Abstract
Purpose
To construct a nomogram based on subjective CT signs and artificial intelligence (AI) histogram parameters to identify invasiveness of lung adenocarcinoma presenting as pure ground-glass nodules (pGGNs) and to evaluate its diagnostic performance.
Methods
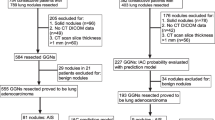
187 patients with 228 pGGNs confirmed by postoperative pathology were collected retrospectively and divided into pre-invasive group [atypical adenomatous hyperplasia (AAH) and adenocarcinoma in situ (AIS)] and invasive group [minimally invasive adenocarcinoma (MIA) and invasive adenocarcinoma (IAC)]. All pGGNs were randomly assigned to training cohort (n = 160) and validation cohort (n = 68). Nomogram was developed using subjective CT signs and AI-based histogram parameters by logistic regression analysis. The diagnostic performance was evaluated by receiver operating characteristic (ROC) curve, calibration curve, and decision curve analysis (DCA) curve.
Results
The nomogram was constructed with nodule shape, 3D mean diameter, maximum CT value, and skewness. It showed better discriminative power in differentiating invasive lesions from pre-invasive lesions with area under curve (AUC) of 0.849 (95% CI 0.790–0.909) in the training cohort and 0.831 (95% CI 0.729–0.934) in the validation cohort, which performed better than nodule shape (AUC 0.675, 95% CI 0.609–0.741), 3D mean diameter (AUC 0.762, 95% CI 0.688–0.835), maximum CT value (AUC 0.794, 95% CI 0.727–0.862), or skewness (AUC 0.594, 95% CI 0.506–0.682) alone in training cohort (for all, P < 0.05).
Conclusion
For pulmonary pGGNs, the nomogram based on subjective CT signs and AI histogram parameters had a good predictive ability to discriminate invasive lung adenocarcinoma from pre-invasive lung adenocarcinoma, and it has the potential to improve diagnostic efficiency and to help the patient management.




Similar content being viewed by others
Data availability
The data (anonymized) that support the findings of this study are available from the corresponding author upon request.
References
Altorki NK, Yip R, Hanaoka T, Bauer T, Aye R, Kohman L, Sheppard B, Thurer R, Andaz S, Smith M, Mayfield W, Grannis F, Korst R, Pass H, Straznicka M, Flores R, Henschke CI (2014) Sublobar resection is equivalent to lobectomy for clinical stage 1A lung cancer in solid nodules. J Thorac Cardiovasc Surg 147(2):754–762. https://doi.org/10.1016/j.jtcvs.2013.09.065
Ardila D, Kiraly AP, Bharadwaj S, Choi B, Reicher JJ, Peng L, Tse D, Etemadi M, Ye W, Corrado G, Naidich DP, Shetty S (2019) End-to-end lung cancer screening with three-dimensional deep learning on low-dose chest computed tomography. Nat Med 25(6):954–961. https://doi.org/10.1038/s41591-019-0447-x
Bi WL, Hosny A, Schabath MB, Giger ML, Birkbak NJ, Mehrtash A, Allison T, Arnaout O, Abbosh C, Dunn IF, Mak RH, Tamimi RM et al (2019) Artificial intelligence in cancer imaging: clinical challenges and applications. CA Cancer J Clin 69(2):127–157. https://doi.org/10.3322/caac.21552
Chu ZG, Li WJ, Fu BJ, Lv FJ (2020) CT characteristics for predicting invasiveness in pulmonary pure ground-glass nodules. AJR Am J Roentgenol 215(2):351–358. https://doi.org/10.2214/AJR.19.22381
Du W, He B, Luo X, Chen M (2022) Diagnostic value of artificial intelligence based on CT image in benign and malignant pulmonary nodules. J Oncol 2022:5818423. https://doi.org/10.1155/2022/5818423
Eriguchi D, Shimada Y, Imai K, Furumoto H, Okano T, Masuno R, Matsubayashi J, Kajiwara N, Ohira T, Ikeda N (2018) Predictive accuracy of lepidic growth subtypes in early-stage adenocarcinoma of the lung by quantitative CT histogram and FDG-PET. Lung Cancer 125:14–21. https://doi.org/10.1016/j.lungcan.2018.08.027
Fan L, Liu SY, Li QC, Yu H, **ao XS (2011) Pulmonary malignant focal ground-glass opacity nodules and solid nodules of 3 cm or less: comparison of multi-detector CT features. J Med Imaging Radiat Oncol 55(3):279–285. https://doi.org/10.1111/j.1754-9485.2011.02265.x
Fan L, Liu SY, Li QC, Yu H, **ao XS (2012) Multidetector CT features of pulmonary focal ground-glass opacity: differences between benign and malignant. Br J Radiol 85(1015):897–904. https://doi.org/10.1259/bjr/33150223
Fang W, Zhang G, Yu Y, Chen H, Liu H (2022) Identification of pathological subtypes of early lung adenocarcinoma based on artificial intelligence parameters and CT signs. Biosci Rep 42(1):BSR20212416. https://doi.org/10.1042/BSR20212416
Gao F, Li M, Ge X, Zheng X, Ren Q, Chen Y, Lv F, Hua Y (2013) Multi-detector spiral CT study of the relationships between pulmonary ground-glass nodules and blood vessels. Eur Radiol 23(12):3271–3277. https://doi.org/10.1007/s00330-013-2954-3
Gao J, Qi Q, Li H, Wang Z, Sun Z, Cheng S, Yu J, Zeng Y, Hong N, Wang D, Wang H, Yang F et al (2023) Artificial-intelligence-based computed tomography histogram analysis predicting tumor invasiveness of lung adenocarcinomas manifesting as radiological part-solid nodules. Front Oncol 13:1096453. https://doi.org/10.3389/fonc.2023.1096453
Han L, Zhang P, Wang Y, Gao Z, Wang H, Li X, Ye Z (2018) CT quantitative parameters to predict the invasiveness of lung pure ground-glass nodules (pGGNs). Clin Radiol 73(5):504.e1-504.e7. https://doi.org/10.1016/j.crad.2017.12.021
Heidinger BH, Anderson KR, Nemec U, Costa DB, Gangadharan SP, VanderLaan PA, Bankier AA (2017) Lung adenocarcinoma manifesting as pure ground-glass nodules: correlating CT Size, volume, density, and roundness with histopathologic invasion and size. J Thorac Oncol 12(8):1288–1298. https://doi.org/10.1016/j.jtho.2017.05.017
Huang G, Wei X, Tang H, Bai F, Lin X, Xue D (2021) A systematic review and meta-analysis of diagnostic performance and physicians’ perceptions of artificial intelligence (AI)-assisted CT diagnostic technology for the classification of pulmonary nodules. J Thorac Dis 13(8):4797–4811. https://doi.org/10.21037/jtd-21-810
Hwang IP, Park CM, Park SJ, Lee SM, McAdams HP, Jeon YK, Goo JM (2015) Persistent pure ground-glass nodules larger than 5 mm: differentiation of invasive pulmonary adenocarcinomas from preinvasive lesions or minimally invasive adenocarcinomas using texture analysis. Invest Radiol 50(11):798–804. https://doi.org/10.1097/RLI.0000000000000186
Ichinose J, Kawaguchi Y, Nakao M, Matsuura Y, Okumura S, Ninomiya H, Oikado K, Nishio M, Mun M (2020) Utility of maximum CT value in predicting the invasiveness of pure ground-glass nodules. Lung Cancer 21(3):281–287. https://doi.org/10.1016/j.cllc.2020.01.015
** X, Zhao SH, Gao J, Wang DJ, Wu J, Wu CC et al (2015) CT characteristics and pathological implications of early stage (T1N0M0) lung adenocarcinoma with pure ground-glass opacity. Eur Radiol 25(9):2532–2540. https://doi.org/10.1007/s00330-015-3637-z
Kao TN, Hsieh MS, Chen LW, Yang CJ, Chuang CC, Chiang XH, Chen YC, Lee YH, Hsu HH, Chen CM, Lin MW, Chen JS (2022) CT-based radiomic analysis for preoperative prediction of tumor invasiveness in lung adenocarcinoma presenting as pure ground-glass nodule. Cancers. https://doi.org/10.3390/cancers14235888
Kent M, Landreneau R, Mandrekar S, Hillman S, Nichols F, Jones D, Starnes S, Tan A, Putnam J, Meyers B, Daly B, Fernando HC (2013) Segmentectomy versus wedge resection for non-small cell lung cancer in high-risk operable patients. Ann Thorac Surg 96(5):1747–1755. https://doi.org/10.1016/j.athoracsur.2013.05.104
Kitami A, Sano F, Hayashi S, Suzuki K, Uematsu S, Kamio Y, Suzuki T, Kadokura M, Omatsu M, Kunimura T (2016) Correlation between histological invasiveness and the computed tomography value in pure ground-glass nodules. Surg Today 46(5):593–598. https://doi.org/10.1007/s00595-015-1208-1
Koike H, Ashizawa K, Tsutsui S, Kurohama H, Okano S, Nagayasu T, Kido S, Uetani M, Toya R (2023) Differentiation between heterogeneous GGN and part-solid nodule using 2 d grayscale histogram analysis of thin-section CT image. Clin Lung Cancer. https://doi.org/10.1016/j.cllc.2023.06.001. (S1525-7304(23)00121-3)
Lai J, Li Q, Fu F, Zhang Y, Li Y, Liu Q, Chen H (2022) Subsolid lung adenocarcinomas: radiological, clinical and pathological features and outcomes. Semin Thorac Cardiovasc Surg 34(2):702–710. https://doi.org/10.1053/j.semtcvs.2021.04.051
Lederlin M, Revel MP, Khalil A, Ferretti G, Milleron B, Laurent F (2013) Management strategy of pulmonary nodule in 2013. Diagn Interv Imaging 94(11):1081–1094. https://doi.org/10.1016/j.diii.2013.05.007
Lee GD, Park CH, Park HS, Byun MK, Lee IJ, Kim TH, Lee S (2019) Lung adenocarcinoma invasiveness risk in pure ground-glass opacity lung nodules smaller than 2 cm. Thorac Cardiovasc Surg 67(4):321–328. https://doi.org/10.1055/s-0037-1612615
Li Q, Fan L, Cao ET, Li QC, Gu YF, Liu SY (2017) Quantitative CT analysis of pulmonary pure ground-glass nodule predicts histological invasiveness. Eur J Radiol 89:67–71. https://doi.org/10.1016/j.ejrad.2017.01.024
Li K, Liu K, Zhong Y, Liang M, Qin P, Li H, Zhang R, Li S, Liu X (2021) Assessing the predictive accuracy of lung cancer, metastases, and benign lesions using an artificial intelligence-driven computer aided diagnosis system. Quant Imaging Med Surg 11(8):3629–3642. https://doi.org/10.21037/qims-20-1314
Shi Z, Deng J, She Y, Zhang L, Ren Y, Sun W, Su H, Dai C, Jiang G, Sun X, **e D, Chen C (2019) Quantitative features can predict further growth of persistent pure ground-glass nodule. Quant Imaging Med Surg 9(2):283–291. https://doi.org/10.21037/qims.2019.01.04
Succony L, Rassl DM, Barker AP, McCaughan FM, Rintoul RC (2021) Adenocarcinoma spectrum lesions of the lung: Detection, pathology and treatment strategies. Cancer Treat Rev 99:102237. https://doi.org/10.1016/j.ctrv.2021.102237
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F (2021) Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 71(3):209–249. https://doi.org/10.3322/caac.21660
Suzuki K, Watanabe SI, Wakabayashi M, Saji H, Aokage K, Moriya Y, Yoshino I, Tsuboi M, Nakamura S, Nakamura K, Mitsudomi T, Asamura H (2022) A single-arm study of sublobar resection for ground-glass opacity dominant peripheral lung cancer. J Thorac Cardiovasc Surg 163(1):289-301.e2. https://doi.org/10.1016/j.jtcvs.2020.09.146
The WHO Classification of Tumours Editorial Board (2021) WHO classification of tumors: Thoracic Tumors, 5th ed. IARC Press, Lyon. https://publications.iarc.fr/Book-And-Report-Series/Who-Classification-Of-Tumours/Thoracic-Tumours-2021
Travis WD, Brambilla E, Noguchi M, Nicholson AG, Geisinger KR, Yatabe Y, Beer DG, Powell CA, Riely GJ, Van Schil PE, Garg K, Austin JH et al (2011) International association for the study of lung cancer/american thoracic society/european respiratory society international multidisciplinary classification of lung adenocarcinoma. J Thorac Oncol 6(2):244–285. https://doi.org/10.1097/JTO.0b013e318206a221
Travis WD, Brambilla E, Nicholson AG, Yatabe Y, Austin JHM, Beasley MB, Chirieac LR, Dacic S, Duhig E, Flieder DB, Geisinger K, Hirsch FR, Ishikawa Y, Kerr KM, Noguchi M, Pelosi G, Powell CA, Tsao MS, Wistuba I (2015) The 2015 World Health Organization classification of lung tumors: impact of genetic, clinical and radiologic advances since the 2004 classification. J Thorac Oncol 10(9):1243–1260. https://doi.org/10.1097/JTO.0000000000000630
Wang Q, Ba W, Yin K, Shen J, Jiang G, Liang Y, Zhu Z, Wu J (2022a) Predicting lung adenocarcinoma invasiveness by measurement of pure ground-glass nodule roundness by using multiplanar reformation: a retrospective analysis. Clin Radiol 77(1):e20–e26. https://doi.org/10.1016/j.crad.2021.10.007
Wang XL, Sun XS, Yan CX, Zhang Q (2022b) CT-Assisted improvements in the accuracy of the intraoperative frozen section examination of ground-glass density nodules. Comput Math Methods Med 2022:8967643. https://doi.org/10.1155/2022/8967643
Yotsukura M, Asamura H, Motoi N, Kashima J, Yoshida Y, Nakagawa K, Shiraishi K, Kohno T, Yatabe Y, Watanabe SI (2021) Long-term prognosis of patients with resected adenocarcinoma in situ and minimally invasive adenocarcinoma of the lung. J Thorac Oncol 16(8):1312–1320. https://doi.org/10.1016/j.jtho.2021.04.007
Zhang T, Pu XH, Yuan M, Zhong Y, Li H, Wu JF, Yu TF (2019) Histogram analysis combined with morphological characteristics to discriminate adenocarcinoma in situ or minimally invasive adenocarcinoma from invasive adenocarcinoma appearing as pure ground-glass nodule. Eur J Radiol 113:238–244. https://doi.org/10.1016/j.ejrad.2019.02.034
Zhang Y, Ma X, Shen X, Wang S, Li Y, Hu H, Chen H (2022) Surgery for pre- and minimally invasive lung adenocarcinoma. J Thorac Cardiovasc Surg 163(2):456–464. https://doi.org/10.1016/j.jtcvs.2020.11.151
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. RG contributed to writing—original draft. YG contributed to conceptualization and methodology. JZ and CY contributed to writing—review and editing. CZ and YZ contributed to data curation and formal analysis. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
The study received ethical approval by the Institutional Ethics Committee of the Second Affiliated Hospital of Shandong First Medical University (No. 2021-086) and informed consent was obtained from all patients.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gao, R., Gao, Y., Zhang, J. et al. A nomogram for predicting invasiveness of lung adenocarcinoma manifesting as pure ground-glass nodules: incorporating subjective CT signs and histogram parameters based on artificial intelligence. J Cancer Res Clin Oncol 149, 15323–15333 (2023). https://doi.org/10.1007/s00432-023-05262-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-023-05262-4