Abstract
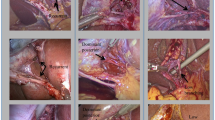
The sulcus of the caudate process is a horizontal groove on the inferior face of the liver. Its prevalence has not previously been determined. Because of its location, it represents a helpful extra-biliary landmark that could be used in biliary surgery to decrease bile duct injury. The goal of this study is to determine the prevalence of Rouviere’s sulcus and describe its anatomy and relevant surgical applications. We conducted a literature review on the various characteristics of the sulcus, selecting anatomical clinical studies and dissections. We performed 10 cadaveric dissections in the Laboratory of Anatomy at Purpan University to determine the contents. We selected 12 anatomical studies, conducted between 1924 and January 1st, 2020, which included 2394 patients. The prevalence of the sulcus is 78.24% ± 9.1. Classification of Singh was used to describe anatomical characteristics. Type I (“deep sulcus”) was identified in 50.4% ± 9.8 of cases, mostly consisting of Type Ia (open). Type II (“slit-like”) was estimated to account for 13.3% ± 13.2, whereas Type III (“scar”) described 12.3% ± 8.0. Average dimensions were estimated for length (26 mm ± 5.7), width (6.5 mm ± 1.5), and depth (7.9 mm ± 1.75). The content of the sulcus consists of the right portal vein and its division, the right hepatic artery, along with the right hepatic bile duct. The sulcus determines the orientation of the common bile duct. The sulcus of the caudate process is a reliable extra-biliary landmark, which presents a useful tool for reducing bile duct injuries during hepatobiliary surgery.



Similar content being viewed by others
References
AL-Naser M (2018) Rouviere’s sulcus: a useful anatomical landmark for safe laparoscopic cholecystectomy. 158–161
Altieri MS, Brunt LM (2019) Elimination of bile duct injury in cholecystectomy. Adv Surg 53:145–160. https://doi.org/10.1016/j.yasu.2019.04.018
Altieri MS, Yang J, Obeid N, Zhu C, Talamini M, Pryor A (2018) Increasing bile duct injury and decreasing utilization of intraoperative cholangiogram and common bile duct exploration over 14 years: an analysis of outcomes in New York State. Surg Endosc 32:667–674. https://doi.org/10.1007/s00464-017-5719-2
Aoki S, Mizuma M, Hayashi H, Nakagawa K, Morikawa T, Motoi F, Naitoh T, Egawa S, Unno M (2016) Surgical anatomy of the right hepatic artery in Rouviere’s sulcus evaluated by preoperative multidetector-row CT images. BMC Surg 16:40. https://doi.org/10.1186/s12893-016-0155-0
Berney CR (2012) Major common bile duct injury and risk of litigation: a surgeon’s perspective. Am J Surg 204:800–802. https://doi.org/10.1016/j.amjsurg.2011.06.009
Buddingh KT, Weersma RK, Savenije RAJ, van Dam GM, Nieuwenhuijs VB (2011) Lower rate of major bile duct injury and increased intraoperative management of common bile duct stones after implementation of routine intraoperative cholangiography. J Am Coll Surg 213:267–274. https://doi.org/10.1016/j.jamcollsurg.2011.03.004
Cimpeanu I, Băjenaru N, Puşcaşu A (2017) A lesser-known hepatic anatomical and surgical structure: the Rouviere-Gans Incisura (RGI). Chrurigia 112:252. https://doi.org/10.21614/chirurgia.112.3.252
Connor SJ, Perry W, Nathanson L, Hugh TB, Hugh TJ (2014) Using a standardized method for laparoscopic cholecystectomy to create a concept operation-specific checklist. HPB (Oxford) 16:422–429. https://doi.org/10.1111/hpb.12161
Couinaud C (1957) Le Foie, études anatomiques et chirurgicales. Masson, Masson et Cie
Dahmane R, Morjane A, Starc A (2013) Anatomy and surgical relevance of Rouviere’s sulcus. Sci World J 2013:254287. https://doi.org/10.1155/2013/254287
Elwan A (2019) Critical view of safety and Rouviere’s sulcus: extrahepatic biliary landmarks as a guide to safe laparoscopic cholecystectomy. Sci J Al-Azhar Med Facl 3:297–301
Gans H (1955) Introduction to Hepatic Surgery. Introduction to Hepatic Surgery. Elsevier, Netherlands, pp 50–53
Halbert C, Altieri MS, Yang J, Meng Z, Chen H, Talamini M, Pryor A, Parikh P, Telem DA (2016) Long-term outcomes of patients with common bile duct injury following laparoscopic cholecystectomy. Surg Endosc 30:4294–4299. https://doi.org/10.1007/s00464-016-4745-9
Hugh TB (2002) New strategies to prevent laparoscopic bile duct injury–surgeons can learn from pilots. Surgery 132:826–835. https://doi.org/10.1067/msy.2002.127681
Hugh TB, Kelly MD, Mekisic A (1997) Rouvière’s sulcus: a useful landmark in laparoscopic cholecystectomy. Br J Surg 84:1253–1254. https://doi.org/10.1046/j.1365-2168.1997.02769.x
Kim JH, Cho BS, Jang J-H (2018) Pure laparoscopic anatomical segment VI resection using the Glissonian approach, Rouviere’s sulcus as a landmark, and a modified liver hanging maneuver (with video). Langenbecks Arch Surg 403:131–135. https://doi.org/10.1007/s00423-018-1652-7
Kim JK, Kim JY, Park JS, Yoon DS (2016) Clinical significance of Rouviere sulcus during laparoscopic cholecystectomy. HPB 18:e515–e516. https://doi.org/10.1016/j.hpb.2016.03.370
Lazarus L, Luckrajh J, Mewa Kinoo S, Singh B (2018) Anatomical parameters of the Rouviere’s sulcus for laparoscopic cholecystectomy. Eur J Anat 22(5):389–395
Lockhart S, Singh-Ranger G (2018) Rouviere’s sulcus-Aspects of incorporating this valuable sign for laparoscopic cholecystectomy. Asian J Surg 41:1–3. https://doi.org/10.1016/j.asjsur.2016.07.012
Macchi V, Feltrin G, Parenti A, De Caro R (2003) Diaphragmatic sulci and portal fissures. J Anat 202:303–308. https://doi.org/10.1046/j.1469-7580.2003.00160.x
Peti N, Moser MAJ (2012) Graphic reminder of Rouviere’s sulcus: a useful landmark in cholecystectomy. ANZ J Surg 82:367–368. https://doi.org/10.1111/j.1445-2197.2012.06032.x
Rafi Y, Mukhtar Z, Zaman B (2018) Rouviere’s sulcus, a safe landmark for laparoscopic cholecystectomy. PJMHS 12:1511–1513
Reynaud BH, Coucoravas GO, Giuly JA (1991) Basis to improve several hepatectomy techniques involving the surgical anatomy of incisura dextra of Gans. Surg Gynecol Obstet 172:490–492
Rouvière H (1924) sur la configuration et la signification du sillon du processus caudé. In: Bulletin de la Société Anatomique de Paris. Paris, pp 355–358
Schendel J, Ball C, Dixon E, Sutherland F (2019) Prevalence of anatomic landmarks for orientation during elective laparoscopic cholecystectomies. Surg Endosc. https://doi.org/10.1007/s00464-019-07131-z
Shimizu A, Lefor A, Noda Y, Sata N (2016) Bile duct anomalies are associated with closed Rouviere’s sulcus of the liver: “the closed Rouviere’s sulcus sign” for increased intraoperative vigilance. HBP- Official J Int Hepato-Pancreatico-Biliary Assoc 18 (suppl 1)
Singh M, Prasad N (2017) The anatomy of Rouviere’s sulcus as seen during laparoscopic cholecystectomy: a proposed classification. J Minim Access Surg 13:89–95. https://doi.org/10.4103/0972-9941.201731
Strasberg SM (2019) A three-step conceptual roadmap for avoiding bile duct injury in laparoscopic cholecystectomy: an invited perspective review. J Hepatobiliary Pancreat Sci 26:123–127. https://doi.org/10.1002/jhbp.616
Strasberg SM, Brunt LM (2010) Rationale and use of the critical view of safety in laparoscopic cholecystectomy. J Am Coll Surg 211:132–138. https://doi.org/10.1016/j.jamcollsurg.2010.02.053
Strasberg SM, Helton WS (2011) An analytical review of vasculobiliary injury in laparoscopic and open cholecystectomy. HPB (Oxford) 13:1–14. https://doi.org/10.1111/j.1477-2574.2010.00225.x
Strasberg SM, Hertl M, Soper NJ (1995) An analysis of the problem of biliary injury during laparoscopic cholecystectomy. J Am Coll Surg 180:101–125
Sutherland F, Dixon E (2017) The importance of cognitive map placement in bile duct injuries. Can J Surg 60:424–425. https://doi.org/10.1503/cjs.008816
Takada T (2018) Tokyo Guidelines 2018: updated Tokyo Guidelines for the management of acute cholangitis/acute cholecystitis. J Hepatobiliary Pancreat Sci 25:1–2. https://doi.org/10.1002/jhbp.526
Thapa PB, Maharjan DK, Tamang TY, Shrestha SK (2015) Visualisation of Rouviere’s sulcus during laparoscopic cholecystectomy. JNMA J Nepal Med Assoc 53:188–191
Tomaszewski KA, Henry BM, Kumar Ramakrishnan P, Roy J, Vikse J, Loukas M, Tubbs RS, Walocha JA (2017) Development of the Anatomical Quality Assurance (AQUA) checklist: guidelines for reporting original anatomical studies. Clin Anat 30:14–20. https://doi.org/10.1002/ca.22800
Yamashita Y, Kimura T, Matsumoto S (2010) A safe laparoscopic cholecystectomy depends upon the establishment of a critical view of safety. Surg Today 40:507–513. https://doi.org/10.1007/s00595-009-4218-z
Zhao W, Wang P, Hu Q, Liu L, Lu Q, Li W, Huang Q (2017) application of Rouviere groove guiding and positioning combined with “safety window” technique in difficult laparoscopic cholecystectomy. Chinese J Gen Surg 26:1506–1510
Richard LD (2019) FIPAT (Federative International Programme on Anatomical Terminologies). Pak J Surg 25:119–121
Terminologia anatomica: international anatomical terminology, 2nd edition. Thieme
Funding
This research was supported by the Laboratory of Anatomy of Purpan University, Toulouse, France.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by PG, BV and MC. The first draft of the manuscript was written by PG and LR, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
Authors do not declare any conflict of interest.
Data availability and material
Material available.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Péré, G., Benvegnu, V., Mercé, C. et al. The sulcus of the caudate process (Rouviere’s sulcus): anatomy and clinical applications—a review of current literature. Surg Radiol Anat 42, 1441–1446 (2020). https://doi.org/10.1007/s00276-020-02529-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-020-02529-0