Abstract
Introduction
Meta-analysis of the results of transanal total mesorectal excision (taTME) and laparoscopic TME (laTME) regarding perioperative and oncological outcomes have been conducted. Due to the lack of high-quality randomized controlled trials (RCTs) and prospective studies in the included literature, the conclusions are unreliable. This study included RCTs and prospective studies for analysis to obtain more reliable conclusions.
Materials and methods
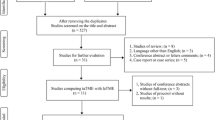
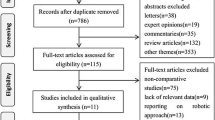
Systematic searches of the PubMed, Embase, and Cochrane Library databases were conducted up to June 2023. To assess the quality, the Cochrane quality assessment tool and the Newcastle–Ottawa Scale were employed. The perioperative and oncological outcomes were then analyzed. The I2 statistic was used to evaluate statistical heterogeneity and sensitivity analyses was conducted.
Results
A total of 22 studies, comprising 5056 patients, were included in the analysis, of which 6 were RCTs and 16 were prospective studies. The conversion rate in the taTME group was significantly lower than that in the laTME group (OR 0.14, 95% CI 0.09 to 0.22, P < 0.01), and the circumferential resection margin (CRM) was longer (MD 0.99 mm, 95% CI 0.66 to 1.32 mm, P < 0.01), with a lower rate of positive CRM involvement (OR 0.68, 95% CI 0.47 to 0.97, P = 0.03). No statistically significant differences were found in terms of the operation time, intraoperative blood loss, complications, anastomotic leakage, uroschesis, obstruction, secondary operation, hospital stay, urethral injury, readmission, mortality rate within 30 days, mesorectal resection quality, number of harvested lymph nodes, distal resection margin (DRM), positive DRM, local recurrence, and distance recurrence (P > 0.05).
Conclusion
According to the findings of this meta-analysis, which is based on RCTs and prospective studies, taTME appears to have an advantage over laTME in terms of conversion rate and CRM involvement.
Graphical abstract









Similar content being viewed by others
Data availability
With the publication, the data set used for this meta-analysis will be shared upon request from the study authors.
References
Siegel RL, Miller KD, Wagle NS, Jemal A (2023) Cancer statistics, 2023. CA Cancer J Clin 73:17–48
Brouwer NPM, Bos A, Lemmens V, Tanis PJ, Hugen N, Nagtegaal ID, de Wilt JHW, Verhoeven RHA (2018) An overview of 25 years of incidence, treatment and outcome of colorectal cancer patients. Int J Cancer 143:2758–2766
Sylla P, Rattner DW, Delgado S, Lacy AM (2010) NOTES transanal rectal cancer resection using transanal endoscopic microsurgery and laparoscopic assistance. Surg Endosc 24:1205–1210
Larsen SG, Pfeffer F, Kørner H (2019) Norwegian moratorium on transanal total mesorectal excision. Br J Surg 106:1120–1121
Roodbeen SX, Penna M, van Dieren S, Moran B, Tekkis P, Tanis PJ, Hompes R (2021) Local recurrence and disease-free survival after transanal total mesorectal excision: results from the international TaTME registry. J Natl Compr Cancer Netw 19:1232–1240
Rubinkiewicz M, Czerwińska A, Zarzycki P, Małczak P, Nowakowski M, Major P, Budzyński A, Pędziwiatr M (2018) Comparison of short-term clinical and pathological outcomes after transanal versus laparoscopic total mesorectal excision for low anterior rectal resection due to rectal cancer: a systematic review with meta-analysis. J Clin Med 7:448
Ren J, Luo H, Liu S, Wang B, Wu F (2021) Short- and mid-term outcomes of transanal versus laparoscopic total mesorectal excision for low rectal cancer: a meta-analysis. Ann Surg Treat Res 100:86–99
Perdawood SK, Thinggaard BS, Bjoern MX (2018) Effect of transanal total mesorectal excision for rectal cancer: comparison of short-term outcomes with laparoscopic and open surgeries. Surg Endosc 32:2312–2321
Aubert M, Mege D, Panis Y (2020) Total mesorectal excision for low and middle rectal cancer: laparoscopic versus transanal approach—a meta-analysis. Surg Endosc 34:3908–3919
Moon JY, Lee MR, Ha GW (2022) Long-term oncologic outcomes of transanal TME compared with transabdominal TME for rectal cancer: a systematic review and meta-analysis. Surg Endosc 36:3122–3135
Li L, Wang T, Hu D, Wu D, Bi L, Luo Y, Guo Y, Yang X (2022) Pathologic outcomes of transanal versus laparoscopic total mesorectal excision for rectal cancer: a meta-analysis of 26 studies. Int J Colorectal Dis 37:1063–1071
Jiang HP, Li YS, Wang B, Wang C, Liu F, Shen ZL, Ye YJ, Wang S (2018) Pathological outcomes of transanal versus laparoscopic total mesorectal excision for rectal cancer: a systematic review with meta-analysis. Surg Endosc 32:2632–2642
Kwon SH, Joo YI, Kim SH, Lee DH, Baek JH, Chung SS, Shin JY, Eun CS, Kim NK (2021) Meta-analysis of transanal versus laparoscopic total mesorectal excision for rectal cancer: a ‘New Health Technology’ assessment in South Korea. Ann Surg Treat Res 101:167–180
Zhang X, Gao Y, Dai X, Zhang H, Shang Z, Cai X, Shen T, Cheng X, Yu K, Li Y (2019) Short- and long-term outcomes of transanal versus laparoscopic total mesorectal excision for mid-to-low rectal cancer: a meta-analysis. Surg Endosc 33:972–985
Liu H, Zeng Z, Zhang H, Wu M, Ma D, Wang Q, **e M, Xu Q, Ouyang J, **ao Y, Song Y, Feng B, Xu Q, Wang Y, Zhang Y, Hao Y, Luo S, Zhang X, Yang Z, Peng J, Wu X, Ren D, Huang M, Lan P, Tong W, Ren M, Wang J, Kang L (2023) Morbidity, mortality, and pathologic outcomes of transanal versus laparoscopic total mesorectal excision for rectal cancer short-term outcomes from a multicenter randomized controlled trial. Ann Surg 277:1–6
Serra-Aracil X, Zarate A, Bargalló J, Gonzalez A, Serracant A, Roura J, Delgado S, Mora-López L (2023) Transanal versus laparoscopic total mesorectal excision for mid and low rectal cancer (Ta-LaTME study): multicentre, randomized, open-label trial. Br J Surg 110:150–158
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, Shamseer L, Tetzlaff JM, Akl EA, Brennan SE, Chou R, Glanville J, Grimshaw JM, Hróbjartsson A, Lalu MM, Li T, Loder EW, Mayo-Wilson E, McDonald S, McGuinness LA, Stewart LA, Thomas J, Tricco AC, Welch VA, Whiting P, Moher D (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:n71
Wells G (2014) The Newcastle-Ottawa Scale (NOS) for assessing the quality of non-randomised studies in meta-analyses. In: Symposium on systematic reviews: beyond the basics, Oxford, UK, 3–5 July 2000
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560
Hozo SP, Djulbegovic B, Hozo I (2005) Estimating the mean and variance from the median, range, and the size of a sample. BMC Med Res Methodol 5:13
Denost Q, Loughlin P, Chevalier R, Celerier B, Didailler R, Rullier E (2018) Transanal versus abdominal low rectal dissection for rectal cancer: long-term results of the Bordeaux’ randomized trial. Surg Endosc 32:1486–1494
Fernández-Hevia M, Delgado S, Castells A, Tasende M, Momblan D, Díaz del Gobbo G, DeLacy B, Balust J, Lacy AM (2015) Transanal total mesorectal excision in rectal cancer: short-term outcomes in comparison with laparoscopic surgery. Ann Surg 261:221–227
Gordeyev SS, Dzhumabaev KE, Mamedli ZZ, Kozlov NA, Surayeva YE, Fedyanin MY, Rasulov AOJES (2018) Transanal total mesorectal excision in selected patients with “difficult pelvis”: a case–control study of “difficult” rectal cancer patients. Eur Surg 51:13–18
Lelong B, Meillat H, Zemmour C, Poizat F, Ewald J, Mege D, Lelong JC, Delpero JR, de Chaisemartin C (2017) Short- and mid-term outcomes after endoscopic transanal or laparoscopic transabdominal total mesorectal excision for low rectal cancer: a single institutional case-control study. J Am Coll Surg 224:917–925
Mege D, Hain E, Lakkis Z, Maggiori L, Prost À la Denise J, Panis Y (2018) Is trans-anal total mesorectal excision really safe and better than laparoscopic total mesorectal excision with a perineal approach first in patients with low rectal cancer? A learning curve with case-matched study in 68 patients. Colorectal Dis 20:O143–O151
Perdawood SK, Al Khefagie GA (2016) Transanal vs laparoscopic total mesorectal excision for rectal cancer: initial experience from Denmark. Colorectal Dis 18:51–58
Rasulov AO, Mamedli ZZ, Gordeyev SS, Kozlov NA, Dzhumabaev HE (2016) Short-term outcomes after transanal and laparoscopic total mesorectal excision for rectal cancer. Tech Coloproctol 20:227–234
Ren J, Liu S, Luo H, Wang B, Wu F (2021) Comparison of short-term efficacy of transanal total mesorectal excision and laparoscopic total mesorectal excision in low rectal cancer. Asian J Surg 44:181–185
Rubinkiewicz M, Zarzycki P, Witowski J, Pisarska M, Gajewska N, Torbicz G, Nowakowski M, Major P, Budzyński A, Pędziwiatr M (2019) Functional outcomes after resections for low rectal tumors: comparison of transanal with laparoscopic total mesorectal excision. BMC Surg 19:79
Sparreboom CL, Komen N, Rizopoulos D, van Westreenen HL, Doornebosch PG, Dekker JWT, Menon AG, Tuynman JB, Daams F, Lips D, van Grevenstein WMU, Karsten TM, Lange JF, D’Hoore A, Wolthuis AM (2019) Transanal total mesorectal excision: how are we doing so far? Colorectal Dis 21:767–774
Sun R, Cong L, Qiu HZ, Lin GL, Wu B, Niu BZ, Sun XY, Zhou JL, Xu L, Lu JY, **ao Y (2022) Safety and prognosis analysis of transanal total mesorectal excision versus laparoscopic mesorectal excision for mid-low rectal cancer. Zhonghua Wei Chang Wai Ke Za Zhi 25:522–530
Zeng Z, Luo S, Chen J, Cai Y, Zhang X, Kang L (2020) Comparison of pathological outcomes after transanal versus laparoscopic total mesorectal excision: a prospective study using data from randomized control trial. Surg Endosc 34:3956–3962
Zuhdy M, Elmore U, Shams N, Hegazy MAF, Roshdy S, Eldamshety O, Metwally IH, Rosati R (2020) Transanal versus laparoscopic total mesorectal excision: a comparative prospective clinical trial from two centers. J Laparoendosc Adv Surg Tech A 30:769–776
Pontallier A, Denost Q, Van Geluwe B, Adam JP, Celerier B, Rullier E (2016) Potential sexual function improvement by using transanal mesorectal approach for laparoscopic low rectal cancer excision. Surg Endosc 30:4924–4933
Roodbeen SX, Penna M, Mackenzie H, Kusters M, Slater A, Jones OM, Lindsey I, Guy RJ, Cunningham C, Hompes R (2019) Transanal total mesorectal excision (TaTME) versus laparoscopic TME for MRI-defined low rectal cancer: a propensity score-matched analysis of oncological outcomes. Surg Endosc 33:2459–2467
Ose I, Perdawood SK (2021) A nationwide comparison of short-term outcomes after transanal, open, laparoscopic, and robot-assisted total mesorectal excision. Colorectal Dis 23:2671–2680
Detering R, Roodbeen SX, van Oostendorp SE, Dekker JT, Sietses C, Bemelman WA, Tanis PJ, Hompes R, Tuynman JB (2019) Three-year nationwide experience with transanal total mesorectal excision for rectal cancer in the Netherlands: a propensity score-matched comparison with conventional laparoscopic total mesorectal excision. J Am Coll Surg 228:235–244.e231
Li Y, Bai X, Niu B, Zhou J, Qiu H, **ao Y, Lin G (2021) A prospective study of health related quality of life, bowel and sexual function after TaTME and conventional laparoscopic TME for mid and low rectal cancer. Tech Coloproctol 25:449–459
Bjoern MX, Clausen FB, Seiersen M, Bulut O, Bech-Knudsen F, Jansen JE, Gögenur I, Klein MF (2022) Quality of life and functional outcomes after transanal total mesorectal excision for rectal cancer-results from the implementation period in Denmark. Int J Colorectal Dis 37:1997–2011
Kneist W, Aigner F (2015) Total mesorectal excision via transanal minimally invasive surgery. An alternative technique. Coloproctology 37:253–261
Bhattacharya P, Patel I, Fazili N, Hajibandeh S, Hajibandeh S (2022) Meta-analysis of transanal vs laparoscopic total mesorectal excision of low rectal cancer: importance of appropriate patient selection. World J Gastrointest Surg 14:1397–1410
Lei P, Ruan Y, Yang X, Fang J, Chen T (2018) Trans-anal or trans-abdominal total mesorectal excision? A systematic review and meta-analysis of recent comparative studies on perioperative outcomes and pathological result. Int J Surg (London, Engl) 60:113–119
group ESoCEc (2018) An international multicentre prospective audit of elective rectal cancer surgery; operative approach versus outcome, including transanal total mesorectal excision (TaTME). Colorectal Dis 20(Suppl 6):33–46
Hgm VDP, Martijn, Haglind E, Cuesta MA, Fürst A, Lacy AM, Hop WC, Bonjer HJJLO (2013) Laparoscopic versus open surgery for rectal cancer (COLOR II): short-term outcomes of a randomised, phase 3 trial. Lancet Oncol 14:210–218
Guillou PJ, Quirke P, Thorpe H, Walker J, Jayne DG, Smith AM, Heath RM, Brown JM, Group MCTJL (2005) Short-term endpoints of conventional versus laparoscopic-assisted surgery in patients with colorectal cancer (MRC CLASICC trial): multicentre, randomised controlled trial. The Lancet 365:1718–1726
Thorpe H, Jayne DG, Guillou PJ, Quirke P, Copeland J, Brown JM (2008) Patient factors influencing conversion from laparoscopically assisted to open surgery for colorectal cancer. Br J Surg 95:199–205
Pandya S, Murray JJ, Coller JA, Rusin LC (1999) Laparoscopic colectomy: indications for conversion to laparotomy. Arch Surg (Chicago, IL: 1960) 134:471–475
Hajibandeh S, Hajibandeh S, Eltair M, George AT, Thumbe V, Torrance AW, Budhoo M, Joy H, Peravali R (2020) Meta-analysis of transanal total mesorectal excision versus laparoscopic total mesorectal excision in management of rectal cancer. Int J Colorectal Dis 35:575–593
Nagtegaal ID, Quirke P (2008) What is the role for the circumferential margin in the modern treatment of rectal cancer? J Clin Oncol 26:303–312
Birbeck KF, Macklin CP, Tiffin NJ, Parsons W, Dixon MF, Mapstone NP, Abbott CR, Scott N, Finan PJ, Johnston D, Quirke P (2002) Rates of circumferential resection margin involvement vary between surgeons and predict outcomes in rectal cancer surgery. Ann Surg 235:449–457
Bonjer HJ, Deijen CL, Abis GA, Cuesta MA, van der Pas MH, de Lange-de Klerk ES, Lacy AM, Bemelman WA, Andersson J, Angenete E, Rosenberg J, Fuerst A, Haglind E (2015) A randomized trial of laparoscopic versus open surgery for rectal cancer. N Engl J Med 372:1324–1332
Quirke P, Steele R, Monson J, Grieve R, Khanna S, Couture J, O’Callaghan C, Myint AS, Bessell E, Thompson LC, Parmar M, Stephens RJ, Sebag-Montefiore D (2009) Effect of the plane of surgery achieved on local recurrence in patients with operable rectal cancer: a prospective study using data from the MRC CR07 and NCIC-CTG CO16 randomised clinical trial. Lancet (London, Engl) 373:821–828
Marks JH, Montenegro GA, Salem JF, Shields MV, Marks GJ (2016) Transanal TATA/TME: a case-matched study of taTME versus laparoscopic TME surgery for rectal cancer. Tech Coloproctol 20:467–473
Acknowledgements
None
Funding
This work was supported by the Clinical Medical Technology Innovation Guidance Project of Hunan Provincial Science and Technology Department (No. 2018SK51609) and the Natural Science Foundation of Hunan Province (No. 2021JJ70118).
Author information
Authors and Affiliations
Contributions
Study concepts and design: XY, JO. Literature search: XY, XZ. Data extraction: XY, XZ, QL. Data analysis: XY, XZ. Manuscript preparation: XY, XZ. Critical revision: JO. All authors have participated sufficiently in the study and approved the final version.
Corresponding author
Ethics declarations
Disclosures
**anhao Yi, Xuan Zhang, Qingchun Li, Jun Ouyang have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
464_2023_10495_MOESM1_ESM.tiff
Supplementary file1 (TIFF 211 kb) Figure S1. Risk of bias in randomized controlled trials sutdies. (A) Risks of bias across all included randomized controlled trials, (B) summary of risks of bias for the different domains.
464_2023_10495_MOESM2_ESM.tiff
Supplementary file2 (TIFF 548 kb) Figure S2. Sensitivity analysis by omitt single study. (A) operation time, (B) intraoperative blood loss, (C) complications.
464_2023_10495_MOESM3_ESM.tiff
Supplementary file3 (TIFF 431 kb) Figure S3. Sensitivity analysis by omitt single study. (A) hospital stay, (B) readmission.
464_2023_10495_MOESM4_ESM.tiff
Supplementary file4 (TIFF 386 kb) Figure S4. Funnel plots and Egger’s test. (A) operation time, (B) intraoperative blood loss, (C) conversion, (D) complications, (E) anastomotic leakage, (F) uroschesis, (G) obstruction, (H) secondary operation, (I) hospital stay, (J) urethral injury.
464_2023_10495_MOESM5_ESM.tiff
Supplementary file5 (TIFF 387 kb) Figure S5. Funnel plots and Egger’s test. (A) readmission, (B) mortality rate within 30 days, (C) mesorectal resection quality, (D) number of harvested lymph nodes, (E) DRM, (F) positive DRM, (G) CRM, (H) positive CRM, (I) local recurrence, (J) distance recurrence.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yi, X., Zhang, X., Li, Q. et al. Comparing perioperative and oncological outcomes of transanal and laparoscopic total mesorectal excision for rectal cancer: a meta-analysis of randomized controlled trials and prospective studies. Surg Endosc 37, 9228–9243 (2023). https://doi.org/10.1007/s00464-023-10495-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-10495-y