Abstract
Objective
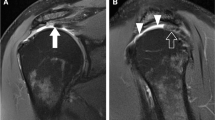
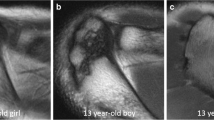
To determine if a Bennett lesion and its size are associated with additional MRI shoulder abnormalities in an overhead athlete.
Materials and methods
An IRB-approved retrospective review of our database from 1 January 2012 to 1 April 2018 identified 35 overhead athletes with a Bennett lesion on MRI. A control group consisting of 35 overhead athletes without a Bennett lesion were matched for age, level of play (professional vs non-professional), and type of study (arthrogram vs non-arthrogram). Each study was assessed independently by two MSK fellowship trained radiologists. The sizes of the Bennett lesions were measured. Each MRI was assessed for the presence of a labral tear, posterior glenoid cartilage abnormality, humeral head notching or cysts, and fraying or tear of the supraspinatus or infraspinatus tendons. Statistical analyses were performed using Student’s t test, Fisher’s exact test, and Chi-squared test.
Results
There was an increased incidence of posterior glenoid cartilage abnormalities in athletes with Bennett lesions vs those without (23% vs 3%, p value = 0.01). There was no difference in any other MRI abnormalities, including labral tears and findings of internal im**ement between these two groups (p value range = 0.09–0.46). There was no association between the size of a Bennett lesion and the presence of glenoid cartilage lesions, labral tears, internal im**ement, age, professional status, or need for surgery (p value range = 0.08–0.96).
Conclusion
Symptomatic overhead athletes with Bennett lesions have an increased frequency of posterior glenoid cartilage abnormalities, but not labral tears or findings of internal im**ement compared to those without Bennett lesions.




Similar content being viewed by others
References
Wright RW, Paletta GA. Prevalence of the Bennett lesion of the shoulder in major league pitchers. Am J Sports Med. 2004;32(1):121–4.
Barnes DA, Tullos HS. An analysis of 100 symptomatic baseball players. Am J Sports Med. 1978;6(2):62–7.
Bennett GE. Shoulder and elbow lesions of the professional baseball pitcher. JAMA. 1941;117(7):510–4.
Bennett GE. Elbow and shoulder lesions of baseball players. Am J Surg. 1959;98(3):484–92.
Lombardo SJ, Jobe FW, Kerlan RK, Carter VS, Shields CL. Posterior shoulder lesions in throwing athletes. Am J Sports Med. 1977;5(3):106–10.
Ferrari JD, Ferrari DA, Coumas J, Pappas AM. Posterior ossification of the shoulder: the Bennett lesion. Etiology, diagnosis, and treatment. Am J Sports Med. 1994;22(2):171–6.
Nakagawa S, Yoneda M, Hayashida K, Mizuno N, Yamada S. Posterior shoulder pain in throwing athletes with a Bennett lesion: factors that influence throwing pain. J Shoulder Elbow Surg. 2006;15(1):72–7.
Park JY, Noh YM, Chung SW, et al. Bennett lesions in baseball players detected by magnetic resonance imaging: assessment of association factors. J Shoulder Elbow Surg. 2016;25(5):730–8.
Miniaci A, Mascia AT, Salonen DC, Becker EJ. Magnetic resonance imaging of the shoulder in asymptomatic professional baseball pitchers. Am J Sports Med. 2002;30(1):66–73.
Giaroli EL, Major NM, Higgins LD. MRI of internal im**ement of the shoulder. AJR Am J Roentgenol. 2005;185(4):925–9.
Meister K, Andrews JR, Batts J, Wilk K, Baumgarten T. Symptomatic thrower’s exostosis. Arthroscopic evaluation and treatment. Am J Sports Med. 1999;27(2):133–6.
Grossman MG, Tibone JE, McGarry MH, Schneider DJ, Veneziani S, Lee TQ. A cadaveric model of the throwing shoulder: a possible etiology of superior labrum anterior-to-posterior lesions. J Bone Joint Surg Am. 2005;87(4):824–31.
Koike Y, Komatsuda T, Sato K. Osteochondritis dissecans of the glenoid associated with the nontraumatic, painful throwing shoulder in a professional baseball player: a case report. J Shoulder Elbow Surg. 2008;17(5):e9–12.
Yoneda M, Nakagawa S, Hayashida K, Fukushima S, Wakitani S. Arthroscopic removal of symptomatic Bennett lesions in the shoulders of baseball players: arthroscopic Bennett-plasty. Am J Sports Med. 2002;30(5):728–36.
De Jesus JO, Parker L, Frangos AJ, Nazarian LN. Accuracy of MRI, MR arthrography, and ultrasound in the diagnosis of rotator cuff tears: a meta-analysis. AJR Am J Roentgenol. 2009;192(6):1701–7.
Magee T. 3-T MRI of the shoulder: is MR arthrography necessary? AJR Am J Roentgenol. 2009;192(1):86–92.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This is an IRB-approved study.
Conflicts of interest
Tony T. Wong is a Consultant for SoundStim Therapeutics (not relevant to this work).
The authors declare that they have no other conflicts of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Karcich, J., Kazam, J.K., Rasiej, M.J. et al. Bennett lesions in overhead athletes and associated shoulder abnormalities on MRI. Skeletal Radiol 48, 1233–1240 (2019). https://doi.org/10.1007/s00256-019-03176-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-019-03176-2