Abstract
Background
Endoscopic submucosal dissection (ESD) is an alternative to surgical resection for treating early gastric cancer (EGC). However, there have been limited reports on the long-term outcome of ESD compared to that of surgical resection. The aim of this study was to evaluate the immediate and long-term clinical and oncologic outcomes of ESD compared to surgical resection.
Method
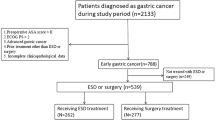
We retrospectively reviewed data of patients in five centers who were treated with ESD or surgical resection for EGC within expanded criteria for ESD from 2006 to 2008.
Result
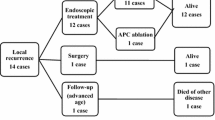
ESD group had significantly shorter procedure times, shorter fasting period, and shorter hospital stay than the surgical resection group. Immediate complications in the surgical resection group were more common compared to those in the ESD group. Five-year cancer recurrence rate of the ESD group was 12.3 % and significantly higher than 2.1 % of the surgical resection group (P = 0.001). Five-year disease-free survival rate of the surgical resection group was 97 %, which was significantly higher than 85 % of the ESD group (P = 0.001). Metachronous lesions were equally found every year during the follow-up period in the ESD group. Five-year overall survival rates were 100 % for both groups.
Conclusion
ESD might be an acceptable and effective treatment for EGC considering overall survival rates with fewer early complication rates and shorter duration of hospital stay compared to surgical resection. However, intensive and persistent endoscopic surveillance should be performed after ESD for early detection of metachronous lesions.


Similar content being viewed by others
References
Association JGC (2011) Japanese gastric cancer treatment guidelines 2010 (ver. 3). Gastric Cancer 14:113–123
Chiu PW, Teoh AY, To KF, Wong SK, Liu SY, Lam CC, Yung MY, Chan FK, Lau JY, Ng EK (2012) Endoscopic submucosal dissection (ESD) compared with gastrectomy for treatment of early gastric neoplasia: a retrospective cohort study. Surg Endosc 26:3584–3591
Gotoda T (2008) Endoscopic resection for premalignant and malignant lesions of the gastrointestinal tract from the esophagus to the colon. Gastrointest Endosc Clin N Am 18:435–450
Gotoda T, Yanagisawa A, Sasako M, Ono H, Nakanishi Y, Shimoda T, Kato Y (2000) Incidence of lymph node metastasis from early gastric cancer: estimation with a large number of cases at two large centers. Gastric Cancer 3:219–225
Gotoda T (2007) Endoscopic resection of early gastric cancer. Gastric Cancer 10:1–11
Choi KS, Jung HY, Choi KD, Lee GH, Song HJ, Kim DH, Lee JH, Kim MY, Kim BS, Oh ST, Yook JH, Jang SJ, Yun SC, Kim SO, Kim JH (2011) EMR versus gastrectomy for intramucosal gastric cancer: comparison of long-term outcomes. Gastrointest Endosc 73:942–948
Nagano H, Ohyama S, Fukunaga T, Seto Y, Fujisaki J, Yamaguchi T, Yamamoto N, Kato Y, Yamaguchi A (2005) Indications for gastrectomy after incomplete EMR for early gastric cancer. Gastric Cancer 8:149–154
Bruce J, Krukowski ZH, Al-Khairy G, Russell EM, Park KG (2001) Systematic review of the definition and measurement of anastomotic leak after gastrointestinal surgery. Br J Surg 88:1157–1168
Vather R, Trivedi S, Bissett I (2013) Defining postoperative ileus: results of a systematic review and global survey. J Gastrointest Surg 17:962–972
Park CH, Shin S, Park JC, Shin SK, Lee SK, Lee YC, Lee H (2013) Long-term outcome of early gastric cancer after endoscopic submucosal dissection: expanded indication is comparable to absolute indication. Dig Liver Dis 45:651–656
Nasu J, Doi T, Endo H, Nishina T, Hirasaki S, Hyodo I (2005) Characteristics of metachronous multiple early gastric cancers after endoscopic mucosal resection. Endoscopy 37:990–993
Chung IK, Lee JH, Lee SH, Kim SJ, Cho JY, Cho WY, Hwangbo Y, Keum BR, Park JJ, Chun HJ, Kim HJ, Kim JJ, Ji SR, Seol SY (2009) Therapeutic outcomes in 1000 cases of endoscopic submucosal dissection for early gastric neoplasms: Korean ESD Study Group multicenter study. Gastrointest Endosc 69:1228–1235
Cho KB, Jeon WJ, Kim JJ (2011) Worldwide experiences of endoscopic submucosal dissection: not just Eastern acrobatics. World J Gastroenterol 17:2611–2617
Choi IJ, Lee JH, Kim YI, Kim CG, Cho SJ, Lee JY, Ryu KW, Nam BH, Kook MC, Kim YW (2015) Long-term outcome comparison of endoscopic resection and surgery in early gastric cancer meeting the absolute indication for endoscopic resection. Gastrointest Endosc 81(333–341):e331
Chun HJ, Keum B, Kim JH, Seol SY (2011) Current status of endoscopic submucosal dissection for the management of early gastric cancer: a Korean perspective. World J Gastroenterol 17:2592–2596
Choi JH, Kim ES, Lee YJ, Cho KB, Park KS, Jang BK, Chung WJ, Hwang JS, Ryu SW (2015) Comparison of quality of life and worry of cancer recurrence between endoscopic and surgical treatment for early gastric cancer. Gastrointest Endosc 82:299–307
Kim Y, Kim YW, Choi IJ, Cho JY, Kim JH, Kwon JW, Lee JY, Lee NR, Seol SY (2015) Cost comparison between surgical treatments and endoscopic submucosal dissection in patients with early gastric cancer in Korea. Gut Liver 9:174–180
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Seung Jee Ryu, Byung-Wook Kim, Boo Gyeong Kim, Ji Hee Kim, Joon Sung Kim, ** Il Kim, Jae-Myung Park, Jung-Hwan Oh, Tae Ho Kim, **-Jo Kim, Seung-Man Park, Cho Hyun Park, Kyo Young Song, Jun Hyun Lee, Sung Geun Kim, Dong ** Kim, and Wook Kim have no conflict of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Ryu, S.J., Kim, BW., Kim, B.G. et al. Endoscopic submucosal dissection versus surgical resection for early gastric cancer: a retrospective multicenter study on immediate and long-term outcome over 5 years. Surg Endosc 30, 5283–5289 (2016). https://doi.org/10.1007/s00464-016-4877-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-016-4877-y