Abstract
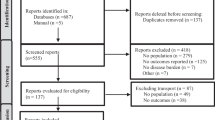
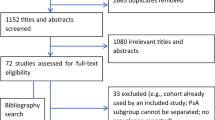
Systematic reviews and meta-analysis evaluating the prevalence, incidence, and psychological comorbidities of psoriatic arthritis (PsA) are increasing, so it’s time to perform an overview of systematic reviews. To summarize the pooled prevalence, incidence, and psychological comorbidities rates of PsA, and to explore possible continent disparities. In this overview of systematic reviews the CINAHL, EMBASE, PsycINFO, and PubMed were searched to October 25, 2023. This overview included systematic reviews with meta-analysis of people with PsA, providing the pooled prevalence or incidence rates of PsA in general, or clinical populations and/or psychological comorbidities. The Preferred Reporting Items for Overviews of Reviews (PRIOR) statement was followed. AMSTAR-2 assessed the quality of reviews. The degree of overlap was calculated using the corrected covered area (CCA). Maps were developed using the location of where primary studies were conducted using DataWrapper App. The protocol was prospectively registered with Open Science Framework registry. Pooled prevalence and incidence rates of PsA or its associated psychological comorbidities in general or specific populations. We also collected locations from the primary studies of the included meta-analyses. Only the assessment of prevalence rates of PsA in people with psoriasis showed slight overlap (CCA = 3.3%). Items 2, 3, 4, 7, 8, 10, 12, and 13 were poorly reported in AMSTAR-2. The pooled prevalence of PsA ranged from 0.13 to 0.15% in the general population, and 15.5% to 19.7% in people with psoriasis. The pooled incidence of PsA ranged from 8.26 to 9.27 cases per 100,000 inhabitants to 0.87 cases in individuals with hidradenitis suppurativa. The pooled prevalence of psychological comorbidities was 11.9–20% for depression, 19–33% anxiety, 38% alexithymia, and 72.9% in poor sleep quality. Only the pooled incidence of depression was assessed with 21.3 per 1000-person year. PsA seems to be prevalent and incident not only in people with psoriasis, but also in general population. Depression and anxiety symptoms may be present in some patients with PsA. Finally, continent disparities exist, and methodological and clinical issues were found, which could be helpful in the future agenda of the epidemiology of PsA.
Graphical abstract




Similar content being viewed by others
Data availability
There are no data available.
References
Merola JF, Chakravarty SD, Choi O, Chan D, Gottlieb AB (2024) A clinical review of structural damage in psoriatic arthritis for dermatologists: from pathogenesis to ongoing controversies. J Am Acad Dermatol 90:349–357. https://doi.org/10.1016/j.jaad.2023.10.021
Ritchlin CT, Colbert RA, Gladman DD (2017) Psoriatic arthritis. N Engl J Med 376:957–970. https://doi.org/10.1056/NEJMra1505557
Tucker L, Allen A, Chandler D, Ciurtin C, Dick A, Foulkes A et al (2022) The 2022 British Society for rheumatology guideline for the treatment of psoriatic arthritis with biologic and targeted synthetic DMARDs. Rheumatology 61:e255–e266. https://doi.org/10.1093/rheumatology/keac295
Singh JA, Guyatt G, Ogdie A, Gladman DD, Deal C, Deodhar A et al (2019) 2018 American college of rheumatology/national psoriasis foundation guideline for the treatment of psoriatic arthritis. Arthritis Rheumatol 71:5–32. https://doi.org/10.1002/art.40726
Gossec L, Baraliakos X, Kerschbaumer A, de Wit M, McInnes I, Dougados M et al (2020) EULAR recommendations for the management of psoriatic arthritis with pharmacological therapies: 2019 update. Ann Rheum Dis 79(700):1–712. https://doi.org/10.1136/annrheumdis-2020-217159
Ishchenko A, Pazmino S, Neerinckx B, Lories R, de Vlam K (2024) Comorbidities in early psoriatic arthritis: data from the metabolic disturbances in psoriatic arthritis cohort study. Arthritis Care Res (Hoboken) 76:231–240. https://doi.org/10.1002/acr.25230
Orbai AM, de Wit M, Mease P, Shea JA, Gossec L, Leung YY et al (2017) International patient and physician consensus on a psoriatic arthritis core outcome set for clinical trials. Ann Rheum Dis 76:673–680. https://doi.org/10.1136/annrheumdis-2016-210242
Haugeberg G, Hoff M, Kavanaugh A, Michelsen B (2020) Psoriatic arthritis: exploring the occurrence of sleep disturbances, fatigue, and depression and their correlates. Arthritis Res Ther 22:198. https://doi.org/10.1186/s13075-020-02294-w
Haugeberg G, Lund Nilsen TI, Kavanaugh A, Thomsen RS, Gulati AM, Hoff M (2021) Physical and psychosocial burden of psoriatic arthritis: longitudinal data from a population-based study in Norway. Arthritis Care Res (Hoboken) 73:138–145. https://doi.org/10.1002/acr.24412
Tobin AM, Sadlier M, Collins P, Rogers S, FitzGerald O, Kirby B (2017) Fatigue as a symptom in psoriasis and psoriatic arthritis: an observational study. Br J Dermatol 176:827–828. https://doi.org/10.1111/bjd.15258
Toledano E, Hidalgo C, Gómez-Lechón L, Ibáñez M, Chacón CC, Martín-Vallejo J, Pastor S, Montilla C (2023) SLEEP quality in patients with psoriatic arthritis and its relationship with disease activity and comorbidities: a cross-sectional study. Sci Rep 13:22927. https://doi.org/10.1038/s41598-023-48723-z
Mathew AJ, Chandran V (2020) Depression in psoriatic arthritis: dimensional aspects and link with systemic inflammation. Rheumatol Ther 7:287–300. https://doi.org/10.1007/s40744-020-00207-6
Husted JA, Tom BD, Farewell VT, Gladman DD (2012) Longitudinal study of the bidirectional association between pain and depressive symptoms in patients with psoriatic arthritis. Arthritis Care Res (Hoboken) 64:758–765. https://doi.org/10.1002/acr.21602
Parperis K, Kyriakou A, Voskarides K, Koliou E, Evangelou M, Chatzittofis A (2023) Insights into suicidal behavior among psoriatic arthritis patients: a systematic review and a genetic linkage disequilibrium analysis. Semin Arthritis Rheum 62:152241. https://doi.org/10.1016/j.semarthrit.2023.152241
Tang FY, **ong Q, Gan T, Yuan L, Liao Q, Yu YF (2022) The prevalence of alexithymia in psoriasis: a systematic review and meta-analysis. J Psychosom Res 161:111017. https://doi.org/10.1016/j.jpsychores.2022.111017
Zhao SS, Miller N, Harrison N, Duffield SJ, Dey M, Goodson NJ (2020) Systematic review of mental health comorbidities in psoriatic arthritis. Clin Rheumatol 39:217–225. https://doi.org/10.1007/s10067-019-04734-8
Gupta S, Syrimi Z, Hughes DM, Zhao SS (2021) Comorbidities in psoriatic arthritis: a systematic review and meta-analysis. Rheumatol Int 41:275–284. https://doi.org/10.1007/s00296-020-04775-2
Kamalaraj N, El-Haddad C, Hay P, Pile K (2019) Systematic review of depression and anxiety in psoriatic arthritis. Int J Rheum Dis 22:967–973. https://doi.org/10.1111/1756-185X.13553
Zusman EZ, Howren AM, Park JYE, Dutz J, De Vera MA (2020) Epidemiology of depression and anxiety in patients with psoriatic arthritis: a systematic review and meta-analysis. Semin Arthritis Rheum 50:1481–1488. https://doi.org/10.1016/j.semarthrit.2020.02.001
Taylor W, Gladman D, Helliwell P, Marchesoni A, Mease P, Mielants H, CASPAR Study Group (2006) Classification criteria for psoriatic arthritis: development of new criteria from a large international study. Arthritis Rheum 54:2665–2673. https://doi.org/10.1002/art.21972
Villani AP, Rouzaud M, Sevrain M, Barnetche T, Paul C, Richard MA et al (2015) Prevalence of undiagnosed psoriatic arthritis among psoriasis patients: systematic review and meta-analysis. J Am Acad Dermatol 73:242–248. https://doi.org/10.1016/j.jaad.2015.05.001
Gates M, Gates A, Pieper D, Fernandez RM, Tricco AC, Moher D et al (2022) Reporting guideline for overviews of reviews of healthcare interventions: development of the PRIOR statement. BMJ 378:e070849. https://doi.org/10.1136/bmj-2022-070849
Beller EM, Glasziou PP, Altman DG, Hopewell S, Bastian H, Chalmers I et al (2013) PRISMA for abstracts: reporting systematic reviews in journal and conference abstracts. PLoS Med 10:e1001419. https://doi.org/10.1371/journal.pmed.1001419
Morgan RL, Whaley P, Thayer KA, Schünemann HJ (2018) Identifying the PECO: a framework for formulating good questions to explore the association of environmental and other exposures with health outcomes. Environ Int 121:1027–1031. https://doi.org/10.1016/j.envint.2018.07.015
Hanna N, Silverberg OM, Reaume M, Gladman D, Davis MDP, Piguet V, Alavi A (2022) Incidence, prevalence, and predictors of inflammatory arthritis in patients with hidradenitis suppurativa: a systematic review and meta-analysis. Int J Dermatol 61:1069–1079. https://doi.org/10.1111/ijd.15860
Shea BJ, Reeves BC, Wells G, Thuku M, Hamel C, Moran J et al (2017) AMSTAR 2: a critical appraisal tool for systematic reviews that include randomised or non-randomised studies of healthcare interventions, or both. BMJ 358:j4008. https://doi.org/10.1136/bmj.j4008
Pieper D, Antoine SL, Mathes T, Neugebauer EAM, Eikermann M (2014) Systematic review finds overlap** reviews were not mentioned in every other overview. J Clin Epidemiol 67:368–375. https://doi.org/10.1016/j.jclinepi.2013.11.007
Stolwijk C, van Onna M, Boonen A, van Tubergen A (2016) Global prevalence of spondyloarthritis: a systematic review and meta-regression analysis. Arthritis Care Res (Hoboken) 68:1320–1331. https://doi.org/10.1002/acr.22831
Scotti L, Franchi M, Marchesoni A, Corrao G (2018) Prevalence and incidence of psoriatic arthritis: a systematic review and meta-analysis. Semin Arthritis Rheum 48:28–34. https://doi.org/10.1016/j.semarthrit.2018.01.003
Alamanos Y, Pelechas E, Voulgari PV, Drosos AA (2021) Incidence of spondyloarthritis and its subtypes: a systematic review. Clin Exp Rheumatol 39:660–667. https://doi.org/10.55563/clinexprheumatol/yycy0o
Alinaghi F, Calov M, Kristensen LE, Gladman DD, Coates LC, Jullien D et al (2019) Prevalence of psoriatic arthritis in patients with psoriasis: a systematic review and meta-analysis of observational and clinical studies. J Am Acad Dermatol 80:251-265.e19. https://doi.org/10.1016/j.jaad.2018.06.027
Grant C, Woodbury M, Skougaard M, Boldsen JK, Ogdie A, Klerman EB, Merola JF, Perez-Chada LM (2023) Sleep problems in patients with psoriatic arthritis: a systematic literature review and metaanalysis. J Rheumatol 50:1594–1609. https://doi.org/10.3899/jrheum.2022-1169
Coates LC, Soriano ER, Corp N, Bertheussen H, Duffiin KC, Campanholo CB et al (2022) Group for research and assessment of psoriasis and psoriatic arthritis (GRAPPA): updated treatment recommendations for psoriatic arthritis 2021. Nat Rev Rheumatol 18:465–479. https://doi.org/10.1038/s41584-022-00798-0
Ogdie A, Rozycki M, Arndt T, Shi C, Kim N, Hur P (2021) Longitudinal analysis of the patient pathways to diagnosis of psoriatic arthritis. Arthritis Res Ther 23:252. https://doi.org/10.1186/s13075-021-02628-2
Saalfeld W, Mixon AM, Zelie J, Lydon EJ (2021) Differentiating psoriatic arthritis from osteoarthritis and rheumatoid arthritis: a narrative review and guide for advanced practice providers. Rheumatol Ther 8:1493–1517. https://doi.org/10.1007/s40744-021-00365-1
Ribeiro AL, Dullius L, Sartori NS, Azeredo-da-Silva A, Kohem CL, Coates L, Monticielo OA, Palominos P (2023) Challenges in the management of psoriatic arthritis in Latin America: a systematic review. Clin Ther 45:860–867. https://doi.org/10.1016/j.clinthera.2023.04.005
Vargas-Cruz L, Boechat-Farani J, Rabello-Costa J, de Andrade-Águas JV, Ruschel B, de Almeida-Menegat F et al (2024) Patients with longstanding psoriatic arthritis can achieve DAPSA remission or low disease activity and it correlates to better functional outcomes: results from a Latin-American real-life cohort. Adv Rheumatol 64:3. https://doi.org/10.1186/s42358-023-00338-8
Kuang-Ng BC, Rohit-Jadon D (2021) Unmet needs in psoriatic arthritis. Best Pract Res Clin Rheumatol 35:101693. https://doi.org/10.1016/j.berh.2021.101693
Bedaiwi M, Al-Homood IA, El-Garf A, Uthman I, Sunna N, Nassier R, Mohamed H, Al-Saleh J (2019) Disease burden and treatment challenges of psoriatic arthritis in Africa and the Middle East. Rheumatol Int 39:1321–1329. https://doi.org/10.1007/s00296-019-04319-3
Maharaj AB, Adebajo A (2021) Psoriatic arthritis in Africa. Clin Rheumatol 40:3411–3418. https://doi.org/10.1007/s10067-021-05841-1
Patel AA, Ferrante SA, Lin I, Fu AZ, Campbell AK, Tieng A (2023) Racial and ethnic disparities in treatment initiation among patients with newly diagnosed psoriatic arthritis: a retrospective medicaid claims database study. Rheumatol Ther 10:1241–1253. https://doi.org/10.1007/s40744-023-00580-y
Husni ME, Merola JF, Davin S (2017) The psychosocial burden of psoriatic arthritis. Semin Arthritis Rheum 47:351–360. https://doi.org/10.1016/j.semarthrit.2017.05.010
Funding
This research was not funded by any specific grant from any public, commercial, or non-profit sectors.
Author information
Authors and Affiliations
Contributions
Conception or design of the work: JCHR and JMC. Acquisition, analysis, or interpretation of data for the work: JCHR, CGM and JMC. Drafting the work or revising it critically for important intellectual content: JCHR and JMC. Final approval of the version to be published: JCHR, MIC, CGM, JMS and JMC. All authors approve the final version of the manuscript for publication and agree to take full responsibility for the integrity and accuracy of all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
Authors declare they have no conflict of interest.
Ethical approval
Not applicable.
Informed consent
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hernández-Rodríguez, JC., Infante-Cano, M., García-Muñoz, C. et al. Psoriatic arthritis with psychological comorbidities: an overview of systematic reviews on incidence, prevalence, and geographic disparities. Rheumatol Int (2024). https://doi.org/10.1007/s00296-024-05617-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00296-024-05617-1