Abstract
Purpose
Following head and neck cancer (HNC) treatment, individuals experience an array of side effects which can impact on physical, emotional, and practical aspects of their lives. Responsive, supportive rehabilitation services are therefore essential to address ongoing survivorship needs. This study examined the nature of patient-reported goals from acute to long-term post-treatment, to inform design/delivery of future rehabilitation services.
Methods
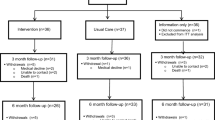
Using a cross-sectional cohort design, 91 patients between 2 weeks and 5 years of post non-surgical HNC treatment (acute n = 29; sub-acute n = 28; long-term n = 34), provided their top four rehabilitation goals considering any aspect of their lives. Content analysis was used to categorise responses at each time point.
Results
Three core categories of patient goals were identified relating to: (1) treatment side effects (TSE), (2) overall health (OH), and (3) living life (LL). TSE goals were a priority during the acute and sub-acute phases, with less focus long-term. LL goals were prevalent across all time points, though increased in the long-term. Approximately a third of all goals at each time point related to OH.
Conclusions
A variety of rehabilitation goals were identified, and the focus shifted over time. These data highlight the importance of changing the focus of rehabilitation as patients’ priorities vary over time. Early multidisciplinary care from allied health services is crucial to provide support with managing side effects and returning to daily activities. In the long-term, greater input from services to address health, nutrition, leisure, and fitness goals may be more beneficial.

Similar content being viewed by others
References
Dirix P, Nuyts S (2010) Evidence-based organ-sparing radiotherapy in head and neck cancer. Lancet Oncol 11(1):85–91. https://doi.org/10.1016/S1470-2045(09)70231-1
Ang KK, Harris J, Wheeler R, Weber R, Rosenthal DI, Nguyen-Tân PF, Westra WH, Chung CH, Jordan RC, Lu C, Kim H, Axelrod R, Silverman CC, Redmond KP, Gillison ML (2010) Human papillomavirus and survival of patients with oropharyngeal cancer. N Engl J Med 363(1):24–35. https://doi.org/10.1056/NEJMoa0912217
Beadle BM, Liao K-P, Elting LS, Buchholz TA, Ang KK, Garden AS, Guadagnolo BA (2014) Improved survival using intensity-modulated radiation therapy in head and neck cancers: a SEER-Medicare analysis. Cancer 120(5):702–710. https://doi.org/10.1002/cncr.28372
Miller MC, Shuman AG, for the American H, Neck Society’s Committee on S (2016) Survivorship in head and neck cancer: a primer. JAMA Otolaryngo Head Neck Surg 142(10):1002–1008. https://doi.org/10.1001/jamaoto.2016.1615
Ghazali N, Roe B, Lowe D, Rogers SN (2015) Patients concerns inventory highlights perceived needs and concerns in head and neck cancer survivors and its impact on health-related quality of life. Br J Oral Maxillofac Surg 53(4):371–379. https://doi.org/10.1016/j.bjoms.2015.01.022
Cohen EEW, LaMonte SJ, Erb NL, Beckman KL, Sadeghi N, Hutcheson KA, Stubblefield MD, Abbott DM, Fisher PS, Stein KD, Lyman GH, Pratt-Chapman ML (2016) American Cancer Society head and neck cancer survivorship care guideline. CA Cancer J Clin 66(3):203–239. https://doi.org/10.3322/caac.21343
Barnhart MK, Robinson RA, Simms VA, Ward EC, Cartmill B, Chandler SJ, Smee RI (2018) Treatment toxicities and their impact on oral intake following non-surgical management for head and neck cancer: a 3-year longitudinal study. Support Care Cancer 26:2341–2351. https://doi.org/10.1007/s00520-018-4076-6
Ringash J, Bernstein LJ, Devins G, Dunphy C, Giuliani M, Martino R, McEwen S (2018) Head and neck cancer survivorship: learning the needs, meeting the needs. Semin Radiat Oncol 28(1):64–74. https://doi.org/10.1016/j.semradonc.2017.08.008
Giuliani M, McQuestion M, Jones J, Papadakos J, Le LW, Alkazaz N, Cheng T, Waldron J, Catton P, Ringash J (2016) Prevalence and nature of survivorship needs in patients with head and neck cancer. Head Neck 38(7):1097–1103. https://doi.org/10.1002/hed.24411
Bressan V, Bagnasco A, Aleo G, Catania G, Zanini MP, Timmins F, Sasso L (2017) The life experience of nutrition impact symptoms during treatment for head and neck cancer patients: a systematic review and meta-synthesis. Support Care Cancer 25(5):1699–1712. https://doi.org/10.1007/s00520-017-3618-7
Murphy BA, Beaumont JL, Isitt J, Garden AS, Gwede CK, Trotti AM, Meredith RF, Epstein JB, Le QT, Brizel DM, Bellm LA, Wells N, Cella D (2009) Mucositis-related morbidity and resource utilization in head and neck cancer patients receiving radiation therapy with or without chemotherapy. J Pain Symptom Manag 38(4):522–532. https://doi.org/10.1016/j.jpainsymman.2008.12.004
Pauloski, Rademaker AW, Logemann JA, Lundy D, Bernstein M, McBreen C, Santa D, Campanelli A, Kelchner L, Klaben B, Discekici-Harris M (2011) Relation of mucous membrane alterations to oral intake during the first year after treatment for head and neck cancer. Head Neck 33(6):774–779. https://doi.org/10.1002/hed.21542
McLaughlin LRNP (2013) Taste dysfunction in head and neck cancer survivors. Oncol Nurs Forum 40(1):E4–E13
Kraaijenga SC, van der Molen L, Jacobi I, Hamming-Vrieze O, Hilgers FM, van den Brekel MM (2015) Prospective clinical study on long-term swallowing function and voice quality in advanced head and neck cancer patients treated with concurrent chemoradiotherapy and preventive swallowing exercises. Eur Arch Otorhinolaryngol 272(11):3521–3531. https://doi.org/10.1007/s00405-014-3379-6
Vainshtein JM, Samuels S, Tao Y, Lyden T, Haxer M, Spector M, Schipper M, Eisbruch A (2016) Impact of xerostomia on dysphagia after chemotherapy–intensity-modulated radiotherapy for oropharyngeal cancer: prospective longitudinal study. Head Neck 38(S1):E1605–E1612. https://doi.org/10.1002/hed.24286
Bressan V, Stevanin S, Bianchi M, Aleo G, Bagnasco A, Sasso L (2016) The effects of swallowing disorders, dysgeusia, oral mucositis and xerostomia on nutritional status, oral intake and weight loss in head and neck cancer patients: a systematic review. Cancer Treat Rev 45:105–119. https://doi.org/10.1016/j.ctrv.2016.03.006
Molassiotis A, Rogers M (2012) Symptom experience and regaining normality in the first year following a diagnosis of head and neck cancer: a qualitative longitudinal study. Palliat Support Care 10(3):197–204. https://doi.org/10.1017/S147895151200020X 10.1016/j.critrevonc.2006.07.005
Larsson M, Hedelin B, Athlin E (2007) Needing a hand to hold: lived experiences during the trajectory of care for patients with head and neck cancer treated with radiotherapy. Cancer Nurs 30(4):324–334. https://doi.org/10.1097/01.ncc.0000281722.56996.07
Holm LV, Hansen DG, Johansen C, Vedsted P, Larsen PV, Kragstrup J, Søndergaard J (2012) Participation in cancer rehabilitation and unmet needs: a population-based cohort study. Support Care Cancer 20(11):2913–2924. https://doi.org/10.1007/s00520-012-1420-0
Jefford M, Karahalios E, Pollard A, Baravelli C, Carey M, Franklin J, Aranda S, Schofield P (2008) Survivorship issues following treatment completion—results from focus groups with Australian cancer survivors and health professionals. J Cancer Surviv 2(1):20–32. https://doi.org/10.1007/s11764-008-0043-4
Passchier E, Stuiver MM, van der Molen L, Kerkhof SI, van den Brekel MW, Hilgers FJ (2016) Feasibility and impact of a dedicated multidisciplinary rehabilitation program on health-related quality of life in advanced head and neck cancer patients. Eur Arch Otorhinolaryngol 273(6):1577–1587. https://doi.org/10.1007/s00405-015-3648-z
Eades M, Murphy J, Carney S, Amdouni S, Lemoignan J, Jelowicki M (2013) Effect of an interdisciplinary rehabilitation program on quality of life in patients with head and neck cancer: review of clinical experience. Head Neck 35:343–349. https://doi.org/10.1002/hed.22972
McEwen S, Rodriguez AM, Martino R, Poon I, Dunphy C, Rios JN, Ringash J (2016) “I didn’t actually know there was such a thing as rehab”: survivor, family, and clinician perceptions of rehabilitation following treatment for head and neck cancer. Support Care Cancer 24(4):1449–1453. https://doi.org/10.1007/s00520-015-3021-1
Cancer Australia and Cancer Voices Australia (2011) National framework for consumer involvement in cancer control. Cancer Australia. ACT, Canberra
Tschiesner U, Sabariego C, Linseisen E, Becker S, Stier-Jarmer M, Cieza A, Harreus U (2013) Priorities of head and neck cancer patients: a patient survey based on the brief ICF core set for HNC. Eur Arch Otorhinolaryngol 270(12):3133–3142. https://doi.org/10.1007/s00405-013-2446-8
Kanatas A, Ghazali N, Lowe D, Udberg M, Heseltine J, O’Mahony E, Rogers SN (2013) Issues patients would like to discuss at their review consultation: variation by early and late stage oral, oropharyngeal and laryngeal subsites. Eur Arch Otorhinolaryngol 270(3):1067–1074. https://doi.org/10.1007/s00405-012-2092-6
Metcalfe CW, Lowe D, Rogers SN (2014) What patients consider important: temporal variations by early and late stage oral, oropharyngeal and laryngeal subsites. J Cranio-Maxillofac Surg 42(5):641–647. https://doi.org/10.1016/j.jcms.2013.09.008
Rogers SN, El-Sheikha J, Lowe D (2009) The development of a Patients Concerns Inventory (PCI) to help reveal patients concerns in the head and neck clinic. Oral Oncol 45(7):555–561. https://doi.org/10.1016/j.oraloncology.2008.09.004
Sharp HM, List M, MacCracken E, Stenson K, Stocking C, Siegler M (1999) Patients’ priorities among treatment effects in head and neck cancer: evaluation of a new assessment tool. Head Neck 21(6):538–546
Rogers SN, Laher SH, Overend L, Lowe D (2002) Importance-rating using the University of Washington Quality of Life questionnaire in patients treated by primary surgery for oral and oro-pharyngeal cancer. J Cranio-Maxillofac Surg 30(2):125–132. https://doi.org/10.1054/jcms.2001.0273
Clinical Oncology Society of Australia Model of Survivorship Care Working Group (2016) Model of survivorship care: critical components of cancer survivorship care in Australia position statement. Clinical Oncology Society of Australia
Bodenheimer T, Lorig K, Holman H, Grumbach K (2002) Patient self-management of chronic disease in primary care. JAMA 288(19):2469–2475
Cartmill B, Cornwell P, Ward E, Davidson W, Porceddu S (2012) Long-term functional outcomes and patient perspective following altered fractionation radiotherapy with concomitant boost for oropharyngeal cancer. Dysphagia 27(4):481–490. https://doi.org/10.1007/s00455-012-9394-0
Cooperstein E, Gilbert J, Epstein JB, Dietrich MS, Bond SM, Ridner SH, Wells N, Cmelak A, Murphy BA (2012) Vanderbilt head and neck symptom survey version 2.0: report of the development and initial testing of a subscale for assessment of oral health. Head Neck 34(6):797–804. https://doi.org/10.1002/hed.21816
Ganzer H, Rothpletz-Puglia P, Byham-Gray L, Murphy BA, Touger-Decker R (2015) The eating experience in long-term survivors of head and neck cancer: a mixed-methods study. Support Care Cancer 23(11):3257–3268. https://doi.org/10.1007/s00520-015-2730-9
Hutcheson KA, Lewin JS, Holsinger FC, Steinhaus G, Lisec A, Barringer DA, Lin HY, Villalobos S, Garden AS, Papadimitrakopoulou V, Kies MS (2014) Long-term functional and survival outcomes after induction chemotherapy and risk-based definitive therapy for locally advanced squamous cell carcinoma of the head and neck. Head Neck 36(4):474–480. https://doi.org/10.1002/hed.23330
Graneheim UH, Lundman B (2004) Qualitative content analysis in nursing research: concepts, procedures and measures to achieve trustworthiness. Nurse Educ Today 24(2):105–112. https://doi.org/10.1016/j.nedt.2003.10.001
Nund WEC, Scarinci NA, Cartmill B, Kuipers P, Porceddu SV (2014) The lived experience of dysphagia following non-surgical treatment for head and neck cancer. Int J Speech Lang Pathol 16(3):282–289. https://doi.org/10.3109/17549507.2013.861869
Semple CJ, Dunwoody L, George Kernohan W, McCaughan E, Sullivan K (2008) Changes and challenges to patients’ lifestyle patterns following treatment for head and neck cancer. J Adv Nurs 63(1):85–93. https://doi.org/10.1111/j.1365-2648.2008.04698.x
de Ridder D, Geenen R, Kuijer R, van Middendorp H (2008) Psychological adjustment to chronic disease. Lancet 372(9634):246–255. https://doi.org/10.1016/S0140-6736(08)61078-8
McEwen S, Dunphy C, Rios JN, Davis A, Jones J, Lam A, Poon I, Martino R, Ringash J (2017) Development and pre-testing of a rehabilitation planning consultation for head-and-neck cancer. 24(3):8. https://doi.org/10.3747/co.24.3529
Hodgkinson K, Butow P, Hunt GE et al (2007) The development and evaluation of a measure to assess cancer survivors’ unmet supportive care needs: the CaSUN (Cancer Survivors’ Unmet Needs measure). Psychooncology 16:796–804. https://doi.org/10.1002/pon.1137
Acknowledgements
The authors wish to thank the speech pathology department, research team, and multidisciplinary team at Prince of Wales Hospital and Princess Alexandra Hospital for their contributions and continued support to this project.
Funding
This project was funded by the Head and Neck Cancer Research Fund at Prince of Wales Hospital, Sydney, Australia.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author has been funded by the institution (Prince of Wales Hospital, Australia) where the research was conducted. The author has full control of all primary data and agrees to allow the journal to review the data if requested.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Barnhart, M.K., Ward, E.C., Cartmill, B. et al. Content analysis of rehabilitation goals for patients following non-surgical head and neck cancer treatment. Support Care Cancer 27, 639–647 (2019). https://doi.org/10.1007/s00520-018-4364-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-018-4364-1