Abstract
Purpose
Hypothalamic hamartomas (HH) are malformations responsible for drug-resistant epilepsy. HH are usually isolated or part of a genetic syndrome, such as Pallister-Hall. Exceptionally they can be associated with other brain malformations such as polymicrogyria (PMG) and periventricular nodular heterotopia (PNH). We discuss the origin of the seizures associated with this combination of malformations, through electrophysiological studies, and review the literature on this rarely reported syndrome.
Methods
We retrospectively reviewed the patients with HH who had surgery between 1998 and 2020 and selected those with associated focal PMG and PNH, detected on MRIs. All patients had comprehensive clinical evaluation and surface video-EEG and one underwent stereoelectroencephalography (SEEG).
Results
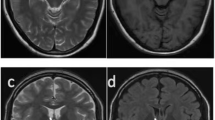
Three male patients out of 182 were identified with a mean age at surgery of 7.5 years. MRI showed unilateral focal PMG (fronto-insulo-parietal, fronto-insulo-parieto-opercular, and fronto-insular, respectively) and multiple PNH homolateral to the main HH implantation side. In two patients, there were strong clinical and scalp EEG arguments for seizure onset within the HH. In the third, due to abnormalities on scalp video-EEG in the same area as PMG and the lack of gelastic seizures, SEEG was indicated and demonstrated seizure onset within the hamartoma. With a mean follow-up of 6 years, two patients were seizure-free.
Conclusion
Our results show that HH is the trigger of epilepsy, which confirms the high epileptogenic potential of this malformation. In patients such as ours, as in those with isolated HH, we recommend to begin by operating the HH independently of seizure semiology or electrophysiological abnormalities.







Similar content being viewed by others
Availability of data and materials
All authors declare that all data and materials and software application or custom code support their published claims and comply with field standards.
References
Alves C, Barbosa V, Machado M (2013) Giant hypothalamic hamartoma: case report and literature review. Childs Nerv Syst 29:513–516. https://doi.org/10.1007/s00381-013-2022-y
Amado C, Amado J (2021) Letter to the editor regarding “hypothalamic hamartoma, gray matter heterotopia, and polymicrogyria in a boy: case report and literature review”. World Neurosurg 146:430. https://doi.org/10.1016/j.wneu.2020.09.172.
Arita K, Ikawa F, Kurisu K, Sumida M, Harada K, Uozumi T, Monden S, Yoshida J, Nishi Y (1999) The relationship between magnetic resonance imaging findings and clinical manifestations of hypothalamic hamartoma. J Neurosurg 91:212–220. https://doi.org/10.3171/jns.1999.91.2.0212
Berkovic S, Arzimanoglou A, Kuzniecky R, Harvey A, Palmini A, Andermann F (2003) Hypothalamic hamartoma and seizures: a treatable epileptic encephalopathy. Epilepsia 44:969–973. https://doi.org/10.1046/j.1528-1157.2003.59102.x
Delalande O, Fohlen M (2003) Disconnecting surgical treatment of hypothalamic hamartoma in children and adults with refractory epilepsy and proposal of a new classification. Neurol Med Chir 43:61–68. https://doi.org/10.2176/nmc.43.61
Engel JJ, Van Ness P, Rasmussen T, Ojemann L (1993) Outcome with respect to epileptic seizures. In: Engel JJ (ed) Surgical treatment of the epilepsies. Raven Press, New York, pp 609–621
Ferrand-Sorbets S, Fohlen M, Delalande O, Zuber K, Bulteau C, Levy M, Chamard P, Taussig D, Dorison N, Bekaert O, Tisdall M, Chipaux M, Dorfmüller G (2020) Seizure outcome and pronostic factors for surgical management of hypothalamic hamartoma in children. Seizure 75:28–33. https://doi.org/10.1016/j.seizure.2019.11.013
Freeman J, ColemanLT WR, Kean M, Rosenfeld J, Jackson G, Berkovic S, Harvey A (2004) MR imaging and spectroscopic study of epileptogenic hypothalamic hamartomas: analysis of 72 cases. Am J Neuroradiol 25:450–462
Freese K, Driess S, Bornholdt D, Shoenle E, Seidel H, Tinschert S, Grzeschik K-H, Kalff-Suske M (2003) Gene symbol: GLI3. Disease: Pallister-Hall syndrome. Hum Genet 112:103
Hall J, Pallister P, Clarren S, Beckwith J, Wiglesworth F, Fraser F, Cho S, Benke P, Reed S (1980) Congenital hypothalamic hamartoblastoma, hypopituitarism, imperforate anus and postaxial polydactyly–a new syndrome? Part I: clinical, causal, and pathogenetic considerations Case Reports Am J Med Genet 7:47–74. https://doi.org/10.1002/ajmg.1320070110
Hildebrand M, Griffin N, Damiano J, Cops E, Burgess R, Ozturk E, Jones N, Leventer R, Freeman J, Harvey A, Sadleir L, Scheffer I, Major H, Darbro B, Allen A, Goldstein D, Kerrigan J, Berkovic S, Heinzen E (2016) Mutations of the sonic hedgehog pathway underlie hypothalamic hamartoma with gelastic epilepsy. Am J Hum Genet 99:423–429. https://doi.org/10.1016/j.ajhg.2016.05.031
Kahane P, Ryvlin P, Hoffmann D, Minotti L, Benabid A (2003) From hypothalamic hamartoma to cortex: what can be learnt from depth recordings and stimulation? Epileptic Disord 5:205–217
Kahane P, Tassi LH, D, Francione S, Gratadou-Juery G, Pasquier BM, C, (1994) Crises dacrystiques et hamartome hypothalamique : à propos d’une observation vidéo-stéréo-EEG. Epilepsies 6:259–279
Kang S, Graham JJ, Olney A, Biesecker L (1997) GLI3 frameshift mutations cause autosomal dominant Pallister-Hall syndrome. Nat Genet 15:266–268. https://doi.org/10.1038/ng0397-266
Kerrigan J, Ng Y, Chung S, Rekate H (2005) The hypothalamic hamartoma: a model of subcortical epileptogenesis and encephalopathy. Semin Pediatr Neurol 12:119–131. https://doi.org/10.1016/j.spen.2005.04.002
Kuzniecky R, Guthrie B, Mountz J, Bebin M, Faught E, Gilliam F, Liu H (1997) Intrinsic epileptogenesis of hypothalamic hamartomas in gelastic epilepsy. Ann Neurol 42:60–67. https://doi.org/10.1002/ana.410420111
Lange-Cosack H (1951) Verschiedene Gruppen der hypothalamischen Pubertas praecox. Dtsch Z Nervenheilk 166:499–545
Leventer R, Jansen A, Pilz D, Stoodley N, Marini C, Dubeau F et al (2010) Clinical and imaging heterogeneity of polymicrogyria: a study of 328 patients. Brain 133:1415–1427. https://doi.org/10.1093/brain/awq078
List C, Dowman C, Bagchi B, Bebin J (1958) Posterior hypothalamic hamartomas and gangliogliomas causing precocious puberty. Neurology 8:164–174. https://doi.org/10.1212/wnl.8.3.164
Minotti L, Montavont A, Scholly J, Tyvaert L, Taussig D (2018) Indications and limits of stereoelectroencephalography (SEEG). Neurophysiologie clinique = Clinical neurophysiology 48:15–24. https://doi.org/10.1016/j.neucli.2017.11.006
Mullatti N, Selway R, Nashef L, Elwes R, Honavar M, Chandler C, Morris R, Jarosz J, Buchanan C, Polkey C (2003) The clinical spectrum of epilepsy in children and adults with hypothalamic hamartoma. Epilepsia 44:1310–1319
Schmidt E, Hallervorden J, Spatz H (1958) Die Entstehung der Hamartome am Hypothalamus mit und ohne pubertas praecox. Dtsch Z Nervenheilk 177:235–262
Scholly J, Staack A, Kahane P, Scavarda D, Régis J, Hirsch E, Bartolomei F (2017) Hypothalamic hamartoma: epileptogenesis beyond the lesion? Epilepsia 58. Suppl 2:32–40. https://doi.org/10.1111/epi.13755
Scholly J, Valenti M, Staack A, Strobl K, Bast T, Kehrli P, Steinhoff B, Hirsch E (2013) Hypothalamic hamartoma: is the epileptogenic zone always hypothalamic? Arguments for independent (third stage) secondary epileptogenesis. Epilepsia 54:123–128. https://doi.org/10.1111/epi.12456
Sculier C, Taussig D, David O, Blujstajn J, Ayoubian L, Bonheur J, Bulteau C, Chipaux M, Dorison N, Raffo E, Ferrand-Sorbets E, Dorfmüller G, Fohlen M (2021) Focal polymicrogyria in children: contribution of invasive explorations and epileptogenicity map** in the surgical decision. Seizure 86:19–28. https://doi.org/10.1016/j.seizure.2021.01.010
Striano S, Santulli L, Ianniciello M, Ferretti M, Romanelli P, Striano P (2012) The gelastic seizures-hypothalamic hamartomasyndrome: facts, hypotheses, and perspectives. Epilepsy Behav 24:7–13. https://doi.org/10.1016/j.yebeh.2012.02.013
Stutterd C, Leventer R (2014) Polymicrogyria: a common and heterogeneous malformation of cortical development. Am J Med Genet C Semin Med Genet. https://doi.org/10.1002/ajmg.c.31399
Tassi L, Colombo N, Cossu M, Mai R, Francione S, Lo Russo G, Galli C, Bramerio M, Battaglia G, Garbelli R, Meroni A, Spreafico R (2005) Electroclinical, MRI and neuropathological study of 10 patients with nodular heterotopia, with surgical outcomes. Brain 128:321–337. https://doi.org/10.1093/brain/awh357
Troester M, Haine-Schlagel R, Ng Y, Chapman K, Chung S, Drees C, Prenger E, Rekate H, Kerrigan J (2011) EEG and video-EEG seizure monitoring has limited utility in patients with hypothalamic hamartoma and epilepsy. Epilepsia 52:1137–1143. https://doi.org/10.1111/j.1528-1167.2011.03095.x
Tsugu H, Fukushima T, Nagashima T, Utsunomiya H, Tomonaga M, Mitsudome A (1998) Hypothalamic hamartoma associated with multiple congenital abnormalities. Two patients and a review of reported cases. Pediatr Neurosurg 29:290–296. https://doi.org/10.1159/000028739
Wang D, Shan Y, Bartolomei F, Kahane P, An Y, Li M, Zhang H, Fan X, Ou S, Yang Y, Wei P, Lu C, Wang Y, Du J, Ren L, Wang Y, Zhao G (2020) Electrophysiological properties and seizure networks in hypothalamic hamartoma. Ann Clin Transl Neurol 7:653–666
Zhang H, Li Y, Liu B, Shen L, Wang S, Yao H (2020) Hypothalamic hamartoma, gray matter heterotopia, and polymicrogyria in a boy: case report and literature review. World neurosurgery 142:396–400. https://doi.org/10.1016/j.wneu.2020.07.098
Acknowledgements
We are indebted to our EEG technologists Mrs M. Benghezal and Mrs I. Cheramy.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation was done by Martine Fohlen and Delphine Taussig; data collection was done by Tom Pieper, Serge Rivera, and Martine Fohlen. EEG analysis and EEG figures were done by Delphine Taussig. MRI analysis and MRI figures were done by Jerry Blustajn. The patients were operated on by Georg Dorfmuller and Sarah Ferrand Sorbets. The first draft of the manuscript was written by Martine Fohlen and Delphine Taussig and all authors commented on previous versions of the manuscript. English revision was done by Jerry Blustajn, a native English speaker. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Ethical approval was waived by the local Ethics Committee of Foundation Rothschild Hospital in view of the retrospective nature of the study, and all the procedures being performed were part of the routine care. The study was conducted in accordance with the declaration of Helsinki. Informed consent form was signed by the parents.
Consent for publication
All authors (1) made substantial contributions to the acquisition, analysis, and interpretation of data; 2) drafted or revised it the work critically for important intellectual content; (3) approved the version to be published; and (4) agreed to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Conflict of interest
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Fohlen, M., Taussig, D., Blustajn, J. et al. Hypothalamic hamartoma associated with polymicrogyria and periventricular nodular heterotopia in children: report of three cases and discussion of the origin of the seizures. Childs Nerv Syst 38, 1965–1975 (2022). https://doi.org/10.1007/s00381-022-05573-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-022-05573-w