Abstract
Introduction
Surgical site occurrences (SSO), including surgical site infection, dehiscence, and incisional hernia, are complications following laparotomy. SSO rates in premature neonates are poorly understood. We hypothesize that SSO rates are higher among extremely low birth weight (ELBW) infants compared to very low birth weight (VLBW) infants and strive to determine the optimal abdominal closure method for these infants.
Methods
We conducted a prospective observational study of infants < 1.5 kg (kg) undergoing laparotomy at two institutions from 1/1/2020 to 5/1/2022. Patients were grouped by weight and closure; SSO rates were computed and the association tested using Fisher’s exact test.
Results
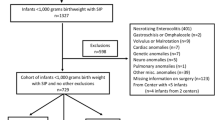
We identified 59 patients and 104 total operations. At initial surgery, 37 patients weighed < 1 kg (ELBW); 22 patients weighed 1–1.5 kg (VLBW). Complication rate for ELBW was 6(16%) vs. 2(9%) in VLBW, but not significant (p = 0.45). More complications followed a single-layer compared to a two-layer closure (18 vs. 2), but not significant (p = 0.30).
Conclusions
SSO rates are higher for ELBW infants undergoing laparotomy, and fewer complications follow two-layer closure. However, these findings did not reach statistical significance. Further studies are needed to identify modifiable factors to reduce postoperative complications in these infants.
Similar content being viewed by others
Data availability
The data for this study is available upon request.
Abbreviations
- ELBW:
-
Extremely low birthweight
- kg:
-
Kilogram
- SSO:
-
Surgical site occurrence
- VLBW:
-
Very low birthweight
References
Surgical site infection event (SSI). Natl Healthc Saf Netw Surg Site Infect Event 2022. https://www.cdc.gov/nhsn/pdfs/pscmanual/9pscssicurrent.pdf (Accessed 8 Aug 2022).
Ban KA, Minei JP, Laronga C, Harbrecht BG, Jensen EH, Fry DE et al (2017) American college of surgeons and surgical infection society: surgical site infection guidelines, 2016 update. J Am Coll Surg 224:59–74. https://doi.org/10.1016/j.jamcollsurg.2016.10.029
Zimlichman E, Henderson D, Tamir O, Franz C, Song P, Yamin CK et al (2013) Health care-associated infections: a meta-analysis of costs and financial impact on the US health care system. JAMA Intern Med 173:2039–2046. https://doi.org/10.1001/jamainternmed.2013.9763
Patel SV, Paskar DD, Nelson RL, Vedula SS, Steele SR (2017) Closure methods for laparotomy incisions for preventing incisional hernias and other wound complications. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD005661.pub2
Willy C, Engelhardt M, Stichling M, Grauhan O (2016) The impact of surgical site occurrences and the role of closed incision negative pressure therapy. Int Wound J 13:35–46. https://doi.org/10.1111/iwj.12659
Catania VD, Boscarelli A, Lauriti G, Morini F, Zani A (2019) Risk factors for surgical site infection in neonates: a systematic review of the literature and meta-analysis. Front Pediatr. https://doi.org/10.3389/fped.2019.00101
Bartz-Kurycki MA, Green C, Anderson KT, Alder AC, Bucher BT, Cina RA et al (2018) Enhanced neonatal surgical site infection prediction model utilizing statistically and clinically significant variables in combination with a machine learning algorithm. Am J Surg 216:764–777. https://doi.org/10.1016/j.amjsurg.2018.07.041
Clements KE, Fisher M, Quaye K, O’Donnell R, Whyte C, Horgan MJ (2016) Surgical site infections in the NICU. J Pediatr Surg 51:1405–1408. https://doi.org/10.1016/j.jpedsurg.2016.04.002
Woldemicael AY, Bradley S, Pardy C, Richards J, Trerotoli P, Giuliani S (2019) Surgical site infection in a tertiary neonatal surgery centre. Eur J Pediatr Surg Off J Austrian Assoc Pediatr Surg Al Z Kinderchir 29:260–265. https://doi.org/10.1055/s-0038-1636916
Segal I, Kang C, Albersheim SG, Skarsgard ED, Lavoie PM (2014) Surgical site infections in infants admitted to the neonatal intensive care unit. J Pediatr Surg 49:381–384. https://doi.org/10.1016/j.jpedsurg.2013.08.001
Eeftinck Schattenkerk LD, Musters GD, Coultre SEL, de Jonge WJ, van Heurn LE, Derikx JPM (2021) Incisional hernia after abdominal surgery in infants: a retrospective analysis of incidence and risk factors. J Pediatr Surg 56:2107–2112. https://doi.org/10.1016/j.jpedsurg.2021.01.037
Prasad PA, Wong-McLoughlin J, Patel S, Coffin SE, Zaoutis TE, Perlman J et al (2016) Surgical site infections in a longitudinal cohort of neonatal intensive care unit patients. J Perinatol Off J Calif Perinat Assoc 36:300–305. https://doi.org/10.1038/jp.2015.191
Kirk RM (1972) Effect of method of opening and closing the abdomen on incidence of wound bursting. Lancet 300:352–353. https://doi.org/10.1016/S0140-6736(72)91736-9
Goligher JC, Irvin TT, Johnston D, De Dombal FT, Hill GL, Horrocks JC (1975) A controlled clinical trial of three methods of closure of laparotomy wounds. Br J Surg 62:823–829. https://doi.org/10.1002/bjs.1800621019
Henriksen NA, Deerenberg EB, Venclauskas L, Fortelny RH, Miserez M, Muysoms FE (2018) Meta-analysis on materials and techniques for laparotomy closure: the MATCH review. World J Surg 42:1666–1678. https://doi.org/10.1007/s00268-017-4393-9
Luo W, Tao Y, Wang Y, Ouyang Z, Huang J, Long X (2022) Comparing running vs interrupted sutures for skin closure: a systematic review and meta-analysis. Int Wound J. https://doi.org/10.1111/iwj.13863
Chana RS, Saxena VC, Agarwal A (1993) A prospective study of closure techniques of abdominal incisions in infants and children. J Indian Med Assoc 91:59–61
Inoue M, Uchida K, Nagano Y, Matsushita K, Koike Y, Otake K et al (2018) Impact of relationship between the stoma site and the primary incision on occurrence of laparotomy wound infection in contaminated or dirty wound operations in neonates. Pediatr Surg Int 34:957–960. https://doi.org/10.1007/s00383-018-4310-9
Kronfli R, Maguire K, Walker GM (2013) Neonatal stomas: does a separate incision avoid complications and a full laparotomy at closure? Pediatr Surg Int 29:299–303. https://doi.org/10.1007/s00383-012-3234-z
Blakely ML, Tyson JE, Lally KP, Hintz SR, Eggleston B, Stevenson DK et al (2021) Initial laparotomy versus peritoneal drainage in extremely low birthweight infants with surgical necrotizing enterocolitis or isolated intestinal perforation: a multicenter randomized clinical trial. Ann Surg 274:e370–e380. https://doi.org/10.1097/SLA.0000000000005099
Funding
This research did not receive any specific grant from the funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
LL wrote the initial draft of the main manuscript text and created the database used for data management. NH performed the statistical analysis and prepared the tables. TN and CM collected data for the study and provided major edits to the main manuscript. KL developed the research question and supervised the research design, methodology, and provided major edits to the main manuscript. All authors reviewed the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest relevant to this article to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, L.T., Hebballi, N.B., Nguyen, T. et al. Complication rates in very low and extremely low birth weight infants following laparotomy: a prospective study. Pediatr Surg Int 39, 237 (2023). https://doi.org/10.1007/s00383-023-05520-z
Accepted:
Published:
DOI: https://doi.org/10.1007/s00383-023-05520-z