Abstract
Background
Recent studies have reported that overall survival of elderly patients with primary central nervous system lymphoma (PCNSL), who have the highest incidence of this disease, had failed to benefit from the advancements in treatment strategies over the past decades. This highlights the necessity for intensified research to guide treatment decisions for this specific patient population.
Methods
The Surveillance, Epidemiology, and End Results (SEER) program of the National Cancer Institute (NCI) was used to extract data of elderly PCNSL patients (age ≥ 60) who were divided into training and validation groups at the ratio of 7:3, for our analysis. Conditional survival [CS(y|x)] was defined as the probability at survival additional y years given that the patient had not died of PCNSL at a specified period of time (x years) after initial diagnosis. The CS pattern of elderly PCNSL patients was analyzed. The least absolute shrinkage and selection operator (LASSO) regression and multivariate Cox regression analysis were applied to develop a novel CS-based nomogram.
Results
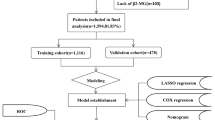
A total of 3315 elderly patients diagnosed with CNS lymphoma between 2000 and 2019 were extracted from the SEER database, of whom 2320 patients were divided into the training group and 995 into the internal validation group. CS analysis revealed a noteworthy escalation in the 5-year survival rate among elderly PCNSL patients for every additional year of survival. The rates progressed from an initial 21–49%, 63%, and 75%, culminating in an impressive 88% and the survival improvement over time was nonlinear. The LASSO regression identified nine predictors and multivariate Cox regression was used to successfully construct the CS-based nomogram model with favorable prediction performance.
Conclusion
CS of elderly PCNSL patients was dynamic and increased over time. Our newly-established CS-based nomogram can provide a real-time dynamic survival estimation, allowing clinicians to better guide treatment decision for these patients.






Similar content being viewed by others
Data availability
The data sets used and/or analyzed during the current study are available from the Surveillance, Epidemiology, and End Results (SEER) database http://seer.cancer.gov/.
References
Bui A, Yang L, Myint A, May F (2021) Race, ethnicity, and socioeconomic status are associated with prolonged time to treatment after a diagnosis of colorectal cancer: a large population-based study. Gastroenterology 160(4):1394-1396.e3. https://doi.org/10.1053/j.gastro.2020.10.010
Burns E, Sanchez C, Mathur S, Guerrero C, Muhsen I, Sarfraz H, Hu C, Tang C, Shah S, Tremont I, Teh B, Ganguly S, **ali S (2023) Long term outcomes in older patients with primary central nervous system lymphoma: an analysis of the texas cancer registry. Ann Hematol 102(5):1111–1120. https://doi.org/10.1007/s00277-023-05140-6
Chukwueke U, Nayak L (2019) Central nervous system lymphoma. Hematol Oncol Clin North Am 33(4):597–611. https://doi.org/10.1016/j.hoc.2019.03.008
David K, Sundaram S, Kim S, Vaca R, Lin Y, Singer S, Malecek M, Carter J, Zayac A, Kim M, Reddy N, Ney D, Habib A, Strouse C, Graber J, Bachanova V, Salman S, Vendiola J, Hossain N, Tsang M, Major A, Bond D, Agrawal P, Mier-Hicks A, Torka P, Rajakumar P, Venugopal P, Berg S, Glantz M, Goldlust S, Folstad M, Kumar P, Ollila T, Cai J, Spurgeon S, Sieg A, Cleveland J, Chang J, Epperla N, Karmali R, Naik S, Martin P, Smith S, Rubenstein J, Kahl B, Evens A (2023) Older patients with primary central nervous system lymphoma: survival and prognostication across 20 US cancer centers. Am J Hematol 98(6):900–912. https://doi.org/10.1002/ajh.26919
Deng X, Xu X, Lin D, Zhang X, Yu L, Sheng H, Yin B, Zhang N, Lin J (2020) Real-world impact of surgical excision on overall survival in primary central nervous system lymphoma. Front Oncol 10:131. https://doi.org/10.3389/fonc.2020.00131
Dikken J, Baser R, Gonen M, Kattan M, Shah M, Verheij M, van de Velde C, Brennan M, Coit D (2013) Conditional probability of survival nomogram for 1-, 2-, and 3-year survivors after an R0 resection for gastric cancer. Ann Surg Oncol 20(5):1623–1630. https://doi.org/10.1245/s10434-012-2723-6
Furst T, Hoffman H, Chin L (2019) All-cause and tumor-specific mortality trends in elderly primary central nervous system lymphoma (PCNSL) patients: a surveillance, epidemiology, and end results (SEER) analysis. J Neurosurg Sci. https://doi.org/10.23736/s0390-5616.19.04785-4
Grommes C, DeAngelis L (2017) Primary CNS lymphoma. J Clin Oncol 35(21):2410–2418. https://doi.org/10.1200/jco.2017.72.7602
Harlan L, Hankey B (2003) The surveillance, epidemiology, and end-results program database as a resource for conducting descriptive epidemiologic and clinical studies. J Clin Oncol 21(12):2232–2233. https://doi.org/10.1200/jco.2003.94.023
Hieke S, Kleber M, König C, Engelhardt M, Schumacher M (2015) Conditional survival: a useful concept to provide information on how prognosis evolves over time. Clin Cancer Res 21(7):1530–1536. https://doi.org/10.1158/1078-0432.Ccr-14-2154
Holdhoff M, Mrugala M, Grommes C, Kaley T, Swinnen L, Perez-Heydrich C, Nayak L (2020) Challenges in the treatment of newly diagnosed and recurrent primary central nervous system lymphoma. J Natl Comprehen Cancer Net JNCCN 18(11):1571–1578. https://doi.org/10.6004/jnccn.2020.7667
Latenstein A, van Roessel S, van der Geest L, Bonsing B, Dejong C, Groot Koerkamp B, de Hingh I, Homs M, Klaase J, Lemmens V, Molenaar I, Steyerberg E, Stommel M, Busch O, van Eijck C, van Laarhoven H, Wilmink J, Besselink M (2020) Conditional survival after resection for pancreatic cancer: a population-based study and prediction model. Ann Surg Oncol 27(7):2516–2524. https://doi.org/10.1245/s10434-020-08235-w
Liu Y, Yao Q, Zhang F (2021) Diagnosis, prognosis and treatment of primary central nervous system lymphoma in the elderly population (Review). Int J Oncol 58(3):371–387. https://doi.org/10.3892/ijo.2021.5180
Lv C, Wang J, Zhou M, Xu J, Chen B, Wan Y (2022) Primary central nervous system lymphoma in the United States, 1975–2017. Therap Adv Hematol 13:20406207211066170. https://doi.org/10.1177/20406207211066166
Maloney N, Aasi S, Kibbi N, Hirotsu K, Zaba L (2023) Online risk calculator and nomogram for predicting sentinel lymph node positivity in Merkel Cell Carcinoma. J Am Acad Dermatol. https://doi.org/10.1016/j.jaad.2023.05.042
Mendez J, Ostrom Q, Gittleman H, Kruchko C, DeAngelis L, Barnholtz-Sloan J, Grommes C (2018) The elderly left behind-changes in survival trends of primary central nervous system lymphoma over the past 4 decades. Neuro Oncol 20(5):687–694. https://doi.org/10.1093/neuonc/nox187
Meng X, Cai Y, Chang X, Guo Y (2023) A novel conditional survival nomogram for monitoring real-time prognosis of non-metastatic triple-negative breast cancer. Front Endocrinol 14:1119105. https://doi.org/10.3389/fendo.2023.1119105
Norden A, Drappatz J, Wen P, Claus E (2011) Survival among patients with primary central nervous system lymphoma, 1973–2004. J Neurooncol 101(3):487–493. https://doi.org/10.1007/s11060-010-0269-7
Omofuma O, Cook M, Abnet C, Camargo M (2023) Race and ethnicity, stage-specific mortality, and cancer treatment in esophageal and gastric cancers: surveillance, epidemiology, and end results (2000–2018). Gastroenterology 164(3):473-475.e4. https://doi.org/10.1053/j.gastro.2022.11.032
Ötleş E, Denton B, Qu B, Murali A, Merdan S, Auffenberg G, Hiller S, Lane B, George A, Singh K (2022) Development and validation of models to predict pathological outcomes of radical prostatectomy in regional and national cohorts. J Urol 207(2):358–366. https://doi.org/10.1097/ju.0000000000002230
Shiels M, Pfeiffer R, Besson C, Clarke C, Morton L, Nogueira L, Pawlish K, Yanik E, Suneja G, Engels E (2016) Trends in primary central nervous system lymphoma incidence and survival in the U.S. Br J Haematol 174(3):417–24. https://doi.org/10.1111/bjh.14073
Skuladottir H, Olsen J (2003) Conditional survival of patients with the four major histologic subgroups of lung cancer in Denmark. J Clin Oncol 21(16):3035–3040. https://doi.org/10.1200/jco.2003.04.521
Tang D, Chen Y, Shi Y, Tao H, Tao S, Zhang Q, Ding B, He Z, Yu L, Wang C (2022) Epidemiologic characteristics, prognostic factors, and treatment outcomes in primary central nervous system lymphoma: a SEER-based study. Front Oncol 12:817043. https://doi.org/10.3389/fonc.2022.817043
van der Meulen M, Dinmohamed A, Visser O, Doorduijn J, Bromberg J (2017) Improved survival in primary central nervous system lymphoma up to age 70 only: a population-based study on incidence, primary treatment and survival in the Netherlands, 1989–2015. Leukemia 31(8):1822–1825. https://doi.org/10.1038/leu.2017.128
Velicu M, Lavrador J, Sibtain N, Vergani F, Bhangoo R, Gullan R, Ashkan K (2023) Neurosurgical management of central nervous system lymphoma: lessons learnt from a neuro-oncology multidisciplinary team approach. J Person Med. https://doi.org/10.3390/jpm13050783
Villanueva G, Guscott M, Schaiquevich P, Sampor C, Combs R, Tentoni N, Hwang M, Lowe J, Howard S (2023) A systematic review of high-dose methotrexate for adults with primary central nervous system lymphoma. Cancers. https://doi.org/10.3390/cancers15051459
Wang L, Qu H, Ma X, Liu X (2022a) Identification of oxidative stress-associated molecular subtypes and signature for predicting survival outcome of cervical squamous cell carcinoma. Oxid Med Cell Longev 2022:1056825. https://doi.org/10.1155/2022/1056825
Wang Q, Wang Y, Wang X, Nakamura Y, Hydbring P, Yamauchi Y, Zhao X, Cao M (2022b) Development and validation of a dynamic survival nomogram for metastatic non-small cell lung cancer based on the SEER database and an external validation cohort. Transl Lung Cancer Res 11(8):1678–1691. https://doi.org/10.21037/tlcr-22-544
Wismann J, Sommer-Sørensen R, Kofoed M, Halle B, Pedersen C, Schulz M, Grønhøj M, Larsen T, Møller M, Poulsen F (2022) Diagnosis, treatment, and outcome of primary CNS lymphoma-a single-center experience. Acta Neurochir 164(5):1365–1373. https://doi.org/10.1007/s00701-022-05170-5
Yang C, Ren X, Cui Y, Jiang H, Yu K, Li M, Zhao X, Zhu Q, Lin S (2021) Nomograms for predicting cancer-specific survival in patients with primary central nervous system lymphoma: a population-based analysis. Ann Transl Med 9(13):1055. https://doi.org/10.21037/atm-21-753
Yu X, Gao S, Xue Q, Tan F, Gao Y, Mao Y, Wang D, Zhao J, Li Y, Wang F, Cheng H, Zhao C, Mu J (2021) Development of a nomogram for predicting the operative mortality of patients who underwent pneumonectomy for lung cancer: a population-based analysis. Transl Lung Cancer Res 10(1):381–391. https://doi.org/10.21037/tlcr-20-561
Zabor E, Gonen M, Chapman P, Panageas K (2013) Dynamic prognostication using conditional survival estimates. Cancer 119(20):3589–3592. https://doi.org/10.1002/cncr.28273
Acknowledgements
The authors would like to thank the SEER database for the availability of the data.
Funding
None.
Author information
Authors and Affiliations
Contributions
HQ and HC designed the study; HQ, ZY, LC, and HC contributed to data analysis. HQ wrote the initial draft of the manuscript; HQ, ZY, LC, and HC reviewed and edited the manuscript. All authors read and approved the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Qian, H., Yang, Z., Cai, L. et al. Conditional survival of elderly primary central nervous system lymphoma. J Cancer Res Clin Oncol 149, 13391–13401 (2023). https://doi.org/10.1007/s00432-023-05200-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-023-05200-4