Abstract
Purpose
This study aimed to identify the characteristics associated with the need for urinary intervention for a blunt renal injury with collection system involvement using a computed tomography (CT) protocol for trauma.
Materials and Methods
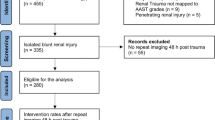
Abdominal CT images of patients with blunt renal injuries from 2016 to 2020 were reviewed. Patients with low-grade renal trauma, non-collecting system involvement, American Association for the Surgery of Trauma grade V shattered kidney, and emergent nephrectomy were excluded. The largest perinephric mass thickness was measured in the axial view using CT, and a cutoff value was obtained using a receiver-operating characteristic curve analysis. Risk factors for further urinary intervention were analyzed.
Results
Among the 70 patients included in this study, those with perinephric mass thicknesses < 25 mm (n = 36) had a significantly lower rate of urinary intervention than those with perinephric mass thicknesses ≥ 25 mm (0 vs. 5; p = 0.023). There was no significant difference in the follow-up durations of the groups (19 days vs. 38 days; p = 0.198). More than 90% of the perinephric mass in the < 25 mm group resolved within a median follow-up duration of 38 days, whereas nearly half of the ≥ 25 mm group had a residual perinephric mass during a median follow-up duration of 19 days.
Conclusion
The initial CT protocol for trauma was useful for predicting the need for further urinary interventions for collecting system injuries. A perinephric mass thickness < 25 mm is predictive of a low likelihood of requiring urinary intervention.



Similar content being viewed by others
Data availability
The datasets analyzed during the current study are not publicly available due to institutional policy but are available from the corresponding author upon reasonable request.
Abbreviations
- AAST:
-
American Association for the Surgery of Trauma
- AUA:
-
American Urological Association
- AUC:
-
Areas under the ROC curve
- BMI:
-
Body mass index
- CI:
-
Confidence interval
- CT:
-
Computed tomography
- EAU:
-
European Association of Urology
- ED:
-
Emergency department
- GU:
-
Genitourinary
- HGRT:
-
High-grade renal trauma
- ICU LOS:
-
Length of stay in intensive care unit stay
- ISS:
-
Injury Severity Score
- LOS:
-
Length of stay in hospital
- ROC:
-
Receiver operating characteristic
- RTS:
-
Revised Trauma Score
- SD:
-
Standard Deviation
- TAE:
-
Trans-arterial embolization
- TRISS:
-
Trauma Injury Severity Score
References
Paparel P, N’Diaye A, Laumon B et al (2006) The epidemiology of trauma of the genitourinary system after traffic accidents: analysis of a register of over 43,000 victims. BJU Int 97:338–341
Keihani S, Anderson RE, Hotaling JM, Myers JB (2019) Diagnosis and management of urinary extravasation after high-grade renal trauma. Nat Rev Urol 16:54–64
Kozar RA, Crandall M, Shanmuganathan K et al (2018) Organ injury scaling 2018 update: Spleen, liver, and kidney. J Trauma Acute Care Surg 85:1119–1122
Koch GE, Huang JJ, Walton WJ et al (2021) The impact of delayed-phase imaging at admission on the management of urinary extravasation in high-grade renal trauma. J Urol 206:1373–1379
Chiron P, Hornez E, Boddaert G et al (2016) Grade IV renal trauma management. A revision of the AAST renal injury grading scale is mandatory. Eur J Trauma Emerg Surg 42:237–241
Ballon-Landa E, Raheem OA, Fuller TW et al (2019) Renal trauma classification and management: Validating the revised renal injury grading scale. J Urol 202:994–1000
Kitrey ND (2022) EAU Guidelines on Renal Trauma 2022. In: EAU Guidelines Office. Arnhem, the Netherlands
Keihani S, Anderson RE, Fiander M et al (2018) Incidence of urinary extravasation and rate of ureteral stenting after high-grade renal trauma in adults: a meta-analysis. Transl Androl Urol 7:S169–S178
Locke JA, Neu S, Navaratnam R et al (2021) Management of high-grade renal traumas with collecting system injuries. Can Urol Assoc J 15:E588–E592
Hardee MJ, Lowrance W, Stevens MH et al (2013) Process improvement in trauma. J Trauma Acute Care Surg 74:558–562
(2022) EAU Guidelines on Renal Trauma 2022. EAU Guidelines on Renal Trauma
Alsikafi NF, McAninch JW, Elliott SP, Garcia M (2006) Nonoperative management outcomes of isolated urinary extravasation following renal lacerations due to external trauma. J Urol 176:2494–2497
Jung H, Osther PJS (2015) Intraluminal pressure profiles during flexible ureterorenoscopy. Springerplus 4:373
Morey AF, Broghammer JA, Hollowell CMP et al (2021) Urotrauma guideline 2020: AUA guideline. J Urol 205:30–35
Chebbi A, Peyronnet B, Giwerc A et al (2021) Observation vs. early drainage for grade IV blunt renal trauma: a multicenter study. World J Urol 39:963–969
Presti JC Jr, Carroll PR, McANINCH JW (1989) Ureteral and renal pelvic injuries from external trauma. J Trauma 29:370–374
Zemp L, Mann U, Rourke KF (2018) Perinephric hematoma size is independently associated with the need for urological intervention in multisystem blunt renal trauma. J Urol 199:1283–1288
Nuss GR, Morey AF, Jenkins AC et al (2009) Radiographic predictors of need for angiographic embolization after traumatic renal injury. J Trauma 67:578–582
Lin W-C, Lin C-H, Chen J-H et al (2013) Computed tomographic imaging in determining the need of embolization for high-grade blunt renal injury. J Trauma Acute Care Surg 74:230–235
Davis P, Bultitude MF, Koukounaras J et al (2010) Assessing the usefulness of delayed imaging in routine followup for renal trauma. J Urol 184:973–977
Acknowledgements
The authors thank Yu-Ching Wang for the statistical assistance and acknowledge the support of the Maintenance Project of the Center for Big Data Analytics and Statistics (grant CLRPG3N0011) at Chang Gung Memorial Hospital for study design and monitoring and data analysis and interpretation.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
Po-Ting Lin: Data collection, data analysis, manuscript writing. Yu-Hsiang Lin: Project development, manuscript editing Yu-San Tee: Project development, data analysis, manuscript editing. Chi-Tung Cheng: Project development, data analysis. Chien-Hung Liao: Project development. Chi-Hsun Hsieh: Project development. Chih-Yuan Fu: Project development, data collection.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lin, PT., Lin, YH., Tee, YS. et al. Does a collecting system injury with grade iv renal blunt trauma always need urinary intervention?. World J Urol 42, 15 (2024). https://doi.org/10.1007/s00345-023-04710-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00345-023-04710-7