Abstract
Purpose
To measure the pedicle dimensions in high grade lytic spondylolisthesis (HGL) and to classify them, which helps the spine surgeon in proper selection of pedicle screws.
Methods
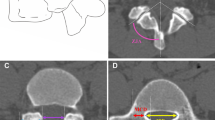
A study of CT scans in 100 consecutive patients between Jan 2017 and April 2021 diagnosed as single-level HGL on standing radiographs. Pedicle height (PH), Pedicle width (PW), Differential pedicle height (DPH), Screw length (SL) and Transverse pedicle angle (TPA) were measured and analyzed. PH and PW were classified into four grades as—grade A less than 5.0 mm, grade B between 5.0 and 6.0 mm, grade C between 6.0 and 7.0 mm, and grade D above 7.0 mm.
Results
5 males and 95 females with mean age of 49.1 years. PH in 44% lytic vertebra were grade A, B (less than 6 mm) and the rest 56% had grade C, D (greater than 6 mm). PH averaged 6.6 mm in grade 3 HGL, 5.61 mm in grade 4 HGL. Change in PW, SL and TPA was not statistically significant with regards to grade or level of listhesis. A total of 37 cases were noted to have DPH (25 cases had a difference < 2 mm and 12 had a difference > 2 mm).
Conclusion
44% of the PH in lytic vertebra was grade A and B (less than 6 mm) that stresses the importance of pre-op CT assessment and planning the appropriate screw dimensions. Change in PH was statistically significant with regards to the grade of listhesis (P-value < 0.01). Differential pedicle height also need to be looked for.



Similar content being viewed by others
References
Kalichman L, Kim DH, Li L et al (2009) Spondylolysis and spondylolisthesis: prevalence and association with low back pain in the adult community-based population. Spine 34(2):199–205
Gaines RW (2005) L5 vertebrectomy for the surgical treatment of spondyloptosis: thirty cases in 25 years. Spine 30(Suppl 6):S66–S70
Min K, Liebscher T, Rothenfluh D (2012) Sacral dome resection and single-stage posterior reduction in the treatment of high-grade high dysplastic spondylolisthesis in adolescents and young adults. Eur Spine J 21(Suppl 6):S785–S791
Bouyer B, Bachy M, Courvoisier A et al (2014) High-grade lumbosacral spondylolisthesis reduction and fusion in children using trans sacral rod fixation. Childs Nerv Syst 30(3):505–513
Gertzbein SD, Robbins SE (1990) Accuracy of pedicular screw placement in vivo. Spine 15:11–14
Weinstein JN, Spratt KF, Spengler D et al (1998) Spinal pedicle fixation: reliability and validity of roentgenograms based assessment and surgical factors on successful screw placement. Spine 13:1012–1018
Choi HJ, Park JY, Chin DK (2014) Anatomical parameters of a fifth lumbar vertebra in L5–S1 spondylolytic spondylolisthesis from a surgical point of view. Eur Spine J 23(9):1896–1902
Bajwa NS, Toy JO, Ahn NU (2012) L5 pedicle length is increased in subjects with spondylolysis: an anatomic study of 1072 cadavers. Clin Orthop Relat Res 470(11):3202–3206
Ergun T, Sahin MS, Lakadamyali H (2011) Evaluation of the relationship between L5–S1 spondylolysis and isthmic spondyl- olisthesis and lumbosacral-pelvic morphology by imaging via 2- and 3-dimensional reformatted computed tomography. J Comput Assist Tomogr 35:9–15
Masharawi Y (2012) Lumbar shape characterization of the neural arch and vertebral body in spondylolysis: a comparative skeletal study. Clin Anat 25:224–230
Mehta JS, Kochhar S, Harding IJ (2012) A slip above a slip: retrolisthesis of the motion segment above a spondylolytic spondylolisthesis. Eur Spine J 21:2128–2133
Rankine JJ, Dickson RA (2010) Unilateral spondylolysis and the presence of facet joint tropism. Spine (Phila Pa 1976)s 35:E1111–E1114
Krag MH, Weaver DL, Beynnon BD (1988) Morphometry of the thoracic and lumbar spine-related to transpedicular screw placement for surgical spinal fixation. Spine (Phila Pa 1976) 13:27–32
Mitra SR, Datir SP, Jadhav SO (2002) Morphometric study of the lumbar pedicle in the Indian population as related to pedicular screw fixation. Spine (Phila Pa 1976) 27:453–459
Bernard TN, Seibert CE (1992) Pedicle diameter determined by computed tomography. Its relevance to pedicle screw fixation in the lumbar spine. Spine (Phila Pa 1976) 17:S160–S163
Chadha M, Balain B, Maini L (2003) Pedicle morphology of the lower thoracic, lumbar, and S1 vertebrae: an Indian perspective. Spine (Phila Pa 1976) 28:744–749
Zindrick MR, Wiltse LL, Widell EH et al (1986) A biomechanical study of intrapeduncular screw fixation in the lumbosacral spine. Clin Orthop 203:99–112
Esses SI, Sachs BL, Dreyzin V (1993) Complications associated with the technique of pedicle screw fixation. A selected survey of ABS members. Spine (Phila Pa 1976) 18:2231–2238
Makino T, Kaito T, Fujiwara H (2012) Analysis of lumbar pedicle morphology in degenerative spines using multiplanar reconstruction computed tomography: what can be the reliable index for optimal pedicle screw diameter? Eur Spine J 21(8):1516–1521
Okuda S, Miyauchi A, Oda T et al (2006) Surgical complications of posterior lumbar interbody fusion with total facetectomy in 251 patients. J Neurosurg Spine 4:304–309
Okuyama K, Abe E, Suzuki T et al (1999) Posterior lumbar interbody fusion: a retrospective study of complications after facet joint excision and pedicle screw fixation in 148 cases. Acta Orthop Scand 70:329–334
Freeman BJ, Licina P, Mehdian SH (2000) Posterior lumbar interbody fusion combined with instrumented postero-lateral fusion: 5-year results in 60 patients. Eur Spine J9:42–46
Jutte PC, Castelein RM (2002) Complications of pedicle screws in lumbar and lumbosacral fusions in 105 consecutive primary operations. Eur Spine J 11:594–598
Suk SI, Lee CK, Kim WJ et al (1997) Adding posterior lumbar interbody fusion to pedicle screw fixation and postero-lateral fusion after decompression in spondylolytic spondylolisthesis. Spine (Phila Pa 1976) 22:210–219
Belfi LM, Ortiz AO, Katz DS (2006) Computed tomography evaluation of spondylolysis and spondylolisthesis in asymptomatic patients. Spine (Phila Pa 1976) 31:E907–E910
Hajek PC, Baker LL, Goobar JE et al (1987) Focal fat deposition in axial bone marrow: MR characteristics. Radiology 162:245–249
de Roos A, Kressel H, Spitzer C (1987) MR imaging of marrow changes adjacent to end plates in degenerative lumbar disk disease. AJR Am J Roentgenol 149:531–534
Acknowledgement
Sources of support - Study has been sponsored by AO spine international.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have not disclosed any conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Degulmadi, D., Dave, B., Krishnan, A. et al. ‘Higher the grade-smaller the pedicle’: a study of pedicle dimensional variations in 100 cases of high grade lytic spondylolisthesis. Eur Spine J 32, 455–461 (2023). https://doi.org/10.1007/s00586-022-07277-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-022-07277-w