, WBCB2, MCAC1, MCAC2, SIBM, APWR, SL, and BLTR.
Conclusion
Narrow space between IDC and the buccal cortical margin, along with the decrease in the thickness of both buccal cancellous bone and total cancellous bone at the inferior border of the mandible along the course of SSRO, has been implicated in the occurrence of bad split intraoperatively.




Similar content being viewed by others
References
Hou M, Yu T-P, Wang J-G (2015) Evaluation of the mandibular split patterns in sagittal split ramus osteotomy. J Oral Maxillofac Surg 73:985–993
Schuchardt G (1942) Ein Beitrag zur chirurgischen Kieferorthpadie unter Berucksichtigung ihrer fur di Behandlung angeborener und erworbener Kiefer deformitaten bei soldaten. Dtsch Zahn Mund Kieferheilkd 9:73–89
Wang T, Han JJ, Oh H-K, Park H-J, Jung S, Park Y-J, Kook M-S (2016) Evaluation of mandibular anatomy associated with bad splits in sagittal split ramus osteotomy of mandible. J Craniofac Surg 27:e500–e504
Aarabi M, Tabrizi R, Hekmat M, Shahidi S, Puzesh A (2014) Relationship between mandibular anatomy and the occurrence of a bad split upon sagittal split osteotomy. J Oral Maxillofac Surg 72:2508–2513
Muto T, Shigeo K, Yamamoto K, Kawakami J (2003) Computed tomography morphology of the mandibular ramus in prognathism: effect on the medial osteotomy of the sagittal split ramus osteotomy. J Oral Maxillofac Surg 61:89–93
Verweij JP, Mensink G, Houppermans PN, van Merkesteyn JR (2015) Angled osteotomy design aimed to influence the lingual fracture line in bilateral sagittal split osteotomy: a human cadaveric study. J Oral Maxillofac Surg 73:1983–1993
Smith BR, Rajchel JL, Waite DE, Read L (1991) Mandibular ramus anatomy as it relates to the medial osteotomy of the sagittal split ramus osteotomy. J Oral Maxillofac Surg 49:112–116
Trauner R, Obwegeser H (1957) The surgical correction of mandibular prognathism and retrognathia with consideration of genioplasty: Part I. Surgical procedures to correct mandibular prognathism and resha** of the chin. Oral Surg Oral Med Oral Pathol 10:677–689
Veras R, Kriwalsky M, Hoffmann S, Maurer P, Schubert J (2008) Functional and radiographic long-term results after bad split in orthognathic surgery. Int J Oral Maxillofac Surg 37:606–611
Guernsey LH, DeChamplain RW (1971) Sequelae and complications of the intraoral sagittal osteotomy in the mandibular rami. Oral Surg Oral Med Oral Pathol 32:176–192
Teltzrow T, Kramer F-J, Schulze A, Baethge C, Brachvogel P (2005) Perioperative complications following sagittal split osteotomy of the mandible. J Craniomaxillofac Surg 33:307–313
Macintosh RB (1981) Experience with the sagittal osteotomy of the mandibular ramus: a 13-year review. J Maxillofac Surg 9:151–165
Panula K, Finne K, Oikarinen K (2001) Incidence of complications and problems related to orthognathic surgery: a review of 655 patients. J Oral Maxillofac Surg 59:1128–1136
Steenen S, Becking A (2016) Bad splits in bilateral sagittal split osteotomy: systematic review of fracture patterns. Int J Oral Maxillofac Surg 45:887–897
Kriwalsky MS, Maurer P, Veras RB, Eckert AW, Schubert J (2008) Risk factors for a bad split during sagittal split osteotomy. Br J Oral Maxillofac Surg 46:177–179
Turvey TA (1985) Intraoperative complications of sagittal osteotomy of the mandibular ramus: incidence and management. J Oral Maxillofac Surg Offic J Am Assoc Oral Maxillofac Surg 43:504–509
Falter B, Schepers S, Vrielinck L, Lambrichts I, Thijs H, Politis C (2010) Occurrence of bad splits during sagittal split osteotomy. Oral Surg Oral Med Oral Path Oral Radio Endodont 110:430–435
Al-Nawas B, Kämmerer PW, Hoffmann C, Moergel M, Koch FP, Wriedt S, Walter C (2014) Influence of osteotomy procedure and surgical experience on early complications after orthognathic surgery in the mandible. J CranioMaxillofac Surg 42:e284–e288
Mensink G, Verweij JP, Frank MD, Bergsma JE, Van Merkesteyn JR (2013) Bad split during bilateral sagittal split osteotomy of the mandible with separators: a retrospective study of 427 patients. Br J Oral Maxillofac Surg 51:525–529
Yang X-W, Long X, Yeweng S-J, Kao C-T (2007) Evaluation of mandibular setback after bilateral sagittal split osteotomy with the Hunsuck modification and miniplate fixation. J Oral Maxillofac Surg 65:2176–2180
Benjamini Y, Hochberg Y (1995) Controlling the false discovery rate: a practical and powerful approach to multiple testing. J Roy Stat Soc: Ser B (Methodol) 57:289–300. https://doi.org/10.1111/j.2517-6161.1995.tb02031.x
Friscia M, Sbordone C, Petrocelli M, Vaira LA, Attanasi F, Cassandro FM, Paternoster M, Iaconetta G, Califano L (2017) Complications after orthognathic surgery: our experience on 423 cases. Oral Maxillofac Surg 21:171–177
Mehra P, Castro V, Freitas RZ and Wolford LM (2001) Complications of the mandibular sagittal split ramus osteotomy associated with the presence or absence of third molars. J Oral Maxillofac Surg 59:854-8; discussion 859. https://doi.org/10.1053/joms.2001.2501
Kriwalsky MS, Maurer P, Veras RB, Eckert AW, Schubert J (2008) Risk factors for a bad split during sagittal split osteotomy. Br J Oral Maxillofac Surg 46:177–179. https://doi.org/10.1016/j.bjoms.2007.09.011
Jiang N, Wang M, Bi R, Wu G, Zhu S, Liu Y (2021) Risk factors for bad splits during sagittal split ramus osteotomy: a retrospective study of 964 cases. Br J Oral Maxillofac Surg 59:678–682
Yu I, Wong Y (2008) Evaluation of mandibular anatomy related to sagittal split ramus osteotomy using 3-dimensional computed tomography scan images. Int J Oral Maxillofac Surg 37:521–528
Jääskeläinen SK, Teerijoki-Oksa T, Forssell K, Vähätalo K, Peltola JK, Forssell H (2000) Intraoperative monitoring of the inferior alveolar nerve during mandibular sagittal-split osteotomy. Muscle Nerve 23:368–375. https://doi.org/10.1002/(sici)1097-4598(200003)23:3%3c368::aid-mus8%3e3.0.co;2-0
Westermark A, Bystedt H, von Konow L (1998) Inferior alveolar nerve function after sagittal split osteotomy of the mandible: correlation with degree of intraoperative nerve encounter and other variables in 496 operations. Br J Oral Maxillofac Surg 36:429–433. https://doi.org/10.1016/s0266-4356(98)90458-2
Yates C, Olson D, Guralnick W (1976) The antilingula as an anatomic landmark in oral surgery. Oral Surg Oral Med Oral Pathol 41:705–708. https://doi.org/10.1016/0030-4220(76)90182-1
Cunha G, Oliveira MR, Salmen FS, Gabrielli MFR, Gabrielli MAC (2020) How does bone thickness affect the split pattern of sagittal ramus osteotomy? Int J Oral Maxillofac Surg 49:218–223. https://doi.org/10.1016/j.ijom.2019.05.011
Akcay H, Kalabalık F, Tatar B, Ulu M (2019) Location of the mandibular lingula: comparison of skeletal Class I and Class III patients in relation to ramus osteotomy using cone-beam computed tomography. J Stomatol Oral Maxillofac Surg 120:504–508. https://doi.org/10.1016/j.jormas.2019.07.013
Kalabalik F, Akçay H, Tatar B (2020) Morphometric analysis of mandibular corpus relevance to sagittal split osteotomy: comparison of dentoskeletal Class I and Class III patients. J Stomatol Oral Maxillofac Surg 121:615–620. https://doi.org/10.1016/j.jormas.2020.03.016
Beukes J, Reyneke JP, Becker PJ (2013) Variations in the anatomical dimensions of the mandibular ramus and the presence of third molars: its effect on the sagittal split ramus osteotomy. Int J Oral Maxillofac Surg 42:303–307. https://doi.org/10.1016/j.ijom.2012.09.020
Funding
This study was supported by grants from the National Natural Science Foundation of China (81901026) and the Department of Science and Technology of Sichuan Province (2021YFH0139).
Author information
Authors and Affiliations
Contributions
Wael Telha: Conceptualization, data collection, data curation, anthropometric measurements, statistical analysis, writing—original draft preparation, review, and editing.
Bassam Abotaleb: Conceptualization, statistical analysis, review, and editing.
Jie Zhang: Data curation, methodology, reviewing.
Rui Bi: Conceptualization, statistical analysis, review, and editing.
Songsong Zhu: Conceptualization, reviewing and editing, project administration, supervision.
Nan Jiang: Conceptualization, project administration, reviewing and editing, supervision.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
This research was approved by the institutional review board of West China Stomatology Hospital Sichuan University (WCHS-IRB-CT-2019–221). Patients’ permission was obtained.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Telha, W., Abotaleb, B., Zhang, J. et al. Correlation between mandibular anatomy and bad split occurrence during bilateral sagittal split osteotomy: a three-dimensional study. Clin Oral Invest 27, 1035–1042 (2023). https://doi.org/10.1007/s00784-022-04665-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-022-04665-w