Abstract
Summary
Our study demonstrated a high incidence of recollapse of the augmented vertebrae after PVP treatment for OVCFs. A risk score based on all significant factors can predict the rate of recollapse and gain clinical benefits to prevent recollapse in patients at high risk.
Background
Recollapse of the augmented vertebrae after percutaneous vertebroplasty (PVP) treatment for osteoporotic vertebral compression fractures (OVCFs) has obtained much attention. However, little is known about risk factors and score for recollapse of the augmented vertebrae.
Objective
To determine risk factors and furthermore develop a risk score related to recollapse of the augmented vertebrae after PVP treatment for OVCFs.
Methods
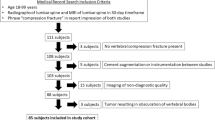
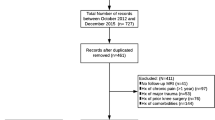
Patients who were treated with PVP for single OVCFs and met this study’s inclusion criteria were retrospectively reviewed. The follow-up period was at least 2 years. Associations of recollapse with co-variates (age, gender, bone mass density [BMD] with a T-score, fracture level, intravertebral cleft [IVC], fracture type, cement volume, cement leakage, leakage into a disc, cement distribution pattern, Non-PMMA-endplate-contact [NPEC], preoperative fracture severity, reduction rate [RR], reduction angle [RA]) were analyzed and a risk score for recollapse was further developed to predict recollapse.
Results
A total of 152 patients were included. Recollapse group was found in 42 (27.6%) patients. Preoperative IVC, solid lump cement distribution pattern, more RR (a cutoff value of 7%) and larger RA (a cutoff value of 3°) was significantly associated with increased risk for recollapse of the augmented vertebrae. A risk score was developed based on the number of risk factors present in each patient. Patients with a score of 4 had an approximately ninefold increased risk of develo** recollapse over patients with a score of 0. The receiver operating characteristic curve of the risk score generated an area under the curve of 0.899 (95% CI 0.642–0.836, P = 0.000).
Conclusion
A risk score based on preoperative IVC, cement distribution pattern, reduction rate, and reduction angle predicts the rate of recollapse. Additional studies should aim to validate this score and inspect clinical benefits of recollapse prophylaxis in patients at high risk.




Similar content being viewed by others
Reference
Johnell O, Kanis JA (2006) An estimate of the worldwide prevalence and disability associated with osteoporotic fractures. Osteoporos Int 17:1726–1733
Borgstrom F, Sobocki P, Strom O et al (2007) The societal burden of osteoporosis in Sweden. Bone 40:1602–1609
Garfin SR, Yuan HA, Reiley M (2001) A new technologies in spine: kyphoplasty and vertebroplasty for the treatment of painful osteoporotic compression fractures. Spine (Phila Pa 1976) 26:1511–1515
Zethraeus N, Borgstrom F, Strom O et al (2007) Cost-effectiveness of the treatment and prevention of osteoporosis--a review of the literature and a reference model. Osteoporos Int 18:9–23
McConnell CT Jr, Wippold FJ, Ray CE Jr et al (2014) ACR appropriateness criteria management of vertebral compression fractures. J Am Coll Radiol 11:757–763
Kim DH, Vaccaro AR (2006) Osteoporotic compression fractures of the spine; current options and considerations for treatment. Spine J 6:479–487
Melton LJ, Kan SH, Frye MA et al (1989) Epidemiology of vertebral fractures in women. Am J Epidemiol 129:1000–1011
Suzuki N, Ogikubo O, Hansson T (2008) The course of the acute vertebral body fragility fracture: its effect on pain, disability and quality of life during 12 months. Eur Spine J 17:1380–1390
Barr JD, Barr MS, Lemley TJ, McCann RM (2000) Percutaneous vertebroplasty for pain relief and spinal stabilization. Spine (Phila Pa 1976) 25:923–928
Jang JS, Kim DY, Lee SH (2003) Efficacy of percutaneous vertebroplasty in the treatment of intravertebral pseudarthrosis associated with noninfected avascular necrosis of the vertebral body. Spine (Phila Pa 1976) 28:1588–1592
Masala S, Mastrangeli R, Petrella MC, Massari F, Ursone A, Simonetti G (2009) Percutaneous vertebroplasty in 1,253 levels: results and long-term effectiveness in a single centre. Eur Radiol 19:165–171
Kang SK, Lee CW, Park NK, Kang TW, Lim JW, Cha KY, Kim JH (2011) Predictive risk factors for refracture after percutaneous vertebroplasty. Ann Rehabil Med 35:844–851
Heo DH, Chin DK, Yoon YS, Kuh SU (2009) Recollapse of previous vertebral compression fracture after percutaneous vertebroplasty. Osteoporos Int 20:473–480
Lin WC, Lee YC, Lee CH, Kuo YL, Cheng YF, Lui CC, Cheng TT (2008) Refractures in cemented vertebrae after percutaneous vertebroplasty: a retrospective analysis. Eur Spine J 17:592–599
Lin WC, Lu CH, Chen HL, Wang HC, Yu CY, Wu RW, Cheng YF, Lui CC (2010) The impact of preoperative magnetic resonance images on outcome of cemented vertebrae. Eur Spine J 19:1899–1906
Jensen ME, Evans AJ, Mathis JM et al (1997) Percutaneous polymethylmethacrylate vertebroplasty in the treatment of osteoporotic vertebral body compression fractures: technical aspects. AJNR Am J Neuroradiol 18:1897–1904
Yu W, Liang, Yao Z et al (2017) Risk factors for recollapse of the augmented vertebrae after percutaneous vertebroplasty for osteoporotic vertebral fractures with intravertebral vacuum cleft. Medicine 96:e5675
Libicher M, Appelt A, Berger I, Baier M, Meeder PJ, Grafe I, DaFonseca K, Nöldge G, Kasperk C (2007) The intravertebral vacuum phenomen as specific sign of osteonecrosis in vertebral compression fractures: results from a radiological and histological study. Eur Radiol 17:2248–2252
Linn J, Birkenmaier C, Hoffmann RT, Reiser M, Baur-Melnyk A (2009) The intravertebral cleft in acute osteoporotic fractures: fluid in magnetic resonance imaging-vacuum in computed tomography? Spine (Phila Pa 1976) 34:E88–E93
Kim MJ, Lindsey DP, Hannibal M et al (2006) Vertebroplasty versus kyphoplasty: biomechanical behavior under repetitive loading conditions. Spine (Phila Pa 1976) 31:2079–2084
Kim YY, Rhyu KW (2010) Recompression of vertebral body after balloon kyphoplasty for osteoporotic vertebral compression fracture. Eur Spine J 19:1907–1912
Buchbinder R, Osborne RH, Ebeling PR, Wark JD, Mitchell P, Wriedt C, Graves S, Staples MP, Murphy B (2009) A randomized trial of vertebroplasty for painful osteoporotic vertebral fractures. N Engl J Med 361:557–568
Kallmes DF, Comstock BA, Heagerty PJ, Turner JA, Wilson DJ, Diamond TH, Edwards R, Gray LA, Stout L, Owen S, Hollingworth W, Ghdoke B, Annesley-Williams DJ, Ralston SH, Jarvik JG (2009) A randomized trial of vertebroplasty for osteoporotic spinal fractures. N Engl J Med 361:569–579
McGuire R (2011) AAOS clinical practice guideline: the treatment of symptomatic osteoporotic spinal compression fractures. J Am Acad Orthop Surg 19:183–184
Brodano GB, Amendola L, Martikos K, Bettuzzi C, Boriani L, Gasbarrini A, Bandiera S, Terzi S, Greggi T, Boriani S (2011) Vertebroplasty: benefits are more than risks in selected and evidence-based informed patients. A retrospective study of 59 cases. Eur Spine J 20:1265–1271
Gerling MC, Eubanks JD, Patel R, Whang PG, Bohlman HH, Ahn NU (2011) Cement augmentation of refractory osteoporotic vertebral compression fractures: survivorship analysis. Spine (Phila Pa 1976) 36:E1266–E1269
Kotwica Z, Saracen A (2011) Early and long-term outcomes of vertebroplasty for single osteoporotic fractures. Neurol Neurochir Pol 45:431–435
Kung-Chia Li WMW, Tak-Uee Wong WMW, Fu-Chi Kung WMW et al (2004) STAGING of Kümmell’s disease. J Musculoskelet Res 8:43–55
Yu W, Jiang X, Liang et al (2017) Intravertebral vacuum cleft and its varied locations within osteoporotic vertebral compression fractures: effect on therapeutic efficacy. Pain Physician 20:E979–E986
Chen YJ, Chen WH, Chen HT, Hsu HC (2012) Repeat needle insertion in vertebroplasty to prevent re-collapse of the treated vertebrae. Eur J Radiol 81:558–561
Niu J, Zhou H, Meng Q, Shi J, Meng B, Yang H (2015) Factors affecting recompression of augmented vertebrae after successful percutaneous balloon kyphoplasty: a retrospective analysis. Acta Radiol 56:1380–1387
Chen LH, Hsieh MK, Liao JC, Lai PL, Niu CC, Fu TS, Tsai TT, Chen WJ (2011) Repeated percutaneous vertebroplasty for refracture of cemented vertebrae. Arch Orthop Trauma Surg 131:927–933
Yu WB, Liang D, Jiang XB, Yao ZS, Qiu T, Ye LQ (2017) Efficacy and safety of the target puncture technique for treatment of osteoporotic vertebral compression fractures with intravertebral clefts. J Neurointerv Surg 9:1113–1117
McKiernan F, Faciszewski T, Jensen R (2003) Reporting height restoration in vertebral compression fractures. Spine (Phila Pa 1976) 28:2517–2521
Funding
The authors gratefully acknowledge the support from the National Natural Science Foundation of China (81804113).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Statement of informed consent
For this type of study formal consent is not required.
Rights and permissions
About this article
Cite this article
Yu, W.B., Jiang, X.B., Liang, D. et al. Risk factors and score for recollapse of the augmented vertebrae after percutaneous vertebroplasty in osteoporotic vertebral compression fractures. Osteoporos Int 30, 423–430 (2019). https://doi.org/10.1007/s00198-018-4754-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-018-4754-8