Abstract
Purpose
To identify elements of timely integration of palliative care (PC) into hospital oncology care from best practices. Thereafter, to assess the level of consensus among oncology and PC specialists and patient and relative representatives on the characteristics of timely integration of PC.
Methods
A three-round modified Delphi study was conducted. The expert panel consisted of 83 healthcare professionals (HCPs) from 21 Dutch hospitals (43 physicians, 40 nurses), 6 patient and 2 relative representatives. In the first round, four elements of integrated PC were considered: (1) identification of potential PC needs, (2) advance care planning (ACP), (3) routine symptom monitoring and (4) involvement of the specialist palliative care team (SPCT). In subsequent rounds, the panellists assessed which characteristics were triggers for initiating an element. A priori consensus was set at ≥ 70%.
Results
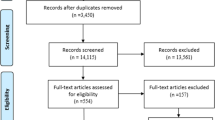
A total of 71 (78%) panellists completed the first questionnaire, 65 (71%) the second and 49 (54%) the third. Panellists agreed that all patients with incurable cancer should have their PC needs assessed (97%), symptoms monitored (91%) and ACP initiated (86%). The SPCT should be involved at the patient’s request (86%) or when patients suffer from increased symptom burden on multiple dimensions (76%). Patients with a life expectancy of less than 3 months should be offered a consultation (71%).
Conclusion
The expert panel agreed that timely integration of PC into oncology is important for all patients with incurable cancer, using early identification, ACP and routine symptom monitoring. Involvement of the SPCT is particularly needed in patients with multidimensional symptom burden and in those nearing death.

Similar content being viewed by others
References
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA: Cancer J Clin 71:209–249
Mathers CD, Loncar D (2006) Projections of global mortality and burden of disease from 2002 to 2030. PLoS Med 3:e442
Etkind SN, Bone AE, Gomes B, Lovell N, Evans CJ, Higginson IJ, Murtagh FEM (2017) How many people will need palliative care in 2040? Past trends, future projections and implications for services. BMC Med 15:102
Vanbutsele G, Pardon K, Van Belle S, Surmont V, De Laat M, Colman R, Eecloo K, Cocquyt V, Geboes K, Deliens L (2018) Effect of early and systematic integration of palliative care in patients with advanced cancer: a randomised controlled trial. Lancet Oncol 19:394–404
Zimmermann C, Swami N, Krzyzanowska M, Hannon B, Leighl N, Oza A, Moore M, Rydall A, Rodin G, Tannock I, Donner A, Lo C (2014) Early palliative care for patients with advanced cancer: a cluster-randomised controlled trial. The Lancet 383:1721–1730
Bakitas MA, Tosteson TD, Li Z, Lyons KD, Hull JG, Li Z, Dionne-Odom JN, Frost J, Dragnev KH, Hegel MT, Azuero A, Ahles TA (2015) Early versus delayed initiation of concurrent palliative oncology care: patient outcomes in the ENABLE III randomized controlled trial. J Clin Oncol 33:1438–1445
Temel JS, Greer JA, Muzikansky A, Gallagher ER, Admane S, Jackson VA, Dahlin CM, Blinderman CD, Jacobsen J, Pirl WF (2010) Early palliative care for patients with metastatic non–small-cell lung cancer. New Engl J Med 363:733–742
Hui D, Bansal S, Strasser F, Morita T, Caraceni A, Davis M, Cherny N, Kaasa S, Currow D, Abernethy A (2015) Indicators of integration of oncology and palliative care programs: an international consensus. Ann Oncol 26:1953–1959
Kaasa S, Loge JH, Aapro M, Albreht T, Anderson R, Bruera E, Brunelli C, Caraceni A, Cervantes A, Currow DC (2018) Integration of oncology and palliative care: a Lancet Oncology Commission. Lancet Oncol 19:e588–e653
Boddaert MS, Pereira C, Adema J, Vissers KC, van der Linden YM, Raijmakers NJ, Fransen HP (2022) Inappropriate end-of-life cancer care in a generalist and specialist palliative care model: a nationwide retrospective population-based observational study. BMJ supportive & palliative care 12(e1):e137–e145
van der Padt-Pruijsten A, Leys MBL, Oomen-de Hoop E, van der Heide A, van der Rijt CCD (2021) Effects of implementation of a standardized palliative care pathway for patients with advanced cancer in a hospital: a prospective pre- and postintervention study. J Pain Symptom Manage 62:451–459
Groenewoud AS, Wichmann AB, Dijkstra L, Knapen E, Warmerdam F, De Weerdt-Spaetgens C, Dominicus W, Akkermans R, Meijers J (2021) Effects of an integrated palliative care pathway: more proactive GPs, well timed, and less acute care: a clustered, partially controlled before-after study. J Am Med Dir Assoc 22:297–304
Schuit AS, Holtmaat K, Lissenberg-Witte BI, Eerenstein SEJ, Zijlstra JM, Eeltink C, Becker-Commissaris A, van Zuylen L, van Linde ME, der Houven Menke-van, van Oordt CW, Sommeijer DW, Verbeek N, Bosscha K, Tewarie RN, Sedee R-J, de Bree R, de Graeff A, de Vos F, Cuijpers P, Verdonck-de Leeuw IM (2022) Efficacy of the eHealth application Oncokompas, facilitating incurably ill cancer patients to self-manage their palliative care needs: a randomized controlled trial. Lancet Reg Health - Europe 18
Stoppelenburg A, Arslan M, Owusuaa C, Gunnink N, van der Linden YM, Luelmo SA, van der Heide A (2022) The prognostic value of the 12-, 6-, 3-and 1-month ‘Surprise Question’in cancer patients: A prospective cohort study in three hospitals. Eur J Cancer Care 31(6):e13551
Junger S, Payne S, Brearley S, Ploenes V, Radbruch L (2012) Consensus building in palliative care: a Europe-wide delphi study on common understandings and conceptual differences. J Pain Symptom Manage 44:192–205
Junger S, Payne SA, Brine J, Radbruch L, Brearley SG (2017) Guidance on Conducting and REporting DElphi Studies (CREDES) in palliative care: recommendations based on a methodological systematic review. Palliat Med 31:684–706
Boddaert M, Douma J, Dijxhoorn F, Bijkerk M (2017) Netherlands quality framework for palliative care. IKNL/Palliactief
Walsh RI, Mitchell G, Francis L, van Driel ML (2015) What diagnostic tools exist for the early identification of palliative care patients in general practice? A systematic review. J Palliat Care 31:118–123
Boddaert MS, Stoppelenburg A, Hasselaar J, van der Linden YM, Vissers KCP, Raijmakers NJH, Brom L (2021) Specialist palliative care teams and characteristics related to referral rate: a national cross-sectional survey among hospitals in the Netherlands. BMC Palliat Care 20:175
Vogt J, Beyer F, Sistermanns J, Kuon J, Kahl C, Alt-Ep** B, Stevens S, Ahlborn M, George C, Heider A, Tienken M, Loquai C, Stahlhut K, Ruellan A, Kubin T, Dietz A, Oechsle K, Mehnert-Theuerkauf A, van Oorschot B, Thomas M, Ortmann O, Engel C, Lordick F, ArbeitsgemeinschaftPalliativmedizin of the German Cancer S (2021) Symptom burden and palliative care needs of patients with incurable cancer at diagnosis and during the disease course. Oncologist 26:e1058–e1065
Verkissen MN, Hjermstad MJ, Van Belle S, Kaasa S, Deliens L, Pardon K (2019) Quality of life and symptom intensity over time in people with cancer receiving palliative care: results from the international European Palliative Care Cancer Symptom study. PLoS ONE 14:e0222988
Beernaert K, Pardon K, Van den Block L, Devroey D, De Laat M, Geboes K, Surmont V, Deliens L, Cohen J (2016) Palliative care needs at different phases in the illness trajectory: a survey study in patients with cancer. Eur J Cancer Care (Engl) 25:534–543
Veldhoven CMM, Nutma N, De Graaf W, Schers H, Verhagen C, Vissers KCP, Engels Y (2019) Screening with the double surprise question to predict deterioration and death: an explorative study. BMC Palliat Care 18:118
Houben CHM, Spruit MA, Groenen MTJ, Wouters EFM, Janssen DJA (2014) Efficacy of advance care planning: a systematic review and meta-analysis. J Am Med Dir Assoc 15:477–489
Brinkman-Stoppelenburg A, Rietjens JA, Van der Heide A (2014) The effects of advance care planning on end-of-life care: a systematic review. Palliat Med 28:1000–1025
Schrijvers D, Cherny NI, Group EGW (2014) ESMO clinical practice guidelines on palliative care: advanced care planning. Ann Oncol 25(Suppl 3):iii138-142
Bestvina CM, Polite BN (2017) Implementation of advance care planning in oncology: a review of the literature. J Oncol Pract 13:657–662
Seifart C, Koch M, Leppin N, Nagelschmidt K, Knorrenschild JR, Timmesfeld N, Rief W, von Blanckenburg P (2020) Collaborative advance care planning in advanced cancer patients: col-ACP -study - study protocol of a randomised controlled trial. BMC Palliat Care 19:134
Ermers DJ, van Bussel KJ, Perry M, Engels Y, Schers HJ (2019) Advance care planning for patients with cancer in the palliative phase in Dutch general practices. Fam Pract 36:587–593
Chandar M, Brockstein B, Zunamon A, Silverman I, Dlouhy S, Ashlevitz K, Tabachow C, Lapin B, Ewigman B, Mazzone T, Obel J (2017) Perspectives of health-care providers toward advance care planning in patients with advanced cancer and congestive heart failure. Am J Hosp Palliat Care 34:423–429
Mack JW, Smith TJ (2012) Reasons why physicians do not have discussions about poor prognosis, why it matters, and what can be improved. J Clin Oncol 30:2715–2717
Agarwal R, Epstein AS (2018) Advance care planning and end-of-life decision making for patients with cancer. Semin Oncol Nurs 34:316–326
de Graaf E, Zweers D, de Graeff A, Stellato RK, Teunissen S (2018) Symptom intensity of hospice patients: a longitudinal analysis of concordance between patients’ and nurses’ outcomes. J Pain Symptom Manage 55:272–281
Hamer J, McDonald R, Zhang L, Verma S, Leahey A, Ecclestone C, Bedard G, Pulenzas N, Bhatia A, Chow R, DeAngelis C, Ellis J, Rakovitch E, Lee J, Chow E (2017) Quality of life (QOL) and symptom burden (SB) in patients with breast cancer. Supp Care Cancer 25:409–419
Deshields TL, Potter P, Olsen S, Liu J (2014) The persistence of symptom burden: symptom experience and quality of life of cancer patients across one year. Support Care Cancer 22:1089–1096
Basch E, Deal AM, Kris MG, Scher HI, Hudis CA, Sabbatini P, Rogak L, Bennett AV, Dueck AC, Atkinson TM, Chou JF, Dulko D, Sit L, Barz A, Novotny P, Fruscione M, Sloan JA, Schrag D (2016) Symptom monitoring with patient-reported outcomes during routine cancer treatment: a randomized controlled trial. J Clin Oncol 34:557–565
Antunes B, Harding R, Higginson IJ, Euroimpact (2014) Implementing patient-reported outcome measures in palliative care clinical practice: a systematic review of facilitators and barriers. Palliat Med 28:158–175
de Vries S, Lormans T, de Graaf E, Leget C, Teunissen S (2021) the content validity of the items related to the social and spiritual dimensions of the Utrecht symptom diary-4 dimensional from a patient’s perspective: a qualitative study. J Pain Symptom Manage 61:287-294.e282
Hui D, Bruera E (2017) The Edmonton Symptom Assessment System 25 years later: past, present, and future developments. J Pain Symptom Manage 53:630–643
Raijmakers NJH, Zijlstra M, van Roij J, Husson O, Oerlemans S, van de Poll-Franse LV (2018) Health-related quality of life among cancer patients in their last year of life: results from the PROFILES registry. Support Care Cancer 26:3397–3404
Grant M, de Graaf E, Teunissen S (2021) A systematic review of classifications systems to determine complexity of patient care needs in palliative care. Palliat Med 35:636–650
Cherny NI, Catane R, European Society of Medical Oncology Taskforce on P, Supportive C (2003) Attitudes of medical oncologists toward palliative care for patients with advanced and incurable cancer: report on a survery by the European Society of Medical Oncology Taskforce on Palliative and Supportive Care. Cancer 98:2502–2510
Quill TE, Abernethy AP (2013) Generalist plus specialist palliative care—creating a more sustainable model. New Engl J Med 368:1173–1175
Hui D, Bruera E (2015) Models of integration of oncology and palliative care Ann. Palliat Med 4:89–98
Hui D, Mori M, Meng Y-C, Watanabe SM, Caraceni A, Strasser F, Saarto T, Cherny N, Glare P, Kaasa S (2018) Automatic referral to standardize palliative care access: an international Delphi survey. Support Care Cancer 26:175–180
Funding
This work was supported by the Maarten van der Weijden Foundation.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. CH, NR and LB conducted the data collection and analysis. YL, DR and AR contributed to the interpretation. CH drafted the manuscript. All authors were involved in the critical revision of the manuscript and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Ethics approval
This study was carried out in line with the principles of the Declaration of Helsinki. The Medical Ethics Committee of Brabant (METC NW2021-71) assessed the study and granted it exemption from full approval of an ethics committee due to the fact that there was no invasive intervention nor were there vulnerable patients involved (CCMO, 2020).
Consent to participate
Informed consent was obtained from all panellists included in the study.
Consent for publication
N/a.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Heipon, C.S., Brom, L., van der Linden, Y.M. et al. Characteristics of timely integration of palliative care into oncology hospital care for patients with incurable cancer: results of a Delphi Study. Support Care Cancer 32, 324 (2024). https://doi.org/10.1007/s00520-024-08508-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00520-024-08508-0