Abstract
Objectives
To develop and validate a machine learning model based on contrast-enhanced CT to predict the risk of occurrence of the composite clinical endpoint (hospital-based intervention or death) in cirrhotic patients with acute variceal bleeding (AVB).
Methods
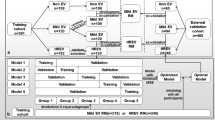
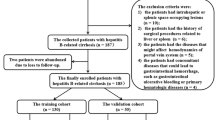
This retrospective study enrolled 330 cirrhotic patients with AVB between January 2017 and December 2020 from three clinical centers. Contrast-enhanced CT and clinical data were collected. Centers A and B were divided 7:3 into a training set and an internal test set, and center C served as a separate external test set. A well-trained deep learning model was applied to segment the liver and spleen. Then, we extracted 106 original features of the liver and spleen separately based on the Image Biomarker Standardization Initiative (IBSI). We constructed the Liver-Spleen (LS) model based on the selected radiomics features. The performance of LS model was evaluated by receiver operating characteristics and calibration curves. The clinical utility of models was analyzed using decision curve analyses (DCA).
Results
The LS model demonstrated the best diagnostic performance in predicting the composite clinical endpoint of AVB in patients with cirrhosis, with an AUC of 0.782 (95% CI 0.650–0.882) and 0.789 (95% CI 0.674–0.878) in the internal test and external test groups, respectively. Calibration curves and DCA indicated the LS model had better performance than traditional clinical scores.
Conclusion
A novel machine learning model outperforms previously known clinical risk scores in assessing the prognosis of cirrhotic patients with AVB
Clinical relevance statement
The Liver-Spleen model based on contrast-enhanced CT has proven to be a promising tool to predict the prognosis of cirrhotic patients with acute variceal bleeding, which can facilitate decision-making and personalized therapy in clinical practice.
Key Points
• The Liver-Spleen machine learning model (LS model) showed good performance in assessing the clinical composite endpoint of cirrhotic patients with AVB (AUC ≥ 0.782, sensitivity ≥ 80%).
• The LS model outperformed the clinical scores (AUC ≤ 0.730, sensitivity ≤ 70%) in both internal and external test cohorts.



Similar content being viewed by others
Abbreviations
- ALBI:
-
Albumin–bilirubin
- ARS:
-
Admission Rockall score
- AUC:
-
Area under the curve
- AVB:
-
Acute variceal bleeding
- CTP:
-
Child-Turcotte-Pugh score
- DCA:
-
Decision curve analysis
- GBS:
-
Glasgow-Blatchford score
- IBSI:
-
Image Biomarker Standardization Initiative
- LS:
-
Liver-Spleen
- MELD:
-
Model for End-Stage Liver Disease
- ROC:
-
Receiver operating characteristics
- UGIB:
-
Upper gastrointestinal bleeding
References
Ibrahim M, Mostafa I, Devière J (2018) New developments in managing variceal bleeding. Gastroenterology 154:1964–1969
Diaz-Soto MP, Garcia-Tsao G (2022) Management of varices and variceal hemorrhage in liver cirrhosis: a recent update. Therap Adv Gastroenterol 15:175628482211017
Takehara T, Sakamori R (2020) Remaining challenges for the noninvasive diagnosis of esophageal varices in liver cirrhosis. Esophagus 17:19–24
Reverter E, Tandon P, Augustin S et al (2014) A MELD-based model to determine risk of mortality among patients with acute variceal bleeding. Gastroenterology 146:412-419.e3
Fortune BE, Garcia-Tsao G, Ciarleglio M et al (2017) Child-Turcotte-Pugh Class is best at stratifying risk in variceal hemorrhage: analysis of a US multicenter prospective study. J Clin Gastroenterol 51:446–453
Jairath V, Rehal S, Logan R et al (2014) Acute variceal haemorrhage in the United Kingdom: patient characteristics, management and outcomes in a nationwide audit. Dig Liver Dis 46:419–426
Yang L, Sun R, Wei N, Chen H (2021) Systematic review and meta-analysis of risk scores in prediction for the clinical outcomes in patients with acute variceal bleeding. Ann Med 53:1806–1815
Xu F, Zhang L, Wang Z et al (2021) A new scoring system for predicting in-hospital death in patients having liver cirrhosis with esophageal varices. Front Med 8:1–12
Stanley AJ, Laine L, Dalton HR et al (2017) Comparison of risk scoring systems for patients presenting with upper gastrointestinal bleeding: international multicentre prospective study. BMJ 356:1–8
Guha IN, Harris R, Berhane S et al (2019) Validation of a model for identification of patients with compensated cirrhosis at high risk of decompensation. Clin Gastroenterol Hepatol 17:2330-2338.e1
La Huo T, Lee SD, Lin HC (2008) Selecting an optimal prognostic system for liver cirrhosis: the model for end-stage liver disease and beyond. Liver Int 28:606–613
Motola-Kuba M, Escobedo-Arzate A, Tellez-Avila F et al (2016) Validation of prognostic scores for clinical outcomes in cirrhotic patients with acute variceal bleeding. Ann Hepatol 15:895–901
Tantai XX, Liu N, Yang LB et al (2019) Prognostic value of risk scoring systems for cirrhotic patients with variceal bleeding. World J Gastroenterol 25:6668–6680
Robertson M, Ng J, Abu Shawish W et al (2020) Risk stratification in acute variceal bleeding: comparison of the AIMS65 score to established upper gastrointestinal bleeding and liver disease severity risk stratification scoring systems in predicting mortality and rebleeding. Dig Endosc 32:761–768
Shung DL, Au B, Taylor RA et al (2020) Validation of a machine learning model that outperforms clinical risk scoring systems for upper gastrointestinal bleeding. Gastroenterology 158:160–167
Park HJ, Park B, Lee SS (2020) Radiomics and deep learning: hepatic applications. Korean J Radiol 21:387–401
Wang J, Tang S, Mao Y et al (2022) Radiomics analysis of contrast-enhanced CT for staging liver fibrosis: an update for image biomarker. Hepatol Int 16:627–639
Milletari F, Navab N, Ahmadi SA (2016) V-Net: fully convolutional neural networks for volumetric medical image segmentation. Proc - 2016 4th Int Conf 3D Vision, 3DV 2016 565–571.
Yu Q, Huang Y, Li X et al (2022) An imaging-based artificial intelligence model for non-invasive grading of hepatic venous pressure gradient in cirrhotic portal hypertension. Cell Reports Med 3:100563
Yu Q, Xu C, Li Q, et al (2022) Spleen volume-based non-invasive tool for predicting hepatic decompensation in patients with compensated cirrhosis. JHEP Reports 100575.
Zwanenburg A, Vallières M, Abdalah MA et al (2020) The image biomarker standardization initiative: standardized quantitative radiomics for high-throughput image-based phenoty**. Radiology 295:328–338
Kalkhoran S, Benowitz NL, Rigotti NA (2018) Computational radiomics system to decode the radiographic phenotype. Rev del Col Am Cardiol 72:2964–2979
Fitzgerald M, Saville BR, Lewis RJ (2015) Decision curve analysis. JAMA 313:409–410
Chen S, Feng S, Wei J et al (2019) Pretreatment prediction of immunoscore in hepatocellular cancer: a radiomics-based clinical model based on Gd-EOB-DTPA-enhanced MRI imaging. Eur Radiol 29:4177–4187
Kim S, Shin J, Kim DY et al (2019) Radiomics on gadoxetic acid-enhanced magnetic resonance imaging for prediction of postoperative early and late recurrence of single hepatocellular carcinoma. Clin Cancer Res 25:3847–3855
Ji GW, Zhu FP, Zhang YD et al (2019) A radiomics approach to predict lymph node metastasis and clinical outcome of intrahepatic cholangiocarcinoma. Eur Radiol 29:3725–3735
Park HJ, Lee SS, Park B et al (2019) Radiomics analysis of gadoxetic acid–enhanced MRI for staging liver fibrosis. Radiology 290:380–387
Lin Y, Li L, Yu D et al (2021) A novel radiomics–platelet nomogram for the prediction of gastroesophageal varices needing treatment in cirrhotic patients. Hepatol Int 15:995–1005
Yan Y, Li Y, Fan C et al (2022) A novel machine learning-based radiomic model for diagnosing high bleeding risk esophageal varices in cirrhotic patients. Hepatol Int 16:423–432
Mohammad AN, Morsy KH, Ali MA (2016) Variceal bleeding in cirrhotic patients: what is the best prognostic score? Turkish J Gastroenterol 27:464–469
Funding
This study has received funding by the National Key R&D Program of China (2021YFF0501504), the National Natural Science Foundation of China (NSFC, Nos. 81830053, 92059202, and 61821002), and the Key Research and Development Program of Jiangsu Province (BE2020717).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Prof. Shenghong Ju.
Conflict of interest
The authors declare no competing interests.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was waived by the Institutional Review Board.
Ethical approval
Institutional Review Board approval was obtained.
Methodology
-
retrospective
-
diagnostic or prognostic study
-
multicenter study
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Yin Gao and Qian Yu are primary authors and contributed equally.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gao, Y., Yu, Q., Li, X. et al. An imaging-based machine learning model outperforms clinical risk scores for prognosis of cirrhotic variceal bleeding. Eur Radiol 33, 8965–8973 (2023). https://doi.org/10.1007/s00330-023-09938-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-023-09938-w