Abstract
Purpose
To compare early changes in the ASIA Motor Score (AMS) between patients with central cord syndrome (CCS) from an acute fracture to patients without a fracture.
Methods
Patients with CCS were identified and stratified based on the presence of a fracture. The AMS through the first week of the patients’ hospitalization was obtained. Initial injury severity as well as early neurologic recovery was measured using the AMS. Analysis of variance was performed to determine if age, gender, rectal tone at presentation, congenital stenosis, or surgery within 24 h significantly effected the change in AMS.
Results
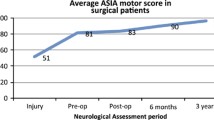
A strong trend (p = 0.0504) towards a more severe initial neurologic injury in patients with a fracture (AMS 59.7) than in patients without a fracture (AMS 70.2) was identified. However, in the week after injury, patients with a fracture had an improvement in their neurologic function (ΔAMS +4.8) while patients without a fracture demonstrated neurologic decline (ΔAMS −5.9). The change in AMS between patients with and without a fracture was nearly significant (p = 0.06).
Conclusion
Patients with central cord syndrome present with similar symptoms, but injuries with and without a fracture may be associated with a different early neurologic recovery. Patients with a fracture have a more severe injury at initial presentation, but tend to have neurologic improvement in the first week; conversely patients without a fracture have a less severe initial neurologic injury, but tend to have a slight decline in neurologic function over the first week.
Similar content being viewed by others
References
Aarabi B, Koltz M, Ibrahimi D (2008) Hyperextension cervical spine injuries and traumatic central cord syndrome. Neurosurg Focus 25:E9. doi:10.3171/FOC.2008.25.11.E9
Raja Rampersaud Y, Fisher C, Wilsey J, Arnold P, Anand N, Bono CM, Dailey AT, Dvorak M, Fehlings MG, Harrop JS, Oner FC, Vaccaro AR (2006) Agreement between orthopedic surgeons and neurosurgeons regarding a new algorithm for the treatment of thoracolumbar injuries: a multicenter reliability study. J Spinal Disord Tech 19:477–482. doi:10.1097/01.bsd.0000211237.14211.21
Fehlings MG, Vaccaro A, Wilson JR, Singh A, Cadotte DW, Harrop JS, Aarabi B, Shaffrey C, Dvorak M, Fisher C, Arnold P, Massicotte EM, Lewis S, Rampersaud R (2012) Early versus delayed decompression for traumatic cervical spinal cord injury: results of the Surgical Timing in Acute Spinal Cord Injury Study (STASCIS). PLoS ONE 7:e32037. doi:10.1371/journal.pone.0032037
Schneider RC, Cherry G, Pantek H (1954) The syndrome of acute central cervical spinal cord injury; with special reference to the mechanisms involved in hyperextension injuries of cervical spine. J Neurosurg 11:546–577. doi:10.3171/jns.1954.11.6.0546
Anderson DG, Sayadipour A, Limthongkul W, Martin ND, Vaccaro A, Harrop JS (2012) Traumatic central cord syndrome: neurologic recovery after surgical management. Am J Orthop (Belle Mead NJ) 41:E104–E108
Chen L, Yang H, Yang T, Xu Y, Bao Z, Tang T (2009) Effectiveness of surgical treatment for traumatic central cord syndrome. J Neurosurg Spine 10:3–8. doi:10.3171/2008.9.SPI0822
Guest J, Eleraky MA, Apostolides PJ, Dickman CA, Sonntag VK (2002) Traumatic central cord syndrome: results of surgical management. J Neurosurg 97:25–32
Stevens EA, Marsh R, Wilson JA, Sweasey TA, Branch CL Jr, Powers AK (2010) A review of surgical intervention in the setting of traumatic central cord syndrome. Spine J 10:874–880. doi:10.1016/j.spinee.2010.07.388
Ishida Y, Tominaga T (2002) Predictors of neurologic recovery in acute central cervical cord injury with only upper extremity impairment. Spine (Phila Pa 1976) 27:1652–1658; discussion 1658. pii:00007632-200208010-00011
Karadimas SK, Erwin WM, Ely CG, Dettori JR, Fehlings MG (2013) Pathophysiology and natural history of cervical spondylotic myelopathy. Spine (Phila Pa 1976) 38:S21–S36. doi:10.1097/BRS.0b013e3182a7f2c3
Karadimas SK, Moon ES, Yu WR, Satkunendrarajah K, Kallitsis JK, Gatzounis G, Fehlings MG (2013) A novel experimental model of cervical spondylotic myelopathy (CSM) to facilitate translational research. Neurobiol Dis 54:43–58. doi:10.1016/j.nbd.2013.02.013
Yu WR, Liu T, Kiehl TR, Fehlings MG (2011) Human neuropathological and animal model evidence supporting a role for Fas-mediated apoptosis and inflammation in cervical spondylotic myelopathy. Brain 134:1277–1292. doi:10.1093/brain/awr054
Fawcett JW, Curt A, Steeves JD, Coleman WP, Tuszynski MH, Lammertse D, Bartlett PF, Blight AR, Dietz V, Ditunno J, Dobkin BH, Havton LA, Ellaway PH, Fehlings MG, Privat A, Grossman R, Guest JD, Kleitman N, Nakamura M, Gaviria M, Short D (2007) Guidelines for the conduct of clinical trials for spinal cord injury as developed by the ICCP panel: spontaneous recovery after spinal cord injury and statistical power needed for therapeutic clinical trials. Spinal Cord 45:190–205. doi:10.1038/sj.sc.3102007
Marino RJ, Graves DE (2004) Metric properties of the ASIA motor score: subscales improve correlation with functional activities. Arch Phys Med Rehabil 85:1804–1810 (pii:S0003999304004800)
Dvorak MF, Fisher CG, Hoekema J, Boyd M, Noonan V, Wing PC, Kwon BK (2005) Factors predicting motor recovery and functional outcome after traumatic central cord syndrome: a long-term follow-up. Spine (Phila Pa 1976) 30:2303–2311 (pii:00007632-200510150-00012)
Aarabi B, Alexander M, Mirvis SE, Shanmuganathan K, Chesler D, Maulucci C, Iguchi M, Aresco C, Blacklock T (2011) Predictors of outcome in acute traumatic central cord syndrome due to spinal stenosis. J Neurosurg Spine 14:122–130. doi:10.3171/2010.9.SPINE09922
Yamazaki T, Yanaka K, Fujita K, Kamezaki T, Uemura K, Nose T (2005) Traumatic central cord syndrome: analysis of factors affecting the outcome. Surg Neurol 63:95–99. doi:10.1016/j.surneu.2004.03.020 (discussion 99–100)
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Schroeder, G.D., Kepler, C.K., Hjelm, N. et al. The effect of vertebral fracture on the early neurologic recovery in patients with central cord syndrome. Eur Spine J 24, 985–989 (2015). https://doi.org/10.1007/s00586-015-3865-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-015-3865-6