Abstract
Background
Presently, a consistent strategy for determining the stability of unruptured intracranial aneurysms (UIAs) in elderly patients is lacking, primarily due to the unique characteristics of this demographic. Our objective was to assess the risk factors contributing to aneurysm instability (growth or rupture) within the elderly population.
Methods
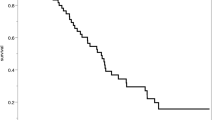
In this study, we compiled data from follow-up patients with UIAs spanning from November 2016 to August 2021. We specifically focused on patients aged ≥ 60 years. Clinical histories were gathered, and morphological parameters of aneurysms were measured. The growth of aneurysms was determined using the computer-assisted semi-automated measurement (CASAM). Growth and rupture rates of UIAs were calculated, and both univariate and multivariate Cox regression analyses were conducted. Additionally, Kaplan–Meier survival curves were plotted.
Results
A total of 184 patients with 210 aneurysms were enrolled in the study. The follow-up period encompasses 506.6 aneurysm-years and 401.4 patient-years. Among all the aneurysms, 23 aneurysms exhibited growth, with an annual aneurysm growth rate of 11.0%, and 1 (4.5%) experienced rupture, resulting in an annual aneurysm rupture rate of 0.21%. Multivariate Cox analysis identified poorly controlled hypertension (P = 0.011) and high-risk aneurysms (including anterior cerebral artery (ACA), anterior communicating artery (AcoA), posterior communicating artery aneurysm (PcoA), posterior circulation (PC) > 4 mm or distal internal carotid artery (ICAd), middle cerebral artery (MCA), and PC > 7 mm) (P = 0.006) as independent risk factors for the development of unstable aneurysms.
Conclusions
In the elderly, poorly controlled hypertension and high-risk aneurysms emerge as significant risk factors for aneurysm instability. This underscores the importance of rigorous surveillance or timely intervention in patients presenting with these risk factors.



Similar content being viewed by others
Data availability
Data can be obtained by contacting the corresponding author via email under reasonable requirements.
Code availability
Not applicable.
Abbreviations
- UIA:
-
Unruptured intracranial aneurysm
- CASAM:
-
Computer-assisted semi-automated measurement
- SAH:
-
Subarachnoid hemorrhage
- TOF-MRA:
-
Time of flight magnetic resonance angiogram
- PCoA:
-
Posterior communicating artery
- ACoA:
-
Anterior communicating artery
- MCA:
-
Middle cerebral artery
- CCA:
-
Cavernous carotid artery
- ACA:
-
Anterior cerebral artery
- ICAp:
-
Proximal internal carotid artery
- ICAd:
-
Distal internal carotid artery
- PC:
-
Posterior circulation
- D:
-
Diameter
- W:
-
Width
- H:
-
Height
- V:
-
Volume
- AA:
-
Aneurysm angle
- N:
-
Neck width
- V:
-
Volume
- FA:
-
Flow angle
- NS:
-
Neck surface
- UI:
-
Undulation index
- NSI:
-
Nonsphericity index
- AR:
-
Aspect ratio
- SR:
-
Size ratio
References
Backes D, Vergouwen MD, Tiel Groenestege AT, Bor AS, Velthuis BK, Greving JP, Algra A, Wermer MJ, van Walderveen MA, terBrugge KG, Agid R, Rinkel GJ (2015) PHASES score for prediction of intracranial aneurysm growth. Stroke 46:1221–1226. https://doi.org/10.1161/strokeaha.114.008198
Baharoglu MI, Lauric A, Gao BL, Malek AM (2012) Identification of a dichotomy in morphological predictors of rupture status between sidewall- and bifurcation-type intracranial aneurysms. J Neurosurg 116:871–881. https://doi.org/10.3171/2011.11.Jns11311
Baharoglu MI, Schirmer CM, Hoit DA, Gao BL, Malek AM (2010) Aneurysm inflow-angle as a discriminant for rupture in sidewall cerebral aneurysms: morphometric and computational fluid dynamic analysis. Stroke 41:1423–1430. https://doi.org/10.1161/strokeaha.109.570770
Bor AS, Tiel Groenestege AT, terBrugge KG, Agid R, Velthuis BK, Rinkel GJ, Wermer MJ (2015) Clinical, radiological, and flow-related risk factors for growth of untreated, unruptured intracranial aneurysms. Stroke 46:42–48. https://doi.org/10.1161/strokeaha.114.005963
Brisman JL, Song JK, Newell DW (2006) Cerebral aneurysms. N Engl J Med 355:928–939. https://doi.org/10.1056/NEJMra052760
Caffes N, Wenger N, Cannarsa G, Oliver J, Onwukwe C, Gandhi D, Simard JM (2021) Unruptured cerebral aneurysms in elderly patients: key challenges and management. Ann Med 53:1839–1849. https://doi.org/10.1080/07853890.2021.1990393
Chen Y, **ng H, Lin B, Zhou J, Ding S, Wan J, Yang Y, Pan Y, Zhao B (2020) Morphological risk model assessing anterior communicating artery aneurysm rupture: development and validation. Clin Neurol Neurosurg 197:106158. https://doi.org/10.1016/j.clineuro.2020.106158
Darsaut TE, Findlay JM, Magro E, Kotowski M, Roy D, Weill A, Bojanowski MW, Chaalala C, Iancu D, Lesiuk H, Sinclair J, Scholtes F, Martin D, Chow MM, O’Kelly CJ, Wong JH, Butcher K, Fox AJ, Arthur AS, Guilbert F, Tian L, Chagnon M, Nolet S, Gevry G, Raymond J (2017) Surgical clip** or endovascular coiling for unruptured intracranial aneurysms: a pragmatic randomised trial. J Neurol Neurosurg Psychiatry 88:663–668. https://doi.org/10.1136/jnnp-2016-315433
Dhar S, Tremmel M, Mocco J, Kim M, Yamamoto J, Siddiqui AH, Hopkins LN, Meng H (2008) Morphology parameters for intracranial aneurysm rupture risk assessment. Neurosurgery 63:185–96; discussion 196–7. https://doi.org/10.1227/01.Neu.0000316847.64140.81
Etminan N, Brown RD Jr, Beseoglu K, Juvela S, Raymond J, Morita A, Torner JC, Derdeyn CP, Raabe A, Mocco J, Korja M, Abdulazim A, Amin-Hanjani S, Al-Shahi Salman R, Barrow DL, Bederson J, Bonafe A, Dumont AS, Fiorella DJ, Gruber A, Hankey GJ, Hasan DM, Hoh BL, Jabbour P, Kasuya H, Kelly ME, Kirkpatrick PJ, Knuckey N, Koivisto T, Krings T, Lawton MT, Marotta TR, Mayer SA, Mee E, Pereira VM, Molyneux A, Morgan MK, Mori K, Murayama Y, Nagahiro S, Nakayama N, Niemelä M, Ogilvy CS, Pierot L, Rabinstein AA, Roos YB, Rinne J, Rosenwasser RH, Ronkainen A, Schaller K, Seifert V, Solomon RA, Spears J, Steiger HJ, Vergouwen MD, Wanke I, Wermer MJ, Wong GK, Wong JH, Zipfel GJ, Connolly ES Jr, Steinmetz H, Lanzino G, Pasqualin A, Rüfenacht D, Vajkoczy P, McDougall C, Hänggi D, LeRoux P, Rinkel GJ, Macdonald RL (2015) The unruptured intracranial aneurysm treatment score: a multidisciplinary consensus. Neurology 85:881–889. https://doi.org/10.1212/wnl.0000000000001891
Etminan N, de Sousa DA, Tiseo C, Bourcier R Desal H, Lindgren A, Koivisto T, Netuka D, Peschillo S, Lémeret S, Lal A, Vergouwen MD, Rinkel GJ (2022) European Stroke Organisation (ESO) guidelines on management of unruptured intracranial aneurysms. Eur Stroke J 7:V. https://doi.org/10.1177/23969873221099736
Geng J, Hu P, Ji Z, Li C, Li L, Shen J, Feng X, Wang W, Yang G, Li J, Zhang H (2020) Accuracy and reliability of computer-assisted semi-automated morphological analysis of intracranial aneurysms: an experimental study with digital phantoms and clinical aneurysm cases. Int J Comput Assist Radiol Surg 15:1749–1759. https://doi.org/10.1007/s11548-020-02218-8
van Gijn J, Kerr RS, Rinkel GJ (2007) Subarachnoid haemorrhage. Lancet 369:306–318. https://doi.org/10.1016/s0140-6736(07)60153-6
Greving JP, Wermer MJ, Brown RD Jr, Morita A, Juvela S, Yonekura M, Ishibashi T, Torner JC, Nakayama T, Rinkel GJ, Algra A (2014) Development of the PHASES score for prediction of risk of rupture of intracranial aneurysms: a pooled analysis of six prospective cohort studies. Lancet Neurol 13:59–66. https://doi.org/10.1016/s1474-4422(13)70263-1
Ikawa F, Michihata N, Akiyama Y, Iihara K, Matano F, Morita A, Kato Y, Iida K, Kurisu K, Fushimi K, Yasunaga H (2019) Treatment risk for elderly patients with unruptured cerebral aneurysm from a nationwide database in Japan. World Neurosurg 132:e89–e98. https://doi.org/10.1016/j.wneu.2019.08.252
Inagawa T, Hirano A (1990) Autopsy study of unruptured incidental intracranial aneurysms. Surg Neurol 34:361–365. https://doi.org/10.1016/0090-3019(90)90237-j
Ingall T, Asplund K, Mähönen M, Bonita R (2000) A multinational comparison of subarachnoid hemorrhage epidemiology in the WHO MONICA stroke study. Stroke 31:1054–1061. https://doi.org/10.1161/01.str.31.5.1054
International Study of Unruptured Intracranial Aneurysms Investigators (1998) Unruptured intracranial aneurysms–risk of rupture and risks of surgical intervention. N Engl J Med 339:1725–1733. https://doi.org/10.1056/nejm199812103392401
Iwamoto H, Kiyohara Y, Fujishima M, Kato I, Nakayama K, Sueishi K, Tsuneyoshi M (1999) Prevalence of intracranial saccular aneurysms in a Japanese community based on a consecutive autopsy series during a 30-year observation period. The Hisayama Study Stroke 30:1390–1395. https://doi.org/10.1161/01.str.30.7.1390
Juvela S, Korja M (2017) Intracranial aneurysm parameters for predicting a future subarachnoid hemorrhage: a long-term follow-up study. Neurosurgery 81:432–440. https://doi.org/10.1093/neuros/nyw049
Koffijberg H, Buskens E, Granath F, Adami J, Ekbom A, Rinkel GJ, Blomqvist P (2008) Subarachnoid haemorrhage in Sweden 1987–2002: regional incidence and case fatality rates. J Neurol Neurosurg Psychiatry 79:294–299. https://doi.org/10.1136/jnnp.2007.123901
Lauric A, Miller EL, Baharoglu MI, Malek AM (2011) 3D shape analysis of intracranial aneurysms using the writhe number as a discriminant for rupture. Ann Biomed Eng 39:1457–1469. https://doi.org/10.1007/s10439-010-0241-x
Li MH, Chen SW, Li YD, Chen YC, Cheng YS, Hu DJ, Tan HQ, Wu Q, Wang W, Sun ZK, Wei XE, Zhang JY, Qiao RH, Zong WH, Zhang Y, Lou W, Chen ZY, Zhu Y, Peng DR, Ding SX, Xu XF, Hou XH, Jia WP (2013) Prevalence of unruptured cerebral aneurysms in Chinese adults aged 35 to 75 years: a cross-sectional study. Ann Intern Med 159:514–521. https://doi.org/10.7326/0003-4819-159-8-201310150-00004
Li M, Hu S, Yu N, Zhang Y, Luo M (2019) Association between meteorological factors and the rupture of intracranial aneurysms. J Am Heart Assoc 8:e012205. https://doi.org/10.1161/jaha.119.012205
Morita A, Kirino T, Hashi K, Aoki N, Fukuhara S, Hashimoto N, Nakayama T, Sakai M, Teramoto A, Tominari S, Yoshimoto T (2012) The natural course of unruptured cerebral aneurysms in a Japanese cohort. N Engl J Med 366:2474–2482. https://doi.org/10.1056/NEJMoa1113260
Morris Z, Whiteley WN, Longstreth WT Jr, Weber F, Lee YC, Tsushima Y, Alphs H, Ladd SC, Warlow C, Wardlaw JM, Al-Shahi Salman R (2009) Incidental findings on brain magnetic resonance imaging: systematic review and meta-analysis. BMJ 339:b3016. https://doi.org/10.1136/bmj.b3016
Rajabzadeh-Oghaz H, Varble N, Shallwani H, Tutino VM, Mowla A, Shakir HJ, Vakharia K, Atwal GS, Siddiqui AH, Davies JM, Meng H (2018) Computer-assisted three-dimensional morphology evaluation of intracranial aneurysms. World Neurosurg 119:e541–e550. https://doi.org/10.1016/j.wneu.2018.07.208
Sonobe M, Yamazaki T, Yonekura M, Kikuchi H (2010) Small unruptured intracranial aneurysm verification study: SUAVe study, Japan. Stroke 41:1969–1977. https://doi.org/10.1161/strokeaha.110.585059
Turhon M, Li M, Kang H, Huang J, Zhang F, Zhang Y, Zhang Y, Maimaiti A, Gheyret D, Axier A, Aisha M, Yang X, Liu J (2023) Development and validation of a deep learning model for prediction of intracranial aneurysm rupture risk based on multi-omics factor. Eur Radiol 33:6759–6770. https://doi.org/10.1007/s00330-023-09672-3
Ujiie H, Tamano Y, Sasaki K, Hori T (2001) Is the aspect ratio a reliable index for predicting the rupture of a saccular aneurysm? Neurosurgery 48:495–502; discussion 502–3. https://doi.org/10.1097/00006123-200103000-00007
Vlak MH, Algra A, Brandenburg R, Rinkel GJ (2011) Prevalence of unruptured intracranial aneurysms, with emphasis on sex, age, comorbidity, country, and time period: a systematic review and meta-analysis. Lancet Neurol 10:626–636. https://doi.org/10.1016/s1474-4422(11)70109-0
Wiebers DO (2005) Patients with small, asymptomatic, unruptured intracranial aneurysms and no history of subarachnoid hemorrhage should generally be treated conservatively: for. Stroke 36:408–409. https://doi.org/10.1161/01.Str.0000152270.22970.48
Xu WD, Wang H, Wu Q, Wen LL, You ZQ, Yuan B, Chen SJ, Wang HD, Zhang X (2020) Morphology parameters for rupture in middle cerebral artery mirror aneurysms. J Neurointerv Surg 12:858–861. https://doi.org/10.1136/neurintsurg-2019-015620
Zhai X, Geng J, Zhu C, Yu J, Li C, Jiang N, **ang S, Fang G, Hu P, Zhang H (2021) Risk factors for pericallosal artery aneurysm rupture based on morphological computer-assisted semiautomated measurement and hemodynamic analysis. Front Neurosci 15:759806. https://doi.org/10.3389/fnins.2021.759806
Zhai XD, Yu JX, Li CJ, Ren J, Ji Z, He C, Ye M, Hu P, Zhang HQ (2020) Morphological characteristics of pericallosal artery aneurysms and their high propensity for rupture. World Neurosurg 133:e320–e326. https://doi.org/10.1016/j.wneu.2019.09.003
Funding
This work received support from the National Key Research Development Program (grant number 2016YFC1300800) and the Bei**g Scientific and Technologic Project (grant number Z201100005520021).
Author information
Authors and Affiliations
Contributions
SM-W and HQ-Z conceived and designed the research. SM-W, JW-G, and WZ-W developed the algorithm and conducted the CASAM and hemodynamic analysis. SM-W assessed aneurysm growth. SM-W, JW-G, and YD-W collected and reviewed the data. SM-W analyzed the data and performed statistical analysis. PH, CH, and HQ-Z managed funding and supervision. SM-W drafted the manuscript. All authors made critical revisions to the manuscript and reviewed the final version.
Corresponding author
Ethics declarations
Ethics approval
The study received approval from the research institute's committee on human research, and informed consent was obtained from all individual participants (Xuanwu Hospital; No. 2017082).
Informed consent
Informed consent was obtained from the parents or legal guardians of all individual participants included in the study.
Consent for publication
Not applicable.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Comments
The elderly present a distinct cohort of patients concerning aneurysms. In our assessment of risk factors contributing to the unstable growth of aneurysms in this demographic, we considered clinical information, morphological parameters. The Computer-Assisted Semi-Automatic Measurement (CASAM) method was employed to evaluate the three-dimensional morphological aspects of aneurysms. Utilizing these methodologies, we scrutinized 210 cases of unruptured aneurysms, aiming to discern the risk factors associated with aneurysm instability. Our objective was to assess the risk factors contributing to aneurysm instability (growth or rupture) within the elderly population. As dedicated readers of Acta Neurochirurgica, we hold confidence in the journal's ability to disseminate cutting-edge technologies and ideas to the broader community of neurosurgeons and neurointerventional physicians. We sincerely hope that our manuscript aligns with the publication standards of your esteemed journal.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, S., Geng, J., Wang, Y. et al. Risk factors of unruptured intracranial aneurysms instability in the elderly. Acta Neurochir 166, 35 (2024). https://doi.org/10.1007/s00701-024-05901-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00701-024-05901-w