Abstract
Background
Periprosthetic joint infections (PJI) are a major concern in shoulder arthroplasty, which in some cases require two-stage exchange. While it was shown that low-virulence bacteria are the most isolated pathogens in shoulder PJI, little is known about changes in microbiological spectrum and resistance patterns during two-stage revision.
Methods
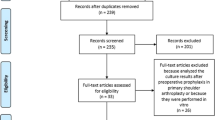
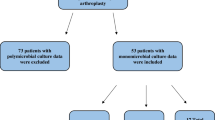
This retrospective study included all patients (n = 25) who received a two-stage revision from January 2011 to December 2020 for shoulder PJI in one institution. Microbiological spectrum, antimicrobial resistance patterns, and re-revision rates of culture positive first- and second-stage procedures were analyzed. The mean follow-up time was 29.7 months (range 8; 115 months). At final follow-up, subjective shoulder value (SSV) and visual analog scale (VAS) score for pain and satisfaction with the surgery were assessed.
Results
In 25 patients, a total of 54 2-stage exchange procedures were performed and positive cultures were obtained in 36 of these surgeries (66.7%). A total of 7 out of 25 patients (28.0%) showed a positive microbiological culture at first and second stages. In those patients, the mean time between first and second stages was 30.9 weeks (range 6; 70). Three out of those seven patients (42.9%) had a polymicrobial spectrum with one microorganism persistent at stage two, including Cutibacterium acnes (n = 1) and Staphylococcus epidermidis (MRSE) (n = 2). In all these cases, antimicrobial resistance patterns changed. All cultures with monomicrobial spectrum (n = 4) at first stage showed a changed spectrum. Patients with positive first- and second-stage revisions showed a mean SSV of 49.3% ± 23.5 versus 52.9% ± 29.5 in single positive patients (p = 0.76). Re-revision was performed in five cases, two of those in patients with positive first- and second-stage cultures.
Conclusion
There is a high rate of changes in microbiological spectrum and resistance patterns between culture positive first- and second-stage procedures as well as subsequent re-revisions. Intraoperative samples during reimplantation should be taken and resistance reconsidered in case of re-revision.



Similar content being viewed by others
References
Akgun D, Maziak N, Plachel F et al (2020) The role of implant sonication in the diagnosis of periprosthetic shoulder infection. J Shoulder Elbow Surg. https://doi.org/10.1016/j.jse.2019.10.011
Akgun D, Wietholter M, Maziak N et al (2021) Two-stage exchange arthroplasty for periprosthetic shoulder infection is associated with high rate of failure to reimplant and mortality. J Clin Med. https://doi.org/10.3390/jcm10215186
Akgun D, Wietholter M, Siegert P et al (2021) The role of serum C-reactive protein in the diagnosis of periprosthetic shoulder infection. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-021-03779-2
Beekman PD, Katusic D, Berghs BM, Karelse A, De Wilde L (2010) One-stage revision for patients with a chronically infected reverse total shoulder replacement. J Bone Jt Surg Br 92(6):817–822. https://doi.org/10.1302/0301-620X.92B6.23045
Bonnevialle N, Dauzeres F, Toulemonde J, Elia F, Laffosse JM, Mansat P (2017) Periprosthetic shoulder infection: an overview. EFORT Open Rev 2(4):104–109. https://doi.org/10.1302/2058-5241.2.160023
Buchalter DB, Mahure SA, Mollon B, Yu S, Kwon YW, Zuckerman JD (2017) Two-stage revision for infected shoulder arthroplasty. J Shoulder Elbow Surg 26(6):939–947. https://doi.org/10.1016/j.jse.2016.09.056
Constant CR, Murley AH (1987) A clinical method of functional assessment of the shoulder. Clin Orthop Relat Res 214:160–164
Coste JS, Reig S, Trojani C, Berg M, Walch G, Boileau P (2004) The management of infection in arthroplasty of the shoulder. J Bone Jt Surg Br 86(1):65–69
Dillon MT, Chan PH, Inacio MCS, Singh A, Yian EH, Navarro RA (2017) Yearly trends in elective shoulder arthroplasty, 2005–2013. Arthritis Care Res (Hoboken) 69(10):1574–1581. https://doi.org/10.1002/acr.23167
Fink B, Sevelda F (2017) Periprosthetic joint infection of shoulder arthroplasties: diagnostic and treatment options. Biomed Res Int 2017:4582756. https://doi.org/10.1155/2017/4582756
Frank BJH, Aichmair A, Simon S, Schwarz GM, Dominkus M, Hofstaetter JG (2021) Analysis of culture positive first and second stage procedures in periprosthetic knee and hip joint infections. J Arthroplasty. https://doi.org/10.1016/j.arth.2021.01.074
Garrigues GE, Zmistowski B, Cooper AM, Green A, Group ICMS (2019) Proceedings from the 2018 International Consensus Meeting on Orthopedic Infections: the definition of periprosthetic shoulder infection. J Shoulder Elbow Surg 28(6S):S8–S12. https://doi.org/10.1016/j.jse.2019.04.034
George DA, Volpin A, Scarponi S, Haddad FS, Romano CL (2016) Does exchange arthroplasty of an infected shoulder prosthesis provide better eradication rate and better functional outcome, compared to a permanent spacer or resection arthroplasty? a systematic review. BMC Musculoskelet Disord 17:52. https://doi.org/10.1186/s12891-016-0901-6
Gilbart MK, Gerber C (2007) Comparison of the subjective shoulder value and the Constant score. J Shoulder Elbow Surg 16(6):717–721. https://doi.org/10.1016/j.jse.2007.02.123
Ince A, Seemann K, Frommelt L, Katzer A, Loehr JF (2005) One-stage exchange shoulder arthroplasty for peri-prosthetic infection. J Bone Jt Surg Br 87(6):814–818. https://doi.org/10.1302/0301-620X.87B6.15920
Jacquot A, Sirveaux F, Roche O, Favard L, Clavert P, Mole D (2015) Surgical management of the infected reversed shoulder arthroplasty: a French multicenter study of reoperation in 32 patients. J Shoulder Elbow Surg 24(11):1713–1722. https://doi.org/10.1016/j.jse.2015.03.007
Klatte TO, Junghans K, Al-Khateeb H et al (2013) Single-stage revision for peri-prosthetic shoulder infection: outcomes and results. Bone Jt J 95-B(3):391–395. https://doi.org/10.1302/0301-620X.95B3.30134
Meshram P, Rojas J, Joseph J, Zhou Y, McFarland E (2021) Midterm results of two-stage revision surgery for periprosthetic shoulder infection. Semin Arthroplasty. https://doi.org/10.1053/j.sart.2020.12.008
Padegimas EM, Maltenfort M, Ramsey ML, Williams GR, Parvizi J, Namdari S (2015) Periprosthetic shoulder infection in the United States: incidence and economic burden. J Shoulder Elbow Surg 24(5):741–746. https://doi.org/10.1016/j.jse.2014.11.044
Padolino A, Cataldo G, Tarallo L et al (2021) Implant sonication versus intraoperative tissue sample cultures for Periprosthetic Joint Infection (PJI) of shoulder arthroplasty. Acta Biomed 92(S3):e2021009. https://doi.org/10.23750/abm.v92iS3.11693
Plachel F, Siegert P, Ruttershoff K et al (2020) Long-term results of arthroscopic rotator cuff repair: a follow-up study comparing single-row versus double-row fixation techniques. Am J Sports Med. https://doi.org/10.1177/0363546520919120
Romano CL, Borens O, Monti L, Meani E, Stuyck J (2012) What treatment for periprosthetic shoulder infection? Results from a multicentre retrospective series. Int Orthop 36(5):1011–1017. https://doi.org/10.1007/s00264-012-1492-y10.1007/s00264-011-1467-4
Schairer WW, Nwachukwu BU, Lyman S, Craig EV, Gulotta LV (2015) National utilization of reverse total shoulder arthroplasty in the United States. J Shoulder Elbow Surg 24(1):91–97. https://doi.org/10.1016/j.jse.2014.08.026
Sperling JW, Kozak TK, Hanssen AD, Cofield RH (2001) Infection after shoulder arthroplasty. Clin Orthop Relat Res 382:206–216. https://doi.org/10.1097/00003086-200101000-00028
Strickland JP, Sperling JW, Cofield RH (2008) The results of two-stage re-implantation for infected shoulder replacement. J Bone Jt Surg Br 90(4):460–465. https://doi.org/10.1302/0301-620X.90B4.20002
Torrens C, Santana F, Puig L, Sorli L, Alier A (2018) Results of cement spacer sonication in the second stage of two-stage treatment of shoulder arthroplasty infection. J Orthop Surg Res 13(1):58. https://doi.org/10.1186/s13018-018-0763-8
Acknowledgements
We thank Sophie Bischofter for her involvement in the primary data collection.
Funding
None.
Author information
Authors and Affiliations
Contributions
All the listed authors have contributed substantially to this work: PS, JGH and BJHF for the study conception and design; PS, BJHF and SS for the data collection, PS, DM and AP-O for the data analysis; PS, DM and CW for the data interpretation; PS, JGH, BJHF and JD for the first drafting of the manuscript, the figures, and the literature research. All the authors contributed to the writing and critical reading of the final manuscript and approved it for submission.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Obtained.
Informed consent
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Siegert, P., Frank, B.J.H., Simon, S. et al. Changes in microbiological spectrum and antibiotic susceptibility in two-stage exchange for periprosthetic shoulder infections. Arch Orthop Trauma Surg 143, 3871–3878 (2023). https://doi.org/10.1007/s00402-022-04635-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-022-04635-7