Abstract
Background
Chemoradiotherapy (CRT) modulates the tumor immune microenvironment of multiple cancer types, including esophageal cancer, which potentially induces both immunogenicity and immunosuppression by upregulating the presentation of tumor-specific antigens and immune checkpoint molecules in tumors, respectively. The prognostic effects of immune modification by CRT in esophageal squamous cell carcinoma (ESCC) remain controversial because of the lack of detailed immunological analyses using paired clinical specimens before and after CRT. We aimed to clarify the immunological changes in the tumor microenvironment caused by CRT and elucidate the predictive importance of clinical response and prognosis and the rationale for the necessity of subsequent programmed cell death protein 1 (PD-1) inhibitor treatment.
Methods
In this study, we performed a comprehensive immunological analysis of paired biopsy specimens using multiplex immunohistochemistry before and after CRT in patients with unresectable locally advanced ESCC.
Results
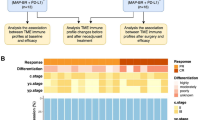
CRT significantly increased the intra-tumoral infiltration and PD-1 expression of CD8+ T cells and conventional CD4+ T cells but decreased those of regulatory T cells and the accumulation of tumor-associated macrophages. Multivariate analysis of tumor-infiltrating T-cell phenotypes revealed that the density of PD-1+CD8+ T cells in the tumor after CRT could predict a confirmed complete response and favorable survival.
Conclusions
This study showed that CRT improved the immunological characteristics of unresectable locally advanced ESCC and identified the density of PD-1+CD8+ T cells as a predictive factor for prognosis. This finding supports the rationale for the necessity of subsequent PD-1 inhibitor treatment.




Similar content being viewed by others
References
Sung H, Ferlay J, Siegel RL, et al. Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2021;71:209–49.
Shah MA, Altorki N, Patel P, et al. Improving outcomes in patients with oesophageal cancer. Nat Rev Clin Oncol. 2023;20:390–407.
Grille VJ, Campbell S, Gibbs JF, Bauer TL. Esophageal cancer: the rise of adenocarcinoma over squamous cell carcinoma in the Asian belt. J Gastrointest Oncol. 2021;12:S339–49.
Tahara M, Ohtsu A, Hironaka S, et al. Clinical impact of criteria for complete response (CR) of primary site to treatment of esophageal cancer. Jpn J Clin Oncol. 2005;35:316–23.
Ohtsu A, Boku N, Muro K, et al. Definitive chemoradiotherapy for T4 and/or M1 lymph node squamous cell carcinoma of the esophagus. J Clin Oncol. 1999;17:2915–21.
Shinoda M, Ando N, Kato K, et al. Randomized study of low-dose versus standard-dose chemoradiotherapy for unresectable esophageal squamous cell carcinoma (JCOG0303). Cancer Sci. 2015;106:407–12.
Habu T, Kumanishi R, Ogata T, et al. Complete response to definitive chemoradiotherapy in unresectable locally advanced esophageal squamous cell carcinoma. Esophagus. 2023;20:533–40.
Sun JM, Shen L, Shah MA, et al. Pembrolizumab plus chemotherapy versus chemotherapy alone for first-line treatment of advanced oesophageal cancer (KEYNOTE-590): a randomised, placebo-controlled, phase 3 study. Lancet. 2021;398:759–71.
Doki Y, Ajani JA, Kato K, et al. Nivolumab combination therapy in advanced esophageal squamous-cell carcinoma. N Engl J Med. 2022;386:449–62.
Kelly RJ, Ajani JA, Kuzdzal J, et al. Adjuvant nivolumab in resected esophageal or gastroesophageal junction cancer. N Engl J Med. 2021;384:1191–203.
Bando H, Tsukada Y, Ito M, Yoshino T. Novel immunological approaches in the treatment of locally advanced rectal cancer. Clin Colorectal Cancer. 2022;21:3–9.
Antonia SJ, Villegas A, Daniel D, et al. Durvalumab after chemoradiotherapy in stage III non-small-cell lung cancer. N Engl J Med. 2017;377:1919–29.
Soeratram TT, Creemers A, Meijer SL, et al. Tumor-immune landscape patterns before and after chemoradiation in resectable esophageal adenocarcinomas. J Pathol. 2022;256:282–96.
Kotsafti A, Scarpa M, Cavallin F, et al. Immune surveillance activation after neoadjuvant therapy for esophageal adenocarcinoma and complete response. Oncoimmunology. 2020;9:1804169.
Brierley JD, Gospodarowicz MK, Wittekind C. TNM classification of malignant tumours. 8th ed. Wiley Blackwell; 2017.
Japan ES. Japanese classification of esophageal cancer, 11th edition: part I. Esophagus. 2017;14:1–36.
Eisenhauer EA, Therasse P, Bogaerts J, et al. New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer. 2009;45:228–47.
Kanda Y. Investigation of the freely available easy-to-use software “EZR” for medical statistics. Bone Marrow Transplant. 2013;48:452–8.
Herter-Sprie GS, Koyama S, Korideck H, et al. Synergy of radiotherapy and PD-1 blockade in Kras-mutant lung cancer. JCI Insight. 2016;1: e87415.
An L, Li M, Jia Q. Mechanisms of radiotherapy resistance and radiosensitization strategies for esophageal squamous cell carcinoma. Mol Cancer. 2023;22:140.
Deng L, Liang H, Xu M, et al. STING-dependent cytosolic DNA sensing promotes radiation-induced type I interferon-dependent antitumor immunity in immunogenic tumors. Immunity. 2014;41:843–52.
Fucikova J, Kepp O, Kasikova L, et al. Detection of immunogenic cell death and its relevance for cancer therapy. Cell Death Dis. 2020;11:1013.
Apetoh L, Ghiringhelli F, Tesniere A, et al. Toll-like receptor 4-dependent contribution of the immune system to anticancer chemotherapy and radiotherapy. Nat Med. 2007;13:1050–9.
Sato H, Niimi A, Yasuhara T, et al. DNA double-strand break repair pathway regulates PD-L1 expression in cancer cells. Nat Commun. 2017;8:1751.
Haddad R, Zlotnik O, Goshen-Lago T, et al. Tumor lymphocyte infiltration is correlated with a favorable tumor regression grade after neoadjuvant treatment for esophageal adenocarcinoma. J Pers Med. 2022;12:627.
Zingg U, Montani M, Frey DM, et al. Tumour-infiltrating lymphocytes and survival in patients with adenocarcinoma of the oesophagus. Eur J Surg Oncol. 2010;36:670–7.
Koemans WJ, van Dieren JM, van den Berg JG, et al. High CD8(+) tumour-infiltrating lymphocyte density associates with unfavourable prognosis in oesophageal adenocarcinoma following poor response to neoadjuvant chemoradiotherapy. Histopathology. 2021;79:238–51.
Zingg U, Montani M, Frey DM, et al. Influence of neoadjuvant radio-chemotherapy on tumor-infiltrating lymphocytes in squamous esophageal cancer. Eur J Surg Oncol. 2009;35:1268–72.
Park S, Joung JG, Min YW, et al. Paired whole exome and transcriptome analyses for the Immunogenomic changes during concurrent chemoradiotherapy in esophageal squamous cell carcinoma. J Immunother Cancer. 2019;7:128.
Wen J, Fang S, Hu Y, et al. Impacts of neoadjuvant chemoradiotherapy on the immune landscape of esophageal squamous cell carcinoma. EBioMedicine. 2022;86: 104371.
Minashi K, Nihei K, Mizusawa J, et al. Efficacy of endoscopic resection and selective chemoradiotherapy for stage I esophageal squamous cell carcinoma. Gastroenterology. 2019;157:382–90 (e3).
Kato K, Ito Y, Nozaki I, et al. Parallel-group controlled trial of surgery versus chemoradiotherapy in patients with stage I esophageal squamous cell carcinoma. Gastroenterology. 2021;161:1878–86 (e2).
Sudo K, **ao L, Wadhwa R, et al. Importance of surveillance and success of salvage strategies after definitive chemoradiation in patients with esophageal cancer. J Clin Oncol. 2014;32:3400–5.
Motoori M, Yano M, Ishihara R, et al. Comparison between radical esophagectomy and definitive chemoradiotherapy in patients with clinical T1bN0M0 esophageal cancer. Ann Surg Oncol. 2012;19:2135–41.
Takeuchi H, Ito Y, Machida R, et al. A single-arm confirmatory study of definitive chemoradiation therapy including salvage treatment for clinical stage II/III esophageal squamous cell carcinoma (JCOG0909 study). Int J Radiat Oncol Biol Phys. 2022;114:454–62.
Yang H, Liu H, Chen Y, et al. Long-term efficacy of neoadjuvant chemoradiotherapy plus surgery for the treatment of locally advanced esophageal squamous cell carcinoma: the NEOCRTEC5010 randomized clinical trial. JAMA Surg. 2021;156:721–9.
van Hagen P, Hulshof MC, van Lanschot JJ, et al. Preoperative chemoradiotherapy for esophageal or junctional cancer. N Engl J Med. 2012;366:2074–84.
Cooper JS, Guo MD, Herskovic A, et al. Chemoradiotherapy of locally advanced esophageal cancer: long-term follow-up of a prospective randomized trial (RTOG 85–01). Radiat Ther Oncol Group JAMA. 1999;281:1623–7.
Kumagai S, Togashi Y, Kamada T, et al. The PD-1 expression balance between effector and regulatory T cells predicts the clinical efficacy of PD-1 blockade therapies. Nat Immunol. 2020;21:1346–58.
Thommen DS, Koelzer VH, Herzig P, et al. A transcriptionally and functionally distinct PD-1(+) CD8(+) T cell pool with predictive potential in non-small-cell lung cancer treated with PD-1 blockade. Nat Med. 2018;24:994–1004.
Kim S, Boustani J, Vernerey D, et al. Phase II INTERACT-ION study: ezabenlimab (BI 754091) and mDCF (docetaxel, cisplatin, and 5-fluorouracil) followed by chemoradiotherapy in patients with Stage III squamous cell anal carcinoma. Front Oncol. 2022;12: 918499.
Bando H, Kotani D, Tsushima T, et al. TENERGY: multicenter phase II study of Atezolizumab monotherapy following definitive Chemoradiotherapy with 5-FU plus Cisplatin in patients with unresectable locally advanced esophageal squamous cell carcinoma. BMC Cancer. 2020;20:336.
Klug F, Prakash H, Huber PE, et al. Low-dose irradiation programs macrophage differentiation to an iNOS+/M1 phenotype that orchestrates effective T cell immunotherapy. Cancer Cell. 2013;24:589–602.
Peranzoni E, Lemoine J, Vimeux L, et al. Macrophages impede CD8 T cells from reaching tumor cells and limit the efficacy of anti-PD-1 treatment. Proc Natl Acad Sci USA. 2018;115:E4041–50.
Arlauckas SP, Garris CS, Kohler RH, et al. In vivo imaging reveals a tumor-associated macrophage-mediated resistance pathway in anti-PD-1 therapy. Sci Transl Med. 2017. https://doi.org/10.1126/scitranslmed.aal3604.
Acknowledgements
We thank all patients who participated in this study and their families and caregivers. We thank T. Takaku, K. Onagawa, M. Takemura, M. Hoshino, Y. Osada, C. Ozawa, and X. Takakura for their technical assistance.
Funding
This study was supported by a Grant-in-Aid for Scientific Research (C Grant No. 21K07252 [S. Koyama], JSPS Fellows no. 22KJ3156 [S. Kumagai], Early-Career Scientists no. 23K15088 [S. Kumagai], PAGS nos. 202130, 212126, 221184, and 231279 [S. Kumagai]); Japan Agency for Medical Research and Development (AMED)—the Moonshot Research and Development Program grant (no. 22zf0127009h0001 [H. Nishikawa, S. Koyama]); AMED—the Project for Promotion of Cancer Research and Therapeutic Evolution (P-PROMOTE no. 22ama221301h0001 [H. Nishikawa, S. Koyama.], no. 22ama221507h0001 [S. Kumagai], no. 23ama221329h0001 [S.Koyama]); AMED—the Practical Research for Innovative Cancer Control (no. 22ck0106724h0001 [H. Nishikawa, S. Koyama], no.22ck0106773h0001 [S. Kumagai], no. 23ck0106796h0001 [S. Koyama]); Canon Foundation (S. Koyama.); Mitsubishi Foundation (S. Koyama.); Takeda Science Foundation (S. Kumagai); Taiju Life Social Welfare Foundation (S. Kumagai); Astellas Foundation for Research on Metabolic Disorders (S. Kumagai); Senri Life Science Foundation (S. Kumagai); Uehara Memorial Foundation (S. Kumagai); Chugai Foundation for Innovative Drug Discovery Science (S. Kumagai); Japan Neurosurgical Society (S. Kumagai); and Japan Lung Cancer Society (a nonprofit organization) (S. Kumagai).
Author information
Authors and Affiliations
Contributions
T. Habu, S. Kumagai, H. Bando, S. Koyama, and T. Kojima designed the study. T. Habu, S. Kumagai, and S. Koyama wrote the initial draft of the manuscript. T. Habu, S. Kumagai, H. Bando, S. Koyama, and T. Kojima contributed to the analysis and interpretation of the data and assisted in manuscript preparation. All the other authors contributed to the data collection, interpretation, and critical review of the manuscript. All authors have approved the final version of the manuscript and agreed to be accountable for all aspects of the study. We ensured that all questions related to the accuracy or integrity of any part of the study were appropriately investigated and resolved.
Corresponding authors
Ethics declarations
Conflict of interest
H. Bando reports honoraria from Ono Pharmaceutical, Taiho Pharmaceutical and Eli Lilly Japan. D. Kotani reports honoraria from Takeda, Chugai, Lilly, MSD, Ono, Seagen, Guardant Health, Eisai, Taiho, Bristol Myers Squibb, Daiichi-Sankyo, Pfizer, Merckbiopharma, and Sysmex, research funding from Ono, MSD, Novartis, Servier, Janssen, IQVIA, Syneoshealth, CIMIC, and Cimicshiftzero. M. Nakamura reports receiving personal fees from AstraZeneca and a research grant from illumina, outside the submitted work. S. Mitsunaga reports honoraria and research funding from Toray Industries, Pharmaceutical Co. Ltd., Chugai Pharmaceutical Co., Ltd., Astellas Pharma, A**omoto, Taiho Pharmaceutical Co., Ltd., PFDeNA outside the submitted work, and personal fees from Ono Pharmaceutical Co. Ltd. outside the submitted work. H. Nishikawa received research funding and honoraria from Ono Pharmaceutical, Bristol-Myers Squibb, Chugai Pharmaceutical, and MSD, honoraria from Amgen and research funding from Taiho Pharmaceutical, Daiichi-Sankyo, Kyowa Kirin, Zenyaku Kogyo, Oncolys BioPharma, Debiopharma, Asahi-Kasei, Sysmex, Fujifilm, SRL, Astellas Pharmaceutical, Sumitomo Dainippon Pharma, and BD Japan outside of this study. S. Koyama has received research funding from Otsuka Pharmaceutical and Chugai Pharmaceuticals. T. Kojima reports receiving research funding from Beigene Ltd., AstraZeneca, Chugai Pharmaceutical, Parexel International, Shionogi, Taiho Pharmaceutical, Astellas Amgen BioPharma, MSD, and Ono Pharmaceutical; honoraria from Ono Pharmaceutical, Covidien Japan, MSD, Boehringer Ingelheim, Kyowa Kirin, EA Pharma, Bristol-Myers Squibb, 3H Clinical Trial, AstraZeneca, Taiho Pharmaceutical, Liang Yi Hui Healthcare Oncology News China, Japanese Society of Pharmaceutical Health Care and Sciences, Oncolys BioPharma, and BMS; advisory roles for Ono Pharmaceutical, Taiho Pharmaceutical, Japanese Society of Pharmaceutical Health Care and Sciences, and Liang Yi Hui Healthcare Oncology News China. All other authors have no conflicts of interest to disclose.
Ethical approval
The study protocol was approved by the Institutional Review Board of the National Cancer Center (2021–2022). This study was conducted in accordance with the Declaration of Helsinki and the Japanese Ethical Guidelines for Medical and Health Research Involving Human Subjects.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Online Resource 2
The effects of CRT on immune checkpoint molecules expressed by TIL subpopulations. We evaluated the changes in immune checkpoint molecule expression induced by TILs before and after CRT. The densities of each TIL subpopulation before and after CRT were compared using a paired t test. a Programmed cell death protein 1 positivity in CD3+, CD3+CD8+, CD3+CD8–FoxP3–, and CD3+CD8–FoxP3+ lymphocytes before and after CRT. b The densities of CD3+CD8+TIGIT+ (left), CD3+CD8+LAG-3+ (middle), and CD3+CD8+Tim-3+ (right) cells in the tumor bed before and after CRT. c The densities of CD3+CD8–FoxP3+CTLA-4+ lymphocytes before and after CRT. (DOCX 904 KB)
Online Resource 3
The association between TIL phenotypes before CRT and cCR. The densities of the TIL subpopulations before CRT were compared between patients who experienced cCR and those who did not. a The densities of CD3+ (left), CD3+CD8+ (middle), and CD3+CD8–Foxp3– (right) lymphocytes before CRT were compared between the two groups. b The densities of CD3+CD8–Foxp3+ lymphocytes (left) and CD206+ macrophages (right) before CRT were compared between the two groups. c The densities of CD3+PD-1+, CD3+CD8+PD-1+, CD3+CD8–Foxp3−PD-1+, and CD3+CD8–Foxp3+PD-1+ lymphocytes before CRT were compared between the two groups. (DOCX 2214 KB)
Online Resource 4
The association between TIL phenotypes before CRT and PFS. The PFS of patients with esophageal squamous cell carcinoma was evaluated according to TIL phenotypes before CRT using the Kaplan–Meier analysis. The PFS curves of patients are shown, according to the densities of CD3+ (a), CD3+PD-1+ (b), CD3+CD8+ (c), CD3+CD8+PD-1+ (d), CD3+CD8–Foxp3– (e), CD3+CD8–Foxp3–PD-1+ (f), and CD3+CD8–Foxp3+ lymphocytes (g) and CD206+ macrophages (h) in the tumor bed before CRT. (DOCX 834 KB)
Online Resource 5.
The effects of CRT on immune checkpoint molecules expressed by TIL subpopulations in non-cCR patients were evaluated. We assessed the changes in immune checkpoint molecule expression induced by TILs before and after CRT in non-cCR patients (n = 27). The densities of each TIL subpopulation before and after CRT were compared using a paired t test. Programmed cell death protein 1 positivity in CD3+, CD3+CD8+, CD3+CD8–FoxP3–, and CD3+CD8–FoxP3+ lymphocytes before and after CRT were examined. (PDF 246 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Habu, T., Kumagai, S., Bando, H. et al. Definitive chemoradiotherapy induces T-cell-inflamed tumor microenvironment in unresectable locally advanced esophageal squamous cell carcinoma. J Gastroenterol (2024). https://doi.org/10.1007/s00535-024-02120-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00535-024-02120-z