Abstract
Purpose
We conducted this meta-analysis of randomized controlled trials (RCTs) to compare the efficacy of different doses of intravenous tranexamic acid (TXA) in spinal surgery.
Methods
We searched relevant academic articles from PubMed, Embase, the Cochrane Library, and CNKI. Two reviewers independently selected studies, assessed quality, extracted data, and evaluated the risk of bias. RevMan 5.4 was used for data analysis.
Results
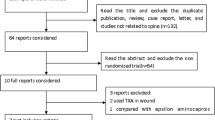
Ten randomized controlled trials (RCTs) met the inclusion criteria and were identified, including 740 patients. According to the different dose regimens of intravenous TXA, the included studies’ patients were divided into the high dose of intravenous TXA group and the low dose of intravenous TXA group. Compared with the low-dose group, the high-dose group can reduce the intraoperative blood loss (MD = − 100.87, 95% CI: [− 147.81, − 53.92], P < 0.0001). For the postoperative Hb and HCT, the high-dose group can separately maintain 4.54 g/dL (MD = 4.54, 95% CI: [2.08, 6.99], P = 0.003) and 1.27% (MD = 1.27, 95% CI: [0.59, 1.94], P = 0.0002). There were no statistically significant differences in total blood loss, preoperative Hb and HCT, operative time, and blood transfusion rate between the high-dose group and the low-dose group.
Conclusions
Based on the present meta-analysis, compared with the low-dose of intravenous TXA in spinal surgery, the high dose of intravenous TXA decreases the intraoperative blood loss and preserves higher postoperative Hb and HCT levels without increasing the operative time and blood transfusion rate.








Similar content being viewed by others
Availability of data and material
All data generated or analyzed during this study are included in this published article [and its supplementary information files].
References
Bess RS, Lenke LG (2006) Blood loss minimization and blood salvage techniques for complex spinal surgery. Neurosurg Clin N Am 17:227–234
Bible JE, Mirza M, Knaub MA (2018) Blood-loss management in spine surgery. J Am Acad Orthop Surg 26:35–44
Zhang L, Li YM, Liu D et al (2020) Combined use of tranexamic acid and rivaroxaban in posterior lumbar interbody fusion safely reduces blood loss and transfusion rates without increasing the risk of thrombosis—a prospective, stratified, randomized, controlled trial. Int Orthop 44:2079–2087. https://doi.org/10.1007/s00264-020-04699-3
Mikhail C, Pennington Z, Arnold PM et al (2020) Minimizing blood loss in spine surgery. Glob Spine J 10:71S-83S
Yoo JS, Ahn J, Karmarkar SS, Lamoutte EH, Singh K (2019) The use of tranexamic acid in spine surgery. Ann Transl Med 7:S172. https://doi.org/10.21037/atm.2019.05.36
Yang L, Jia X, Yang J, Kang J (2020) Tranexamic acid reduces blood cost in long-segment spinal fusion surgery: a randomized controlled study protocol. Medicine 99(37):e22069. https://doi.org/10.1097/MD.0000000000022069
Wang W, Duan K, Ma M et al (2018) Tranexamic acid decreases visible and hidden blood loss without affecting prethrombotic state molecular markers in transforaminal thoracic interbody fusion for treatment of thoracolumbar fracture-dislocation. Spine (Phila Pa 1976) 43:E734–E739
Li ZJ, Fu X, **ng D, Zhang HF, Zang JC, Ma XL (2013) Is tranexamic acid effective and safe in spinal surgery? A meta-analysis of randomized controlled trials. Eur Spine J 22:1950–1957
Kushioka J, Yamashita T, Okuda S et al (2017) High-dose tranexamic acid reduces intraoperative and postoperative blood loss in posterior lumbar interbody fusion. J Neurosurg Spine 26:363–367
Cheriyan T, Maier SP 2nd, Bianco K et al (2015) Efficacy of tranexamic acid on surgical bleeding in spine surgery: a meta-analysis. Spine J 15:752–761. https://doi.org/10.1016/j.spinee.2015.01.013
Xue P, Yang J, Xu X et al (2018) The efficacy and safety of tranexamic acid in reducing perioperative blood loss in patients with multilevel thoracic spinal stenosis: a retrospective observational study. Medicine (Baltimore) 97(50):e13643. https://doi.org/10.1097/MD.0000000000013643
Hasan MS, Yunus SN, Ng CC, Chan CYW, Chiu CK, Kwan MK (2021) Tranexamic acid in pediatric scoliosis surgery: a prospective randomized trial comparing high-dose and low-dose tranexamic acid in adolescent idiopathic scoliosis undergoing posterior spinal fusion surgery. Spine (Phila Pa 1976). 46(22):E1170–E1177. https://doi.org/10.1097/BRS.0000000000004076
Kim KT, Kim CK, Kim YC et al (2017) The effectiveness of low-dose and high-dose tranexamic acid in posterior lumbar interbody fusion: a double-blinded, placebo-controlled randomized study. Eur Spine J 26:2851–2857
Liu M, Zhang H, Yuan J, Yan H, Yang Y (2021) Hemostatic effect of single infusion of tranexamic acid with different loading dose before spinal surgery: a comparative study. Chin J Blood Transfusion 36:362–365 (in Chinese)
Meng X, Bao H, Zhang X et al (2014) The influence of blood lose with different dose of tranexamic acid in spinal surgery for patients. Shangdong Med J 54:62–63 (in Chinese)
Saleh AN, Mostafa RH (2018) Increased nociception following administration of different doses of tranexamic acid in adolescent idiopathic scoliosis surgery. Open Anesth J 12:61–68
**e J, Li T, Wang Y et al (2015) Different dose regimens of tranexamic acid reduces perioperative blood loss and blood transfusion in adolescent idiopathic scoliosis patients: a prospective, randomized control study. Spine J 15:S176
Yang X, Hao D, He B et al (2020) Efficacy and safety of blood loss with different dose of tranexamic acid in lumbar stenosis surgery for elderly patients. Chin J Spine Spinal Cord 30:727–734 (in Chinese)
Zhang NL, Pan ZQ, Zhang NP et al (2020) Effects of large and standard doses of TXA on coagulation functions in patients undergoing spinal orthopedic surgery. Med J Natl Defenging Forces Southwest China 30:431–434 (in Chinese)
Zhang Y, Yang Y (2017) Study of postoperative blood loss on patients with short segmental lumbar spinal stenosis with different doses intravenous tranexamic acid. Chin J Clin (Electron Ed) 11:1298–1302 (in Chinese)
Zhu X, Shi Q, Li D et al (2020) Two doses of tranexamic acid reduce blood loss in primary posterior lumbar fusion surgery. Clin Spine Surg 33:E593–E597
Zhang H, Chen J, Chen F, Que W (2012) The effect of tranexamic acid on blood loss and use of blood products in total knee arthroplasty: a meta-analysis. Knee Surg Sports Traumatol Arthrosc 20:1742–1752
**n W, Gao Y, Shen J, Yang X (2019) Intravenous tranexamic acid reduces bloodtransfusions in revision total hiparthroplasty a meta-analysis. J Comp Eff Res 8:917–928
Yuan QM, Zhao ZH, Xu BS (2017) Efficacy and safety of tranexamic acid in reducing blood loss in scoliosis surgery: a systematic review and meta-analysis. Eur Spine J 26:131–139
Hsu G, Taylor JA, Fiadjoe JE et al (2016) Aminocaproic acid administration is associated with reduced perioperative blood loss and transfusion in pediatric craniofacial surgery. Acta Anaesthesiol Scand 60:158–165
Liang JQ, Rong TH, Liu HZ et al (2020) Topical injection of tranexamic acid via a drain plus drain-clam** to reduce blood loss in degenerative lumbar scoliosis surgery. Orthop Surg 12:67–73
**ong Z, Wu K, Zhang J et al (2020) Different dose regimens of intravenous tranexamic acid in adolescent spinal deformity surgery: a systematic review and meta-analysis. Biomed Res Int 2020:16. https://doi.org/10.1155/2020/3101358
Smith PR, Crighton I (2009) Tranexamic acid dosage in spinal surgery: an on-line survey of UK consultant anaesthetists. Br J Anaesth 103:315P-329P
Chiem J, Ivanova I, Parker A, Krengel W 3rd, Jimenez N (2017) Anaphylactic reaction to tranexamic acid in an adolescent undergoing posterior spinal fusion. Paediatr Anaesth 27:774–775
Gerstein NS, Brierley JK, Culling MD (2015) Left ventricle thrombus after tranexamic acid for spine surgery in an HIV-positive patient. Spine J 16:77–82. https://doi.org/10.1016/j.spinee.2015.10.039
Funding
This work was supported by the following funding: The Joint Project of Yunnan Science and Technology Department and Kunming Medical University Foundation (Grant Number 202201AY070001-054).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Database searching, material preparation, data collection and analysis were performed by CQ, PG, HG, KD. The first draft of the manuscript was written by CQ and KD, and the final draft was modified by CZ and KD. CQ and KD contributed equally to this paper. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Drs. Chao Qin and Kaili Du contributed equally to this paper. And all the authors have given their consent to this choice. There won't be any overlap** interests.
Rights and permissions
About this article
Cite this article
Qin, C., Du, Kl., Guo, Py. et al. Tranexamic acid dosage for spinal surgery: a meta-analysis. Eur Spine J 31, 2493–2501 (2022). https://doi.org/10.1007/s00586-022-07315-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-022-07315-7