Abstract
Purpose
We monitored arterial blood gases during thoracoscopic (TR) and open repair (OR) of congenital diaphragmatic hernia (CDH) to assess the safety of intraoperative hypercapnia and acidosis.
Methods
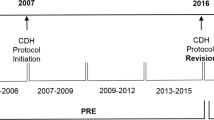
We reviewed 30 neonatal CDH cases (OR = 10, TR = 20) diagnosed prenatally or within 6 h of birth at out institution from 2002 to 2014 not requiring inhaled nitric oxide (NO) intraoperatively. OR, routine until 2006 was replaced by TR in 2007. All subjects were managed identically.
Results
Five TR cases requiring conversion to OR were excluded. Prenatal diagnosis, gestational age at birth, gender, birth weight, and side of CDH were similar. Preoperative PaCO2 and pH were not significantly different. However, while intraoperative increase in mean PaCO2 (38.8–62.8 mmHg; p < 0.01) and decrease in mean pH (7.44–7.25; p < 0.01) were significant in TR, intraoperative PaCO2 was <70 mmHg in 12/15 cases and intraoperative pH was >7.20 in 11/15 cases. Both PaCO2 and pH reverted to normal on completion of surgery; pre- and postoperative results were comparable. There were no postoperative complications.
Conclusions
It would appear that neonatal cases of CDH not requiring NO can tolerate TR, despite transient reversible deterioration in acid/base balance, indicating that TR is safe for the treatment of selected cases of CDH.


Similar content being viewed by others
References
der Zee Van, Bax NM (1995) Laparoscopic repair of congenital diaphragmatic hernia in a 6-month-old child. Surg Endosc 9:1001–1003
Silen ML, Canvasser DA, Kurkchubasche AG, Andrus CH, Naunheim KS (1995) Video-assisted thoracic surgical repair of a foramen of Bochdalek hernia. Ann Thorac Surg 60:448–450
Acra MJ, Barnhart DC, Lelli JL Jr, Greenfeld J, Harmon CM, Hirschl RB, Teitelbaum DH (2003) Early experience with minimally invasive repair of congenital diaphragmatic hernia: results and lessons learned. J Pediatr Surg 38:1563–1568
Yang EY, Allmendinger N, Johnson SM, Chen C, Wilson JM, Fishman SJ (2005) Neonatal thoracoscopic repair of congenital diaphragmatic hernia: selection criteria for successful outcome. J Pediatr Surg 40:1369–1375
Nguyen TL, Le AD (2006) Thoracoscopic repair for congenital diaphragmatic hernia: lessons from 45 cases. J Pediatr Surg 41:1713–1715
Tsao K, Lally PA, Lally KP, for the Congenital Diaphragmatic Hernia Study Group (2011) Minimally invasive repair of congenital diaphragmatic hernia. J Pediatr Surg 46:1158–1164
Okazaki T, Nishimura K, Takahashi T, Shoji H, Shimizu T, Tanaka T, Takeda S, Inada E, Lane GJ, Yamataka A (2011) Indications for thoracoscopic repair of congenital diaphragmatic hernia in neonates. Pediatr Surg Int 27:35–38
Okazaki T, Nishimura K, Koga H, Miyano G, Okawada M, Shoji H, Shimizu T, Makino S, Takeda S, Inada E, Lane GJ, Yamataka A (2012) Pulmonary artery size as an indication for thoracoscopic repair of congenital diaphragmatic hernia. Pediatr Surg Int 28:883–886
Tanaka T, Okazaki T, Fukatsu Y, Okawada M, Koga H, Miyano G, Ogasawara Y, Lane GJ, Yamataka A (2013) Surgical intervention for congenital diaphragmatic hernia: open versus thoracoscopic surgery. Pediatr Surg Int 29:1183–1186
Bishay M, Giacomello L, Retrosi G, Thyoka M, Garriboli M, Brierley J, Harding L, Scuplak S, Cross KM, Curry JI, Kiely EM, De Coppi P, Eaton S, Pierro A (2013) Hypercapnia and acidosis during open and thoracoscopic repair of congenital diaphragmatic hernia and esophageal atresia. Results of a pilot randomized control trail. Ann Surg 258:785–900
Okazaki T, Okawada M, Shiyanagi S, Shoji H, Shimizu T, Tanaka T, Takeda S, Kawashima K, Lane GJ, Yamataka A (2008) Significance of pulmonary artery size and blood flow as a predictor of outcome in congenital diaphragmatic hernia. Pediatr Surg Int 24:1369–1373
Gourlay DM, Cassidy LD, Sato TT, Lal DR, Arca MJ (2009) Beyond feasibility: a comparison of newborns undergoing thoracoscopic and open repair of congenital diaphragmatic hernias. J Pediatr Surg 44:1702–1707
McHoney M, Giacomello L, Nah SA, De Coppi P, Kiely EM, Curry JI, Drake DP, Eaton S, Pierro A (2010) Thoracoscopic repair of congenital diaphragmatic hernia: intraoperative ventilation and recurrence. J Pediatr Surg 45:355–359
Fishman JR, Blackburn SC, Jones NJ, Madden N, Caluwe DD, Haddad MJ, Clarke SA (2011) Does thoracoscopic congenital hernia repair cause a significant intraoperative acidosis when compared to an open abdominal repair? J Pediatr Surg 46:458–461
Liem NT, Dien TM, Ung NQ (2010) Thoracoscopic repair in the neonatal intensive care unit for congenital diaphragmatic hernia during high-frequency ventilation. J Laparoendosc Adv Surg Tech A 20:111–114
Mortellaro VE, Fike FB, Adibe OO, Juang D, Aguayo P, Ostlie DJ, Holcomb GW, St Peter SD (2011) The use of high-frequency oscillating ventilation to facilitate stability during neonatal thoracoscopic operations. J Laparoendosc Adv Surg Tech A 21:877–879
Keijzer R, van de Ven C, Vlot J, Sloots C, Madern G, Tibbol D, Bax K (2011) Thoracoscopic repair in congenital diaphragmatic hernia: patching is safe and reduces the recurrence rate. J Pediatr Surg 45:953–957
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Okazaki, T., Okawada, M., Koga, H. et al. Safety of surgery for neonatal congenital diaphragmatic hernia as reflected by arterial blood gas monitoring: thoracoscopic versus open repair. Pediatr Surg Int 31, 899–904 (2015). https://doi.org/10.1007/s00383-015-3767-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-015-3767-z