Abstract
Purpose
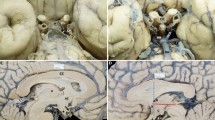
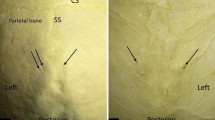
Anatomical knowledge of the floor of the third ventricle (FTV) is essential in avoiding surgical complications during endoscopic third ventriculostomy. The purpose of this study was to characterize the morphometry of FTV and related arteries, particularly the basilar artery (BA), as well as the factors that influence it.
Methods
Twenty-six formalin-fixed adult brains and two hundred adult brain MRIs were studied focusing on FTV and related arteries. Dimensions of interest were measured using image analysis software. Morphometric data obtained were statistically analysed.
Results
Distances between FTV, intermammillary sulcus (IMS), infundibulum, BA bifurcation, and posterior communicating arteries (PCoAs) were described on the cadavers and the MRIs. Distance between right and left PCoAs was greater at their anterior extremity (p < 0.001). Right PCoA was longer (p = 0.016). BA was lateralized in 58.4% of cases and its calibre was larger in males (p < 0.001). The distance from BA apex to FTV was inversely correlated with BA diameter (p < 0.001) and age (p = 0.004). Distance from IMS to infundibulum and the distance between both PCoAs were greater in MRI series when compared to cadaver series (p < 0.001).
Conclusions
A quantitative description of the morphometry of the region of the FTV and related vessels was obtained, hel** neurosurgeons in planning their surgical approach. The distance from BA apex to FTV was shorter in individuals with larger BA calibre and in older subjects. MRI studies were qualitatively superior to cadaveric studies in evaluating the anatomy of this region.






Similar content being viewed by others
References
Hellwig D, Grotenhuis JA, Tirakotai W, Riegel T, Schulte DM, Bauer BL, Bertalanffy H (2005) Endoscopic third ventriculostomy for obstructive hydrocephalus. Neurosurg Rev 28(1):1–34
Jenkinson MD, Hayhurst C, Al-Jumaily M, Kandasamy J, Clark S, Mallucci CL (2009) The role of endoscopic third ventriculostomy in adult patients with hydrocephalus. J Neurosurg 110(5):861–866
Dandy W (1922) An operative procedure for hydrocephalus. Bull Johns Hopkins Hosp 33:189–190
Buxton N, Vloeberghs M, Punt J (1998) Liliequist’s membrane in minimally invasive endoscopic neurosurgery. Clin Anat 11(3):187–190
Bouras T, Sgouros S (2013) Complications of endoscopic third ventriculostomy. World Neurosurg. 79(2):S22.e9-S22.e12
Bouras T, Sgouros S (2011) Complications of endoscopic third ventriculostomy: a review. J Neurosurg Pediatr 7(6):643–649
Lü J, Zhu X (2005) Microsurgical anatomy of the interpeduncular cistern and related arachnoid membranes. J Neurosurg 103(2):337–341
Rhoton AL Jr (2002) The lateral and third ventricles. Neurosurgery 51(4 suppl):S207–S271
Aydin S, Yilmazlar S, Aker S, Korfali E (2009) Anatomy of the floor of the third ventricle in relation to endoscopic ventriculostomy. Clin Anat 22(8):916–924
Lindekleiv HM, Valen-Sendstad K, Morgan MK, Mardal K-A, Faulder K, Magnus JH, Waterloo K, Romner B, Ingebrigtsen T (2010) Sex differences in intracranial arterial bifurcations. Gend Med 7(2):149–155
Ogeng’o JA, Mwachaka PM, Odhiambo DE, Sinkeet SR, Elbusaidy H, Olabu B, Inyimili M (2018) Geometric features of vertebrobasilar arterial system in adult black Kenyans. Int J Morph 36(2):544–550
Volovici V, Varvari I, Dirven CMF, Dammers R (2020) The membrane of Liliequist-a safe haven in the middle of the brain. A narrative review. Acta Neurochir 162(9):2235–2244
Silva SM, Andrade JP (2016) Neuroanatomy: the added value of the Klingler method. Ann Anat 208:187–193
Morota N, Watabe T, Inukai T, Hongo K, Nakagawa H (2000) Anatomical variants in the floor of the third ventricle; implications for endoscopic third ventriculostomy. J Neurol Neurosurg Psychiatry 69(4):531–534
Jones RF, Kwok BC, Stening WA, Vonau M (1994) The current status of endoscopic third ventriculostomy in the management of non-communicating hydrocephalus. Minim Invasive Neurosurg 37(01):28–36
Decq P (2005) Endoscopic anatomy of the ventricles. Morphologie 89(284):12–21
Abtin K, Thompson BG, Walker ML (1998) Basilar artery perforation as a complication of endoscopic third ventriculostomy. Pediatr Neurosurg 28(1):35–41
Colen RR, Kekhia H, Jolesz FA (2010) Multimodality intraoperative MRI for brain tumor surgery. Expert Rev Neurother 10(10):1545–1558
Ganjoo P, Sethi S, Tandon M, Chawla R, Singh D (2009) Incidence and pattern of intraoperative hemodynamic response to endoscopic third ventriculostomy. Neurol India 57(2):162–165
Gunnal S, Farooqui M, Wabale R (2015) Anatomical variability in the termination of the basilar artery in the human cadaveric brain. Turk Neurosurg 25(4):586–594
Wankhede HA, Hosmani P, Nimje DA (2014) Morphological study of the basilar artery in adult human cadavers. Int J Anat Res 2(03):497–502
Pedroza A, Dujovny M, Artero JC, Umansky F, Berman KS, Diaz FG, Ausman JI, Mirchandani HG (1987) Microanatomy of the posterior communicating artery. Neurosurgery 20(2):228–235
Kamath S (1981) Observations on the length and diameter of vessels forming the circle of Willis. J Anat 133(Pt 3):419–423
Lang J (1992) Topographic anatomy of preformed intracranial spaces. Acta Neurochir Suppl 54:1–10
Hayashi N, Endo S, Hamada H, Shibata T, Fukuda O, Takaku A (1999) Role of preoperative midsagittal magnetic resonance imaging in endoscopic third ventriculostomy. Minim Invasive Neurosurg 42(02):79–82
Smoker W, Corbett J, Gentry L, Keyes W, Price M, McKusker S (1986) High-resolution computed tomography of the basilar artery: 2. Vertebrobasilar dolichoectasia: clinical-pathologic correlation and review. AJNR Am J Neuroradiol 7(1):61–72
Ubogu E, Zaidat O (2004) Vertebrobasilar dolichoectasia diagnosed by magnetic resonance angiography and risk of stroke and death: a cohort study. J Neurol Neurosurg Psychiatry 75(1):22–26
El-Dawlatly AA, Murshid WR, Elshimy A, Magboul MA, Samarkandi A, Takrouri MS (2000) The incidence of bradycardia during endoscopic third ventriculostomy. Anesth Analg 91(5):1142–1144
Schulz G, Crooijmans HJ, Germann M, Scheffler M-G, Müller B (2011) Three-dimensional strain fields in human brain resulting from formalin fixation. J Neurosci Methods 202(1):17–27
Owler BK, Pena A, Momjian S, Czosnyka Z, Czosnyka M, Harris NG, Smielewski P, Fryer T, Donvan T, Carpenter A (2004) Changes in cerebral blood flow during cerebrospinal fluid pressure manipulation in patients with normal pressure hydrocephalus: a methodological study. J Cereb Blood Flow Metab 24(5):579–587
Acknowledgements
The authors desire to show deep appreciation for the anonymous cadaver donors of Faculty of Medicine of University of Porto, as well as their families. We also thank Professor Dulce Madeira, Director of the Unit of Anatomy of the Department of Biomedicine and responsible for the Body Donation Program, for her permanent support.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
J Fernandes-Silva: project development, data collection, data analysis, and manuscript writing and editing. SM Silva: project development, data collection, data analysis, and manuscript writing and editing. H Alves: data analysis and manuscript writing and editing. JP Andrade: data collection, data analysis, and manuscript writing and editing. M Arantes: project development, data collection, data analysis, and manuscript writing and editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors wish to declare no conflicts of interests, and no commercial relationships.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fernandes-Silva, J., Silva, S.M., Alves, H. et al. Neurosurgical anatomy of the floor of the third ventricle and related vascular structures. Surg Radiol Anat 43, 1915–1925 (2021). https://doi.org/10.1007/s00276-021-02785-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-021-02785-8