Abstract
Objectives
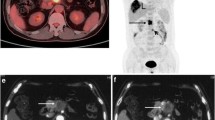
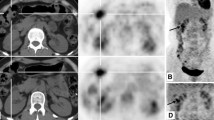
Diagnosing ampullary and duodenal papillary carcinomas (ADPCs) is challenging. In the present study, we investigated the application value of 18F-fluorodeoxyglucose positron emission tomography/computed tomography (18F-FDG PET/CT) in the preoperative evaluation of these tumours.
Methods
18F-FDG PET/CT images of 58 patients with ADPC and 28 patients with benign disease were retrospectively analysed. Preoperative 18F-FDG PET/CT was compared to contrast-enhanced (CE) CT and magnetic resonance imaging (MRI) in terms of diagnostic efficacy, certainty, staging and impact on treatment decisions.
Results
18F-FDG PET/CT showed a high sensitivity (93.1%) and a medium specificity (78.6%) for diagnosing ADPC. Compared to CE CT/MRI, 18F-FDG PET/CT had a higher diagnostic specificity (78.6 vs. 35.7%, p = 0.001) but a similar sensitivity (93.1 vs. 89.6%, p = 0.508). 18F-FDG PET/CT provided a much higher diagnostic certainty than CE CT/MRI (definite reports, 88.4 vs. 50.0%, χ2 = 29.698, p < 0.001), especially for small tumours ≤ 1.5 cm, and found distant metastases in five patients. The 18F-FDG PET/CT findings affected the treatment plans of 11 patients and improved the confidence in the diagnoses of 28 patients.
Conclusions
The present study demonstrated that 18F-FDG PET/CT can supplement CE CT/MRI to provide a more accurate diagnosis for ADPC, and thus, plays an important role in the decision-making process before complicated pancreaticoduodenectomy procedures.
Key Points
• It is a challenge for CT and MRI to diagnose ampullary carcinoma, especially at their early stage.
• Our study demonstrated that the benefit of PET/CT was improving the diagnostic confidence for ampullary and duodenal papillary carcinomas.
• 18 F-FDG PET/CT can change the treatment decision for ampullary and duodenal papillary carcinomas.





Similar content being viewed by others
Abbreviations
- 18F-FDG:
-
18F-fluorodeoxyglucose
- ADPC:
-
Ampullary and duodenal papillary carcinomas
- CE:
-
Contrast-enhanced
- CBD:
-
Common bile duct
- CT:
-
Computed tomography
- ERCP:
-
Endoscopic retrograde cholangiopancreatography
- EUS:
-
Duodenal endoscopy with endoscopic ultrasound
- MRCP:
-
Magnetic resonance cholangiopancreatography
- MRI:
-
Magnetic resonance imaging
- OSEM:
-
Ordered subset expectation maximisation
- PACS:
-
Picture Archiving and Communication Systems
- PD:
-
Pancreaticoduodenectomy
- PET/CT:
-
Positron emission tomography/computed tomography
- ROI:
-
Region of interest
- SUVmax:
-
Maximum standardised uptake value
References
Miyakawa S, Ishihara S, Takada T et al (2018) Flowcharts for the management of biliary tract and ampullary carcinomas. J Hepatobiliary Pancreat Surg 15(1):7–14
Pea A, Riva G, Bernasconi R et al (2018) Ampulla of Vater carcinoma: molecular landscape and clinical implications. World J Gastrointest Oncol 10(11):370–380
Kandler J, Neuhaus H (2018) How to approach a patient with ampullary lesion. Gastroenterology 155(6):1670–1676
Li S, Wang Z, Cai F et al (2019) New experience of endoscopic papillectomy for ampullary neoplasms. Surg Endosc 33(2):612–619
Bae JS, Kim JH, Joo I, Chang W, Han J (2019) MDCT findings predicting postoperative residual tumor and survival in patients with pancreatic cancer. Eur Radiol 29(7):3714–3724
Fernandez Y Viesca M, Arvanitakis M (2019) Early diagnosis and management of malignant distal biliary obstruction: a review on current recommendations and guidelines. Clin Exp Gastroenterol 12:415–432
Mendonca EQ, Bernardo WM, Moura EG (2016) Endoscopic versus surgical treatment of ampullary adenomas: a systematic review and meta-analysis. Clinics (Sao Paulo) 71(1):28–35
Zbar AP, Maor Y, Czerniak A (2012) Imaging tumours of the ampulla of Vater. Surg Oncol 21(4):293–298
Heinzow HS, Kammerer S, Rammes C, Wessling J, Domagk D, Meister T (2014) Comparative analysis of ERCP, IDUS, EUS and CT in predicting malignant bile duct strictures. World J Gastroenterol 20(30):10495–10503
Angthong W, Jiarakoop K, Tangtiang K (2018) Differentiation of benign and malignant ampullary obstruction by multirow detector CT. Jpn J Radiol 36(8):477–488
Cloyd JM (2019) Staging for ampullary carcinoma: is less actually more? Ann Surg Oncol 26(6):1598–1600
Iyer NG, Clark JR, Singham S, Zhu J (2010) Role of pretreatment 18FDG-PET/CT in surgical decision-making for head and neck cancers. Head Neck 32(9):1202–1208
Al-Ibraheem A, Buck A, Krause BJ, Scheidhauer K, Schwaiger M (2009) Clinical applications of FDG PET and PET/CT in head and neck cancer. J Oncol. https://doi.org/10.1155/2009/208725
Bruzzi JF, Munden RF (2006) PET/CT imaging of lung cancer. J Thorac Imaging 21(2):123–136
Bruzzi JF, Munden RF, Truong MT et al (2007) PET/CT of esophageal cancer: its role in clinical management. Radiographics 27(6):1635–1652
Schiepers C (2003) PET/CT in colorectal cancer. J Nucl Med 44(11):1804–1805
Macapinlac HA (2004) FDG PET and PET/CT imaging in lymphoma and melanoma. Cancer J 10(4):262–270
Wu HB, Wang QS, Li BY, Li HS, Zhou Wl, Wang QY (2011) F-18 FDG in conjunction with 11C-choline PET/CT in the diagnosis of hepatocellular carcinoma. Clin Nucl Med 36(12):1092–1097
Sun CH, Li X, Chan T et al (2013) Multidetector computed tomography (MDCT) manifestations of the normal duodenal papilla. Eur J Radiol 82(6):918–922
Qayyum A, Tamm EP, Lalani T et al (2017) ACR Appropriateness Criteria® staging of pancreatic ductal adenocarcinoma. J Am Coll Radiol 14(11S):S560–S569
Choi JY, Kim MJ, Lee JM et al (2008) Magnetic resonance cholangiography: comparison of two- and three-dimensional sequences for assessment of malignant biliary obstruction. Eur Radiol 18(1):78–86
Artifon EL, Couto D, Sakai P, da Silveira EB (2009) Prospective evaluation of EUS versus CT scan for staging of ampullary cancer. Gastrointest Endosc 70(2):290–296
Onishchenko SV, Darvin VV, Klimova NV, Krasnov EA (2018) The features of opisthorchiasis papillitis diagnosis. Khirurgiia (Mosk) (5):33–39
Acknowledgements
We thank our colleagues at Nanfang PET Center who manufactured the radiopharmaceuticals and performed the PET/CT scans. We also express our appreciation to our colleagues at the Department of Hepatobiliary Surgery and Pathology in Nanfang Hospital who provided the follow-up data and pathologic diagnosis.
Funding
This study has received funding from the National Natural Science Foundation Project of China (81371591, 81873905).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Hubing Wu.
Conflict of interest
The authors declare that they have no conflict of interest.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
The Institutional Review Board of Nanfang Hospital at Southern Medical University approved the present retrospective study and waived the requirement for written informed consent because of the retrospective nature of the study.
Ethical approval
Institutional Review Board approval was obtained.
Methodology
• retrospective
• diagnostic or prognostic study
• performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wen, G., Gu, J., Zhou, W. et al. Benefits of 18F-FDG PET/CT for the preoperative characterisation or staging of disease in the ampullary and duodenal papillary. Eur Radiol 30, 5089–5098 (2020). https://doi.org/10.1007/s00330-020-06864-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-020-06864-z