Abstract
Purpose
Diabetic women appear to have adverse pregnancy outcomes. Although there were two meta-analyzes that examined the association between health care and adverse pregnancy outcomes, their results were limited because they only included congenital anomaly and perinatal mortality, and they did not clarify the detailed situations of diabetes and health care. This meta-analysis aims to completely evaluate the effects of health care in improving adverse pregnancy outcomes among diabetic mothers.
Methods
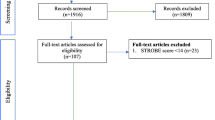
CNKI, EMBASE, Web of Science, and PubMed databases were searched for eligible studies up to December 2017, without any restrictions. Relevant cohort studies characterizing the relationship between health care and adverse pregnancy outcomes were selected for inclusion in the meta-analysis. We also screened the reference list of relevant studies. The fixed-effect models or random-effect models were used to calculate the risk estimates. The potential sources of heterogeneity were explored by stratified and sensitivity analyzes.
Results
Twenty-one studies with 6685 cases were included in our analysis. Health care was associated with significantly decreased risk of congenital anomaly (RR 0.237; 95% CI 0.166–0.338), perinatal death (RR 0.457; 95% CI 0.294–0.712), large for gestational age (LGA) (RR 0.794; 95% CI 0.640–0.986), and neonatal hypoglycemia (RR 0.672; 95% CI 0.486–0.929). Publication bias was not found in most results, with the exception of congenital anomaly and small for gestational age (SGA).
Conclusion
Health care is associated with decreased risk of congenital anomaly, perinatal death, LGA, neonatal hypoglycemia.


Similar content being viewed by others
References
International Diabetes Federation (2017) IDF Diabetes Atlas, 8th edn. International Diabetes Federation, Brussels. https://www.diabetesatlas.org. Accessed 11 Jan 2018
Ray JG, Vermeulen MJ, Meier C, Wyatt PR (2004) Risk of congenital anomalies detected during antenatal serum screening in women with pregestational diabetes. QJM Int J Med 97(10):651–653. https://doi.org/10.1093/qjmed/hch107
The Di, abetes Control and Complications Trial Research Group (1996) Pregnancy outcomes in the Diabetes Control and Complications Trial. Am J Obstet Gynecol 174(4):1343–1353. https://doi.org/10.1016/S0002-9378(96)70683-X
Metcalfe A, Sabr Y, Hutcheon JA, Donovan L, Lyons J et al (2017) Trends in obstetric intervention and pregnancy outcomes of canadian women with diabetes in pregnancy from 2004 to 2015. J Endocr Soc 1(12):1540–1549. https://doi.org/10.1210/js.2017-00376
Øyen Nina, Diaz LJ, Leirgul E, Boyd HA, Priest J et al (2016) Prepregnancy diabetes and offspring risk of congenital heart disease: a nationwide cohort study. Circulation 133(23):2243–2253. https://doi.org/10.1161/CIRCULATIONAHA.115.017465
Hoet JP, Lukens FD (1954) Carbohydrate metabolism during pregnancy. Diabetes 3:1–12
National Institute for Health and Clinical Excellence (2008) Diabetes in pregnancy: management of diabetes and its complications from pre-conception to the postnatal period. NICE, London. https://www.nice.org.uk/CG063. Accessed 11 Jan 2018
Ray JG, O'Brien TE, Chan WS (2001) Preconception care and the risk of congenital anomalies in the offspring of women with diabetes mellitus: a meta-analysis. QJM 94(8):435–444
Wahabi HA, Alzeidan RA, Bawazeer GA, Alansari LA, Esmaeil SA (2010) Preconception care for diabetic women for improving maternal and fetal outcomes: a systematic review and meta-analysis. BMC Pregnancy Childbirth 10:63. https://doi.org/10.1186/1471-2393-10-63
Galindo A et al (2006) Outcome of fetuses in women with pregestational diabetes mellitus. J Perinat Med 34(4):323–331. https://doi.org/10.1515/JPM.2006.063
Peck RW et al (1991) Birthweight of babies born to mothers with type 1 diabetes: is it related to blood glucose control in the first trimester? Diabet Med 8(3):258–262
Mokgokong ET (1983) Management of diabetes mellitus during pregnancy by maintaining normal blood glucose levels. S Afr Med J 64(26):1011–1013
Fuhrmann K et al (1984) The effect of intensified conventional insulin therapy before and during pregnancy on the malformation rate in offspring of diabetic mothers. Exp Clin Endocrinol 83(2):173–177. https://doi.org/10.1055/s-0029-1210327
Pearson DW et al (2007) The relationship between pre-pregnancy care and early pregnancy loss, major congenital anomaly or perinatal death in type I diabetes mellitus. BJOG 114(1):104–107. https://doi.org/10.1111/j.1471-0528.2006.01145.x
Janz NK et al (1995) Diabetes and Pregnancy: Factors associated with seeking pre-conception care. Diabetes Care 18(2):157–165
Correa A et al (2003) Do multivitamin supplements attenuate the risk for diabetes-associated birth defects? Pediatrics 111(5 Pt 2):1146–1151
Tripathi A et al (2010) Preconception counseling in women with diabetes a population-based study in the North of England. Diabetes Care 33(3):586–588. https://doi.org/10.2337/dc09-1585
Dicker D et al (1988) Spontaneous abortion in patients with insulin-dependent diabetes mellitus: the effect of preconceptional diabetic control. Am J Obstet Gynecol 158(5):1161–1164
Banerjee S, Ghosh US, Banerjee D (2004) Effect of tight glycaemic control on fetal complications in diabetic pregnancies. J Assoc Physicians India 52:109–113
Wong VW, Suwandarathne H, Russell H (2013) Women with pre-existing diabetes under the care of diabetes specialist prior to pregnancy: are their outcomes better? Aust N Z J Obstet Gynaecol 53(2):207–210. https://doi.org/10.1111/ajo.12044
Damm P, Molsted-Pedersen L (1989) Significant decrease in congenital malformations in newborn infants of an unselected population of diabetic women. Am J Obstet Gynecol 161(5):1163–1167
Boulot P et al (2003) French multicentric survey of outcome of pregnancy in women with pregestational diabetes. Diabetes Care 26(11):2990–2993
Steel Judith M, Johnstone Frank D, Hepburn David A, Smith Alistair F (1990) Can prepregnancy care of diabetic women reduce the risk of abnormal babies? BMJ 301(6760):1070–1074
Murphy HR et al (2010) Effectiveness of a regional prepregnancy care program in women with type 1 and type 2 diabetes: benefits beyond glycemic control. Diabetes Care 33(12):2514–2520. https://doi.org/10.2337/dc10-1113
Temple RC, Aldridge VJ, Murphy HR (2006) Prepregnancy care and pregnancy outcomes in women with type 1 diabetes. Diabetes Care 29(8):1744–1749. https://doi.org/10.2337/dc05-2265
Dunne FP et al (1999) Pre-conception diabetes care in insulin-dependent diabetes mellitus. QJM 92(3):175–176
Kekalainen R et al (2013) Hemoglobin A1c in pregestational diabetic gravidas and the risk of congenital heart disease in the fetus. Pediatr Cardiol 34(7):1716–1722. https://doi.org/10.1007/s00246-013-0704-6
Rosenn B et al (1991) Pre-conception management of insulin-dependent diabetes: improvement of pregnancy outcome. Obstet Gynecol. 77(6):846–849
Kitzmiller JL et al (1991) Preconception care of diabetes glycemic control prevents congenital anomalies. JAMA 265(6):731–736
Willhoite MB et al (1993) The impact of preconception counseling on pregnancy outcomes. The experience of the Maine Diabetes in Pregnancy Program. Diabetes Care 16(2):450–455
Luo L, Wu T, Xu Y (2014) The analysis of nutrition guidance on pregnant women with pre-gestational diabetes and fetal development. Chin J Fam Plan Obstet Gynecol 02:25–27
Chen Y (2012) Risk factors for gestational diabetes mellitus and nursing intervention on the outcome of maternal and infant research. Dissertation. Dissertation, Guangxi Medical University
Ye Lin, Huang **g**g, Yao Wei (2010) Clinical observation on effective control of gestational diabetes mellitus and blood glucose to improve pregnancy outcome. J Qiqihar Med Coll 18:2874–2875
Wang Huilan, Zhou Wan** (2016) Effect of control of blood glucose in pregnant women with gestational period on prognosis of mother and infant. Matern Child Health Care China 20:4152–4153
Wang Y (2014) Effects on pregnancy outcomes and neonatal complications of glycemic control in pregnant women with gestational diabetes. Dissertation, J Liaoning Medical University
Garcia-Patterson A et al (1997) Does preconceptional counselling in diabetic women influence perinatal outcome? Ann Ist Super Sanita 33(3):333–336
Neff KJ et al (2014) Pre-pregnancy care and pregnancy outcomes in type 1 diabetes mellitus: a comparison of continuous subcutaneous insulin infusion and multiple daily injection therapy. Ir J Med Sci 183(3):397–403. https://doi.org/10.1007/s11845-013-1027-6
Goldman JA et al (1986) Pregnancy outcome in patients with insulin-dependent diabetes mellitus with preconceptional diabetic control: a comparative study. Am J Obstet Gynecol 155(2):293–297
Kekalainen P et al (2016) Pregnancy planning in type 1 diabetic women improves glycemic control and pregnancy outcomes. J Matern Fetal Neonatal Med 29(14):2252–2258. https://doi.org/10.3109/14767058.2015.1081888
Moore TR (2003) Diabetes in pregnancy. In: Creasy RK, Resnik R (eds) Maternal-fetal medicine, 5th edn. wB Saunders, Philadelphia, pp 1023–1062
Rajdl D, Racek J, Steinerova A, Novotny Z, Stozicky F et al (2005) Markers of oxidative stress in diabetic mothers and their infants during delivery. Physiol Res 54:429–436
Wender-Ozgowska E, Wroblewska K, Zawiejska A, Pietryga M, Szczapa J et al (2005) Threshold values of maternal blood glucose in early diabetic pregnancy—Prediction of fetal malformations. Acta Obstet Gynecol Scand 84:17–25. https://doi.org/10.1111/j.0001-6349.2005.00606.x
Barnes-Powell LL (2007) Infants of diabetic mothers: the effects of hyperglycemia on the fetus and neonate. Neonatal Netw 26(5):283–290. https://doi.org/10.1891/0730-0832.26.5.283
Blackburn S (2003) Maternal, fetal, and neonatal physiology: a clinical perspective, 2nd edn. wB Saunders, St. Louis
Ashfaq M, Janjua MZ, Channa MA (2005) effect of gestational diabetes and maternal hypertension on gross morphology of placenta. J Ayub Med Coll Abbottabad 17(1):44–47
Belkacemi L, Lash G, Macdonald-Goodfellow SK, Caldwell JD, Graham CH (2005) Inhibition of human trophoblast invasiveness by high glucose concentrations. J Clin Endocrinol Metab 90:4846–4851. https://doi.org/10.1210/jc.2004-2242
Gamblian VW, Weiland J, Park NC (2003) Assessment and management of the endocrine system. In: Kenner C, Lott JW (eds) Comprehensive neonatal nursing, 3rd edn. WB Saunders, Philadelphia, pp 531–549
Ryckman KK, Spracklen CN, Smith CJ, Robinson JG, Saftlas AF (2015) Maternal lipid levels during pregnancy and gestational diabetes: a systematic review and meta-analysis. BJOG 122:643–651. https://doi.org/10.1111/1471-0528.13261
Schaefer-Graf UM, Graf K, Kulbacka I, Kjos SL, Dudenhausen J et al (2008) Maternal lipids as strong determinants of fetal environment and growth in pregnancies with gestational diabetes mellitus. Diabetes Care 31:1858–1863. https://doi.org/10.2337/dc08-0039
Acknowledgements
We are grateful to everyone who helped us to complete this study successfully.
Funding
This work was supported by a Grant from National Natural Science Foundation of China (no: 81773530).
Author information
Authors and Affiliations
Contributions
GX: data collection, data analysis, manuscript writing. ZZ: contributed to the conception. TL: data collection. LQ: data collection. XH: contributed analysis tools. WZ: revised the manuscript. YL: approved the final version.
Corresponding authors
Ethics declarations
Conflict of interest
Author Guohong **e declares that she has no conflict of interest. Author Zan Zheng declares that he has no conflict of interest. Author Taocheng Liu declares that he has no conflict of interest. Author Lulu Qing declares that she has no conflict of interest. Author **uqing Hong declares that she has no conflict of interest. Author Wenting Zha declares that she has no conflict of interest. Author Yuan Lv declares that she has no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
**e, GH., Zheng, Z., Liu, TC. et al. Health care and risk of adverse pregnancy outcomes among diabetic women: an updated meta-analysis. Arch Gynecol Obstet 299, 891–899 (2019). https://doi.org/10.1007/s00404-019-05042-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-019-05042-x